Abstract
Purpose
Chronic granulomatous disease (CGD) is a primary immunodeficiency characterized by an inability of phagocytes to produce reactive oxygen species, impairing their killing of various bacteria and fungi. We summarize here the 93 cases of CGD diagnosed in Mexico from 2011 to 2019.
Methods
Thirteen Mexican hospitals participated in this study. We describe the genetic, immunological, and clinical features of the 93 CGD patients from 78 unrelated kindreds.
Results
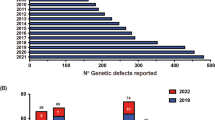
Eighty-two of the patients (88%) were male. All patients developed bacterial infections and 30% suffered from some kind of fungal infection. Fifty-four BCG-vaccinated patients (58%) presented infectious complications of BCG vaccine. Tuberculosis occurred in 29%. Granulomas were found in 56% of the patients. Autoimmune and inflammatory diseases were present in 15% of patients. A biological diagnosis of CGD was made in 89/93 patients, on the basis of NBT assay (n = 6), DHR (n = 27), and NBT plus DHR (n = 56). The deficiency was complete in all patients. The median age of biological diagnosis was 17 months (range, 0–186 months). A genetic diagnosis was made in 83/93 patients (when material was available), corresponding to CYBB (n = 64), NCF1 (n = 7), NCF2 (n = 7), and CYBA (n = 5) mutations.
Conclusions
The clinical manifestations in these Mexican CGD patients were similar to those in patients elsewhere. This cohort is the largest in Latin America. Mycobacterial infections are an important cause of morbidity in Mexico, as in other countries in which tuberculosis is endemic and infants are vaccinated with BCG. X-linked CGD accounted for most of the cases in Mexico, as in other Latin American countries. However, a significant number of CYBA and NCF2 mutations were identified, expanding the spectrum of known causal mutations.





Similar content being viewed by others
References
Roos D, Kuhns DB, Maddalena A, Roesler J, Lopez JA, Ariga T, et al. Hematologically important mutations: X-linked chronic granulomatous disease (third update). Blood Cells Mol Dis. 2010;45(3):246–65.
Roos D, Kuhns DB, Maddalena A, Bustamante J, Kannengiesser C, de Boer M, et al. Hematologically important mutations: the autosomal recessive forms of chronic granulomatous disease (second update). Blood Cells Mol Dis. 2010;44(4):291–9.
Arnadottir GA, Norddahl GL, Gudmundsdottir S, Agustsdottir AB, Sigurdsson S, Jensson BO, et al. A homozygous loss-of-function mutation leading to CYBC1 deficiency causes chronic granulomatous disease. Nat Commun. 2018;9(1):4447.
Thomas DC, Charbonnier LM, Schejtman A, Aldhekri H, Coomber EL, Dufficy ER, et al. EROS/CYBC1 mutations: decreased NADPH oxidase function and chronic granulomatous disease. J Allergy Clin Immunol. 2019;143(2):782–5 e1.
van de Geer A, Nieto-Patlan A, Kuhns DB, Tool AT, Arias AA, Bouaziz M, et al. Inherited p40phox deficiency differs from classic chronic granulomatous disease. J Clin Invest. 2018;128(9):3957–75.
Segal BH, Grimm MJ, Khan AN, Han W, Blackwell TS. Regulation of innate immunity by NADPH oxidase. Free Radic Biol Med. 2012;53(1):72–80.
Chiriaco M, Salfa I, Di Matteo G, Rossi P, Finocchi A. Chronic granulomatous disease: clinical, molecular, and therapeutic aspects. Pediatr Allergy Immunol. 2016;27(3):242–53.
Roos D, de Boer M. Molecular diagnosis of chronic granulomatous disease. Clin Exp Immunol. 2014;175(2):139–49.
Kovacs I, Horvath M, Lanyi A, Petheo GL, Geiszt M. Reactive oxygen species-mediated bacterial killing by B lymphocytes. J Leukoc Biol. 2015;97(6):1133–7.
Baba LA, Ailal F, El Hafidi N, Hubeau M, Jabot-Hanin F, Benajiba N, et al. Chronic granulomatous disease in Morocco: genetic, immunological, and clinical features of 12 patients from 10 kindreds. J Clin Immunol. 2014;34(4):452–8.
