Abstract
Purpose
Catheter ablation is a cornerstone of the therapy for paroxysmal atrial fibrillation. The importance of effective lesion size formation during pulmonary vein isolation is gauged through conduction recovery and recurrence of arrhythmia. Therefore, the lesion size index (LSI) is designed to utilize traditional intraprocedural parameters and predict procedural success. The impact of the optimal LSI index and the respective segments of the pulmonary veins has not been commonly evaluated. We aimed to assess whether higher and targeted LSI on the different segments of pulmonary veins could actually lead to better clinical outcomes of paroxysmal atrial fibrillation ablation.
Methods
Retrospective analyses of drug-refractory paroxysmal atrial fibrillation patients who underwent first catheter ablation were conducted. Targeted LSI of 6.5 at the anterior wall and 5.2 at the posterior wall, roof, and floor of the pulmonary vein was applied. The primary endpoint was defined as arrhythmias recurrence assessed by routine electrocardiograms and 24-h ambulatory electrocardiographic monitoring at 3, 6, and 12 months post-ablation.
Results
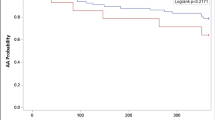
Among the included 39 patients, the single-procedure 12-month freedom from arrhythmias was reached in 92.3% of patients. Interestingly, there was no tendency towards an increased number of adverse effects using a higher LSI index.
Conclusions
Atrial fibrillation ablation guided by targeted LSI value showed efficiency on the freedom from arrhythmias during 1-year follow-up period without harmful effects.

Similar content being viewed by others
Data availability
Yes.
Code availability
Not applicable.
References
Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, Blomström-Lundqvist C, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): The Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) Developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur Heart J. 2021;42:373–498. https://doi.org/10.1093/eurheartj/ehaa612.
Packer DL, Mark DB, Robb RA, Monahan KH, Bahnson TD, Poole JE, Noseworthy PA, et al. Effect of catheter ablation vs antiarrhythmic drug therapy on mortality, stroke, bleeding, and cardiac arrest among patients with atrial fibrillation: the CABANA randomized clinical trial. JAMA. 2019;321:1261–74. https://doi.org/10.1001/jama.2019.0693.
Andrade JG, Wells GA, Deyell MW, Bennett M, Essebag V, Champagne J, et al. Cryoablation or drug therapy for initial treatment of atrial fibrillation. N Engl J Med. 2021;384:305–15. https://doi.org/10.1056/NEJMoa2029980.
Natale A, Reddy VY, Monir G, Wilber DJ, Lindsay BD, McElderry HT, et al. Paroxysmal AF catheter ablation with a contact force sensing catheter: results ofthe prospective, multicenter SMART-AF trial. J Am CollCardiol. 2014;64:647–56.
Reddy VY, Shah D, Kautzner J, Schmidt B, Saoudi N, Herrera C, et al. The relationship between contact force and clinical outcome during radiofrequency catheter ablation of atrial fibrillation in the TOCCATA study. Heart Rhythm. 2012;9:1789–95.
Kimura M, Sasaki S, Owada S, Horiuchi D, Sasaki K, Itoh T, et al. Comparison of lesion formation between contact force guided and non-guided circumferential pulmonary vein isolation: a prospective, randomized study. Heart Rhythm. 2014;11:984–91.
Marijon E, Fazaa S, Narayanan K, Guy-Moyat B, Bouzeman A, Providencia R, et al. Real-time contact force sensing for pulmonary vein isolation in the setting of paroxysmal atrial fibrillation: procedural and 1-year results. J Cardiovasc Electrophysiol. 2014;25:130–7. https://doi.org/10.1111/jce.12303.
Neuzil P, Reddy VY, Kautzner J, Petru J, Wichterle D, Shah D, et al. Electrical reconnection after pulmonary vein isolation is contingent on contact force during initial treatment: results from the EFFICAS I study. Circ Arrhythmia Electrophysiol. 2013;6:327–33.
