Abstract
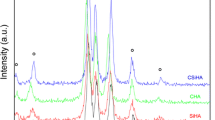
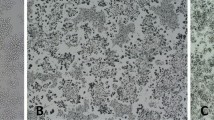
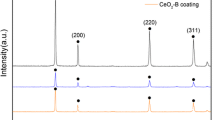
Inflammatory effects are significant elements of the immune response to biomaterials. Previously, we reported inflammatory effects in response to dicalcium silicate (Ca2SiO4, C2S) particles. However, the immunological effects of C2S coatings have not been studied. C2S often used as coatings materials in orthopedic and dentistry applications. It may have different effect from C2S particles. Further, it remains unclear whether C2S coating is equally biocompatible as 45S5 coating. The aim of this study was to test the cytotoxicity and pro-inflammatory effects of C2S coating on RAW 264.7 macrophages. C2S and 45S5 coatings were characterized using scanning electron microscopy (SEM), atomic force microscopy (AFM), energy dispersive analysis (EDS) and X-ray diffraction (XRD). inductively coupled plasma optical emission spectroscopy (ICP-OES) was used to detect ionic concentrations after soaking coated discs in medium. The cytotoxicity of C2S and 45S5 coatings against RAW 264.7 macrophages was measured using the LDH Cytotoxicity Assay Kit, Cell Counting Kit-8 (CCK-8) assays and flow cytometry for apoptosis assays. The gene and protein expression of TNF-α, IL-6 and IL-1β were detected using RT-q PCR and ELISA, respectively. The tested coating materials are not cytotoxic to macrophages. The C2S-coated surface stimulated macrophages to express pro-inflammatory mediators, such as TNF-α, IL-6 and IL-1β, and C2S coating caused less IL-6 but greater IL-1β production than the 45S5 coating. C2S coating have no cytotoxicity when directly cultured with macrophages. C2S and 45S5 coatings both have the potential to induce pro-inflammatory effects, and the biocompatibility of C2S is similar to that of 45S5.






Similar content being viewed by others
References
Wu C, Chen Z, Yi D, Chang J, Xiao Y. Multidirectional effects of Sr-, Mg-, and Si-containing bioceramic coatings with high bonding strength on inflammation, osteoclastogenesis, and osteogenesis. ACS Appl Mater Interfaces. 2014;6(6):4264–76.
Kokubo T. Surface chemistry of bioactive glass-ceramics. J Non Cryst Solids. 1990;120:138–51.
Sun J, Li J, Liu X, Wei L, Wang G, Meng F. Proliferation and gene expression of osteoblasts cultured in DMEM containing the ionic products of dicalcium silicate coating. Biomed Pharmacother. 2009;63(9):650–7.
Liu XY, Xie YT, Ding CX, Chu PK. Early apatite deposition and osteoblasts growth on plasma sprayed dicalcium silicate coating. J Biomed Mater Res. 2005;74A:356–65.
Gandolfi MG, Ciapetti G, Perut F, Taddei P, Modena E, Rossi PL, Prati C. Biomimetic calcium-silicate cements aged in simulated body solutions. Osteoblast response and analyses of apatite coating. J Appl Biomater Biomech. 2009;7(3):160–70.
Gandolfi MG, Ciapetti G, Taddei P, Perut F, Tinti A, Cardoso MV, Van Meerbeek B, Prati C. Apatite formation on bioactive calcium-silicate cements for dentistry affects surface topography and human marrow stromal cells proliferation. Dent Mater. 2010;26(10):974–92.
Wu BC, Wei CK, Hsueh NS, Ding SJ. Comparative cell attachment, cytotoxicity and antibacterial activity of radiopaque dicalcium silicate cement and white-coloured mineral trioxide aggregate. Int Endod J. 2015;48(3):268–76.
Chiang TY, Ding SJ. Comparative physicochemical and biocompatible properties of radiopaque dicalcium silicate cement and mineral trioxide aggregate. Journal of Endod. 2010;36(10):1683–7.
Gou Z, Chang J, Zhai W, Wang J. Study on the self-setting property and the in vitro bioactivity of beta-Ca2SiO4. J Biomed Mater Res B. 2005;73(2):244–51.
Liu X, Tao S, Ding C. Bioactivity of plasma sprayed dicalcium silicate coatings. Biomaterials. 2002;23(3):963–8.
