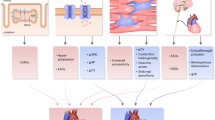
Abstract
Introduction
Irreversible electroporation (IRE) utilizing high voltage pulses is an emerging strategy for catheter-based cardiac ablation with considerable growth in the preclinical arena.
Methods
A systematic search for articles was performed from three sources (PubMed, EMBASE, and Google Scholar). The primary outcome was the efficacy of tissue ablation with characteristics of lesion formation evaluated by histologic analysis. The secondary outcome was focused on safety and damage to collateral structures.
Results
Sixteen studies met inclusion criteria. IRE was most commonly applied to the ventricular myocardium (n = 7/16, 44%) by a LifePak 9 Defibrillator (n = 9/16, 56%), NanoKnife Generator (n = 2/16, 13%), or other custom generators (n = 5/16, 31%). There was significant heterogeneity regarding electroporation protocols. On histological analysis, IRE was successful in creating ablation lesions with variable transmurality depending on the electric pulse parameters and catheter used.
Conclusion
Preclinical studies suggest that cardiac tissue ablation using IRE shows promise in delivering efficacious, safe lesions.

Similar content being viewed by others
Abbreviations
- CA:
-
Coronary arteries
- DC:
-
Direct current
- ECG:
-
Electrocardiogram
- IRE:
-
Irreversible electroporation
- PV:
-
Pulmonary vein
- RF:
-
Radiofrequency
- SVC:
-
Superior vena cava
- VF:
-
Ventricular fibrillation
References
Edmonds JH, Ellison RG, Crews TL. Surgically induced atrioventricular block as treatment for recurrent atrial tachycardia in Wolff-Parkinson-White syndrome. Circulation. 1969;39(5S1):I-105–I-11.
Calkins H, Leon AR, Deam AG, Kalbfleisch SJ, Langberg JJ, Morady F. Catheter ablation of atrial flutter using radiofrequency energy. Am J Cardiol. 1994;73(5):353–6.
Swartz J. A catheter-based curative approach to atrial fibrillation in humans. Circulation. 1994;90:I-335.
Jai P, Hai M, Shah DC, Chouairi S, Gencel L, Cle J. A focal source of atrial fibrillation treated by discrete radiofrequency ablation. Circulation. 1997;95(3):572–6.
Haissaguerre M, Gencel L, Fischer B, Le Metayer P, Poquet F, Marcus FI, et al. Successful catheter ablation of atrial fibrillation. J Cardiovasc Electrophysiol. 1994;5(12):1045–52.
Hindricks G, Haverkamp W, Rissel U, Richter K, Gülker H. Experimental observations on the use of radiofrequency energy for ablation of ventricular tissue. New Trends Arrhyt. 1988;4(1–2):337–42.
Gonska B, Brune S, Bethge K, Kreuzer H. Radiofrequency catheter ablation in recurrent ventricular tachycardia. Eur Heart J. 1991;12(12):1257–65.
Nathan AW, Bennett DH, Ward DE, Bexton RS, Camm AJ. Catheter ablation of atrioventricular conduction. Lancet (London, England). 1984;1(8389):1280–4.
Gallagher JJ, Svenson RH, Kasell JH, German LD, Bardy GH, Broughton A, et al. Catheter technique for closed-chest ablation of the atrioventricular conduction system: a therapeutic alternative for the treatment of refractory supraventricular tachycardia. N Engl J Med. 1982;306(4):194–200.
Ward DE, Davies M. Transvenous high energy shock for ablating atrioventricular conduction in man. Observations on the histological effects. Heart. 1984;51(2):175–8.
Huang SKS. Advances in applications of radiofrequency current to catheter ablation therapy. Pacing Clin Electrophysiol. 1991;14(1):28–42.
Olgin JE, Scheinman MM. Comparison of high energy direct current and radiofrequency catheter ablation of the atrioventricular junction. J Am Coll Cardiol. 1993;21(3):557–64.
Pappone C, Oral H, Santinelli V, Vicedomini G, Lang CC, Manguso F, et al. Atrio-esophageal fistula as a complication of percutaneous transcatheter ablation of atrial fibrillation. Circulation. 2004;109(22):2724–6.
Black-Maier E, Pokorney SD, Barnett AS, Zeitler EP, Sun AY, Jackson KP, et al. Risk of atrioesophageal fistula formation with contact force-sensing catheters. Heart Rhythm. 2017;14(9):1328–33.
