Abstract
Purpose
To assess whether live birth rates (LBR) and maternal/neonatal complications differed following single fresh and frozen-warmed blastocyst transfer.
Methods
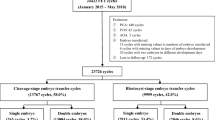
The present retrospective observational study analyzed 4,613 single embryo transfers (SET) (646 fresh and 3,967 frozen) from January 1, 2014, to December 31, 2018. Fresh embryo transfer at blastocyst stage was considered according to the age of the patient and her prognosis. In case of the risk of ovarian hyperstimulation syndrome, premature progesterone rise, non-optimal endometrial growth, or supernumerary embryos, cryopreservation with subsequent frozen embryo transfer (FET) was indicated.
Results
No differences in LBR were recorded. Fresh embryo transfers yielded an increase both in neonatal complications OR 2.15 (95% CI 1.20–3.86, p 0.010), with a higher prevalence of singletons weighting below the 5th percentile (p 0.013) and of intrauterine growth retardation (p 0.015), as well as maternal complications, with a higher placenta previa occurrence OR 3.58 (95% CI 1.54–8.28, p 0.003), compared to FET.
Conclusion
LBR appears not to be affected by the transfer procedure preferred. Fresh embryo transfer is associated with higher risk of neonatal complications (specifically a higher prevalence of singletons weighting below the 5th percentile and of intrauterine growth retardation) and placenta previa. Reflecting on the increased practice of ART procedures, it is imperative to understand whether a transfer procedure yields less complications than the other and if it is time to switch to a “freeze-all” procedure as standard practice.
Trial registration: Clinical Trial Registration Number: NCT04310761. Date of registration: March 17, 2020, retrospectively registered.
Similar content being viewed by others
Data availability
Data and supplementary materials are available under request.
Code availability
Only under request.
References
Levi Setti PE, Albani E, Cesana A, Novara PV, Zannoni E, Baggiani AM, et al. Italian Constitutional Court modifications of a restrictive assisted reproduction technology law significantly improve pregnancy rate. Hum Reprod. 2011;26:376–81.
Gera PS, Tatpati LL, Allemand MC, Wentworth MA, Coddington CC. Ovarian hyperstimulation syndrome: steps to maximize success and minimize effect for assisted reproductive outcome. Fertil Steril. 2010;94:173–8.
D’Angelo A, Amso NN. Embryo freezing for preventing ovarian hyperstimulation syndrome: a Cochrane review. Hum Reprod. 2002;17:2787–94.
Martikainen H, Tiitinen A, Tomás C, Tapanainen J, Orava M, Tuomivaara L, et al. One versus two embryo transfer after IVF and ICSI: a randomized study. Hum Reprod. 2001;16:1900–3.
Veleva Z, Karinen P, Tomás C, Tapanainen JS, Martikainen H. Elective single embryo transfer with cryopreservation improves the outcome and diminishes the costs of IVF/ICSI. Hum Reprod. 2009;24:1632–9.
Malizia BA, Hacker MR, Penzias AS. Cumulative live-birth rates after in vitro fertilization. N Engl J Med. 2009;360:236–43.
El-Toukhy T, Coomarasamy A, Khairy M, Sunkara K, Seed P, Khalaf Y, et al. The relationship between endometrial thickness and outcome of medicated frozen embryo replacement cycles. Fertil Steril. 2008;89:832–9.
Ubaldi FM, Cimadomo D, Capalbo A, Vaiarelli A, Buffo L, Trabucco E, et al. Preimplantation genetic diagnosis for aneuploidy testing in women older than 44 years: a multicenter experience. Fertil Steril. 2017;107:1173–80.
Sacchi L, Albani E, Cesana A, Smeraldi A, Parini V, Fabiani M et al. Preimplantation genetic testing for aneuploidy improves clinical, gestational, and neonatal outcomes in advanced maternal age patients without compromising cumulative live-birth rate. J Assist Reprod Genet. 2019.