Hirakawa K, Jacobs JJ, Urban R, Saito T. Mechanisms of failure of total hip replacements: lessons learned from retrieval studies. Clin Orthop Relat Res. 2004;420:10–7.
Pazár B, Ea HK, Narayan S, Kolly L, Bagnoud N, Chobaz V, Roger T, Lioté F, So A, Busso N. Basic calcium phosphate crystals induce monocyte/macrophage IL-1β secretion through the NLRP3 inflammasome in vitro. J Immunol. 2011;186(4):2495–502.
Ion R, Stoian AB, Dumitriu C, Grigorescu S, Mazare A, Cimpean A, Demetrescu I, Schmuki P.Nanochannels formed on TiZr alloy improve biological response. Acta biomateriala. 2015, 16, S1742-7061(15)00282-2.
Velard F, Laurent-Maquin D, Braux J, Guillaume C, Bouthors S, Jallot E, Nedelec JM, Belaaouaj A, Laquerriere P. The effect of zinc on hydroxyapatite-mediated activation of human polymorphonuclear neutrophils and bone implant-associated acute inflammation. Biomaterials. 2010;31(8):2001–9.
Kaufman AM, Alabre CI, Rubash HE, Shanbhag AS. Human macrophage response to UHMWPE, TiAlV, CoCr, and alumina particles: analysis of multiple cytokines using protein arrays. J Biomed Mater Res A. 2008;84(2):464–74.
Jones JR, Hench LL. Effect of surfactant concentration and composition on the structure and properties of sol–gel-derived bioactive glass foam scaffolds for tissue engineering. J Biomed Mater Res B. 2004;68(1):36–44.
Laquerriere P, Grandjean-Laquerriere A, Jallot E, Balossier G, Frayssinet P, Guenounou M. Importance of hydroxyapatite particles characteristics on cytokines production by human monocytes in vitro. Biomaterials. 2003;24(16):2739–47.
Buache E, Velard F, Bauden E, Guillaume C, Jallot E, Nedelec JM, Laurent-Maquin D, Laquerriere P. Effect of strontium-substituted biphasic calcium phosphate on inflammatory mediators production by human monocytes. Acta Biomater. 2012;8(8):3113–9.
Laquerriere P, Grandjean-Laquerriere A, Addadi-Rebbah S, Jallot E, Lauernt-Maquin D, Frayssinet P. MMP-2, MMP-9 and their inhibitors TIMP-2 and TIMP-1 production by human monocytes in vitro in presence of differents hydroxyapatite: importance of particle physical characteristics. Biomaterials. 2004;25(13):2515–24.
Liangjiao C, Ping Z, Ruoyu L, Yanli Z, Ting S, Yanjun L, Longquan S. Potential proinflammatory and osteogenic effects of dicalcium silicate particles in vitro. J Mech Behav Biomed Mater. 2014;44:10–22.
Varanasi VG, Saiz E, Loomer PM, Ancheta B, Uritani N, Ho SP, Tomsia AP, Marshall SJ, Marshall GW. Enhanced osteocalcin expression by osteoblast-like cells (MC3T3-E1) exposed to bioactive coating glass (SiO2–CaO–P2O5–MgO–K2O–Na2O system) ions. Acta Biomater. 2009;5(9):3536–47.
Newman SD, Lotfibakhshaiesh N, O’Donnell M, Walboomers XF, Horwood N, Jansen JA, Amis AA, Cobb JP, Stevens MM. Enhanced osseous implant fixation with strontium-substituted bioactive glass coating. Tissue Eng A. 2014;20(13–14):1850–7.
Eberhard J, Reimers N, Dommisch H, Hacker J, Freitag S, Acil Y, Albers HK, Jepsen S. The effect of the topical administration of bioactive glass on inflammatory markers of human experimental gingivitis. Biomaterials. 2005;26(13):1545–51.
Day RM, Boccaccini AR. Effect of particulate bioactive glasses on human macrophages and monocytes in vitro. J Biomed Mater Res A. 2005;73(1):73–9.
Bosetti M, Hench L, Cannas M. Interaction of bioactive glasses with peritoneal macrophages and monocytes in vitro. J Biomed Mater Res. 2002;60(1):79–85.
