Abstract
Purpose
Transcatheter aortic valve replacement (TAVR) is an increasingly prevalent therapy in patients with severe symptomatic aortic stenosis. Conduction disturbances requiring permanent pacemaker (PPM) implantation are a known complication of TAVR. This study investigated the progression of cardiac conduction disease in the post-TAVR pacemaker population and identified predictors of post-TAVR right ventricular (RV) pacing dependence.
Methods
Prospectively collected echocardiographic, ECG, and PPM interrogation data of 262 consecutive patients who underwent TAVR with placement of a balloon-expandable valve at one institution from March 2012 to October 2016 were analyzed.
Results
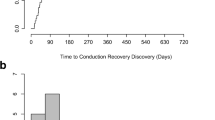
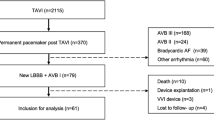
A total of 25 patients (11.1%) required post-TAVR PPM implantation. Seventeen patients who received PPMs did not require RV pacing at 30 days. Nine of these 17 patients had no RV pacing requirement within 10 days. Pre-existing right bundle branch block (RBBB) (OR 105.4, 4.52–2458.5, p = 0.0002), bifascicular block (OR 12.50, 1.60–97.65, p = 0.02), intra-procedural complete heart block (OR 12.83, 1.26–130.52, p = 0.03), and QRS duration > 120 ms (OR 70.43, 3.23–1535.22, p = 0.0002) on pre-TAVR ECG were associated with RV pacing dependence at 30 days.
Conclusions
Sixty-eight percent of patients meeting post-procedural guideline indications for PPM did not require RV pacing at 30 days. Fifty-two percent of these patients demonstrated recovery of sinus node function or AV conduction within 10 days post-implant. RBBB, intra-procedural complete heart block, bifascicular block, and QRS duration > 120 ms were associated with RV pacing dependence at 30 days. These findings suggest that post-TAVR conduction disturbances may be acutely reversible in a significant proportion of patients receiving PPM within 10–30 days of implant.

Similar content being viewed by others
Abbreviations
- TAVR:
-
Transcatheter aortic valve replacement
- PPM:
-
Permanent pacemaker
- RV:
-
Right ventricular
- MCV:
-
Medtronic CoreValve
- ESV:
-
Edwards SAPIEN valve
- ECG:
-
Electrocardiogram
- eGFR:
-
Estimated glomerular filtration rate
- LVOTd:
-
Left ventricular outflow tract diameter
- AV:
-
Atrioventricular
- BMI:
-
Body mass index
- CAD:
-
Coronary artery disease
- CHF:
-
Congestive heart failure
- COPD:
-
Chronic obstructive pulmonary disease
- PVD:
-
Peripheral vascular disease
- CABG:
-
Coronary artery bypass grafting
- PCI:
-
Percutaneous coronary intervention
- ACE-I/ARB:
-
Angiotensin-converting enzyme inhibitor/angiotensin receptor blocker
- LAFB:
-
Left anterior fascicular block
- LPFB:
-
Left posterior fascicular block
- LVEF:
-
Left ventricular ejection fraction
- LVEDd:
-
Left ventricular end diastolic diameter
References
Khatri PJ, Webb JG, Rodés-Cabau J, Fremes SE, Ruel M, Lau K, et al. Adverse effects associated with transcatheter aortic valve implantation: a meta-analysis of contemporary studies. Ann Intern Med. 2013;158(1):35–46. https://doi.org/10.7326/0003-4819-158-1-201301010-00007.
Jilaihawi H, Chakravarty T, Weiss RE, Fontana GP, Forrester J, Makkar RR. Meta-analysis of complications in aortic valve replacement: comparison of Medtronic-Corevalve, Edwards-Sapien and surgical aortic valve replacement in 8,536 patients. Catheter Cardiovasc Interv. 2012;80(1):128–38. https://doi.org/10.1002/ccd.23368.