Scaravelli G, Levi-Setti PE, Livi C, La Sala G, Ubaldi FM, Greco E, et al. Contribution of cryopreservation to the cumulative live birth rate: a large multicentric cycle-based data analysis from the Italian National Registry. J Assist Reprod Genet. 2019;36:2287–95.
Ishihara O, Araki R, Kuwahara A, Itakura A, Saito H, Adamson GD. Impact of frozen-thawed single-blastocyst transfer on maternal and neonatal outcome: an analysis of 277,042 single-embryo transfer cycles from 2008 to 2010 in Japan. Fertil Steril. 2014;101:128–33.
Sha T, Yin X, Cheng W, Massey IY. Pregnancy-related complications and perinatal outcomes resulting from transfer of cryopreserved versus fresh embryos in vitro fertilization: a meta-analysis. Fertil Steril. 2018;109:330-42.e9.
Zhang J, Wang Y, Liu H, Mao X, Chen Q, Fan Y, et al. Effect of in vitro culture period on birth weight after vitrified-warmed transfer cycles: analysis of 4,201 singleton newborns. Fertil Steril. 2019;111:97–104.
Practice Committee of the American Society for Reproductive Medicine, Practice Committee of the Society for Assisted Reproductive Technology. Guidance on the limits to the number of embryos to transfer: a committee opinion. Fertil Steril. 2017;107:901–3.
Levi Setti PE, Cirillo F, De Cesare R, Morenghi E, Canevisio V, Ronchetti C, et al. Seven years of vitrified blastocyst transfers: comparison of 3 preparation protocols at a single ART center. Front Endocrinol (Lausanne). 2020;11:346.
Levi Setti PE, Albani E, Cavagna M, Bulletti C, Colombo GV, Negri L. The impact of embryo transfer on implantation–a review. Placenta. 2003;24 Suppl B:S20-6.
Zegers-Hochschild F, Adamson GD, Dyer S, Racowsky C, de Mouzon J, Sokol R, et al. The International Glossary on Infertility and Fertility Care, 2017. Fertil Steril. 2017;108:393–406.
Nicolaides KH, Wright D, Syngelaki A, Wright A, Akolekar R. Fetal Medicine Foundation fetal and neonatal population weight charts. Ultrasound Obstet Gynecol. 2018;52:44–51.
Levi-Setti PE, Cirillo F, Scolaro V, Morenghi E, Heilbron F, Girardello D, et al. Appraisal of clinical complications after 23,827 oocyte retrievals in a large assisted reproductive technology program. Fertil Steril. 2018;109:1038-43.e1.
Roy TK, Bradley CK, Bowman MC, McArthur SJ. Single-embryo transfer of vitrified-warmed blastocysts yields equivalent live-birth rates and improved neonatal outcomes compared with fresh transfers. Fertil Steril. 2014;101:1294–301.
Pandey S, Shetty A, Hamilton M, Bhattacharya S, Maheshwari A. Obstetric and perinatal outcomes in singleton pregnancies resulting from IVF/ICSI: a systematic review and meta-analysis. Hum Reprod Update. 2012;18:485–503.
Zeilmaker GH, Alberda AT, van Gent I, Rijkmans CM, Drogendijk AC. Two pregnancies following transfer of intact frozen-thawed embryos. Fertil Steril. 1984;42:293–6.
Aflatoonian A, Mansoori Moghaddam F, Mashayekhy M, Mohamadian F. Comparison of early pregnancy and neonatal outcomes after frozen and fresh embryo transfer in ART cycles. J Assist Reprod Genet. 2010;27:695–700.
Zhu D, Zhang J, Cao S, Heng BC, Huang M, Ling X, et al. Vitrified-warmed blastocyst transfer cycles yield higher pregnancy and implantation rates compared with fresh blastocyst transfer cycles–time for a new embryo transfer strategy? Fertil Steril. 2011;95:1691–5.