Li J, Wei L, Sun J, Guan G. Effect of ionic products of dicalcium silicate coating on osteoblast differentiation and collagen production via TGF-β1 pathway. J Biomater Appl. 2013;7(5):595–604.
Cacciotti I, Lombardi M, Bianco A, Ravaglioli A, Montanaro L. Sol-gel derived 45S5 bioglass: synthesis, microstructural evolution and thermal behaviour. J Mater Sci Mater Med. 2012;23(8):1849–66.
Velasquez P, Luklinska ZB, Meseguer-Olmo L, de Val Mate-Sanchez JE, Delgado-Ruiz RA, Calvo-Guirado JL, Ramirez-Fernandez MP, de Aza PN. αTCP ceramic doped with dicalcium silicate for bone regeneration applications prepared by powder metallurgy method: in vitro and in vivo studies. J Biomed Mater Res A. 2013;101(7):1943–54.
Meseguer-Olmo L, Aznar-Cervantes S, Mazón P, De Aza PN. “In vitro” behavior of adult mesenchymal stem cells of human bone marrow origin seeded on a novel bioactive ceramics in the Ca2SiO4-Ca3(PO4)2 system. J Mater Sci Mater Med. 2012;23(12):3003–14.
Nelson GM, Nychka JA, McDonald AG. Structure, phases, and mechanical response of Ti-alloy bioactive glass composite coatings. Mater Sci Eng C Mater Biol Appl. 2014;36:261–76.
Khor KA, Gu YW, Pan D, Cheang P. Microstructure and mechanical properties of plasma sprayed HA/YSZ/Ti–6Al–4V composite coatings. Biomaterials. 2004;25(18):4009–17.
Kitsugi T, Nakamura T, Oka M, Senaha Y, Goto T, Shibuya T. Bone-bonding behavior of plasma-sprayed coatings of BioglassR, AW-glass ceramic, and tricalcium phosphate on titanium alloy. J Biomed Mater Res. 1996;30(2):261–9.
Scislowska-Czarnecka A, Menaszek E, Szaraniec B, Kolaczkowska E. Ceramic modifications of porous titanium: effects on macrophage activation. Tissue Cell. 2012;44(6):391–400.
Curran JM, Gallagher JA, Hunt JA. The inflammatory potential of biphasic calcium phosphate granules in osteoblast/macrophage coculture. Biomaterials. 2005;26(26):5313–20.
de Aza PN, Luklinska ZB, de Val Mate-Sanchez JE, Calvo-Guirado JL. Biodegradation process of α-tricalcium phosphate and α-tricalcium phosphate solid solution bioceramics in vivo: a comparative study. Microsc Microanal. 2013;19(5):1350–7.
Jakobsen SS, Larsen A, Stoltenberg M, Bruun JM, Soballe K. Hydroxyapatite coatings did not increase TGF-beta and BMP-2 secretion in murine J774A.1 macrophages, but induced a pro-inflammatory cytokine response. J Biomater Sci Polym Ed. 2009;20(4):455–65.
Ding H, Zhu Z, Tang T, Yu D, Yu B, Dai K. Comparison of the cytotoxic and inflammatory responses of titanium particles with different methods for endotoxin removal in RAW264.7 macrophages. J Mater Sci Mater Med. 2012;23(4):1055–62.
Li HW, Sun JY. Effects of dicalcium silicate coating ionic dissolution products on human mesenchymal stem-cell proliferation and osteogenic differentiation. J Int Med Res. 2011;39(1):112–28.
Sun J, Wei L, Liu X, Li J, Li B, Wang G, Meng F. Influences of ionic dissolution products of dicalcium silicate coating on osteoblastic proliferation, differentiation and gene expression. Acta Biomater. 2009;5(4):1284–93.
Lee TM, Tsai RS, Chang E, Yang CY, Yang MR. Biological responses of neonatal rat calvarial osteoblasts on plasma-sprayed HA/ZrO2 composite coating. J Mater Sci Mater Med. 2002;13(3):281–7.
van Oirschot BA, Alghamdi HS, Närhi TO, Anil S, Al Farraj Aldosari A, van den Beucken JJ, Jansen JA. In vivo evaluation of bioactive glass-based coatings on dental implants in a dog implantation model. Clin Oral Implants Res. 2014;25(1):21–8.
