Abstract
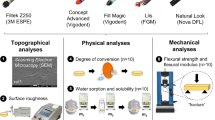
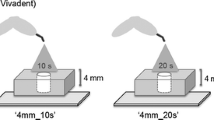
The aim of the present study was to characterize nanohybrid and nanofilled composites in terms of degree of conversion (DC), rate of cure (RC), microhardness (Vickers hardness number; VHN), depth of cure, and contraction stress (CS). Ceram.X® universal- A3, duo enamel E2, and duo dentin D3 composites were compared to Tetric EvoCeram® and FiltekTMSupreme XTE composites of equivalent dentin and enamel shades under a 40 s photopolymerization protocol. DC was measured by infrared spectroscopy, calculating RC from the kinetic curve. Top and bottom VHN were determined using a Vickers indenter, and bottom/top surface ratio (Vickers hardness ratio; VHR) calculated. CS vs. time was assessed by a universal testing machine and normalized for the specimen bonding area. All materials showed DC < 60%, Ceram.X® composites reaching higher values than the other composites of corresponding shades. RC at 5 s of photopolymerization was always higher than that at 10 s. All the Ceram.X® composites and the lighter-shaded Tetric EvoCeram® and FiltekTMSupreme XTE composites reached the RC plateau after 25 s, the remaining materials showed a slower kinetic trend. Tetric EvoCeram® and FiltekTMSupreme XTE composites displayed the softest and the hardest surfaces, respectively. Differently from darker-shaded materials, the universal and the three enamel-shaded composites resulted optimally cured (VHR > 80%). The tested composites differed in CS both during and after light cure, Tetric EvoCeram® and FiltekTMSupreme XTE composites displaying the highest and the lowest CS, respectively. Only the Ceram.X® universal-A3 reached a CS plateau value. The tested composites exhibited material-dependent chemo-mechanical properties. Increasing the curing time and/or reducing the composite layer thickness for dentin-shaded composites appears advisable.



Similar content being viewed by others
References
Sadowsky SJ. An overview of treatment considerations for esthetic restorations: a review of the literature. J Prosthet Dent. 2006;96:433–42.
Cramer NB, Stansbury JW, Bowman CN. Recent advances and developments in composite dental restorative materials. J Dent Res. 2011;90:402–16.
Pratap B, Gupta RK, Bhardwaj B, Nag M. Resin based restorative dental materials: characteristics and future perspectives. Jpn Dent Sci Rev. 2019;55:126–38.
Kim KH, Ong JL, Okuno O. The effect of filler loading and morphology on the mechanical properties of contemporary composites. J Prosthet Dent. 2002;87:642–9.
Randolph LD, Palin WM, Leloup G, Leprince JG. Filler characteristics of modern dental resin composites and their influence on physico-mechanical properties. Dent Mater. 2016;32:1586–99.
Heymann H, Sturdevant CM. Sturdevant’s art and science of operative dentistry. St. Louis, Mo: Elsevier/Mosby; 2013.
Kundie F, Azhari CH, Muchtar A, Ahmad ZA. Effects of filler size on the mechanical properties of polymer-filled dental composites: a review of recent developments. J Phys Sci. 2018;29:141–65.
Ferracane JL. Resin composite-state of the art. Dent Mater. 2011;27:29–38.
Loguercio AD, Lorini E, Weiss RV, Tori AP, Picinatto CC, Ribeiro NR, et al. A 12-month clinical evaluation of composite resins in class III restorations. J Adhes Dent. 2007;9:57–64.
Angerame D, De Biasi M. Do nanofilled/nanohybrid composites allow for better clinical performance of direct restorations than traditional microhybrid composites? A systematic review. Oper Dent. 2018;43:E191–209.
Blackham JT, Vandewalle KS, Lien W. Properties of hybrid resin composite systems containing prepolymerized filler particles. Oper Dent. 2009;34:697–702.
Thome T, Steagall W Jr., Tachibana A, Braga SR, Turbino ML. Influence of the distance of the curing light source and composite shade on hardness of two composites. J Appl Oral Sci. 2007;15:486–91.
Moore BK, Platt JA, Borges G, Chu TM, Katsilieri I. Depth of cure of dental resin composites: ISO 4049 depth and microhardness of types of materials and shades. Oper Dent. 2008;33:408–12.
