Abstract
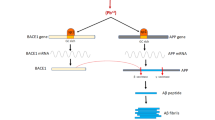
Exposure to the environmental pollutant lead (Pb) has been linked to Alzheimer’s disease (AD), in which mitochondrial dysfunction is a pathological consequence of neuronal degeneration. The toxicity of Pb in combination with β-amyloid peptides (1–40) and (25–35) causes selective death in neuronal cells. However, the precise mechanism through which Pb induces Alzheimer’s disease, particularly mitochondrial damage, is unknown. Changes in mitochondrial mass, membrane potential, mitochondrial complex activities, mitochondrial DNA and oxidative stress were examined in neuronal cells of human origin exposed to Pb and β-amyloid peptides (1–40) and (25–35) individually and in different combinations. The results showed depolarization of mitochondrial membrane potential, decrease in mitochondrial mass, ATP levels and mtDNA copy number in Pb and β-amyloid peptides (1–40) and (25–35) exposed cells. Also, significant reductions in the expression of mitochondrial electron transport chain (ETC) complex proteins (ATP5A, COXIV, UQCRC2, SDHB, NDUFS3), as well as down regulation of ETC complex gene expressions such as COXIV, ATP5F1 and NDUFS3 and antioxidant gene expressions like MnSOD and Gpx4 were observed in exposed cells. Furthermore, Pb and β-amyloid peptides exposure resulted in elevated mitochondrial malondialdehyde levels and a decrease in mitochondrial GSH levels. Our findings suggest that Pb toxicity could be one of the causative factors for the mitochondrial dysfunction and oxidative stress in Alzheimer’s disease progression.




Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- Pb:
-
Lead
- AD:
-
Alzheimer’s disease
- Aβ:
-
Amyloid-beta
- MDA:
-
Malondialdehyde
- ROS:
-
Reactive oxygen species
- ETC:
-
Electron transport chain
- MMP:
-
Mitochondrial membrane potential
- ATP:
-
Adenosine triphosphate
References
Ahamed M, Siddiqui MKJ (2007) Low level lead exposure and oxidative stress: current opinions. Clin Chim Acta 383:57–64. https://doi.org/10.1016/j.cca.2007.04.024
Ahmad F, Salahuddin M, Alamoudi W, Acharya S (2018) Dysfunction of cortical synapse-specific mitochondria in developing rats exposed to lead and its amelioration by ascorbate supplementation. NDT 14:813–824. https://doi.org/10.2147/NDT.S148248
Ahmad F, Haque S, Ravinayagam V et al (2020) Developmental lead (Pb)-induced deficits in redox and bioenergetic status of cerebellar synapses are ameliorated by ascorbate supplementation. Toxicology 440:152492. https://doi.org/10.1016/j.tox.2020.152492
Ayyalasomayajula N, Bandaru M, Dixit PK et al (2020) Inactivation of GAP-43 due to the depletion of cellular calcium by the Pb and amyloid peptide induced toxicity: An in vitro approach. Chem Biol Interact 316:108927. https://doi.org/10.1016/j.cbi.2019.108927
Bandaru LJM, Ayyalasomayajula N, Murumulla L et al (2022) Defective mitophagy and induction of apoptosis by the depleted levels of PINK1 and Parkin in Pb and β-amyloid peptide induced toxicity. Toxicol Mech Methods 1–10. https://doi.org/10.1080/15376516.2022.2054749
Baranowska-Bosiacka I, Gutowska I, Marchetti C et al (2011) Altered energy status of primary cerebellar granule neuronal cultures from rats exposed to lead in the pre- and neonatal period. Toxicology 280:24–32. https://doi.org/10.1016/j.tox.2010.11.004
Bazrgar M, Goudarzi I, Lashkarbolouki T, Elahdadi Salmani M (2015) Melatonin ameliorates oxidative damage induced by maternal lead exposure in rat pups. Physiol Behav 151:178–188. https://doi.org/10.1016/j.physbeh.2015.06.040
Bolin CM, Basha R, Cox D et al (2006) Exposure to lead and the developmental origin of oxidative DNA damage in the aging brain. FASEB J 20:788–790. https://doi.org/10.1096/fj.05-5091fje