Bustamante J, Aksu G, Vogt G, de Beaucoudrey L, Genel F, Chapgier A, et al. BCG-osis and tuberculosis in a child with chronic granulomatous disease. J Allergy Clin Immunol. 2007;120(1):32–8.
van den Berg JM, van Koppen E, Ahlin A, Belohradsky BH, Bernatowska E, Corbeel L, et al. Chronic granulomatous disease: the European experience. PLoS One. 2009;4(4):e5234.
Zhou Q, Hui X, Ying W, Hou J, Wang W, Liu D, et al. A cohort of 169 chronic granulomatous disease patients exposed to BCG vaccination: a retrospective study from a single center in Shanghai, China (2004-2017). J Clin Immunol. 2018;38(3):260–72.
Ben-Ari J, Wolach O, Gavrieli R, Wolach B. Infections associated with chronic granulomatous disease: linking genetics to phenotypic expression. Expert Rev Anti-Infect Ther. 2012;10(8):881–94.
Conti F, Lugo-Reyes SO, Blancas-Galicia L, He J, Aksu G, Borges de Oliveira E Jr, et al. Mycobacterial disease in patients with chronic granulomatous disease: a retrospective analysis of 71 cases. J Allergy Clin Immunol. 2016;138(1):241–8 e3.
Lee PP, Chan KW, Jiang L, Chen T, Li C, Lee TL, et al. Susceptibility to mycobacterial infections in children with X-linked chronic granulomatous disease: a review of 17 patients living in a region endemic for tuberculosis. Pediatr Infect Dis J. 2008;27(3):224–30.
Parvaneh N, Barlogis V, Alborzi A, Deswarte C, Boisson-Dupuis S, Migaud M, et al. Visceral leishmaniasis in two patients with IL-12p40 and IL-12Rbeta1 deficiencies. Pediatr Blood Cancer. 2017;64(6).
Magnani A, Brosselin P, Beaute J, de Vergnes N, Mouy R, Debre M, et al. Inflammatory manifestations in a single-center cohort of patients with chronic granulomatous disease. J Allergy Clin Immunol. 2014;134(3):655–62 e8.
Huang C, De Ravin SS, Paul AR, Heller T, Ho N, Wu Datta L, et al. Genetic risk for inflammatory bowel disease is a determinant of Crohn’s disease development in chronic granulomatous disease. Inflamm Bowel Dis. 2016;22(12):2794–801.
Dinauer MC. Inflammatory consequences of inherited disorders affecting neutrophil function. Blood. 2019;133(20):2130–9.
De Ravin SS, Naumann N, Cowen EW, Friend J, Hilligoss D, Marquesen M, et al. Chronic granulomatous disease as a risk factor for autoimmune disease. J Allergy Clin Immunol. 2008;122(6):1097–103.
Ben Abdallah Chabchoub R, Turki H, Mahfoudh A. Systemic lupus erythematosus in a boy with chronic granulomatous disease: case report and review of the literature. Arch Pediatr. 2014;21(12):1364–6.
Matute JD, Arias AA, Wright NA, Wrobel I, Waterhouse CC, Li XJ, et al. A new genetic subgroup of chronic granulomatous disease with autosomal recessive mutations in p40 phox and selective defects in neutrophil NADPH oxidase activity. Blood. 2009;114(15):3309–15.
Winkelstein JA, Marino MC, Johnston RB Jr, Boyle J, Curnutte J, Gallin JI, et al. Chronic granulomatous disease. Report on a national registry of 368 patients. Medicine (Baltimore). 2000;79(3):155–69.
Wolach B, Gavrieli R, de Boer M, van Leeuwen K, Berger-Achituv S, Stauber T, et al. Chronic granulomatous disease: clinical, functional, molecular, and genetic studies. The Israeli experience with 84 patients. Am J Hematol. 2017;92(1):28–36.
