Abstract
Purpose
Amiodarone is commonly used in atrial fibrillation (AF). Long-term use of amiodarone is associated with significant toxicities especially in elderly patients. However, in the short term after hospitalization of AF, it remains uncertain whether the use of amiodarone will increase mortality. We aim to investigate whether Amiodarone affects short-term mortality in elderly patients after hospitalization for atrial fibrillation.
Methods
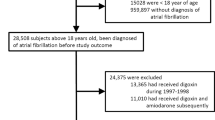
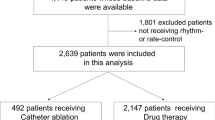
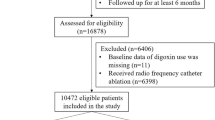
We conducted a single-center retrospective cohort study including patients (Age > = 60 years old) who were hospitalized between 07/01/2004 and 06/30/2019 with primary diagnosis of AF and left ventricular ejection fraction (LVEF) > = 50%. Patients who were prescribed amiodarone during hospitalization but not before hospitalization are classified into Amiodarone group (341 patients). Patients who were not prescribed amiodarone are classified into non-amiodarone group (2171 patients). Propensity score matching was performed with 1:1 nearest-neighbor matching of Amiodarone group and Non-amiodarone group based on baseline variables. Univariate and Multivariate logistic regression were used to calculate the odds ratio of amiodarone use on in-hospital mortality, and multivariate cox regression was adopted to calculate the hazard ratio of amiodarone use on 100-day mortality.
Results
Patients’ baseline demographic and clinical characteristics were well matched in both groups. Both univariate and multivariate logistic regression showed amiodarone group had higher in-hospital mortality (OR 10.27, p = 0.0268; 16.50, p = 0.0171) than non-amiodarone group and multivariate Cox regression suggested increased 100-day all-cause mortality (HR 2.34, p = 0.022).
Conclusion
Amiodarone use in elderly patients with preserved ejection fraction is associated with increased in-hospital and 100-day all-cause mortality after hospitalization for AF.



Similar content being viewed by others
Data availability
Available upon request once approved by Institutional Review Board for data sharing.
Code availability
Available upon request
References
Chugh SS, Havmoeller R, Narayanan K, Singh D, Rienstra M, Benjamin EJ, et al. Worldwide epidemiology of atrial fibrillation: a Global Burden of Disease 2010 Study. Circulation. 2014;129(8):837–47.
Zimetbaum P. Amiodarone for atrial fibrillation. N Engl J Med. 2007;356(9):935–41.
Hou ZY, Chang MS, Chen CY, Tu MS, Lin SL, Chiang HT, et al. Acute treatment of recent-onset atrial fibrillation and flutter with a tailored dosing regimen of intravenous amiodarone. A randomized, digoxin-controlled study. Eur Heart J. 1995;16(4):521–8.
Roy D, Talajic M, Dorian P, Connolly S, Eisenberg MJ, Green M, et al. Amiodarone to prevent recurrence of atrial fibrillation. Canadian Trial of Atrial Fibrillation Investigators. N Engl J Med. 2000;342(13):913–20.
Investigators AFADS. Maintenance of sinus rhythm in patients with atrial fibrillation: an AFFIRM substudy of the first antiarrhythmic drug. J Am Coll Cardiol. 2003;42(1):20–9.
Galve E, Rius T, Ballester R, Artaza MA, Arnau JM, García-Dorado D, et al. Intravenous amiodarone in treatment of recent-onset atrial fibrillation: results of a randomized, controlled study. J Am Coll Cardiol. 1996;27(5):1079–82.
Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association of Cardio-Thoracic Surgery (EACTS). Eur Heart J 2020;42(5):373–498. https://doi.org/10.1093/eurheartj/ehaa612.
Latini R, Tognoni G, Kates RE. Clinical pharmacokinetics of amiodarone. Clin Pharmacokinet. 1984;9(2):136–56.
Papiris SA, Triantafillidou C, Kolilekas L, Markoulaki D, Manali ED. Amiodarone: review of pulmonary effects and toxicity. Drug Saf. 2010;33(7):539–58.
Elnaggar MN, Jbeili K, Nik-Hussin N, Kozhippally M, Pappachan JM. Amiodarone-Induced Thyroid Dysfunction: A Clinical Update. Exp Clin Endocrinol Diabetes. 2018;126(6):333–41.
Lewis JH, Ranard RC, Caruso A, Jackson LK, Mullick F, Ishak KG, et al. Amiodarone hepatotoxicity: prevalence and clinicopathologic correlations among 104 patients. Hepatology. 1989;9(5):679–85.
