Abstract
Purpose
Atrial fibrillation (AF) is one of the most commonly sustained arrhythmias in clinical practice. Long non-coding RNAs (lncRNAs) are gene regulatory elements involved in the development of several diseases. We aimed to explore the expression characteristics of lncRNAs associated with AF.
Methods
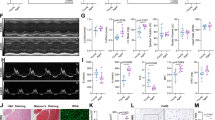
We randomly assigned 12 adult healthy mongrel dogs into a control group and an atrial pacing group. Atrial pacing stimulation was performed at a high frequency of 500 beats per min for 14 consecutive days in the atrial pacing group. HE and Masson staining were used to detect rapid atrial pacing induced atrial fibrosis. Total RNA extraction was performed on dog atrial tissues and was used for high-throughput sequencing of lncRNAs.
Results
A total of 10,310 lncRNAs were detected, and 33 differentially expressed lncRNAs were screened. Among them, 19 lncRNAs were upregulated in the atrial pacing group, and 14 lncRNAs were downregulated. Gene Ontology (GO) classification, Kyoto Encyclopedia of Genes and Genomes (KEGG) analysis, and interaction networks showed that AF-related lncRNAs participate in the regulation of AF in diverse biological processes, cellular components, molecular functions, signaling pathways, and complex interactions with miRNAs and mRNAs. Five differentially expressed lncRNAs were selected for RT-PCR validation, and the verification results were consistent with the results of lncRNA sequencing.
Conclusions
In summary, our study enhances our understanding of the biological functions of AF-related lncRNAs by screening and analyzing differentially expressed lncRNAs, and the results help to enrich the theoretical basis for the treatment of atrial fibrillation.






Similar content being viewed by others
References
Fuster V, Ryden LE, Cannom DS, Crijns HJ, Curtis AB, Ellenbogen KA, et al. ACC/AHA/ESC 2006 Guidelines for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Europace. 2006;8:651–745.
Munger TM, Wu LQ, Shen WK. Atrial fibrillation. J Biomed Res. 2014;28:1–17.
Caplan LR. Atrial fibrillation, past and future: from a stroke non-entity to an over-targeted cause. Cerebrovasc Dis. 2018;45:149–53.
Lindberg T, Wimo A, Elmstahl S, Qiu C, Bohman DM, Sanmartin Berglund J. Prevalence and incidence of atrial fibrillation and other arrhythmias in the general older population: findings from the Swedish National Study on Aging and Care. Gerontol Geriatr Med. 2019;5:2333721419859687.
Calkins H, Kuck KH, Cappato R, Brugada J, Camm AJ, Chen SA, et al. 2012 HRS/EHRA/ECAS expert consensus statement on catheter and surgical ablation of atrial fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design: a report of the Heart Rhythm Society (HRS) Task Force on Catheter and Surgical Ablation of Atrial Fibrillation. Developed in partnership with the European Heart Rhythm Association (EHRA), a registered branch of the European Society of Cardiology (ESC) and the European Cardiac Arrhythmia Society (ECAS); and in collaboration with the American College of Cardiology (ACC), American Heart Association (AHA), the Asia Pacific Heart Rhythm Society (APHRS), and the Society of Thoracic Surgeons (STS). Endorsed by the governing bodies of the American College of Cardiology Foundation, the American Heart Association, the European Cardiac Arrhythmia Society, the European Heart Rhythm Association, the Society of Thoracic Surgeons, the Asia Pacific Heart Rhythm Society, and the Heart Rhythm Society. Heart Rhythm. 2012;9:632–696.e621.
Kannel WB, Wolf PA, Benjamin EJ, Levy D. Prevalence, incidence, prognosis, and predisposing conditions for atrial fibrillation: population-based estimates. Am J Cardiol. 1998;82:2N–9N.
Chugh SS, Havmoeller R, Narayanan K, Singh D, Rienstra M, Benjamin EJ, et al. Worldwide epidemiology of atrial fibrillation: a global burden of disease 2010 study. Circulation. 2014;129:837–47.