Kobayashi S, Murayama S, Takanashi S, Takahashi K, Miyatsuka S, Fujita T, et al. Clinical features and prognoses of 23 patients with chronic granulomatous disease followed for 21 years by a single hospital in Japan. Eur J Pediatr. 2008;167(12):1389–94.
de Oliveira-Junior EB, Zurro NB, Prando C, Cabral-Marques O, Pereira PV, Schimke LF, et al. Clinical and genotypic spectrum of chronic granulomatous disease in 71 Latin American patients: first report from the LASID registry. Pediatr Blood Cancer. 2015;62(12):2101–7.
Meshaal S, El Hawary R, Abd Elaziz D, Alkady R, Galal N, Boutros J, et al. Chronic granulomatous disease: review of a cohort of Egyptian patients. Allergol Immunopathol (Madr). 2015;43(3):279–85.
El Hawary R, Meshaal S, Nagy D, Fikry I, Alkady R, Abd Elaziz D, et al. Study of naive and memory cells in a cohort of Egyptian chronic granulomatous disease patients. J Recept Signal Transduct Res. 2015;35(5):423–8.
Fattahi F, Badalzadeh M, Sedighipour L, Movahedi M, Fazlollahi MR, Mansouri SD, et al. Inheritance pattern and clinical aspects of 93 Iranian patients with chronic granulomatous disease. J Clin Immunol. 2011;31(5):792–801.
Kulkarni M, Hule G, de Boer M, van Leeuwen K, Kambli P, Aluri J, et al. Approach to molecular diagnosis of chronic granulomatous disease (CGD): an experience from a large cohort of 90 Indian patients. J Clin Immunol. 2018;38(8):898–916.
Koker MY, Camcioglu Y, van Leeuwen K, Kilic SS, Barlan I, Yilmaz M, et al. Clinical, functional, and genetic characterization of chronic granulomatous disease in 89 Turkish patients. J Allergy Clin Immunol. 2013;132(5):1156–63 e5.
Condino-Neto A, Sorensen RU, Gomez Raccio AC, King A, Espinosa-Rosales FJ, Franco JL. Current state and future perspectives of the Latin American Society for Immunodeficiencies (LASID). Allergol Immunopathol (Madr). 2015;43(5):493–7.
Barese C, Copelli S, Zandomeni R, Oleastro M, Zelazko M, Rivas EM. X-linked chronic granulomatous disease: first report of mutations in patients of Argentina. J Pediatr Hematol Oncol. 2004;26(10):656–60.
Scheffler-Mendoza SC, Yamazaki-Nakashimada MA, Olaya-Vargas A, Morin-Contreras A, Juarez-Echenique JC, Alcantara-Ortigoza MA, et al. Successful stem cell transplantation in a child with chronic granulomatous disease associated with contiguous gene deletion syndrome and complicated by macrophage activation syndrome. Clin Immunol. 2014;154(2):112–5.
Venegas-Montoya E, Sorcia-Ramirez G, Scheffler-Mendoza S, Blancas-Galicia L, Bustamante J, Espinosa-Rosales F, et al. Use of corticosteroids as an alternative to surgical treatment for liver abscesses in chronic granulomatous disease. Pediatr Blood Cancer. 2016;63(12):2254–5.
Yamazaki-Nakashimada MA, Stiehm ER, Pietropaolo-Cienfuegos D, Hernandez-Bautista V, Espinosa-Rosales F. Corticosteroid therapy for refractory infections in chronic granulomatous disease: case reports and review of the literature. Ann Allergy Asthma Immunol. 2006;97(2):257–61.
Yamazaki-Nakashimada MA, Ramirez-Vargas N, De Rubens-Figueroa J. Chronic granulomatous disease associated with atypical Kawasaki disease. Pediatr Cardiol. 2008;29(1):169–71.
Alvarez-Cardona A, Rodriguez-Lozano AL, Blancas-Galicia L, Rivas-Larrauri FE, Yamazaki-Nakashimada MA. Intravenous immunoglobulin treatment for macrophage activation syndrome complicating chronic granulomatous disease. J Clin Immunol. 2012;32(2):207–11.
Berron-Ruiz L, Morin-Contreras A, Cano-Garcia V, Yamazaki-Nakashimada MA, Gomez-Tello H, Vargas-Camano ME, et al. Detection of inheritance pattern in thirty-three Mexican males with chronic granulomatous disease through 123 dihydrorhodamine assay. Allergol Immunopathol (Madr). 2014;42(6):580–5.
