Abstract
Background/purpose
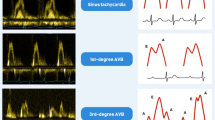
Andersen-Tawil syndrome type 1 is a rare autosomal dominant disease caused by a KCNJ2 gene mutation and clinically characterized by dysmorphic features, periodic muscular paralysis, and frequent ventricular arrhythmias (VAs). Although polymorphic and bidirectional ventricular tachycardias are prevalent, PVCs are the most frequent VAs. In addition, a “dominant” morphology with RBBB pattern associated with either superior or inferior axis is seen in most of the patients. Due to the limited efficacy of most antiarrhythmic drugs, catheter ablation (CA) is an alternative in patients with monomorphic VAs. Based on our experience, we aimed to review the arrhythmogenic mechanisms and substrates for VAs, and we analyzed the potential reasons for CA failure in this group of patients.
Methods
Case report and focused literature review.
Results
Catheter ablation has been reported to be unsuccessful in all of the few cases published so far. Most of the information suggests that VAs are mainly originated from the left ventricle and probably in the Purkinje network. Although identifying well-established and accepted mapping criteria for successful ablation of a monomorphic ventricular arrhythmia, papillary muscles seem not to be the right target.
Conclusions
More research is needed to understand better the precise mechanism and site of origin of VAs in Andersen-Tawil syndrome patients with this particular “dominant” monomorphic ventricular pattern to establish the potential role of CA.





Similar content being viewed by others
References
Tristani-Firouzi M, Jensen JL, Donaldson MR, et al. Functional and clinical characterization of KCNJ2 mutations associated with LQT7 (Andersen syndrome). J Clin Investig. 2002;110(3):381–8. https://doi.org/10.1172/JCI15183.
Tristani-Firouzi M, Etheridge SP. Kir 2.1 channelopathies: the Andersen-Tawil syndrome. Pflugers Arch. 2010;460(2):289–94. https://doi.org/10.1007/s00424-010-0820-6.
Pérez-Riera AR, Barbosa-Barros R, Samesina N, et al. Andersen-Tawil syndrome: a comprehensive review. Cardiol Rev. 2021;29(4):165–77. https://doi.org/10.1097/crd.0000000000000326.
Mazzanti A, Guz D, Trancuccio A, et al. Natural history and risk stratification in Andersen-Tawil syndrome Type 1. J Am Coll Cardiol. 2020;75(15):1772–84. https://doi.org/10.1016/j.jacc.2020.02.033.
Cronin EM, Bogun FM, Maury P, et al. 2019 HRS/EHRA/APHRS/LAHRS expert consensus statement on catheter ablation of ventricular arrhythmias. Heart Rhythm Off J Heart Rhythm Soc. 2019. https://doi.org/10.1016/j.hrthm.2019.03.002.
Haissaguerre M, Extramiana F, Hocini M, et al. Mapping and ablation of ventricular fibrillation associated with long-QT and Brugada syndromes. Circulation. 2003;108(8):925–8. https://doi.org/10.1161/01.CIR.0000088781.99943.95.
Kimura H, Zhou J, Kawamura M, et al. Phenotype variability in patients carrying KCNJ2 mutations. Circ Cardiovasc Genet. 2012;5(3):344–53. https://doi.org/10.1161/CIRCGENETICS.111.962316.
Kawamura M, Ohno S, Naiki N, et al. Genetic background of catecholaminergic polymorphic ventricular tachycardia in Japan. Circ J. 2013;77(7):1705–13. https://doi.org/10.1253/circj.cj-12-1460.
Delannoy E, Sacher F, Maury P, et al. Cardiac characteristics and long-term outcome in Andersen-Tawil syndrome patients related to KCNJ2 mutation. EP Europace. 2013;15(12):1805–11. https://doi.org/10.1093/europace/eut160.
Marquez MF, Totomoch-Serra A, Vargas-Alarcon G, et al. Andersen-Tawil syndrome: a review of its clinical and genetic diagnosis with emphasis on cardiac manifestations. Arch Cardiol Mex. 2014;84(4):278–85. https://doi.org/10.1016/j.acmx.2013.12.007.
Fadahunsi O, Shaikh B, Rettew A, et al. Atrial pacing for the management of ventricular arrhythmias in Andersen-Tawil syndrome. HeartRhythm Case Rep. 2015;1(5):352–5. https://doi.org/10.1016/j.hrcr.2015.06.011.
