Abstract
Background
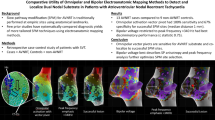
Atrial fibrillation (AF) and cavotricuspid isthmus (CTI)-dependent atrial flutter (AFL) are two separate entities that coexist in a significant percentage of patients. We sought to investigate whether AF inducibility during CTI AFL ablation predicted the occurrence of AF at follow-up after successful AFL ablation.
Methods
A systemic review of Medline, Cochrane, and Embase was done for all the clinical studies in which assessment of AF inducibility in patients undergoing ablation for CTI AFL was performed. Given the low heterogeneity (i.e., I 2 <25), we used a fixed effect model for our analysis.
Results
A total of 10 studies (4 prospective and 6 retrospective) with a total of 1299 patients (male, 73%; mean age 59 ± 11 years) fulfilled the inclusion criteria. During a mean follow-up period of 23 ± 7.6 months, 407 patients (31%) developed AF during AFL ablation. The overall incidence for new-onset AF during follow-up was 29% (47% in the group with inducible AF vs. 21% in the non-inducible group). The odds ratio (OR) for developing AF after AFL ablation in patients with AF inducibility for all studies combined was 3.72, 95% CI 2.83–4.89 [prospective studies (OR 5.52, 95% CI 3.23–9.41) vs. retrospective studies (OR 3.23, 95% CI 2.35–4.45)].
Conclusions
Although ablation for CTI AFL is highly effective, AF continues to be a long-term risk for individuals undergoing this procedure. AF induced by pacing protocols in patients undergoing CTI AFL predicts for future AF. Inducible AF is a clinically relevant finding that may help guide decisions for long-term anticoagulation after successful typical AFL ablation especially in patients with elevated CHADS-VASc scores (≥2) and in considering prophylactic PVI during CTI AFL ablation.




Similar content being viewed by others
Abbreviations
- AF:
-
Atrial fibrillation
- AFL:
-
Atrial flutter
- CTI:
-
Cavotricuspid isthmus
- LAE:
-
Left atrial enlargement
- AAD:
-
Antiarrhythmic drugs
- CA:
-
Catheter ablation
- CI:
-
Confidence interval
- LV:
-
Left ventricle
- LVEF:
-
Left ventricular ejection fraction
- RFA:
-
Radiofrequency ablation
- OR:
-
Odds ratio
References
Tomson TT et al. Risk of stroke and atrial fibrillation after radiofrequency catheter ablation of typical atrial flutter. Heart Rhythm. 2012;9(11):1779–84.
Verma A et al. Canadian Cardiovascular Society atrial fibrillation guidelines 2010: catheter ablation for atrial fibrillation/atrial flutter. Can J Cardiol. 2011;27(1):60–6.
Wells GA, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of non-randomized studies in meta-analyses. Accessed on April 12th, 2016.
Moher D et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177–88.
Egger M et al. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315(7109):629–34.
Altman DG, Bland JM. Interaction revisited: the difference between two estimates. BMJ. 2003;326(7382):219.
Baszko A et al. Occurrence of atrial fibrillation after flutter ablation: the significance of intra-atrial conduction and atrial vulnerability. J Electrocardiol. 2003;36(3):219–25.
Haghjoo M et al. Predictors of the atrial fibrillation following catheter ablation of typical atrial flutter. Res Cardiovasc Med. 2013;2(2):90–4.
Hsieh MH et al. Recurrent atrial flutter and atrial fibrillation after catheter ablation of the cavotricuspid isthmus: a very long-term follow-up of 333 patients. J Interv Card Electrophysiol. 2002;7(3):225–31.
Joza J, et al. Prognostic value of atrial fibrillation inducibility after right atrial flutter ablation. Heart Rhythm. 2014.
Paydak H et al. Atrial fibrillation after radiofrequency ablation of type I atrial flutter: time to onset, determinants, and clinical course. Circulation. 1998;98(4):315–22.
Philippon F et al. The risk of atrial fibrillation following radiofrequency catheter ablation of atrial flutter. Circulation. 1995;92(3):430–5.
Anselme F et al. Radiofrequency catheter ablation of common atrial flutter: significance of palpitations and quality-of-life evaluation in patients with proven isthmus block. Circulation. 1999;99(4):534–40.