Bustamante-Ogando JC, Rivas-Larrauri F, Blancas-Galicia L, Otero-Mendoza F, Yamazaki-Nakashimada MA. Amphotericin B associated pulmonary complications in chronic granulomatous disease patients. Pediatr Blood Cancer. 2016;63(10):1871–2.
Ramirez-Uribe N, Hernandez-Martinez C, Lopez-Hernandez G, Perez-Garcia M, Ramirez-Sanchez E, Espinosa-Padilla SE, et al. Hematopoietic progenitors transplantation in a patient with chronic granulomatous disease in Mexico. Rev Alerg Mex. 2016;63(1):95–103.
Graham SM, Ahmed T, Amanullah F, Browning R, Cardenas V, Casenghi M, et al. Evaluation of tuberculosis diagnostics in children: 1. Proposed clinical case definitions for classification of intrathoracic tuberculosis disease. Consensus from an expert panel. J Infect Dis. 2012;205(Suppl 2):S199–208.
Gurunathan A, Boucher AA, Mark M, Prus KM, O’Brien MM, Breese EH, et al. Limitations of HLH-2004 criteria in distinguishing malignancy-associated hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer. 2018;65(12):e27400.
Kim HY, Kim HJ, Ki CS, Kim DW, Yoo KH, Kang ES. Rapid determination of chimerism status using dihydrorhodamine assay in a patient with X-linked chronic granulomatous disease following hematopoietic stem cell transplantation. Ann Lab Med. 2013;33(4):288–92.
Vowells SJ, Sekhsaria S, Malech HL, Shalit M, Fleisher TA. Flow cytometric analysis of the granulocyte respiratory burst: a comparison study of fluorescent probes. J Immunol Methods. 1995;178(1):89–97.
Kutlug S, Sensoy G, Birinci A, Saraymen B, Yavuz Koker M, Yiotaldiotaran A. Seven chronic granulomatous disease cases in a single-center experience and a review of the literature. Asian Pac J Allergy Immunol. 2018;36(1):35–41.
Gutierrez MJ, McSherry GD, Ishmael FT, Horwitz AA, Nino G. Residual NADPH oxidase activity and isolated lung involvement in X-linked chronic granulomatous disease. Case Rep Pediatr. 2012;2012:974561.
Wu J, Wang WF, Zhang YD, Chen TX. Clinical features and genetic analysis of 48 patients with chronic granulomatous disease in a single center study from Shanghai, China (2005-2015): new studies and a literature review. J Immunol Res. 2017;2017:8745254.
Zwerling A, Behr MA, Verma A, Brewer TF, Menzies D, Pai M. The BCG world atlas: a database of global BCG vaccination policies and practices. PLoS Med. 2011;8(3):e1001012.
Ohga S, Ikeuchi K, Kadoya R, Okada K, Miyazaki C, Suita S, et al. Intrapulmonary Mycobacterium avium infection as the first manifestation of chronic granulomatous disease. J Inf Secur. 1997;34(2):147–50.
Chusid MJ, Parrillo JE, Fauci AS. Chronic granulomatous disease. Diagnosis in a 27-year-old man with Mycobacterium fortuitum. JAMA. 1975;233(12):1295–6.
Allen DM, Chng HH. Disseminated Mycobacterium flavescens in a probable case of chronic granulomatous disease. J Inf Secur. 1993;26(1):83–6.
Marciano BE, Spalding C, Fitzgerald A, Mann D, Brown T, Osgood S, et al. Common severe infections in chronic granulomatous disease. Clin Infect Dis. 2015;60(8):1176–83.
El Kares R, Barbouche MR, Elloumi-Zghal H, Bejaoui M, Chemli J, Mellouli F, et al. Genetic and mutational heterogeneity of autosomal recessive chronic granulomatous disease in Tunisia. J Hum Genet. 2006;51(10):887–95.
Martire B, Rondelli R, Soresina A, Pignata C, Broccoletti T, Finocchi A, et al. Clinical features, long-term follow-up and outcome of a large cohort of patients with chronic granulomatous disease: an Italian multicenter study. Clin Immunol. 2008;126(2):155–64.
