Abstract
Objective
Postoperative atrial fibrillation (POAF) complicating coronary artery bypass grafting surgery (CABG) increases morbidity and stroke risk. Total atrial conduction time (PA-TDI duration) has been identified as an independent predictor of new-onset atrial fibrillation (AF). We aimed to assess whether PA-TDI duration is a predictor of AF after CABG.
Methods
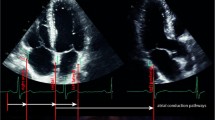
In 128 patients who had undergone CABG, preoperative clinical and echocardiographic data were compared between patients with and without POAF. The PA-TDI duration was assessed by measuring the time interval between the beginning of the P wave on the surface ECG and point of the peak A wave on TDI from left atrium (LA) lateral wall just over the mitral annulus.
Results
Patients with POAF (38/128, 29.6 %) were older (68.1 ± 11.1 vs. 59.3 ± 10.2 years; p < 0.001), had higher LA maximum volume, had prolonged PA-TDI duration, and had lower ejection fraction compared with patients without POAF. PA-TDI duration was found to be significantly increased in POAF group (134.3 ± 19.7 vs. 112.5 ± 17.7 ms; p = 0.01). On multivariate analysis, age (95 % CI = 1.03–1.09; p = 0.003), LA maximum volume (95 % CI = 1.01–1.06; p = 0.03), and prolonged PA-TDI duration (95 % CI, 1.02–1.05; p = 0.001) were found to be the independent risk factors of POAF.
Conclusions
In this study, LA maximum volume and PA-TDI duration were found to be the independent predictors of the development of POAF after CABG. Echocardiographic predictors of left atrial electromechanical dysfunction may be useful in risk stratifying of patients in terms of POAF development after CABG.



Similar content being viewed by others
References
Amar, D., Shi, W., Hogue, C. W., Jr., et al. (2004). Clinical prediction rule for atrial fibrillation after coronary artery bypass grafting. Journal of the American College of Cardiology, 44, 1248–1253.
Hogue, C. W., & Hyder, M. L. (2000). Atrial fibrillation after cardiac operation: risks, mechanisms, and treatment. The Annals of Thoracic Surgery, 69, 300–306.
Mathew, J. P., Fontes, M. L., Tudor, I. C., et al. (2004). A multicenter risk index for atrial fibrillation after cardiac surgery. Journal of the American Medical Association, 291, 1720–1729.
Villareal, R. P., Hariharan, R., Liu, B. C., et al. (2004). Postoperative atrial fibrillation and mortality after coronary artery bypass surgery. Journal of the American College of Cardiology, 43, 742–748.
Mahoney, E. M., Thompson, T. D., Veledar, E., Williams, J., & Weintraub, W. S. (2002). Cost-effectiveness of targeting patients undergoing cardiac surgery for therapy with intravenous amiodarone to prevent atrial fibrillation. Journal of the American College of Cardiology, 40, 737–742.
Sezai, A., Hata, M., Niino, T., et al. (2009). Study of the factors related to atrial fibrillation after coronary artery bypass grafting: a search for a marker to predict the occurrence of atrial fibrillation before surgical intervention. The Journal of Thoracic and Cardiovascular Surgery, 137, 895–900.
El-Chami, M. F., Kilgo, P., Thourani, V., et al. (2010). New-onset atrial fibrillation predicts long-term mortality after coronary artery bypass graft. Journal of the American College of Cardiology, 55, 1370–1376.
Shen, J., Lall, S., Zheng, V., Buckley, P., Damiano, R. J., & Schuessler, R. B. (2011). The persistent problem of new-onset postoperative atrial fibrillation: a single institution experience over two decades. The Journal of Thoracic and Cardiovascular Surgery, 141, 559–570.
Den Uijl, D. W., Gawrysiak, M., Tops, L. F., Trines, S. A., Zeppenfeld, K., Schalij, M. J., et al. (2011). Prognostic value of total atrial conduction time estimated with tissue Doppler imaging to predict the recurrence of atrial fibrillation after radiofrequency catheter ablation. Europace, 13, 1533–1540.