Laurent V et al. Incidence and predictive factors of atrial fibrillation after ablation of typical atrial flutter. J Interv Card Electrophysiol. 2009;24(2):119–25.
Tai CT et al. Long-term outcome of radiofrequency catheter ablation for typical atrial flutter: risk prediction of recurrent arrhythmias. J Cardiovasc Electrophysiol. 1998;9(2):115–21.
Romero J, Estrada R, Holmes A, Goodman D, Roth N, Golive A, et al. Prediction of clinical atrial fibrillation induced during typical atrial flutter ablation. Circulation. 2014;130:A19766.
Chinitz JS et al. Atrial fibrillation is common after ablation of isolated atrial flutter during long-term follow-up. Heart Rhythm. 2007;4(8):1029–33.
Chen K et al. HATCH score in the prediction of new-onset atrial fibrillation after catheter ablation of typical atrial flutter. Heart Rhythm. 2015;12(7):1483–9.
Katritsis D et al. Ablation therapy of type I atrial flutter may eradicate paroxysmal atrial fibrillation. Am J Cardiol. 1996;78(3):345–7.
Navarrete A et al. Ablation of atrial fibrillation at the time of cavotricuspid isthmus ablation in patients with atrial flutter without documented atrial fibrillation derives a better long-term benefit. J Cardiovasc Electrophysiol. 2011;22(1):34–8.
Steinberg JS et al. Prophylactic pulmonary vein isolation during isthmus ablation for atrial flutter: the PReVENT AF Study I. Heart Rhythm. 2014;11(9):1567–72.
Schneider R et al. Pulmonary vein triggers play an important role in the initiation of atrial flutter: initial results from the prospective randomized Atrial Fibrillation Ablation in Atrial Flutter (Triple A) trial. Heart Rhythm. 2015;12(5):865–71.
Wazni O et al. Randomized study comparing combined pulmonary vein-left atrial junction disconnection and cavotricuspid isthmus ablation versus pulmonary vein-left atrial junction disconnection alone in patients presenting with typical atrial flutter and atrial fibrillation. Circulation. 2003;108(20):2479–83.
Mohanty S et al. Results from a single-blind, randomized study comparing the impact of different ablation approaches on long-term procedure outcome in coexistent atrial fibrillation and flutter (APPROVAL). Circulation. 2013;127(18):1853–60.
Maan A et al. Complications from catheter ablation of atrial fibrillation: a systematic review. Crit Pathw Cardiol. 2011;10(2):76–83.
Deshmukh A et al. In-hospital complications associated with catheter ablation of atrial fibrillation in the United States between 2000 and 2010: analysis of 93 801 procedures. Circulation. 2013;128(19):2104–12.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Dr Di Biase is a consultant for Biosense Webster, Boston Scientific, and St. Jude Medical and has received speaker honoraria/travel from Medtronic, Atricure, EPiEP, and Biotronik. Dr. Kumar is a recipient of the Neil Hamilton Fairley Overseas Research scholarship co-funded by the National Health and Medical Research Council and the National Heart Foundation of Australia; and the Bushell Travelling Fellowship funded by the Royal Australasian College of Physicians and the Postdoctoral Research Fellowship by the American Heart Association. Dr. Tedrow receives consulting fees/honoraria from Boston Scientific Corp. and St. Jude Medical and research funding from Biosense Webster, Inc., and St. Jude Medical. Dr. John receives consulting fees/honoraria from St. Jude Medical. Dr. Michaud receives consulting fees/honoraria from Boston Scientific Corp., Medtronic, Inc., and St. Jude Medical, and research funding from Boston Scientific Corp. and Biosense Webster, Inc. Dr. Stevenson is co-holder of a patent for needle ablation that is consigned to Brigham and Women’s Hospital. The remaining authors have no disclosures.
Rights and permissions
About this article
Cite this article
Romero, J., Diaz, J.C., Di Biase, L. et al. Atrial fibrillation inducibility during cavotricuspid isthmus-dependent atrial flutter ablation as a predictor of clinical atrial fibrillation. A meta-analysis. J Interv Card Electrophysiol 48, 307–315 (2017). https://doi.org/10.1007/s10840-016-0211-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-016-0211-9