Brieger K, Schiavone S, Jr M, Krause K (2012) Reactive oxygen species: from health to disease. Swiss Med Wkly. https://doi.org/10.4414/smw.2012.13659
Cha M-Y, Han S-H, Son SM et al (2012) Mitochondria-specific accumulation of amyloid β induces mitochondrial dysfunction leading to apoptotic cell death. PLoS One 7:e34929. https://doi.org/10.1371/journal.pone.0034929
Chen JX, Yan SD (2007) Amyloid-β-induced mitochondrial dysfunction. JAD 12:177–184. https://doi.org/10.3233/JAD-2007-12208
Chibowska K, Korbecki J, Gutowska I et al (2020) Pre- and neonatal exposure to lead (Pb) induces neuroinflammation in the forebrain cortex, Hippocampus and Cerebellum of rat pups. IJMS 21:1083. https://doi.org/10.3390/ijms21031083
Chu S, Li X, Sun N et al (2021) The combination of ultrafine carbon black and lead provokes cytotoxicity and apoptosis in mice lung fibroblasts through oxidative stress-activated mitochondrial pathways. Sci Total Environ 799:149420. https://doi.org/10.1016/j.scitotenv.2021.149420
Clay Montier LL, Deng JJ, Bai Y (2009) Number matters: control of mammalian mitochondrial DNA copy number. J Gen Genomics 36:125–131. https://doi.org/10.1016/S1673-8527(08)60099-5
Crouch PJ, Harding S-ME, White AR et al (2008) Mechanisms of Aβ mediated neurodegeneration in Alzheimer’s disease. Int J Biochem Cell Biol 40:181–198. https://doi.org/10.1016/j.biocel.2007.07.013
David DC, Hauptmann S, Scherping I et al (2005) Proteomic and functional analyses reveal a mitochondrial dysfunction in P301L Tau transgenic mice. J Biol Chem 280:23802–23814. https://doi.org/10.1074/jbc.M500356200
Delbarba A, Abate G, Prandelli C et al (2016) Mitochondrial alterations in peripheral mononuclear blood cells from Alzheimer’s disease and mild cognitive impairment patients. Oxidative Med Cell Longev 2016:1–11. https://doi.org/10.1155/2016/5923938
Du H, Guo L, Yan S et al (2010) Early deficits in synaptic mitochondria in an Alzheimer’s disease mouse model. Proc Natl Acad Sci 107:18670–18675. https://doi.org/10.1073/pnas.1006586107
Du H, Guo L, Yan SS (2012) Synaptic mitochondrial pathology in Alzheimer’s disease. Antioxid Redox Signal 16:1467–1475. https://doi.org/10.1089/ars.2011.4277
Du F, Yu Q, Yan S et al (2017) PINK1 signalling rescues amyloid pathology and mitochondrial dysfunction in Alzheimer’s disease. Brain 140:3233–3251. https://doi.org/10.1093/brain/awx258
Fukui H, Moraes CT (2008) The mitochondrial impairment, oxidative stress and neurodegeneration connection: reality or just an attractive hypothesis? Trends Neurosci 31:251–256. https://doi.org/10.1016/j.tins.2008.02.008
Guo C, Sun L, Chen X, Zhang D (2013) Oxidative stress, mitochondrial damage and neurodegenerative diseases****○. Neural Regen Res 8:12. https://doi.org/10.3969/j.issn.1673-5374.2013.21.009
Hansson Petersen CA, Alikhani N, Behbahani H et al (2008) The amyloid -peptide is imported into mitochondria via the TOM import machinery and localized to mitochondrial cristae. Proc Natl Acad Sci 105:13145–13150. https://doi.org/10.1073/pnas.0806192105
Hauptmann S, Scherping I, Dröse S et al (2009) Mitochondrial dysfunction: an early event in Alzheimer pathology accumulates with age in AD transgenic mice. Neurobiol Aging 30:1574–1586. https://doi.org/10.1016/j.neurobiolaging.2007.12.005
Hroudová J, Singh N, Fišar Z (2014) Mitochondrial dysfunctions in neurodegenerative diseases: relevance to Alzheimer’s disease. Biomed Res Int 2014:1–9. https://doi.org/10.1155/2014/175062
Huang ML-H, Chiang S, Kalinowski DS et al (2019) The role of the antioxidant response in mitochondrial dysfunction in degenerative diseases: cross-talk between antioxidant defense, autophagy, and apoptosis. Oxidative Med Cell Longev 2019:1–26. https://doi.org/10.1155/2019/6392763