Van Ert HA, McCune EC, Orland KM, et al. Flecainide treats a novel KCNJ2 mutation associated with Andersen-Tawil syndrome. HeartRhythm Case Rep. 2017;3(2):151–4. https://doi.org/10.1016/j.hrcr.2016.11.009.
Yilmaz S, Kanat S. Failure of radiofrequency catheter ablation and success of flecainide to suppress premature ventricular contractions in Andersen-Tawil syndrome: a case report. J Electrocardiol. 2021;68:37–40. https://doi.org/10.1016/j.jelectrocard.2021.07.004.
Kukla P, Biernacka EK, Baranchuk A, et al. Electrocardiogram in Andersen-Tawil syndrome. New electrocardiographic criteria for diagnosis of type-1 Andersen-Tawil syndrome. Curr Cardiol Rev. 2014;10(3):222–8. https://doi.org/10.2174/1573403x10666140514102528.
Krych M, Biernacka EK, Poninska J, et al. Andersen-Tawil syndrome: clinical presentation and predictors of symptomatic arrhythmias - Possible role of polymorphisms K897T in KCNH2 and H558R in SCN5A gene. J Cardiol. 2017;70(5):504–10. https://doi.org/10.1016/j.jjcc.2017.01.009.
Lévy S, Aliot E. Bidirectional tachycardia: a new look on the mechanism. Pacing Clin Electrophysiol PACE. 1989;12(5):827–34. https://doi.org/10.1111/j.1540-8159.1989.tb01905.x.
Sansone V, Tawil R. Management and treatment of Andersen-Tawil syndrome (ATS). Neurotherapeutics. 2007;4(2):233–7. https://doi.org/10.1016/j.nurt.2007.01.005.
Zhang L, Benson DW, Tristani-Firouzi M, et al. Electrocardiographic features in Andersen-Tawil syndrome patients with KCNJ2 mutations: characteristic T-U-wave patterns predict the KCNJ2 genotype. Circulation. 2005;111(21):2720–6. https://doi.org/10.1161/CIRCULATIONAHA.104.472498.
Fox DJ, Klein GJ, Hahn A, et al. Reduction of complex ventricular ectopy and improvement in exercise capacity with flecainide therapy in Andersen-Tawil syndrome. Europace. 2008;10(8):1006–8. https://doi.org/10.1093/europace/eun180.
Pellizzon OA, Kalaizich L, Ptacek LJ, et al. Flecainide suppresses bidirectional ventricular tachycardia and reverses tachycardia-induced cardiomyopathy in Andersen-Tawil syndrome. J Cardiovasc Electrophysiol. 2008;19(1):95–7. https://doi.org/10.1111/j.1540-8167.2007.00910.x.
Baher AA, Uy M, Xie F, et al. Bidirectional ventricular tachycardia: ping pong in the His-Purkinje system. Heart Rhythm Off J Heart Rhythm Soc. 2011;8(4):599–605. https://doi.org/10.1016/j.hrthm.2010.11.038.
Inoue YY, Aiba T, Kawata H, et al. Different responses to exercise between Andersen-Tawil syndrome and catecholaminergic polymorphic ventricular tachycardia. EP Europace. 2018;20(10):1675–82. https://doi.org/10.1093/europace/eux351.
Ai T, Fujiwara Y, Tsuji K, et al. Novel KCNJ2 mutation in familial periodic paralysis with ventricular dysrhythmia. Circulation. 2002;105(22):2592–4. https://doi.org/10.1161/01.cir.0000019906.35135.a3.
Liu XL, Huang XJ, Luan XH, et al. Case report: A Chinese child with Andersen-Tawil syndrome due to a de novo KCNJ2 mutation. J Neurol Sci. 2015;352(1–2):105–6. https://doi.org/10.1016/j.jns.2015.02.027.
Sevda D, Pınar G, Senem M, et al. A case with classical triad of Andersen Tawil Syndrome and KCNJ2: c.919A > G mutation. Neurol Sci Neurophysiol. 2018;35:151–3.
Ullah A, Khan R, Naeem M. Whole exome sequencing identified a heterozygous KCNJ2 missense variant underlying autosomal dominant familial hypokalemic periodic paralysis in a Pakistani family. J Pediatr Endocrinol Metab. 2019;32(12):1385–9. https://doi.org/10.1515/jpem-2019-0276.
Horga A, Raja Rayan DL, Matthews E, et al. Prevalence study of genetically defined skeletal muscle channelopathies in England. Neurology. 2013;80(16):1472–5. https://doi.org/10.1212/WNL.0b013e31828cf8d0.