Poggio C, Lombardini M, Gaviati S, Chiesa M. Evaluation of Vickers hardness and depth of cure of six composite resins photo-activated with different polymerization modes. J Conserv Dent. 2012;15:237–41.
Schneider LF, Pfeifer CS, Consani S, Prahl SA, Ferracane JL. Influence of photoinitiator type on the rate of polymerization, degree of conversion, hardness and yellowing of dental resin composites. Dent Mater. 2008;24:1169–77.
Rueggeberg FA, Caughman WF, Curtis JW Jr. Effect of light intensity and exposure duration on cure of resin composite. Oper Dent. 1994;19:26–32.
Al-Hiyasat AS, Darmani H, Milhem MM. Cytotoxicity evaluation of dental resin composites and their flowable derivatives. Clin Oral Investig. 2005;9:21–5.
Silikas N, Eliades G, Watts DC. Light intensity effects on resin-composite degree of conversion and shrinkage strain. Dent Mater. 2000;16:292–6.
Sideridou I, Tserki V, Papanastasiou G. Effect of chemical structure on degree of conversion in light-cured dimethacrylate-based dental resins. Biomaterials. 2002;23:1819–29.
Ribeiro BC, Boaventura JM, Brito-Goncalves J, Rastelli AN, Bagnato VS, Saad JR. Degree of conversion of nanofilled and microhybrid composite resins photo-activated by different generations of LEDs. J Appl Oral Sci. 2012;20:212–7.
Catelan A, Mainardi Mdo C, Soares GP, de Lima AF, Ambrosano GM, Lima DA, et al. Effect of light curing protocol on degree of conversion of composites. Acta Odontol Scand. 2014;72:898–902.
El-Nawawy M, Koraitim L, Abouelatta O, Hegazi H. Depth of cure and microhardness of nanofilled, packable and hybrid dental composite resins. Am J Biomed Eng. 2012;2:241–50.
Ferracane JL, Aday P, Matsumoto H, Marker VA. Relationship between shade and depth of cure for light-activated dental composite resins. Dent Mater. 1986;2:80–4.
Davidson-Kaban SS, Davidson CL, Feilzer AJ, de Gee AJ, Erdilek N. The effect of curing light variations on bulk curing and wall-to-wall quality of two types and various shades of resin composites. Dent Mater. 1997;13:344–52.
Leloup G, Holvoet PE, Bebelman S, Devaux J. Raman scattering determination of the depth of cure of light-activated composites: influence of different clinically relevant parameters. J Oral Rehabil. 2002;29:510–5.
ISO 4049:2019 (5.) Dentistry—polymer-based filling, restorative and luting materials; 7.10 depth of cure, Class 2 materials excluding luting materials. International Organization for Standardization Geneva, Switzerland (2019).
Flury S, Hayoz S, Peutzfeldt A, Husler J, Lussi A. Depth of cure of resin composites: is the ISO 4049 method suitable for bulk fill materials? Dent Mater. 2012;28:521–8.
Abed YA, Sabry HA, Alrobeigy NA. Degree of conversion and surface hardness of bulk-fill composite versus incremental-fill composite. Tanta Dent J. 2015;12:71–80.
Mandikos MN, McGivney GP, Davis E, Bush PJ, Carter JM. A comparison of the wear resistance and hardness of indirect composite resins. J Prosthet Dent. 2001;85:386–95.
Braga RR, Ferracane JL. Contraction stress related to degree of conversion and reaction kinetics. J Dent Res. 2002;81:114–8.
Braga RR, Ballester RY, Ferracane JL. Factors involved in the development of polymerization shrinkage stress in resin-composites: a systematic review. Dent Mater. 2005;21:962–70.
Yu P, Yap A, Wang XY. Degree of conversion and polymerization shrinkage of bulk-fill resin-based composites. Oper Dent. 2017;42:82–9.
Ferracane JL, Hilton TJ. Polymerization stress-is it clinically meaningful? Dent Mater. 2016;32:1–10.
Gajewski V, Pfeifer C, Fróes-Salgado N, Boaro L, Braga R. Monomers used in resin composites: degree of conversion, mechanical properties and water sorption/solubility. Braz Dent J. 2012;23:508–14.
Van Landuyt KL, Snauweart J, De Munck J, Peumans M, Yoshida Y, Poitevin A, et al. Systematic review of the chemical composition of contemporary dental adhesives. Biomaterials. 2007;28:3757–85.