Ko D, Rahman F, Schnabel RB, Yin X, Benjamin EJ, Christophersen IE. Atrial fibrillation in women: epidemiology, pathophysiology, presentation, and prognosis. Nat Rev Cardiol. 2016;13:321–32.
Liu X, Li Y, Zhang H, Ji Y, Zhao Z, Wang C. The research of ion channel-related gene polymorphisms with atrial fibrillation in the Chinese Han population. Mol Genet Genomic Med. 2019;7:e835.
Corden B, Jarman J, Whiffin N, Tayal U, Buchan R, Sehmi J, et al. Association of titin-truncating genetic variants with life-threatening cardiac arrhythmias in patients with dilated cardiomyopathy and implanted defibrillators. JAMA Netw Open. 2019;2:e196520.
Alsina KM, Hulsurkar M, Brandenburg S, Kownatzki-Danger D, Lenz C, Urlaub H, et al. Loss of protein phosphatase 1 regulatory subunit PPP1R3A promotes atrial fibrillation. Circulation. 2019;140:681–93.
Jiang T, Wang YN, Qu Q, Qi TT, Chen YD, Qu J. Association between gene variants and the recurrence of atrial fibrillation: an updated meta-analysis. Medicine. 2019;98:e15953.
Santulli G, Iaccarino G, De Luca N, Trimarco B, Condorelli G. Atrial fibrillation and microRNAs. Front Physiol. 2014;5:15.
Lee C, Kikyo N. Strategies to identify long noncoding RNAs involved in gene regulation. Cell Biosci. 2012;2:37.
Bolha L, Ravnik-Glavac M. Long noncoding RNAs as biomarkers in cancer. Dis Markers. 2017;2017:7243968.
Fernandes JCR, Acuna SM, Aoki JI, Floeter-Winter LM, Muxel SM. Long non-coding RNAs in the regulation of gene expression: physiology and disease. Noncod RNA. 2019;5:17.
Li H, Ma SQ, Huang J, Chen XP, Zhou HH. Roles of long noncoding RNAs in colorectal cancer metastasis. Oncotarget. 2017;8:39859–76.
Zhang Y, Du W, Yang B. Long non-coding RNAs as new regulators of cardiac electrophysiology and arrhythmias: molecular mechanisms, therapeutic implications and challenges. Pharmacol Ther. 2019;107389.
Charles Richard JL, Eichhorn PJA. Platforms for investigating LncRNA functions. SLAS Technol. 2018;23:493–506.
Liu E, Yang S, Xu Z, Li J, Yang W, Li G. Angiotensin-(1-7) prevents atrial fibrosis and atrial fibrillation in long-term atrial tachycardia dogs. Regul Pept. 2010;162:73–8.
Li X, Luo S, Zhang J, Yuan Y, Jiang W, Zhu H, et al. lncRNA H19 alleviated myocardial I/RI via suppressing miR-877-3p/Bcl-2-mediated mitochondrial apoptosis. Mol Ther Nucleic Acids. 2019;17:297–309.
Greco S, Gaetano C, Martelli F. Long noncoding competing endogenous RNA networks in age-associated cardiovascular diseases. Int J Mol Sci. 2019;20:3079.
Monteiro JP, Bennett M, Rodor J, Caudrillier A, Ulitsky I, Baker AH. Endothelial function and dysfunction in the cardiovascular system: the long non-coding road. Cardiovasc Res. 2019;115:1692–704.
Kowatsch C, Woolley RE, Kinnebrew M, Rohatgi R, Siebold C. Structures of vertebrate patched and smoothened reveal intimate links between cholesterol and hedgehog signalling. Curr Opin Struct Biol. 2019;57:204–14.
Santulli G, D'Ascia SL, D'Ascia C. Development of atrial fibrillation in recipients of cardiac resynchronization therapy: the role of atrial reverse remodelling. Can J Cardiol. 2012;28:245.e17.
Brundel BJ, Van Gelder IC, Henning RH, Tuinenburg AE, Wietses M, Grandjean JG, et al. Alterations in potassium channel gene expression in atria of patients with persistent and paroxysmal atrial fibrillation: differential regulation of protein and mRNA levels for K+ channels. J Am Coll Cardiol. 2001;37:926–32.