Stunnenberg BC, Raaphorst J, Deenen JCW, et al. Prevalence and mutation spectrum of skeletal muscle channelopathies in the Netherlands. Neuromuscul Disord. 2018;28(5):402–7. https://doi.org/10.1016/j.nmd.2018.03.006.
Weingart R, Kass RS, Tsien RW. Is digitalis inotropy associated with enhanced slow inward calcium current? Nature. 1978;273(5661):389–92. https://doi.org/10.1038/273389a0.
Levi AJ, Dalton GR, Hancox JC, et al. Role of intracellular sodium overload in the genesis of cardiac arrhythmias. J Cardiovasc Electrophysiol. 1997;8(6):700–21. https://doi.org/10.1111/j.1540-8167.1997.tb01834.x.
Rosenbaum MB, Elizari MV, Lazzari JO. The mechanism of bidirectional tachycardia. Am Heart J. 1969;78(1):4–12. https://doi.org/10.1016/0002-8703(69)90250-6.
Maruyama M, Lin SF, Chen PS. Alternans of diastolic intracellular calcium elevation as the mechanism of bidirectional ventricular tachycardia in a rabbit model of Andersen-Tawil syndrome. Heart Rhythm Off J Heart Rhythm Soc. 2012;9(4):626–7. https://doi.org/10.1016/j.hrthm.2010.12.021.
Cerrone M, Noujaim SF, Tolkacheva EG, et al. Arrhythmogenic mechanisms in a mouse model of catecholaminergic polymorphic ventricular tachycardia. Circ Res. 2007;101(10):1039–48. https://doi.org/10.1161/CIRCRESAHA.107.148064.
Takahashi T, Tandai S, Toki T, et al. KCNJ2 mutation in intractable ventricular arrhythmia with Andersen’s syndrome. Pediatr Int. 2005;47(2):220–3. https://doi.org/10.1111/j.1442-200x.2005.02024.x.
Schoonderwoerd BA, Wiesfeld AC, Wilde AA, et al. A family with Andersen-Tawil syndrome and dilated cardiomyopathy. Heart Rhythm Off J Heart Rhythm Soc. 2006;3(11):1346–50. https://doi.org/10.1016/j.hrthm.2006.07.021.
Smith AH, Fish FA, Kannankeril PJ. Andersen-Tawil syndrome. Indian Pacing Electrophysiol J. 2006;6(1):32–43.
Erdogan O, Aksoy A, Turgut N, et al. Oral verapamil effectively suppressed complex ventricular arrhythmias and unmasked U waves in a patient with Andersen-Tawil syndrome. J Electrocardiol. 2008;41(4):325–8. https://doi.org/10.1016/j.jelectrocard.2008.02.023.
Roden DM. Drug-induced prolongation of the QT interval. N Engl J Med. 2004;350(10):1013–22. https://doi.org/10.1056/NEJMra032426.
Marquez M, Nava S, Gomez J, et al. Lack of efficacy of radiofrequency catheter ablation in Andersen-Tawil syndrome: are we targeting the right spot? EP Europace. 2014;16(11):1697. https://doi.org/10.1093/europace/eut428.
Wilde AA. Andersen-Tawil syndrome, scarier for the doctor than for the patient? Who, when, and how to treat. EP Europace. 2013;15(12):1690–2. https://doi.org/10.1093/europace/eut326.
Wilde AAM, Garan H, Boyden PA. Role of the Purkinje system in heritable arrhythmias. Heart Rhythm Off J Heart Rhythm Soc. 2019;16(7):1121–6. https://doi.org/10.1016/j.hrthm.2019.01.034.
Komatsu Y, Nogami A, Kurosaki K, et al. Fascicular ventricular tachycardia originating from papillary muscles: Purkinje network involvement in the reentrant circuit. Circ Arrhythm Electrophysiol. 2017;10(3):1–11. https://doi.org/10.1161/CIRCEP.116.004549.
Acknowledgements
The authors would like to thank Juan Pablo Fabris for his contribution with clinical information to the case.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The manuscript has not been submitted or is under consideration elsewhere in any other journal. No data has been fabricated or manipulated. Consent to submit has been received explicitly from all co-authors.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 244 KB) ICE imaging during RF delivery at the posteromedial papillary muscle
Rights and permissions
About this article
Cite this article
Keegan, R., Onetto, L., Gregorietti, F. et al. Catheter ablation of frequent monomorphic ventricular arrhythmias in Andersen-Tawil syndrome: case report and focused literature review. J Interv Card Electrophysiol 66, 729–736 (2023). https://doi.org/10.1007/s10840-021-01077-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01077-w