AlShaafi M. Factors affecting polymerization of resin-based composite: a literature review. Saudi Dent J. 2017;29:48–58.
Fontes A, Di Mauro E, Dall’Antonia L, Sano W. Study of the influence of pigments in the polymerization and mechanical performance of commercial dental composites. Rev Odontol Bras Cent. 2012;21:468–72.
Mahn E. Clinical criteria for the successful curing of composite materials. Rev Clin Periodoncia Implantol Rehabil Oral. 2013;6:148–53.
Manhart J, Kunzelmann KH, Chen HY, Hickel R. Mechanical properties of new composite restorative materials. J Biomed Mater Res. 2000;53:353–61.
Ruyter IE, Oysaed H. Conversion in different depths of ultraviolet and visible light activated composite materials. Acta Odontol Scand. 1982;40:179–92.
Okte Z, Villalta P, Garcia-Godoy F, Garcia-Godoy F Jr., Murray P. Effect of curing time and light curing systems on the surface hardness of compomers. Oper Dent. 2005;30:540–5.
Bouschlicher M, Rueggeberg F, Wilson B. Correlation of bottom-to-top surface microhardness and conversion ratios for a variety of resin composite compositions. Oper Dent. 2004;29:698–704.
Habib E, Wang R, Wang Y, Zhu M, Zhu X. Inorganic fillers for dental resin composites: present and future. ACS Biomater Sci Eng. 2016;2:1–11.
Tagtekin D, Yanikoglu F, Bozkurt F, Kologlu B, Sur H. Selected characteristics of an Ormocer and a conventional hybrid resin composite. Dent Mater. 2004;20:487–97.
Poggio C, Viola M, Mirando M, Chiesa M, Beltrami R, Colomo M. Microhardness af different esthetic restorative materials: evaluation and comparison after exposure to acidic drink. Dent Res J. 2018;15:166–72.
Lu H, Lee Y, Oguri M, JM P. Properties of a dental resin composite with a spherical inorganic filler. Oper Dent. 2006;31:734–40.
Shah P, Stansbury J. Role of filler and functional group conversion in the evolution of properties in polymeric dental restoratives. Dent Mater. 2014;30:586–93.
Satterthwaite J, Maisuria A, Vogel K, Watts D. Effect of resin-composite filler particle size and shape on shrinkage-stress. Dent Mater. 2012;28:609–14.
Kleverlaan CJ, Feilzer AJ. Polymerization shrinkage and contraction stress of dental resin composites. Dent Mater. 2005;21:1150–7.
Lu H, Stansbury JW, Bowman CN. Towards the elucidation of shrinkage stress development and relaxation in dental composites. Dent Mater. 2004;20:979–86.
Goncalves F, Kawano Y, Braga RR. Contraction stress related to composite inorganic content. Dent Mater. 2010;26:704–9.
Marchesi G, Breschi L, Antoniolli F, Di Lenarda R, Ferracane J, Cadenaro M. Contraction stress of low-shrinkage composite materials assessed with different testing systems. Dent Mater. 2010;26:947–53.
Fronza BM, Rueggeberg FA, Braga RR, Mogilevych B, Soares LE, Martin AA, et al. Monomer conversion, microhardness, internal marginal adaptation, and shrinkage stress of bulk-fill resin composites. Dent Mater. 2015;31:1542–51.
Kannurpatti AR, Anderson KJ, Anseth JW, Bowman CN. Use of “living” radical polymerizations to study the structural evolution and properties of highly crosslinked polymer networks. J Polym Sci B Polym Phys. 1997;35:2297–307.
Acknowledgements
The authors would like to thank the Laser Laboratory of Elettra Sincrotrone Trieste (Trieste, Italy) for the curing lights’ output and maximum emitted wavelength measurement. The authors declare that they do not have any financial interest in the companies whose materials are included in this article.
Funding
The study was self-funded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fanfoni, L., De Biasi, M., Antollovich, G. et al. Evaluation of degree of conversion, rate of cure, microhardness, depth of cure, and contraction stress of new nanohybrid composites containing pre-polymerized spherical filler. J Mater Sci: Mater Med 31, 127 (2020). https://doi.org/10.1007/s10856-020-06464-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-020-06464-9