Tajiri K, Guichard JB, Qi X, Xiong F, Naud P, Tardif JC, et al. An N−/L-type calcium channel blocker, cilnidipine, auppresses autonomic, electrical and structural remodeling associated with atrial fibrillation. Cardiovasc Res. 2019;115:1975–85.
Hu HJ, Zhang C, Tang ZH, Qu SL, Jiang ZS. Regulating the Warburg effect on metabolic stress and myocardial fibrosis remodeling and atrial intracardiac waveform activity induced by atrial fibrillation. Biochem Biophys Res Commun. 2019;516:653–60.
Maille B, Das M, Hussein A, Shaw M, Chaturvedi V, Williams E, et al. Reverse electrical and structural remodeling of the left atrium occurs early after pulmonary vein isolation for persistent atrial fibrillation. J Interv Card Electrophysiol. 2020;58:9–19.
Paulis L, Fauconnier J, Cazorla O, Thireau J, Soleti R, Vidal B, et al. Activation of sonic hedgehog signaling in ventricular cardiomyocytes exerts cardioprotection against ischemia reperfusion injuries. Sci Rep. 2015;5:7983.
Burstein B, Nattel S. Atrial fibrosis: mechanisms and clinical relevance in atrial fibrillation. J Am Coll Cardiol. 2008;51:802–9.
Jalife J, Kaur K. Atrial remodeling, fibrosis, and atrial fibrillation. Trends Cardiovasc Med. 2015;25:475–84.
Pellman J, Sheikh F. Atrial fibrillation: mechanisms, therapeutics, and future directions. Compr Physiol. 2015;5:649–65.
Gao Y, Gong Y. Simulation of atrial fibrosis using coupled myocyte-fibroblast cellular and human atrial models. Comput Math Methods Med. 2017;2017:9463010.
Menon A, Hong L, Savio-Galimberti E, Sridhar A, Youn SW, Zhang M, et al. Electrophysiologic and molecular mechanisms of a frameshift NPPA mutation linked with familial atrial fibrillation. J Mol Cell Cardiol. 2019;132:24–35.
Willoughby SR, Roberts-Thomson RL, Lim HS, Schultz C, Prabhu A, de Sciscio P, et al. Atrial platelet reactivity in patients with atrial fibrillation. Heart Rhythm. 2010;7:1178–83.
Lenski M, Schleider G, Kohlhaas M, Adrian L, Adam O, Tian Q, et al. Arrhythmia causes lipid accumulation and reduced glucose uptake. Basic Res Cardiol. 2015;110:40.
Mihm MJ, Yu F, Carnes CA, Reiser PJ, McCarthy PM, van Wagoner DR, et al. Impaired myofibrillar energetics and oxidative injury during human atrial fibrillation. Circulation. 2001;104:174–80.
Watschinger K, Werner ER. Orphan enzymes in ether lipid metabolism. Biochimie. 2013;95:59–65.
Daniel H, Levenes C, Crépel F. Cellular mechanisms of cerebellar LTD. Trends Neurosci. 1998;21:401–7.
Availability of data and material
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Funding
The present study was approved by the Science & Technology Development Fund of Tianjin Education Commission for Higher Education(No. 2018KJ058).
Author information
Authors and Affiliations
Contributions
Xue Liang and Enzhao Liu made substantial contributions to the conception and design of the present study; Lijun Wang and Jiageng Cai acquired the data; Wenfeng Shangguan and Rukun Cheng performed the experiments; Baoshuai Zhang and Tong Liu analyzed and interpreted the data; Xue Liang and Enzhao Liu were involved in drafting the manuscript and revising it critically for important intellectual content. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval and consent to participate
The present study was approved by the Experimental Animal Administration Committee of Tianjin Medical University and Tianjin Municipal Commission for Experimental Animal Control (IRM-DWLL-2019018).
Consent for publication
Written informed consent for publication was obtained from all participants.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shangguan, W., Wang, L., Cheng, R. et al. Screening and functional analysis of differentially expressed lncRNAs in rapid atrial pacing dog atrial tissue. J Interv Card Electrophysiol 61, 375–384 (2021). https://doi.org/10.1007/s10840-020-00824-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-020-00824-9