Shapiro BS, Daneshmand ST, Garner FC, Aguirre M, Hudson C, Thomas S. Evidence of impaired endometrial receptivity after ovarian stimulation for in vitro fertilization: a prospective randomized trial comparing fresh and frozen-thawed embryo transfers in high responders. Fertil Steril. 2011;96:516–8.
Boomsma CM, Kavelaars A, Eijkemans MJ, Fauser BC, Heijnen CJ, Macklon NS. Ovarian stimulation for in vitro fertilization alters the intrauterine cytokine, chemokine, and growth factor milieu encountered by the embryo. Fertil Steril. 2010;94:1764–8.
Dieamant FC, Petersen CG, Mauri AL, Comar V, Mattila M, Vagnini LD, et al. Fresh embryos versus freeze-all embryos - transfer strategies: nuances of a meta-analysis. JBRA Assist Reprod. 2017;21:260–72.
Berntsen S, Söderström-Anttila V, Wennerholm UB, Laivuori H, Loft A, Oldereid NB, et al. The health of children conceived by ART: 'the chicken or the egg?' Hum Reprod Update. 2019;25:137–58.
Herruzo AJ, Martínez L, Biel E, Robles R, Rosales MA, Miranda JA. Perinatal morbidity and mortality in twin pregnancies. Int J Gynaecol Obstet. 1991;36:17–22.
Vega M, Zaghi S, Buyuk E, Jindal S. Not all twins are monozygotic after elective single embryo transfer: analysis of 32,600 elective single embryo transfer cycles as reported to the Society for Assisted Reproductive Technology. Fertil Steril. 2018;109:118–22.
Ikemoto Y, Kuroda K, Ochiai A, Yamashita S, Ikuma S, Nojiri S, et al. Prevalence and risk factors of zygotic splitting after 937 848 single embryo transfer cycles. Hum Reprod. 2018;33:1984–91.
Palomba S, Santagni S, Gibbins K, La Sala GB, Silver RM. Pregnancy complications in spontaneous and assisted conceptions of women with infertility and subfertility factors. A comprehensive review. Reprod Biomed Online. 2016;33:612–28.
Saunders DM, Mathews M, Lancaster PA. The Australian Register: current research and future role. A preliminary report. Ann N Y Acad Sci. 1988;541:7–21.
Pinheiro RL, Areia AL, Mota Pinto A, Donato H. Advanced maternal age: adverse outcomes of pregnancy, a meta-analysis. Acta Med Port. 2019;32:219–26.
Brandt JS, Cruz Ithier MA, Rosen T, Ashkinadze E. Advanced paternal age, infertility, and reproductive risks: A review of the literature. Prenat Diagn. 2019;39:81–7.
Wennberg AL, Opdahl S, Bergh C, Aaris Henningsen AK, Gissler M, Romundstad LB, et al. Effect of maternal age on maternal and neonatal outcomes after assisted reproductive technology. Fertil Steril. 2016;106:1142-9.e14.
Acknowledgements
The authors thank all the embryologists and gynecologists working in Humanitas Fertility Center, Rozzano, Milan, Italy.
Author information
Authors and Affiliations
Contributions
FC and PELS were involved in the study concept and design. LG, IP, and EM contributed to the acquisition of data. FC and EM analyzed data. LG and FC wrote the manuscript and had a primary responsibility for final content. FC and EM supervised the analysis. CR and AB contributed to bibliography updating and critically revised the manuscript and helped for data analysis. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Internal Ethical Committee approved the study design on April 7, 2020. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to participate and for publication
Patients who underwent ART cycles had consented in writing that their medical records could be used for research purposes and publication if their anonymity was ensured and protected.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cirillo, F., Grilli, L., Ronchetti, C. et al. Retrospective comparison of pregnancy outcomes of fresh and frozen-warmed single blastocyst transfer: a 5-year single-center experience. J Assist Reprod Genet 39, 201–209 (2022). https://doi.org/10.1007/s10815-021-02362-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-021-02362-3