Abstract
Background
Arterial invasive monitoring is the most common method in the USA for hemodynamic monitoring during atrial fibrillation (AF) ablation. Although studies have shown favorable comparison between non-invasive and invasive hemodynamic monitoring (IHM) in non-cardiac procedures under general anesthesia, limited data is available for complex cardiac procedures such as AF ablation in the USA. With progressive improvement in AF ablation procedural safety, particularly with routine use of intracardiac echocardiography (ICE) to monitor for pericardial effusion, it is unclear if invasive hemodynamic monitoring provides any advantage over non-invasive methods. Therefore, the purpose of this study is to determine whether noninvasive hemodynamic monitoring is non-inferior to invasive hemodynamic monitoring during AF ablation under general anesthesia in patients without major cardiac structural abnormality.
Methods
A multi-center retrospective data of AF ablation from July 2019 to December 2020 was extracted. A total of three hundred and sixty-two patients (362) were included, which were divided into group A (non-invasive hemodynamic monitoring) and group B (invasive hemodynamic monitoring). The primary outcome was to compare procedural safety between the two groups.
Results
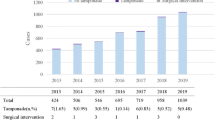
Out of 362 patients, 184 (51%) received non-invasive and 178 (49%) received invasive hemodynamic monitoring with similar baseline characteristics. There was no significant difference between the two groups in complication rates (groin hematoma, pericardial effusion, cardiac tamponade). Mean procedure time was longer in group B with 3.35% arterial site discomfort. Urgent arterial access was required in only 1 patient in group A.
Conclusion
This retrospective multicenter study strongly suggests that catheter ablation for atrial fibrillation under general anesthesia can be safely performed with noninvasive hemodynamic monitoring without requiring arterial access, with potential benefit in procedural duration and cost.
Similar content being viewed by others
References
Calkins H, Hindricks G, Cappato R, et al. 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm. 2017;14:e275–444.
Hosseini SM, Rozen G, Saleh A, et al. Catheter ablation for cardiac arrhythmias: utilization and in-hospital complications, 2000 to 2013. JACC Clin Electrophysiol. 2017;3:1240–8.
Mansour M, Karst E, Heist EK, et al. The impact of first procedure success rate on the economics of atrial fibrillation ablation. JACC: Clin Electrophysiol. 2017;3:129–38.
Cheung JW, Yeo I, Cheng EP, et al. Inpatient hospital procedural volume and outcomes following catheter ablation of atrial fibrillation. J Cardiovasc Electrophysiol. 2020;31:1908–19.
Wazni OM, Dandamudi G, Sood N, et al. Cryoballoon ablation as initial therapy for atrial fibrillation. N Engl J Med. 2021;384:316–24.
Andrade JG, Wells GA, Deyell MW, et al. Cryoablation or drug therapy for initial treatment of atrial fibrillation. N Engl J Med. 2020;384:305–15.
Gerstein NS, Young A, Schulman PM, et al. Sedation in the electrophysiology laboratory: a multidisciplinary review. J Am Heart Assoc. 2016;5:e003629.
Sha Q, Velleca M, Goldstein L, et al. The value of intracardiac echocardiography in catheter ablation of cardiac arrhythmias: insights from recent clinical studies. EMJ Cardiol. 2020;8:2–9.
Muthalaly RG, John RM, Schaeffer B, et al. Temporal trends in safety and complication rates of catheter ablation for atrial fibrillation. J Cardiovasc Electrophysiol. 2018;29:854–60.
Schmidt M, Daccarett M, Marschang H, et al. Intracardiac echocardiography improves procedural efficiency during cryoballoon ablation for atrial fibrillation: a pilot study. J Cardiovasc Electrophysiol. 2010;21:1202–7.
Marrouche NF, Brachmann J, Andresen D, et al. Catheter ablation for atrial fibrillation with heart failure. N Engl J Med. 2018;378:417–27.
Kautzner J, Peichl P, Sramko M, et al. Catheter ablation of atrial fibrillation in elderly population. J Geriatr Cardiol. 2017;14:563–8.
Ad N, Henry L, Hunt S, et al. Should surgical ablation for atrial fibrillation be performed in patients with a significantly enlarged left atrium? J Thorac Cardiovasc Surg. 2014;147:236–41.
Dinshaw L, Münkler P, Schäffer B, et al. Ablation of atrial fibrillation in patients with hypertrophic cardiomyopathy: treatment strategy, characteristics of consecutive atrial tachycardia and long-term outcome. J Am Heart Assoc. 2021;10:e017451.
Kirov MY, Kuzkov VV, Molnar Z. Perioperative haemodynamic therapy. Curr Opin Crit Care. 2010;16:384–92.
