Abstract
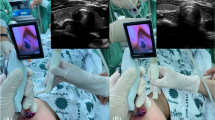
This study aimed to evaluate the 50% and 95% effective paratracheal forces for occluding the esophagus in anesthetized patients. In 46 anesthetized patients, the upper esophagus was examined using ultrasonography, and the lower paratracheal area over the esophagus just above the clavicle was marked. Manual paratracheal force was applied over that area using a novel pressure sensing device set-up. In the first patient, a 20 N paratracheal force was applied, and the patency of the esophagus was assessed by advancing the esophageal stethoscope. Unsuccessful advancement of the esophageal stethoscope was considered an effective paratracheal force. If advancement of the esophageal stethoscope was successful, the paratracheal force was increased by 2 N for the next patient, and if it was unsuccessful, the force was decreased by 2 N for the next patient. These sequential tests were performed using 12- and 18-Fr esophageal stethoscopes, respectively. According to Dixon and Mood method, the 50% effective paratracheal force (confidence interval) was 18.4 (17.5‒19.3) N with the use of a 12-Fr esophageal stethoscope and 12.8 (11.0‒14.6) N with the use of an 18-Fr esophageal stethoscope. Using probit regression analysis, the 50% and 95% effective paratracheal forces were 18.4 (16.8‒19.6) N and 20.6 (19.4‒27.9) N, respectively, with the use of a 12-Fr esophageal stethoscope, and 12.4 (8.3‒14.4) N and 16.9 (14.7‒37.3) N, respectively, with the use of an 18-Fr esophageal stethoscope. Our findings suggest a guide for applying paratracheal force during rapid sequence induction and tracheal intubation.



Similar content being viewed by others
References
Salem MR, Khorasani A, Zeidan A, Crystal GJ. Cricoid pressure controversies: narrative review. Anesthesiology. 2017;126:738–52.
Sellick BA. Cricoid pressure to control regurgitation of stomach contents during induction of anaesthesia. Lancet. 1961;2:404–6.
Smith KJ, Ladak S, Choi PT, Dobranowski J. The cricoid cartilage and the esophagus are not aligned in close to half of adult patients. Can J Anesth. 2002;49:503–7.
Smith KJ, Dobranowski J, Yip G, Dauphin A, Choi PT. Cricoid pressure displaces the esophagus: an observational study using magnetic resonance imaging. Anesthesiology. 2003;99:60–4.
Rice MJ, Mancuso AA, Gibbs C, Morey TE, Gravenstein N, Deitte LA. Cricoid pressure results in compression of the postcricoid hypopharynx: the esophageal position is irrelevant. Anesth Analg. 2009;109:1546–52.
Zeidan AM, Salem MR, Mazoit JX, Abdullah MA, Ghattas T, Crystal GJ. The effectiveness of cricoid pressure for occluding the esophageal entrance in anesthetized and paralyzed patients: an experimental and observational glidescope study. Anesth Analg. 2014;118:580–6.
Zhu SY, Liu RC, Chen LH, Yang H, Feng X, Liao XH. Sonographic anatomy of the cervical esophagus. J Clin Ultrasound. 2004;32:163–71.
Gautier N, Danklou J, Brichant JF, Lopez AM, Vandepitte C, Kuroda MM, et al. The effect of force applied to the left paratracheal oesophagus on air entry into the gastric antrum during positive-pressure ventilation using a facemask. Anaesthesia. 2019;74:22–8.
Dixon WJ, Mood AM. A method for obtaining and analyzing sensitivity data. J Am Stat Assoc. 1948;43:109–26.
Pace NL, Stylianou MP. Advances in and limitations of up-and-down methodology: a precis of clinical use, study design, and dose estimation in anesthesia research. Anesthesiology. 2007;107:144–52.
Paul M, Fisher DM. Are estimates of MAC reliable? Anesthesiology. 2001;95:1362–70.
Noguchi K, Marmolejo-Ramos F. Assessing equality of means using the overlap of range-preserving confidence intervals. Am Stat. 2016;70:325–34.
Andruszkiewicz P, Wojtczak J, Wroblewski L, Kaczor M, Sobczyk D, Kowalik I. Ultrasound evaluation of the impact of cricoid pressure versus novel “paralaryngeal pressure” on anteroposterior oesophageal diameter. Anaesthesia. 2016;71:1024–9.
Vanner RG, Pryle BJ. Regurgitation and oesophageal rupture with cricoid pressure: a cadaver study. Anaesthesia. 1992;47:732–5.
Hartsilver EL, Vanner RG, Bewley J, Clayton T. Gastric pressure during emergency caesarean section under general anaesthesia. Br J Anaesth. 1999;82:752–4.
Zeidan AM, Salem MR, Bamadhaj M, Mazoit J-X, Sadek H, Houjairy H, et al. The cricoid force necessary to occlude the esophageal entrance: is there a gender difference? Anesth Analg. 2017;124:1168–73.
Acknowledgements
Pressure sensor device’s work was supported by Korea Institute of Energy Technology Evaluation and Planning (KETEP) grant funded by the Korea government (MOTIE) (20181510102340, Development of a real-time detection system for unidentified RCS leakage less than 0.5 gpm). The authors would like to thank Myungjin Jang, PhD of the Medical Research Collaborating Center in Seoul National University Biomedical Research Institute for statistical advice.
Author information
Authors and Affiliations
Contributions
HK and JYH designed the study, conducted the study, analyzed the data, and wrote the manuscript. SM and CGC helped design the study, conduct the study, analyze the data, and write the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, H., Mondal, S., Choi, CG. et al. Assessment of the 50 % and 95 % effective paratracheal forces for occluding the esophagus in anesthetized patients. J Clin Monit Comput 36, 335–340 (2022). https://doi.org/10.1007/s10877-021-00652-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-021-00652-w