Di Biase L, et al. Ablation versus amiodarone for treatment of persistent atrial fibrillation in patients with congestive heart failure and an implanted device: results from the AATAC multicenter randomized trial. Circulation. 2016;133(17):1637–44.
Srinivasan M, Ahmad L, Bhindi R, Allahwala U. Amiodarone in the aged. Aust Prescr. 2019;42(5):158–62.
Wang Y, Cai H, Li C, Jiang Z, Wang L, Song J, et al. Optimal caliper width for propensity score matching of three treatment groups: a Monte Carlo study. PLoS One. 2013;8(12):e81045.
Cushing DJ, Cooper WD, Gralinski MR, Lipicky RJ. The hypotensive effect of intravenous amiodarone is sustained throughout the maintenance infusion period. Clin Exp Pharmacol Physiol. 2010;37(3):358–61.
Essebag V, Hadjis T, Platt RW, Pilote L. Amiodarone and the risk of bradyarrhythmia requiring permanent pacemaker in elderly patients with atrial fibrillation and prior myocardial infarction. J Am Coll Cardiol. 2003;41(2):249–54.
Middlekauff HR, Stevenson WG, Saxon LA, Stevenson LW. Amiodarone and torsades de pointes in patients with advanced heart failure. Am J Cardiol. 1995;76(7):499–502.
Akao M. Atrial fibrillation and coronary artery disease: Resembling twins? J Cardiol. 2014;63(2):169–70.
Wang A, Green JB, Halperin JL, Piccini JP Sr. Atrial fibrillation and diabetes mellitus: JACC review topic of the week. J Am Coll Cardiol. 2019;74(8):1107–15.
Kallistratos MS, Poulimenos LE, Manolis AJ. Atrial fibrillation and arterial hypertension. Pharmacol Res. 2018;128:322–6.
Aydin M, Susam I, Kilicaslan B, Dereli M, Sacar M, Ozdogan O. Serum cholesterol levels and postoperative atrial fibrillation. J Cardiothorac Surg. 2014;9:69.
Odutayo A, et al. Atrial fibrillation and risks of cardiovascular disease, renal disease, and death: systematic review and meta-analysis. BMJ. 2016;354:i4482.
Goudis CA. Chronic obstructive pulmonary disease and atrial fibrillation: an unknown relationship. J Cardiol. 2017;69(5):699–705.
Delle Karth G, Geppert A, Neunteufl T, Priglinger U, Haumer M, Gschwandtner M, et al. Amiodarone versus diltiazem for rate control in critically ill patients with atrial tachyarrhythmias. Crit Care Med. 2001;29(6):1149–53.
Diamond JA, Krakoff LR, Goldman A, Coplan N, Gharavi A, Martin K, et al. Comparison of two calcium blockers on hemodynamics, left ventricular mass, and coronary vasodilatory in advanced hypertension. Am J Hypertens. 2001;14(3):231–40.
Dias VC, Weir SJ, Ellenbogen KA. Pharmacokinetics and pharmacodynamics of intravenous diltiazem in patients with atrial fibrillation or atrial flutter. Circulation. 1992;86(5):1421–8.
Patel K, Fonarow GC, Ahmed M, Morgan C, Kilgore M, Love TE, et al. Calcium channel blockers and outcomes in older patients with heart failure and preserved ejection fraction. Circ Heart Fail. 2014;7(6):945–52.
Charnigo R, Khairy P, Guo J, Shohoudi A, Elayi CS. Use of digoxin in atrial fibrillation: one step further in the mortality controversy from the AFFIRM study. Pacing Clin Electrophysiol. 2018;41(7):713–9.
Llacer P, et al. Digoxin and prognosis of heart failure in older patients with preserved ejection fraction: importance of heart rate. Results from an observational and multicenter study. Eur J Intern Med. 2019;60:18–23.
Yeramaneni S, Kleindorfer DO, Sucharew H, Alwell K, Moomaw CJ, Flaherty ML, et al. Hyperlipidemia is associated with lower risk of poststroke mortality independent of statin use: a population-based study. Int J Stroke. 2017;12(2):152–60.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
Approved by Institutional Review Board of Albert Einstein College of Medicine.
Informed consent
Informed consent was waived based on retrospective nature of the study with minimal risk.
Conflict of interest
Dr. Di Biase is a consultant for Biosense Webster, Boston Scientific, and St. Jude Medical and has received speaker honoraria/travel from Medtronic, Atricure, EPiEP, and Biotronik. The remaining authors report no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, W., Wang, YC., Tiwari, N. et al. Amiodarone is associated with increased short-term mortality in elderly atrial fibrillation patients with preserved ejection fraction. J Interv Card Electrophysiol 63, 207–214 (2022). https://doi.org/10.1007/s10840-021-00970-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-00970-8