Patino PJ, Rae J, Noack D, Erickson R, Ding J, de Olarte DG, et al. Molecular characterization of autosomal recessive chronic granulomatous disease caused by a defect of the nicotinamide adenine dinucleotide phosphate (reduced form) oxidase component p67-phox. Blood. 1999;94(7):2505–14.
Noack D, Rae J, Cross AR, Munoz J, Salmen S, Mendoza JA, et al. Autosomal recessive chronic granulomatous disease caused by novel mutations in NCF-2, the gene encoding the p67-phox component of phagocyte NADPH oxidase. Hum Genet. 1999;105(5):460–7.
Beghin A, Comini M, Soresina A, Imberti L, Zucchi M, Plebani A, et al. Chronic granulomatous disease in children: a single center experience. Clin Immunol. 2018;188:12–9.
Movahedi M, Aghamohammadi A, Rezaei N, Shahnavaz N, Jandaghi AB, Farhoudi A, et al. Chronic granulomatous disease: a clinical survey of 41 patients from the Iranian primary immunodeficiency registry. Int Arch Allergy Immunol. 2004;134(3):253–9.
Rawat A, Vignesh P, Sharma A, Shandilya JK, Sharma M, Suri D, et al. Infection profile in chronic granulomatous disease: a 23-year experience from a tertiary care center in North India. J Clin Immunol. 2017;37(3):319–28.
Bassiri-Jahromi S, Doostkam A. Actinomyces and nocardia infections in chronic granulomatous disease. J Global Infect Dis. 2011;3(4):348–52.
Agudelo-Florez P, Prando-Andrade CC, Lopez JA, Costa-Carvalho BT, Quezada A, Espinosa FJ, et al. Chronic granulomatous disease in Latin American patients: clinical spectrum and molecular genetics. Pediatr Blood Cancer. 2006;46(2):243–52.
Yanir AD, Hanson IC, Shearer WT, Noroski LM, Forbes LR, Seeborg FO, et al. High incidence of autoimmune disease after hematopoietic stem cell transplantation for chronic granulomatous disease. Biol Blood Marrow Transplant. 2018;24(8):1643–50.
Valentine G, Thomas TA, Nguyen T, Lai YC. Chronic granulomatous disease presenting as hemophagocytic lymphohistiocytosis: a case report. Pediatrics. 2014;134(6):e1727–30.
Dunogue B, Pilmis B, Mahlaoui N, Elie C, Coignard-Biehler H, Amazzough K, et al. Chronic granulomatous disease in patients reaching adulthood: a nationwide study in France. Clin Infect Dis. 2017;64(6):767–75.
Acknowledgments
We thank the patients and their families for their collaboration.
Funding
The CONACYT-SALUD-2012-01-180910 and FUMENI A.C. supported this project. LBG, SEP, and MAYN have SNI-CONACYT fellowships. The protocol was approved (number 019/2011) at National Institute of Pediatrics Research and Ethics Committees. The Laboratory of Human Genetics of Infectious Diseases is supported by the Rockefeller University, The Foundation for Medical Research (FRM), the St. Giles Foundation, the French National Institute of Health and Medical Research (INSERM), Paris University, the Integrative Biology of Emerging Infectious Diseases Laboratory of Excellence (ANR-10-LABX-62-IBEID), and the French National Research Agency under the “Investments for the future” program (grant number ANR-10-IAHU-01), ANR-GENMSMD (grant number ANR-16-CE17-0005-01 for JB).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Research Involving Human Participants
Informed consent for participation in this study was obtained in accordance with local regulations, with approval from the IRB. The experiments described here were performed in Mexico and France, in accordance with local regulations.
Informed Consent
Written informed consent was obtained from the guardians of the pediatric patients or directly from adult patients.
Conflicts of Interest
The authors have no conflict of interest to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Blancas-Galicia, L., Santos-Chávez, E., Deswarte, C. et al. Genetic, Immunological, and Clinical Features of the First Mexican Cohort of Patients with Chronic Granulomatous Disease. J Clin Immunol 40, 475–493 (2020). https://doi.org/10.1007/s10875-020-00750-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-020-00750-5