Aldhoon B, Wichterle D, Peichl P, et al. Complications of catheter ablation for atrial fibrillation in a high-volume centre with the use of intracardiac echocardiography. EP Europace. 2012;15:24–32.
Wynn GJ, Haq I, Hung J, et al. Improving safety in catheter ablation for atrial fibrillation: a prospective study of the use of ultrasound to guide vascular access. J Cardiovasc Electrophysiol. 2014;25:680–5.
Sharma PS, Padala SK, Gunda S, et al. Vascular complications during catheter ablation of cardiac arrhythmias: a comparison between vascular ultrasound guided access and conventional vascular access. J Cardiovasc Electrophysiol. 2016;27:1160–6.
Wang TKM, Wang MTM, Martin A. Meta-analysis of ultrasound-guided vs conventional vascular access for cardiac electrophysiology procedures. J Arrhythm. 2019;35:858–62.
Tanioku T, Yoshida A, Aratani Y, et al. Validation of noninvasive continuous arterial pressure measurement by ClearSight System™ during induction of anesthesia for cardiovascular surgery. BMC Anesthesiol. 2020;20:176.
Broch O, Renner J, Gruenewald M, et al. A comparison of the Nexfin® and transcardiopulmonary thermodilution to estimate cardiac output during coronary artery surgery. Anaesthesia. 2012;67:377–83.
Ameloot K, Van De Vijver K, Broch O, et al. Nexfin noninvasive continuous hemodynamic monitoring: validation against continuous pulse contour and intermittent transpulmonary thermodilution derived cardiac output in critically ill patients. ScientificWorldJournal. 2013;2013:519080.
Martina JR, Westerhof BE, van Goudoever J, et al. Noninvasive continuous arterial blood pressure monitoring with Nexfin®. Anesthesiology. 2012;116:1092–103.
Maggi R, Viscardi V, Furukawa T, et al. Non-invasive continuous blood pressure monitoring of tachycardic episodes during interventional electrophysiology. Europace. 2010;12:1616–22.
Berkelmans GFN, Kuipers S, Westerhof BE, et al. Comparing volume-clamp method and intra-arterial blood pressure measurements in patients with atrial fibrillation admitted to the intensive or medium care unit. J Clin Monit Comput. 2018;32:439–46.
Pagonas N, Schmidt S, Eysel J, et al. Impact of atrial fibrillation on the accuracy of oscillometric blood pressure monitoring. Hypertension. 2013;62:579–84.
Maass SW, Roekaerts PM, Lancé MD. Cardiac output measurement by bioimpedance and noninvasive pulse contour analysis compared with the continuous pulmonary artery thermodilution technique. J Cardiothorac Vasc Anesth. 2014;28:534–9.
SpernaWeiland NH, de Wever JW, van Duivenvoorde Y, et al. Agreement between ccNexfin CO-trek cardiac output and intermittent cold-bolus pulmonary thermodilution in a prospective multicenter study. Minerva Anestesiol. 2018;84:473–80.
Bollmann A, Ueberham L, Schuler E, et al. Cardiac tamponade in catheter ablation of atrial fibrillation: German-wide analysis of 21 141 procedures in the Helios atrial fibrillation ablation registry (SAFER). EP Europace. 2018;20:1944–51.
Murakawa Y, Yamane T, Goya M, et al. Incidence and predictors of pericardial effusion as an early complication of catheter ablation for atrial fibrillation: the Japanese Catheter Ablation Registry of Atrial Fibrillation (J-CARAF). J Arrhythmia. 2017;33:430–3.
Gellert G, Bramlage P. Use of the ClearSight® System for continuous noninvasive hemodynamic monitoring during heart valve interventions: review of the literature and single-site experience. Heart Surg Forum. 2018;21:E476-e483.
Froehler MT, Chitale R, Magarik JA, Fusco MR. Comparison of a pressure-sensing sheath and radial arterial line for intraoperative blood pressure monitoring in neurointerventional procedures. J NeuroInterv Surg. 2018;10:784–7.
Scheer B, Perel A, Pfeiffer UJ. Clinical review: complications and risk factors of peripheral arterial catheters used for haemodynamic monitoring in anaesthesia and intensive care medicine. Crit Care. 2002;6:199–204.
Mitchell MD, Hong JA, Lee BY, et al. Systematic review and cost-benefit analysis of radial artery access for coronary angiography and intervention. Circ Cardiovasc Qual Outcomes. 2012;5:454–62.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Iqbal, A.M., Li, K.Y., Aznaurov, S.G. et al. Catheter ablation for atrial fibrillation can be safely performed without invasive hemodynamic monitoring: A multi-center study. J Interv Card Electrophysiol 64, 743–749 (2022). https://doi.org/10.1007/s10840-022-01151-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-022-01151-x