Sacher F, Monahan KH, Thomas SP, Davidson N, Adragao P, Sanders P, et al. Phrenic nerve injury after atrial fibrillation catheter ablation: characterization and outcome in a multicenter study. J Am Coll Cardiol. 2006;47(12):2498–503.
Calkins H, Reynolds MR, Spector P, Sondhi M, Xu Y, Martin A, Williams CJ, Sledge I. Treatment of atrial fibrillation with anti–arrhythmic drugs or radio frequency ablation: two systematic literature reviews and meta–analyses. Circ Arrhythm Electrophysiol. 2009:CIRCEP. 108.824789.
Schrickel JW, Lickfett L, Lewalter T, Mittman-Braun E, Selbach S, Strach K, et al. Incidence and predictors of silent cerebral embolism during pulmonary vein catheter ablation for atrial fibrillation. Europace. 2010;12(1):52–7.
Medi C, Evered L, Silbert B, Teh A, Halloran K, Morton J, et al. Subtle post-procedural cognitive dysfunction after atrial fibrillation ablation. J Am Coll Cardiol. 2013;62(6):531–9.
Andrade JG, Dubuc M, Guerra PG, Macle L, Mondésert B, Rivard L, et al. The biophysics and biomechanics of cryoballoon ablation. Pacing Clin Electrophysiol. 2012;35(9):1162–8.
Furnkranz A, Bordignon S, Bohmig M, Konstantinou A, Dugo D, Perrotta L, et al. Reduced incidence of esophageal lesions by luminal esophageal temperature-guided second-generation cryoballoon ablation. Heart Rhythm. 2015;12(2):268–74.
Narui R, Tokuda M, Matsushima M, Isogai R, Tokutake K, Yokoyama K, et al. Incidence and factors associated with the occurrence of pulmonary vein narrowing after cryoballoon ablation. Circ Arrhythm Electrophysiol. 2017;10(6).
Ichihara N, Miyazaki S, Iwasawa J, Matsuda J, Taniguchi H, Nakamura H, et al. Prevalence and pre-procedural predictors associated with right phrenic nerve injury in electromyography-guided, second-generation cryoballoon ablation. JACC Clin Electrophysiol. 2016;2(4):508–14.
Aksu T, Ebru Golcuk S, Yalin K. Haemoptysis and pulmonary haemorrhage associated with cryoballoon ablation. Europace. 2015;17(8):1240.
Rems L, Miklavčič D. Tutorial: electroporation of cells in complex materials and tissue. J Appl Phys. 2016;119(20):201101.
Martin RC, McFarland K, Ellis S, Velanovich V. Irreversible electroporation in locally advanced pancreatic cancer: potential improved overall survival. Ann Surg Oncol. 2013;20(3):443–9.
Paiella S, Butturini G, Frigerio I, Salvia R, Armatura G, Bacchion M, et al. Safety and feasibility of irreversible electroporation (IRE) in patients with locally advanced pancreatic cancer: results of a prospective study. Dig Surg. 2015;32(2):90–7.
Valerio M, Stricker PD, Ahmed HU, Dickinson L, Ponsky L, Shnier R, et al. Initial assessment of safety and clinical feasibility of irreversible electroporation in the focal treatment of prostate cancer. Prostate Cancer Prostatic Dis. 2014;17(4):343–7.
Scheffer HJ, Nielsen K, de Jong MC, van Tilborg AA, Vieveen JM, Bouwman AR, et al. Irreversible electroporation for nonthermal tumor ablation in the clinical setting: a systematic review of safety and efficacy. J Vasc Interv Radiol. 2014;25(7):997–1011.
Welden CV, Christein JD, Wilcox CM, Ahmed AM. Initial experience of irreversible electroporation in the treatment of locally advanced pancreatic adenocarcinoma. Gastroenterology. 2017;152(5):S277.
Wojtaszczyk A, Caluori G, Pesl M, Melajova K, Starek Z. Irreversible electroporation ablation for atrial fibrillation. J Cardiovasc Electrophysiol. 2018;29(4):643–51.
Sugrue A, Maor E, Ivorra A, Vaidya V, Witt C, Kapa S, et al. Irreversible electroporation for the treatment of cardiac arrhythmias. Expert Rev Cardiovasc Ther. 2018;16(5):349–60.