Merckx, K. L., De Vos, C. B., Palmans, A., Habets, J., Cheriex, E. C., Crijns, H. J., et al. (2005). Atrial activation time determined by transthoracic Doppler tissue imaging can be used as an estimate of the total duration of atrial electrical activation. Journal of the American Society of Echocardiography, 18(9), 940–944.
Lang, R. M., Bierig, M., Devereux, R. B., Flachskampf, F. A., Foster, E., Pellikka, P. A., et al. (2005). Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. Journal of the American Society of Echocardiography, 18, 1440–1463.
Quinones, M. A., Otto, C. M., Stoddard, M., Waggoner, A., & Zoghbi, W. A. (2002). Doppler echocardiography: a report from the Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography. Journal of the American Society of Echocardiography, 15, 167–184.
Acar, G., Akcay, A., Sökmen, A., Özkaya, M., Güler, E., Sökmen, G., et al. (2009). Assessment of atrial electromechanical delay, diastolic functions, and left atrial mechanical functions in patients with type 1 diabetes mellitus. Journal of the American Society of Echocardiography, 22, 732–738.
Antoni, M. L., Bertini, M., Atary, J. Z., Delgado, V., ten Brinke, E. A., Boersma, E., et al. (2010). Predictive value of total atrial conduction time estimated with tissue Doppler imaging for the development of new-onset atrial fibrillation after acute myocardial infarction. The American Journal of Cardiology, 106(2), 198–203.
Steinberg, J. S. (2004). Postoperative atrial fibrillation: a billion-dollar problem. Journal of the American College of Cardiology, 43, 1001–1003.
Blommaert, D., Gonzalez, M., Mucumbitsi, J., et al. (2000). Effective prevention of atrial fibrillation by continuous atrial overdrive pacing after coronary artery bypass surgery. Journal of the American College of Cardiology, 35, 1411–1415.
Budeus, M., Hennersdorf, M., Perings, S., et al. (2006). Amiodarone prophylaxis for atrial fibrillation of high risk patients after coronary bypass grafting: a prospective, double blinded, placebo controlled, randomized study. European Heart Journal, 27, 1584–1591.
Açil, T., Cölkesen, Y., Türköz, R., et al. (2007). Value of preoperative echocardiography in the prediction of postoperative atrial fibrillation following isolated coronary artery bypass grafting. The American Journal of Cardiology, 100(9), 1383–1386.
Osranek, M., Fatema, K., Qaddoura, F., et al. (2006). Left atrial volume predicts the risk of atrial fibrillation after cardiac surgery: a prospective study. Journal of the American College of Cardiology, 48, 779–786.
Davies, M., & Pomerance, A. (1972). Pathology of atrial fibrillation in man. British Heart Journal, 34, 520–525.
Nardi, F., Diena, M., Caimmi, P. P., Iraghi, G., Lazzero, M., Cerin, G., et al. (2012). Relationship between left atrial volume and atrial fibrillation following coronary artery bypass grafting. Journal of Cardiac Surgery, 27(1), 128–135.
Gaspo, R., Bosch, R. F., Talajic, M., & Nattel, S. (1997). Functional mechanisms underlying tachycardia-induced sustained atrial fibrillation in a chronic dog model. Circulation, 96, 4027–4035.
Choi, J. I., Ryu, K., Park, E., Benser, M. E., Jang, J. K., Lee, H. S., et al. (2010). Atrial activation time and pattern of linear triple-site vs. single-site atrial pacing after cardioversion in patients with atrial fibrillation. Europace, 12, 508–516.
De Vos, C. B., Weijs, B., Crijns, H. J., Cheriex, E. C., Palmans, A., Habets, J., et al. (2009). Atrial tissue Doppler imaging for prediction of new-onset atrial fibrillation. Heart, 95, 835–840.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Özlü, M.F., Erdem, K., Kırış, G. et al. Predictive value of total atrial conduction time measured with tissue Doppler imaging for postoperative atrial fibrillation after coronary artery bypass surgery. J Interv Card Electrophysiol 37, 27–33 (2013). https://doi.org/10.1007/s10840-012-9756-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-012-9756-4