Abstract
Purpose
We sought to explore the utility of preimplantation genetic testing for aneuploidy (PGT-A) in a poor prognosis group of women with few embryos available for transfer.
Methods
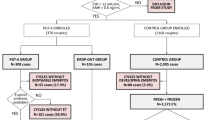
This was a retrospective matched cohort study examining records for first or second-cycle IVF patients with 1 to 3 blastocysts. The study group comprised 130 patients who underwent PGT-A on all embryos. The control group included 130 patients matched by age, BMI, and blastocyst number and quality who did not undergo PGT-A during the same time period.
Results
The live birth rate (LBR) per embryo transfer (ET) were similar in the PGT-A and control groups, and the spontaneous abortion (SAB) rate was the same (23%). However, we found a significantly higher LBR per oocyte retrieval in the control group vs the PGT-A group (43% vs 20%, respectively) likely due to the many no-euploid cycles in the PGT-A group. In a subgroup analysis for age, the similar LBR per ET persisted in women < 38. However, in older women, there was a trend to a higher LBR per ET in the PGT-A group (43%) vs the control group (22%) but a higher LBR per oocyte retrieval in the control group (31%) vs the PGT-A group (13%).
Conclusions
Overall, we observed a significant increase in LBR per oocyte retrieval in women in the control group compared to women undergoing PGT-A, and no difference in SAB rate. Our data suggests that PGT-A has no benefit in a subpopulation of women with few embryos and may cause harm.




Similar content being viewed by others
Change history
03 October 2022
A Correction to this paper has been published: https://doi.org/10.1007/s10815-022-02631-9
References
Gleicher N, Orvieto R. “Is the hypothesis of preimplantation genetic screening (PGS) still supportable? A review,” (in eng). J Ovarian Res. 2017;10(1):21. https://doi.org/10.1186/s13048-017-0318-3.
Gleicher N, Patrizio P, Orvieto R. “How not to introduce laboratory tests to clinical practice: preimplantation genetic testing for aneuploidy,” (in eng). Clin Chem. 2022;68(4):501–3. https://doi.org/10.1093/clinchem/hvac001.
Yang M, et al. “Author Correction: Depletion of aneuploid cells in human embryos and gastruloids,” (in eng). Nat Cell Biol. 2021;23(11):1212. https://doi.org/10.1038/s41556-021-00775-x.
Bolton H, et al. “Mouse model of chromosome mosaicism reveals lineage-specific depletion of aneuploid cells and normal developmental potential,” (in eng). Nat Commun. 2016;7:11165. https://doi.org/10.1038/ncomms11165.
Kang HJ, Melnick AP, Stewart JD, Xu K, Rosenwaks Z. “Preimplantation genetic screening: who benefits?,” (in eng). Fertil Steril. 2016;106(3):597–602. https://doi.org/10.1016/j.fertnstert.2016.04.027.
Munné S, et al. “Preimplantation genetic testing for aneuploidy versus morphology as selection criteria for single frozen-thawed embryo transfer in good-prognosis patients: a multicenter randomized clinical trial,” (in eng). Fertil Steril. 2019;112(6):1071-1079.e7. https://doi.org/10.1016/j.fertnstert.2019.07.1346.
Rubio C, et al. “In vitro fertilization with preimplantation genetic diagnosis for aneuploidies in advanced maternal age: a randomized, controlled study,” (in eng). Fertil Steril. 2017;107(5):1122–9. https://doi.org/10.1016/j.fertnstert.2017.03.011.
Yan J, et al. “Live Birth with or without preimplantation genetic testing for aneuploidy,” (in eng). N Engl J Med. 2021;385(22):2047–58. https://doi.org/10.1056/NEJMoa2103613.
Meriano JS, Alexis J, Visram-Zaver S, Cruz M, Casper RF. “Tracking of oocyte dysmorphisms for ICSI patients may prove relevant to the outcome in subsequent patient cycles,” (in eng). Hum Reprod. 2001;16(10):2118–23. https://doi.org/10.1093/humrep/16.10.2118.
Rama Raju GA, Prakash GJ, Krishna KM, Madan K. “Meiotic spindle and zona pellucida characteristics as predictors of embryonic development: a preliminary study using PolScope imaging,” (in eng). Reprod Biomed Online. 2007;14(2):166–74. https://doi.org/10.1016/s1472-6483(10)60784-5.
Gardner DK, Lane M. “Culture and selection of viable blastocysts: a feasible proposition for human IVF?,” (in eng). Hum Reprod Update. 1997;3(4):367–82. https://doi.org/10.1093/humupd/3.4.367.
Moreno I, et al. “Evidence that the endometrial microbiota has an effect on implantation success or failure,” (in eng). Am J Obstet Gynecol. 2016;215(6):684–703. https://doi.org/10.1016/j.ajog.2016.09.075.
Franasiak JM, Scott RT. “Contribution of immunology to implantation failure of euploid embryos,” (in eng). Fertil Steril. 2017;107(6):1279–83. https://doi.org/10.1016/j.fertnstert.2017.04.019.
Franasiak JM, et al. “The nature of aneuploidy with increasing age of the female partner: a review of 15,169 consecutive trophectoderm biopsies evaluated with comprehensive chromosomal screening,” (in eng). Fertil Steril. 2014;101(3):656-663.e1. https://doi.org/10.1016/j.fertnstert.2013.11.004.
Domar AD, Smith K, Conboy L, Iannone M, Alper M. “A prospective investigation into the reasons why insured United States patients drop out of in vitro fertilization treatment,” (in eng). Fertil Steril. 2010;94(4):1457–9. https://doi.org/10.1016/j.fertnstert.2009.06.020.
Chen M, Wei S, Hu J, Quan S. “Can comprehensive chromosome screening technology improve IVF/ICSI outcomes? A Meta-Analysis,” (in eng). PLoS One. 2015;10(10):e0140779. https://doi.org/10.1371/journal.pone.0140779.
Maxwell SM, McCulloh DH, Lee H, Berkeley AS, Grifo J. Preimplantation genetic screening (PGS) with next generation sequencing (NGS) achieves ongoing pregnancy with fewer transfers and total miscarriages compared to non-PGS cycles. Fertil Steril. 2017;108(3):e20. https://doi.org/10.1016/j.fertnstert.2017.07.082.
Murphy LA, et al. To test or not to test? A framework for counselling patients on preimplantation genetic testing for aneuploidy (PGT-A). Hum Reprod. 2018;34(2):268–75. https://doi.org/10.1093/humrep/dey346.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: In Fig. 3 of this article the bars were incorrect. The figure should have appeared as shown below.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mahesan, A.M., Chang, P.T., Ronn, R. et al. Preimplantation genetic testing for aneuploidy in patients with low embryo numbers: benefit or harm?. J Assist Reprod Genet 39, 2027–2033 (2022). https://doi.org/10.1007/s10815-022-02588-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-022-02588-9