Keller JN, Dimayuga E, Chen Q et al (2004) Autophagy, proteasomes, lipofuscin, and oxidative stress in the aging brain. Int J Biochem Cell Biol 36:2376–2391. https://doi.org/10.1016/j.biocel.2004.05.003
Leão LKR, Bittencourt LO, Oliveira ACA et al (2021) Lead-induced motor dysfunction is associated with oxidative stress, proteome modulation, and neurodegeneration in motor cortex of rats. Oxidative Med Cell Longev 2021:1–10. https://doi.org/10.1155/2021/5595047
Leuner K, Schütt T, Kurz C et al (2012) Mitochondrion-Derived Reactive Oxygen Species Lead to Enhanced Amyloid Beta Formation. Antioxid Redox Signal 16:1421–1433. https://doi.org/10.1089/ars.2011.4173
Levin R, Zilli Vieira CL, Rosenbaum MH et al (2021) The urban lead (Pb) burden in humans, animals and the natural environment. Environ Res 193:110377. https://doi.org/10.1016/j.envres.2020.110377
Li Y, Park J-S, Deng J-H, Bai Y (2006) Cytochrome c oxidase subunit IV is essential for assembly and respiratory function of the enzyme complex. J Bioenerg Biomembr 38:283–291. https://doi.org/10.1007/s10863-006-9052-z
Li R, Kou X, Geng H et al (2015) Mitochondrial damage: An important mechanism of ambient PM2.5 exposure-induced acute heart injury in rats. J Hazard Mater 287:392–401. https://doi.org/10.1016/j.jhazmat.2015.02.006
Liu G, Wang Z-K, Wang Z-Y et al (2016) Mitochondrial permeability transition and its regulatory components are implicated in apoptosis of primary cultures of rat proximal tubular cells exposed to lead. Arch Toxicol 90:1193–1209. https://doi.org/10.1007/s00204-015-1547-0
Ma L, Liu J-Y, Dong J-X et al (2017) Toxicity of Pb 2+ on rat liver mitochondria induced by oxidative stress and mitochondrial permeability transition. Toxicol Res 6:822–830. https://doi.org/10.1039/C7TX00204A
Maiti AK, Saha NC, Paul G (2010) Effect of lead on oxidative stress, Na+K+ATPase activity and mitochondrial electron transport chain activity of the brain of Clarias batrachus L. Bull Environ Contam Toxicol 84:672–676. https://doi.org/10.1007/s00128-010-9997-9
Maiti AK, Saha NC, More SS et al (2017) Neuroprotective efficacy of mitochondrial antioxidant mitoq in suppressing peroxynitrite-mediated mitochondrial dysfunction inflicted by lead toxicity in the rat brain. Neurotox Res 31:358–372. https://doi.org/10.1007/s12640-016-9692-7
Nazari M, Vajed-Samiei T, Torabi N et al (2022) The 40-Hz White Light-Emitting Diode (LED) improves the structure–function of the brain mitochondrial KATP channel and respiratory chain activities in amyloid beta toxicity. Mol Neurobiol 59:2424–2440. https://doi.org/10.1007/s12035-021-02681-7
Neelima A, Rajanna A, Bhanuprakash RG et al (2017) Deleterious effects of combination of lead and β-amyloid peptides in inducing apoptosis and altering cell cycle in human neuroblastoma cells. Interdiscip Toxicol 10:93–98. https://doi.org/10.1515/intox-2017-0015
Paradies G, Petrosillo G, Paradies V, Ruggiero FM (2010) Oxidative stress, mitochondrial bioenergetics, and cardiolipin in aging. Free Radic Biol Med 48:1286–1295. https://doi.org/10.1016/j.freeradbiomed.2010.02.020
Picone P, Nuzzo D, Caruana L et al (2014) Mitochondrial Dysfunction: Different Routes to Alzheimer’s Disease Therapy. Oxidative Med Cell Longev 2014:1–11. https://doi.org/10.1155/2014/780179
Qu M, Ni Y, Guo B et al (2020) Lycopene antagonizes lead toxicity by reducing mitochondrial oxidative damage and mitochondria-mediated apoptosis in cultured hippocampal neurons. MedComm 1:228–239. https://doi.org/10.1002/mco2.17
Rhein V, Song X, Wiesner A et al (2009) Amyloid- and tau synergistically impair the oxidative phosphorylation system in triple transgenic Alzheimer’s disease mice. Proc Natl Acad Sci 106:20057–20062. https://doi.org/10.1073/pnas.0905529106