Erkapic D, et al. Risk for permanent pacemaker after transcatheter aortic valve implantation: a comprehensive analysis of the literature. J Cardiovasc Electrophysiol. 2012;23(4):391–7. https://doi.org/10.1111/j.1540-8167.2011.02211.x.
Nazif TM, Dizon JM, Hahn RT, Xu K, Babaliaros V, Douglas PS, et al. Predictors and clinical outcomes of permanent pacemaker implantation after transcatheter aortic valve replacement: the PARTNER (Placement of AoRtic TraNscathetER Valves) trial and registry. JACC Cardiovasc Interv. 2015;8(1 Pt A):60–9. https://doi.org/10.1016/j.jcin.2014.07.022.
Kawashima T, Sato F. Visualizing anatomical evidences on atrioventricular conduction system for TAVI. Int J Cardiol. 2014;174(1):1–6. https://doi.org/10.1016/j.ijcard.2014.04.003.
Young Lee M, Chilakamarri Yeshwant S, Chava S, Lawrence Lustgarten D. Mechanisms of heart block after transcatheter aortic valve replacement – cardiac anatomy, clinical predictors and mechanical factors that contribute to permanent pacemaker implantation. Arrhythm Electrophysiol Rev. 2015;4(2):81–5. https://doi.org/10.15420/aer.2015.04.02.81.
Maan A, et al. Incidence and predictors of pacemaker implantation in patients undergoing transcatheter aortic valve replacement. Pacing Clin Electrophysiol. 2015;38(7):878–86. https://doi.org/10.1111/pace.12653.
Fadahunsi OO, Olowoyeye A, Ukaigwe A, Li Z, Vora AN, Vemulapalli S, et al. Incidence, predictors, and outcomes of permanent pacemaker implantation following transcatheter aortic valve replacement: analysis from the U.S. Society of Thoracic Surgeons/American College of Cardiology TVT Registry. JACC Cardiovasc Interv. 2016;9(21):2189–99. https://doi.org/10.1016/j.jcin.2016.07.026.
Simms AD, Hogarth AJ, Hudson EA, Worsnop VL, Blackman DJ, O'Regan DJ, et al. Ongoing requirement for pacing post-transcatheter aortic valve implantation and surgical aortic valve replacement. Interact Cardiovasc Thorac Surg. 2013;17(2):328–33. https://doi.org/10.1093/icvts/ivt175.
van der Boon RM, et al. Pacemaker dependency after transcatheter aortic valve implantation with the self-expanding Medtronic CoreValve System. Int J Cardiol. 2013;168(2):1269–73. https://doi.org/10.1016/j.ijcard.2012.11.115.
Schernthaner C, Kraus J, Danmayr F, Hammerer M, Schneider J, Hoppe UC, et al. Short-term pacemaker dependency after transcatheter aortic valve implantation. Wien Klin Wochenschr. 2016;128(5–6):198–203. https://doi.org/10.1007/s00508-015-0906-4.
Nagatomo T, et al. New onset of pacemaker dependency after permanent pacemaker implantation. Pacing Clin Electrophysiol. 2004;27(4):475–9. https://doi.org/10.1111/j.1540-8159.2004.00466.x.
Bagur R, Rodés-Cabau J, Gurvitch R, Dumont É, Velianou JL, Manazzoni J, et al. Need for permanent pacemaker as a complication of transcatheter aortic valve implantation and surgical aortic valve replacement in elderly patients with severe aortic stenosis and similar baseline electrocardiographic findings. JACC Cardiovasc Interv. 2012;5(5):540–51. https://doi.org/10.1016/j.jcin.2012.03.004.
Siontis GC, et al. Predictors of permanent pacemaker implantation in patients with severe aortic stenosis undergoing TAVR: a meta-analysis. J Am Coll Cardiol. 2014;64(2):129–40. https://doi.org/10.1016/j.jacc.2014.04.033.