Reddy VY, Koruth J, Jais P, Petru J, Timko F, Skalsky I, et al. Ablation of atrial fibrillation with pulsed electric fields: an ultra-rapid, tissue-selective modality for cardiac ablation. JACC Clin Electrophysiol. 2018:674.
Vries R, Hooijmans CR, Langendam MW, Luijk J, Leenaars M, Ritskes-Hoitinga M, et al. A protocol format for the preparation, registration and publication of systematic reviews of animal intervention studies. Evid Based Preclin Med. 2015;2(1):1–9.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Kilkenny C, Browne WJ, Cuthill IC, Emerson M, Altman DG. Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol. 2010;8(6):e1000412.
DeSimone CV, Ebrille E, Syed FF, Mikell SB, Suddendorf SH, Wahnschaffe D, et al. Novel balloon catheter device with pacing, ablating, electroporation, and drug-eluting capabilities for atrial fibrillation treatment--preliminary efficacy and safety studies in a canine model. Transl Res. 2014;164(6):508–14.
du Pre BC, van Driel VJ, van Wessel H, Loh P, Doevendans PA, Goldschmeding R, et al. Minimal coronary artery damage by myocardial electroporation ablation. Europace. 2013;15(1):144–9.
Hong J, Stewart MT, Cheek DS, Francischelli DE, Kirchhof N. Cardiac ablation via electroporation. Conf Proc IEEE Eng Med Biol Soc. 2009;2009:3381–4.
Lavee J, Onik G, Mikus P, Rubinsky B, editors. A novel nonthermal energy source for surgical epicardial atrial ablation: irreversible electroporation. Heart Surgery Forum; 2007: FORUM MULTIMEDIA PUBLISHING.
Madhavan M, Venkatachalam K, Swale MJ, Desimone CV, Gard JJ, Johnson SB, et al. Novel percutaneous epicardial autonomic modulation in the canine for atrial fibrillation: results of an efficacy and safety study. Pacing Clin Electrophysiol. 2016;39(5):407–17.
Neven K, van Driel V, van Wessel H, van Es R, Doevendans PA, Wittkampf F. Epicardial linear electroporation ablation and lesion size. Heart Rhythm. 2014;11(8):1465–70.
Neven K, van Driel V, van Wessel H, van Es R, Doevendans PA, Wittkampf F. Myocardial lesion size after epicardial electroporation catheter ablation following subxiphoid puncture. Circ Arrhythm Electrophysiol. 2014:CIRCEP. 114.001659.
Neven K, van Driel V, van Wessel H, van Es R, du Pre B, Doevendans PA, et al. Safety and feasibility of closed chest epicardial catheter ablation using electroporation. Circ Arrhythm Electrophysiol. 2014;7(5):913–9.
van Driel VJ, Neven K, van Wessel H, Vink A, Doevendans PA, Wittkampf FH. Low vulnerability of the right phrenic nerve to electroporation ablation. Heart Rhythm. 2015;12(8):1838–44.
van Driel VJ, Neven KG, van Wessel H, du Pre BC, Vink A, Doevendans PA, et al. Pulmonary vein stenosis after catheter ablation: electroporation versus radiofrequency. Circ Arrhythm Electrophysiol. 2014;7(4):734–8.
Wittkampf FH, van Driel VJ, van Wessel H, Neven KG, Grundeman PF, Vink A, et al. Myocardial lesion depth with circular electroporation ablation. Circ Arrhythm Electrophysiol. 2012;5(3):581–6.
Wittkampf FH, van Driel VJ, van Wessel H, Vink A, Hof IE, Grundeman PF, et al. Feasibility of electroporation for the creation of pulmonary vein ostial lesions. J Cardiovasc Electrophysiol. 2011;22(3):302–9.
Zager Y, Kain D, Landa N, Leor J, Maor E. Optimization of irreversible electroporation protocols for in-vivo myocardial decellularization. PLoS One. 2016;11(11):e0165475. PMCID: PMC5125564 a patent application entitled “Myocardial Ablation by Irreversible Electroporation” (Application #: US14/894,349). This patent relates in part to the results presented in this study. In addition, Dr. Maor has a granted patent entitled “Extracellular matrix material created using non-thermal irreversible electroporation” (US8835166 B2). There are no additional patents, products in development or marketed products to declare. This does not alter our adherence to all the PLOS ONE policies on sharing data and materials, as detailed online in the guide for authors.
