Abstract
Purpose
The use of platelet-rich plasma is being investigated in reproductive medicine and clinically promoted as a fertility treatment for menopause. We aimed to review the literature on the impact of PRP on fertility in menopause.
Methods
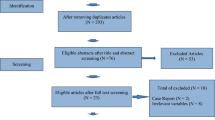
A literature search was performed using the PubMed and MEDLINE search engines. The search was limited to the English language. Articles studying PRP use in menopause were selected for the purpose of this review.
Results
Limited case reports and case series studied fertility outcomes of PRP in menopause. Randomized controlled trials are lacking. Furthermore, no studies have been conducted to evaluate the effect of different PRP concentrations, injection techniques, or side effects on reproductive outcomes in menopausal women.
Conclusion
There is a dearth of data to support the routine implementation of intraovarian PRP injections for fertility restoration in menopausal women. Patients considering such therapy need to be well aware of the lack of adequate data for PRP use in menopause and should be counseled accordingly.
Similar content being viewed by others
References
Alves R, Grimalt R. A review of platelet-rich plasma: history, biology, mechanism of action, and classification. Skin Appendage Disorders. 2018;4(1):18–24.
Dawood AS, Salem HA. Current clinical applications of platelet-rich plasma in various gynecological disorders: an appraisal of theory and practice. Clin Exp Reprod Med. 2018;45(2):67–74.
Seckin S, et al. Ovarian response to intraovarian platelet-rich plasma (PRP) administration: hypotheses and potential mechanisms of action. J Assist Reprod Genet. 2022;39(1):37–61.
Lai LP, et al. Use of platelet-rich plasma in intra-articular knee injections for osteoarthritis: a systematic review. Pm r. 2015;7(6):637–48.
Mishra A, et al. Sports medicine applications of platelet rich plasma. Curr Pharm Biotechnol. 2012;13(7):1185–95.
Everts PA, et al. Is the use of autologous platelet-rich plasma gels in gynecologic, cardiac, and general, reconstructive surgery beneficial? Curr Pharm Biotechnol. 2012;13(7):1163–72.
Nazaroff J, et al. Reporting in clinical studies on platelet-rich plasma therapy among all medical specialties: a systematic review of Level I and II studies. PLoS One. 2021;16(4):e0250007.
Lin Y, Qi J, Sun Y. Platelet-rich plasma as a potential new strategy in the endometrium treatment in assisted reproductive technology. Front Endocrinol. 2021;12.
Sharara FI, et al. A narrative review of platelet-rich plasma (PRP) in reproductive medicine. J Assist Reprod Genet. 2021;38(5):1003–12.
White YA, et al. Oocyte formation by mitotically active germ cells purified from ovaries of reproductive-age women. Nat Med. 2012;18(3):413–21.
Broekmans FJ, Soules MR, Fauser BC. Ovarian aging: mechanisms and clinical consequences. Endocr Rev. 2009;30(5):465–93.
Ozakpinar OB, Maurer AM, Ozsavci D. Ovarian stem cells: from basic to clinical applications. World J Stem Cells. 2015;7(4):757–68.
Wagner M, et al. Single-cell analysis of human ovarian cortex identifies distinct cell populations but no oogonial stem cells. Nat Commun. 2020;11(1):1147.
Vollenhoven B, Hunt S. Ovarian ageing and the impact on female fertility. F1000Res. 2018;7.
Hsu CC, et al. Resumed ovarian function and pregnancy in early menopausal women by whole dimension subcortical ovarian administration of platelet-rich plasma and gonadotropins. Menopause. 2021;28(6):660–6.
Sills ES, Wood SH. Autologous activated platelet-rich plasma injection into adult human ovary tissue: molecular mechanism, analysis, and discussion of reproductive response. Biosci Rep. 2019;39(6).
Battinelli EM, Markens BA, Italiano JE Jr. Release of angiogenesis regulatory proteins from platelet alpha granules: modulation of physiologic and pathologic angiogenesis. Blood. 2011;118(5):1359–69.
Wood SH, Sills ES. Intraovarian vascular enhancement via stromal injection of platelet-derived growth factors: exploring subsequent oocyte chromosomal status and in vitro fertilization outcomes. Clin Exp Reprod Med. 2020;47(2):94–100.
Talevi R, et al. Is oxygen availability a limiting factor for in vitro folliculogenesis? PLoS One. 2018;13(2):e0192501.
Sills ES, Wood SH. Progress in human ovarian rejuvenation: current platelet-rich plasma and condensed cytokine research activity by scope and international origin. Clin Exp Reprod Med. 2021;48(4):311–5.
Sills ES. The scientific and cultural journey to ovarian rejuvenation: background, barriers, and beyond the biological clock. Medicines (Basel). 2021;8(6).
Boudreau LH, et al. Platelets release mitochondria serving as substrate for bactericidal group IIA-secreted phospholipase A2 to promote inflammation. Blood. 2014;124(14):2173–83.
Golan K, et al. Bone marrow regeneration requires mitochondrial transfer from donor Cx43-expressing hematopoietic progenitors to stroma. Blood. 2020;136(23):2607–19.
Sfakianoudis K, et al. Autologous platelet-rich plasma treatment enables pregnancy for a woman in premature menopause. J Clin Med. 2018;8(1).
Pantos K, et al. A case series on natural conceptions resulting in ongoing pregnancies in menopausal and prematurely menopausal women following platelet-rich plasma treatment. Cell Transplant. 2019;28(9–10):1333–40.
Sfakianoudis K, et al. Reactivating ovarian function through autologous platelet-rich plasma intraovarian infusion: pilot data on premature ovarian insufficiency, perimenopausal, menopausal, and poor responder women. J Clin Med. 2020;9(6).
Chan K, Bhandari M. Three-minute critical appraisal of a case series article. Indian J Orthop. 2011;45(2):103–4.
Murad MH, et al. Methodological quality and synthesis of case series and case reports. BMJ Evidence-Based Med. 2018;23(2):60–3.
Roh YH, et al. Cytokine-release kinetics of platelet-rich plasma according to various activation protocols. Bone Joint Res. 2016;5(2):37–45.
Sills ES, Wood SH. Appraisal of experimental methods to manage menopause and infertility: intraovarian platelet-rich plasma vs. condensed platelet-derived cytokines. Medicina (Kaunas). 2021;58(1).
Author information
Authors and Affiliations
Contributions
All authors contributed equally to this review paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kheil, M.H., Bahsoun, R. & Sharara, F.I. Platelet-rich plasma: inconclusive evidence of reproductive outcomes in menopausal women. J Assist Reprod Genet 39, 1987–1991 (2022). https://doi.org/10.1007/s10815-022-02554-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-022-02554-5