Laynez A, Ben-Dor I, Barbash IM, Hauville C, Sardi G, Maluenda G, et al. Frequency of conduction disturbances after Edwards SAPIEN percutaneous valve implantation. Am J Cardiol. 2012;110(8):1164–8. https://doi.org/10.1016/j.amjcard.2012.05.057.
Nazif TM, Williams MR, Hahn RT, Kapadia S, Babaliaros V, Rodés-Cabau J, et al. Clinical implications of new-onset left bundle branch block after transcatheter aortic valve replacement: analysis of the PARTNER experience. Eur Heart J. 2014;35(24):1599–607. https://doi.org/10.1093/eurheartj/eht376.
Godin M, Eltchaninoff H, Furuta A, Tron C, Anselme F, Bejar K, et al. Frequency of conduction disturbances after transcatheter implantation of an Edwards Sapien aortic valve prosthesis. Am J Cardiol. 2010;106(5):707–12. https://doi.org/10.1016/j.amjcard.2010.04.029.
Sinhal A, Altwegg L, Pasupati S, Humphries KH, Allard M, Martin P, et al. Atrioventricular block after transcatheter balloon expandable aortic valve implantation. JACC Cardiovasc Interv. 2008;1(3):305–9. https://doi.org/10.1016/j.jcin.2007.12.009.
Piazza N, de Jaegere P, Schultz C, Becker AE, Serruys PW, Anderson RH. Anatomy of the aortic valvar complex and its implications for transcatheter implantation of the aortic valve. Circ Cardiovasc Interv. 2008;1(1):74–81. https://doi.org/10.1161/CIRCINTERVENTIONS.108.780858.
Moreno R, Dobarro D, Lopez de Sa E, Prieto M, Morales C, Calvo Orbe L, et al. Cause of complete atrioventricular block after percutaneous aortic valve implantation: insights from a necropsy study. Circulation. 2009;120(5):e29–30. https://doi.org/10.1161/CIRCULATIONAHA.109.849281.
Urena M, Mok M, Serra V, Dumont E, Nombela-Franco L, DeLarochellière R, et al. Predictive factors and long-term clinical consequences of persistent left bundle branch block following transcatheter aortic valve implantation with a balloon-expandable valve. J Am Coll Cardiol. 2012;60(18):1743–52. https://doi.org/10.1016/j.jacc.2012.07.035.
Husser O, Pellegrini C, Kessler T, Burgdorf C, Thaller H, Mayr NP, et al. Predictors of permanent pacemaker implantations and new-onset conduction abnormalities with the SAPIEN 3 balloon-expandable transcatheter heart valve. JACC Cardiovasc Interv. 2016;9(3):244–54. https://doi.org/10.1016/j.jcin.2015.09.036.
Dvir D, Webb JG, Piazza N, Blanke P, Barbanti M, Bleiziffer S, et al. Multicenter evaluation of transcatheter aortic valve replacement using either SAPIEN XT or CoreValve: degree of device oversizing by computed-tomography and clinical outcomes. Catheter Cardiovasc Interv. 2015;86(3):508–15. https://doi.org/10.1002/ccd.25823.
Yang TH, Webb JG, Blanke P, Dvir D, Hansson NC, Nørgaard BL, et al. Incidence and severity of paravalvular aortic regurgitation with multidetector computed tomography nominal area oversizing or undersizing after transcatheter heart valve replacement with the Sapien 3: a comparison with the Sapien XT. JACC Cardiovasc Interv. 2015;8(3):462–71. https://doi.org/10.1016/j.jcin.2014.10.014.
Epstein AE, DiMarco JP, Ellenbogen KA, Estes NA 3rd, Freedman RA, Gettes LS, et al. ACC/AHA/HRS 2008 guidelines for device-based therapy of cardiac rhythm abnormalities: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing committee to revise the ACC/AHA/NASPE 2002 guideline update for implantation of cardiac pacemakers and antiarrhythmia devices) developed in collaboration with the American Association for Thoracic Surgery and Society of Thoracic Surgeons. J Am Coll Cardiol. 2008;51(21):e1–62. https://doi.org/10.1016/j.jacc.2008.02.032.