Li J, Wei L, Sun J, Guan G. Effect of ionic products of dicalcium silicate coating on osteoblast differentiation and collagen production via TGF-β1 pathway. J Biomater Appl. 2013;27(5):595–604.
Liu X, Ding C, Chu PK. Mechanism of apatite formation on wollastonite coatings in simulated body fluids. Biomaterials. 2004;25(10):1755–61.
De Aza PN, García-Bernal D, Cragnolini F, Velasquez P, Meseguer-Olmo L. The effects of Ca2SiO4-Ca3(PO4)2 ceramics on adult human mesenchymal stem cell viability, adhesion, proliferation, differentiation and function. Mater Sci Eng C Mater Biol Appl. 2013;33(7):4009–20.
Li J, Wei L, Sun J, Guan G. Effect of ionic products of dicalcium silicate coating on osteoblast differentiation and collagen production via TGF-β1 pathway. J Biomater Appl. 2013;27(5):595–604.
Varanasi VG, Owyoung JB, Saiz E, Marshall SJ, Marshall GW, Loomer PM. The ionic products of bioactive glass particle dissolution enhance periodontal ligament fibroblast osteocalcin expression and enhance early mineralized tissue development. J Biomed Mater Res A. 2011;98(2):177–84.
Silva JM, Zupancic E, Vandermeulen G, Oliveira VG, Salgado A, Videira M, Gaspar M, Graca L, Préat V, Florindo HF. In vivo delivery of peptides and Toll-like receptor ligands by mannose-functionalized polymeric nanoparticles induces prophylactic and therapeutic anti-tumor immune responses in a melanoma model. J Control Release. 2015;198(28):91–103.
Mano SS, Kanehira K, Taniguchi A. Comparison of cellular uptake and inflammatory response via toll-like receptor 4 to lipopolysaccharide and titanium dioxide nanoparticles. Int J Mol Sci. 2013;14(7):13154–70.
Pearl JI, Ma T, Irani AR, Huang Z, Robinson WH, Smith RL, Goodman SB. Role of the Toll-like receptor pathway in the recognition of orthopedic implant wear-debris particles. Biomaterials. 2011;32(24):5535–42.
Landgraeber S, Jäger M, Jacobs JJ, Hallab NJ. The pathology of orthopedic implant failure is mediated by innate immune system cytokines. Mediators Inflamm. 2014;2014:185150.
Refai AK, Textor M, Brunette DM, Waterfield JD. Effect of titanium surface topography on macrophage activation and secretion of proinflammatory cytokines and chemokines. J Biomed Mater Res A. 2004;70(2):194–205.
Kai Soo Tana. Li Qiana, Roy Rosadob, Patrick M. Flooda, c, d, Lyndon F. Cooper. The role of titanium surface topography on J774A.1 macrophage inflammatory cytokines and nitric oxide production. Biomaterials. 2006;27(30):5170–7.
Hamlet Stephen, Ivanovski Saso. Inflammatory cytokine response to titanium chemical composition and nanoscale calcium phosphate surface modification. Acta Biomater. 2011;7(5):2345–53.
Moura CC, Machado JR, Silva MV, Rodrigues DB, Zanetta-Barbosa D, Jimbo R, Tovar N, Coelho PG. Evaluation of human polymorphonuclear behavior on textured titanium and calcium-phosphate coated surfaces. Biomed Mater. 2013;8(3):035010.
Scislowska-Czarnecka A, Menaszek E, Szaraniec B, Kolaczkowska E. Ceramic modifications of porous titanium: effects on macrophage activation. Tissue Cell. 2012;44(6):391–400.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (31070857 and 50973045) and the Project on the Integration of Industry, Education and Research of Guangdong Province, China (2012B091000147). This work was also supported by Medical Research Foundation of Guangdong Province (A2015132) and Scientific research projects of Guangzhou Medical University (2015C43).
Author information
Authors and Affiliations
Corresponding author
Additional information
Liangjiao Chen and Yanli Zhang have contributed equally to this work and should be considered co-first authors.
Rights and permissions
About this article
Cite this article
Chen, L., Zhang, Y., Liu, J. et al. Exposure of the murine RAW 264.7 macrophage cell line to dicalcium silicate coating: assessment of cytotoxicity and pro-inflammatory effects. J Mater Sci: Mater Med 27, 59 (2016). https://doi.org/10.1007/s10856-016-5668-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-016-5668-7