Neven K, van Es R, van Driel V, van Wessel H, Fidder H, Vink A, et al. Acute and long-term effects of full-power electroporation ablation directly on the porcine esophagus. Circ Arrhythm Electrophysiol. 2017;10(5):e004672.
Livia C, Sugrue A, Witt T, Polkinghorne MD, Maor E, Kapa S, et al. Elimination of Purkinje fibers by electroporation reduces ventricular fibrillation vulnerability. J Am Heart Assoc. 2018;7(15):e009070.
Witt CM, Sugrue A, Padmanabhan D, Vaidya V, Gruba S, Rohl J, et al. Intrapulmonary vein ablation without stenosis: a novel balloon-based direct current electroporation approach. J Am Heart Assoc. 2018;7(14):e009575.
Thomson KR, Cheung W, Ellis SJ, Federman D, Kavnoudias H, Loader-Oliver D, et al. Investigation of the safety of irreversible electroporation in humans. J Vasc Interv Radiol. 2011;22(5):611–21.
Charpentier KP, Wolf F, Noble L, Winn B, Resnick M, Dupuy DE. Irreversible electroporation of the liver and liver hilum in swine. HPB. 2011;13(3):168–73.
Cannon R, Ellis S, Hayes D, Narayanan G, Martin RC 2nd. Safety and early efficacy of irreversible electroporation for hepatic tumors in proximity to vital structures. J Surg Oncol. 2013;107(5):544–9.
Mali B, Gorjup V, Edhemovic I, Brecelj E, Cemazar M, Sersa G, et al. Electrochemotherapy of colorectal liver metastases-an observational study of its effects on the electrocardiogram. Biomed Eng Online. 2015;14(3):S5.
Bertacchini C, Margotti PM, Bergamini E, Lodi A, Ronchetti M, Cadossi R. Design of an irreversible electroporation system for clinical use. Technol Cancer Res Treat. 2007;6(4):313–20.
Deodhar A, Dickfeld T, Single GW, Hamilton WC Jr, Thornton RH, Sofocleous CT, et al. Irreversible electroporation near the heart: ventricular arrhythmias can be prevented with ECG synchronization. Am J Roentgenol. 2011;196(3):W330–W5.
Reberšek M. Beyond electroporation pulse parameters: from application to evaluation. Handb Electroporation. 2017:1–21.
Schoenbach KH. From the basic science of biological effects of ultrashort electrical pulses to medical therapies. Bioelectromagnetics. 2018;39:257–76.
Mercadal B, Arena CB, Davalos RV, Ivorra A. Avoiding nerve stimulation in irreversible electroporation: a numerical modeling study. Phys Med Biol. 2017;62(20):8060–79.
Raso J, Frey W, Ferrari G, Pataro G, Knorr D, Teissie J, et al. Recommendations guidelines on the key information to be reported in studies of application of PEF technology in food and biotechnological processes. Innovative Food Sci Emerg Technol. 2016;37:312–21.
Cemazar M, Sersa G, Frey W, Miklavcic D, Teissié J. Recommendations and requirements for reporting on applications of electric pulse delivery for electroporation of biological samples. Bioelectrochemistry. 2018;122:69–76.
Campana LG, Clover AJ, Valpione S, Quaglino P, Gehl J, Kunte C, et al. Recommendations for improving the quality of reporting clinical electrochemotherapy studies based on qualitative systematic review. Radiol Oncol. 2016;50(1):1–13.
Acknowledgments
D.M. would like to acknowledge that this study was conducted within the scope of the LEA EBAM: European Laboratory of Pulsed Electric Fields Applications in Biology and Medicine (2011–2018).
Funding
The study was in part funded by the Slovenian Research Agency (ARRS) through ARRS research programme—Electroporation-based technologies and treatments (P2-0249, 2015–2020).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors SJA/SK/CW/CVD have filed but no issued patents within the realm of tools for electroporation. Author DM receives research funding and consulting fees from Medtronic. All other authors have no disclosures.
Ethical approval
For studies by the authors as include in this review, all applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 238 kb)
Rights and permissions
About this article
Cite this article
Sugrue, A., Vaidya, V., Witt, C. et al. Irreversible electroporation for catheter-based cardiac ablation: a systematic review of the preclinical experience. J Interv Card Electrophysiol 55, 251–265 (2019). https://doi.org/10.1007/s10840-019-00574-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-019-00574-3