Kuck KH, Reddy VY, Schmidt B, Natale A, Neuzil P, Saoudi N, et al. A novel radiofrequency ablation catheter using contact force sensing: Toccata study. Heart Rhythm. 2012;9:18–23. https://doi.org/10.1016/j.hrthm.2011.08.021.
Calzolari V, De Mattia L, Indiani S, Crosato M, Furlanetto A, Licciardello C, et al. In vitro validation of the lesion size index to predict lesion width and depth after irrigated radiofrequency ablation in a porcine model. JACC Clin Electrophysiol. 2017;3:1126–35. https://doi.org/10.1016/j.jacep.2017.08.016.
Ho SY, Cabrera JA, Sanchez-Quintana D. Left atrial anatomy revisited. CircArrhythmElectrophysiol. 2012;5:220–8. https://doi.org/10.1161/CIRCEP.111.962720.
Hall B, Jeevanantham V, Simon R, Filippone J, Vorobiof G, Daubert J. Variation in left atrial transmural wall thickness at sites commonly targeted for ablation of atrial fibrillation. J Interv Card Electrophysiol. 2006;17:127–32. https://doi.org/10.1007/s10840-006-9052-2.
Osorio J, Hunter TD, Rajendra A, Zei P, Silverstein J, Morales G. Predictors of clinical success after paroxysmal atrial fibrillation catheter ablation. J Cardiovasc Electrophysiol. 2021;32:1814–21. https://doi.org/10.1111/jce.15028.
Mattia L, Crosato M, Indiani S, Causin E, Licciardello C, Maria Squasi PA, et al. Prospective evaluation of lesion index-guided pulmonary vein isolation technique in patients with paroxysmal atrial fibrillation: 1-year follow-up. J Atr Fibrillation. 2018;10:1858. https://doi.org/10.4022/jafib.1858.
Dello Russo A, Fassini GM, Casella M, Romanelli E, Pala S, Riva S, et al. Lesion index: a novel guide in the path of successful pulmonary vein isolation. J Interv Card Electrophysiol. 2019;55:27–34. https://doi.org/10.1007/s10840-018-0487-z.
Sundaram S, Choe W, Jordan JR, Boorman C, Mullins N, Davies A, et al. Two year, single center clinical outcome after catheter ablation for paroxysmal atrial fibrillation guided by lesion index. J Atr Fibrillation. 2018;11:1760. https://doi.org/10.4022/jafib.1760.
Goya M, Frame D, Gache L, Ichishima Y, Tayar DO, Goldstein L, et al. The use of intracardiac echocardiography catheters in endocardial ablation of cardiac arrhythmia: meta-analysis of efciency, efectiveness, and safety outcomes. J Cardiovasc Electrophysiol. 2020;31:664–73.
Wang Y, Zhou G, Chen S, Wei Y, Lu X, Xu J, et al. Tailored ablation index for pulmonary vein isolation according to wall thickness within the ablation circle. Pacing Clin Electrophysiol. 2021;44:575–85. https://doi.org/10.1111/pace.14125.
Mulder MJ, Kemme MJB, Hagen AMD, Hopman LHGA, van de Ven PM, Hauer HA, et al. Impact of local left atrial wall thickness on the incidence of acute pulmonary vein reconnection after Ablation Index-guided atrial fibrillation ablation. Int J Cardiol Heart Vasc. 2020;29: 100574. https://doi.org/10.1016/j.ijcha.2020.100574.
Kanamori N, Kato T, Sakagami S, Saeki T, Kato C, Kawai K, et al. Optimal lesion size index to prevent conduction gap during pulmonary vein isolation. J Cardiovasc Electrophysiol. 2018;29:1616–23. https://doi.org/10.1111/jce.13727.
Matsuura G, Kishihara J, Fukaya H, Oikawa J, Ishizue N, Saito et al. Optimized lesion size index (o-LSI): A novel predictor for sufficient ablation of pulmonary vein isolation. J Arrhythm. 2021;37:558–65. https://doi.org/10.1002/joa3.12537.