Lamas GA, Lee KL, Sweeney MO, Silverman R, Leon A, Yee R, et al. Ventricular pacing or dual-chamber pacing for sinus-node dysfunction. N Engl J Med. 2002;346(24):1854–62. https://doi.org/10.1056/NEJMoa013040.
Sweeney MO, Hellkamp AS, Ellenbogen KA, Greenspon AJ, Freedman RA, Lee KL, et al. Adverse effect of ventricular pacing on heart failure and atrial fibrillation among patients with normal baseline QRS duration in a clinical trial of pacemaker therapy for sinus node dysfunction. Circulation. 2003;107(23):2932–7. https://doi.org/10.1161/01.CIR.0000072769.17295.B1.
Tops LF, Schalij MJ, Bax JJ. The effects of right ventricular apical pacing on ventricular function and dyssynchrony implications for therapy. J Am Coll Cardiol. 2009;54(9):764–76. https://doi.org/10.1016/j.jacc.2009.06.006.
De Sisti A, et al. Adverse effects of long-term right ventricular apical pacing and identification of patients at risk of atrial fibrillation and heart failure. Pacing Clin Electrophysiol. 2012;35(8):1035–43. https://doi.org/10.1111/j.1540-8159.2012.03371.x.
Wilkoff BL, Cook JR, Epstein AE, Greene HL, Hallstrom AP, Hsia H, et al. Dual-chamber pacing or ventricular backup pacing in patients with an implantable defibrillator: the Dual Chamber and VVI Implantable Defibrillator (DAVID) Trial. JAMA. 2002;288(24):3115–23.
Urena M, Webb JG, Tamburino C, Munoz-Garcia AJ, Cheema A, Dager AE, et al. Permanent pacemaker implantation after transcatheter aortic valve implantation: impact on late clinical outcomes and left ventricular function. Circulation. 2014;129(11):1233–43. https://doi.org/10.1161/CIRCULATIONAHA.113.005479.
De Carlo M, Giannini C, Bedogni F, Klugmann S, Brambilla N, de Marco F, et al. Safety of a conservative strategy of permanent pacemaker implantation after transcatheter aortic CoreValve implantation. Am Heart J. 2012;163(3):492–9. https://doi.org/10.1016/j.ahj.2011.12.009.
Binder RK, Webb JG, Toggweiler S, Freeman M, Barbanti M, Willson AB, et al. Impact of post-implant SAPIEN XT geometry and position on conduction disturbances, hemodynamic performance, and paravalvular regurgitation. JACC Cardiovasc Interv. 2013;6(5):462–8. https://doi.org/10.1016/j.jcin.2012.12.128.
Mauri V, Reimann A, Stern D, Scherner M, Kuhn E, Rudolph V, et al. Predictors of permanent pacemaker implantation after transcatheter aortic valve replacement with the SAPIEN 3. JACC Cardiovasc Interv. 2016;9(21):2200–9. https://doi.org/10.1016/j.jcin.2016.08.034.
Tarantini G, Mojoli M, Purita P, Napodano M, D’Onofrio A, Frigo A, et al. Unravelling the (arte)fact of increased pacemaker rate with the Edwards SAPIEN 3 valve. EuroIntervention. 2015;11(3):343–50. https://doi.org/10.4244/EIJY14M11_06.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Fig. S1
(DOCX 109 kb)
Rights and permissions
About this article
Cite this article
Sharma, E., Chu, A.F. Predictors of right ventricular pacing and pacemaker dependence in transcatheter aortic valve replacement patients. J Interv Card Electrophysiol 51, 77–86 (2018). https://doi.org/10.1007/s10840-017-0303-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-017-0303-1