Schmidt C, Lepsverdize E, Chi S et al (2008) Amyloid precursor protein and amyloid b-peptide bind to ATP synthase and regulate its activity at the surface of neural cells. Mol Psychiatry 953–69. https://doi.org/10.1038/sj.mp.4002077
Selkoe DJ (2002) Alzheimer’s disease is a synaptic failure. Science 298:789–791. https://doi.org/10.1126/science.1074069
Singh V, Gera R, Purohit M et al (2017) Fluorometric estimation of glutathione in cultured microglial cell lysate. BIO-PROTOCOL 7. https://doi.org/10.21769/BioProtoc.2304
Sousa CA, Soares EV (2014) Mitochondria are the main source and one of the targets of Pb (lead)-induced oxidative stress in the yeast Saccharomyces cerevisiae. Appl Microbiol Biotechnol 98:5153–5160. https://doi.org/10.1007/s00253-014-5631-9
Strużyñska L, Bubko I, Walski M, Rafałowska U (2001) Astroglial reaction during the early phase of acute lead toxicity in the adult rat brain. Toxicology 165:121–131. https://doi.org/10.1016/S0300-483X(01)00415-2
Suresh C, Johnson J, Mohan R, Chetty C (2012) Synergistic effects of amyloid peptides and lead on human neuroblastoma cells. Cell Mol Biol Lett 17. https://doi.org/10.2478/s11658-012-0018-3
Uttara B, Singh A, Zamboni P, Mahajan R (2009) Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. CN 7:65–74. https://doi.org/10.2174/157015909787602823
Wallin C, Sholts SB, Österlund N et al (2017) Alzheimer’s disease and cigarette smoke components: effects of nicotine, PAHs, and Cd(II), Cr(III), Pb(II), Pb(IV) ions on amyloid-β peptide aggregation. Sci Rep 7:14423. https://doi.org/10.1038/s41598-017-13759-5
Wang Y, Zhang M, Li Z et al (2019) Fine particulate matter induces mitochondrial dysfunction and oxidative stress in human SH-SY5Y cells. Chemosphere 218:577–588. https://doi.org/10.1016/j.chemosphere.2018.11.149
Wang L, Zheng Y, Zhang G et al (2021) Lead exposure induced inflammation in bursa of Fabricius of Japanese quail (C. japonica) via NF-κB pathway activation and Wnt/β-catenin signaling inhibition. J Inorg Biochem 224:111587. https://doi.org/10.1016/j.jinorgbio.2021.111587
Weinberg SE, Sena LA, Chandel NS (2015) Mitochondria in the Regulation of Innate and Adaptive Immunity. Immunity 42:406–417. https://doi.org/10.1016/j.immuni.2015.02.002
Ye F, Li X, Liu Y et al (2020) CypD deficiency confers neuroprotection against mitochondrial abnormality caused by lead in SH-SY5Y cell. Toxicol Lett 323:25–34. https://doi.org/10.1016/j.toxlet.2019.12.025
Yu Q, Fang D, Swerdlow RH et al (2016) Antioxidants rescue mitochondrial transport in differentiated Alzheimer’s disease trans-mitochondrial cybrid cells. JAD 54:679–690. https://doi.org/10.3233/JAD-160532
Acknowledgements
We thank the Indian Council of Medical Research (ICMR) for providing funds to carryout research and the University grants commission (UGC), Govt. of India for the award of the fellowship.
Funding
This work has been supported by the grant 58/57/2012-BMS funded by Indian Council of Medical Research (ICMR).
Author information
Authors and Affiliations
Contributions
The entire work was completed by Lakshmi Jaya Madhuri Bandaru, who also wrote the manuscript and did the data analysis. Experiments were assisted by Lokesh Murumulla. The manuscript was edited and corrected by Krishna Prasad D and Bindu Lasya Challa. The project was created, revised, and managed by Suresh Challa.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bandaru, L.J.M., Murumulla, L., C., B.L. et al. Exposure of combination of environmental pollutant, lead (Pb) and β-amyloid peptides causes mitochondrial dysfunction and oxidative stress in human neuronal cells. J Bioenerg Biomembr 55, 79–89 (2023). https://doi.org/10.1007/s10863-023-09956-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10863-023-09956-9