Phlips T, Taghji P, El Haddad M, Wolf M, Knecht S, Vandekerckhove Y, et al. Improving procedural and one-year outcome after contact force-guided pulmonary vein isolation: the role of interlesion distance, ablation index, and contact force variability in the ’CLOSE’-protocol. Europace. 2018;20:419–27. https://doi.org/10.1093/europace/eux376.
Parwani AS, Hohendanner F, Bode D, Kuhlmann S, Blaschke F, Lacour P, et al. The force stability of tissue contact and lesion size index during radiofrequency ablation: an ex-vivo study. Pacing Clin Electrophysiol. 2020;43:327–31. https://doi.org/10.1111/pace.13891.
Shin DG, Ahn J, Han SJ, Lim HE. Efficacy of high-power and short-duration ablation in patients with atrial fibrillation: a prospective randomized controlled trial. Europace. 2020;22:1495–501. https://doi.org/10.1093/europace/euaa144.
Leo M, Pedersen M, Rajappan K, Ginks MR, Hunter RJ, Bowers R, et al. Power, lesion size index and oesophageal temperature alerts during atrial fibrillation ablation: a randomized study. Circ Arrhythm Electrophysiol. 2020;13: e008316. https://doi.org/10.1161/CIRCEP.120.008316.
Jan M, Žižek D, Kuhelj D, Lakič N, Prolič Kalinšek T, Štublar J, et al. Combined use of electro-anatomic mapping system and intracardiac echocardiography to achieve zero-fluoroscopy catheter ablation for treatment of paroxysmal atrial fibrillation: a single centre experience. Int J Cardiovasc Imaging. 2020;36:415–22. https://doi.org/10.1007/s10554-019-01727-1.
Ren JF, Chen S, Callans DJ, Jiang C, Marchlinski FE. Role of intracardiac echocardiography for catheter ablation of atrial fibrillation: reduction of complications and mortality. J Am Coll Cardiol. 2020;75:1244–5. https://doi.org/10.1016/j.jacc.2019.11.067.
Isath A, Padmanabhan D, Haider SW, Siroky G, Perimbeti S, Correa A, et al. Does the use of intracardiac echocardiography during atrial fibrillation catheter ablation improve outcomes and cost? A nationwide 14-year analysis from 2001 to 2014. J Interv Card Electrophysiol. 2020. https://doi.org/10.1007/s10840-020-00844-5.
De Potter T, Hunter TD, Boo LM, Chatzikyriakou S, Strisciuglio T, Silva E, et al. The industrialization of ablation: a highly standardized and reproducible workflow for radiofrequency ablation of atrial fibrillation. J Interv Card Electrophysiol. 2020;59:21–7. https://doi.org/10.1007/s10840-019-00622-y.
Duytschaever M, Vijgen J, De Potter T, Scherr D, Van Herendael H, Knecht S, et al. Standardized pulmonary vein isolation workflow to enclose veins with contiguous lesions: the multicentre VISTAX trial. Europace. 2020;22:1645–52. https://doi.org/10.1093/europace/euaa157.
Calkins H, Hindricks G, Cappato R, Kim YH, Saad EB, Aguinaga L, et al. 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Europace. 2018;20:1–160. https://doi.org/10.1093/europace/eux274.
Author information
Authors and Affiliations
Contributions
Zrinka Jurišić and Ante Anić contributed to the conception and design of the study. Josip Katic screened the articles and assessed the quality of the studies and performed the data extraction and analysis. Josip Katić and Toni Brešković drafted the manuscript, and Ante Anić and Zrinka Jurišić revised the manuscript critically for important intellectual content. All of the authors contributed to the interpretation of the data, gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
Yes.
Consent to participate
No.
Consent for publication
Yes.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Katić, J., Anić, A., Brešković, T. et al. Higher than recommended lesion size index target values for pulmonary vein isolation result in better clinical outcomes in paroxysmal atrial fibrillation patients. J Interv Card Electrophysiol 64, 463–468 (2022). https://doi.org/10.1007/s10840-021-01053-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01053-4