Abstract
Purpose
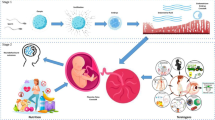
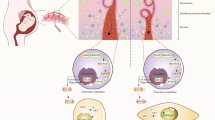
Intrauterine growth restriction (IUGR) is a fetal growth complication that can be caused by ineffective nutrient transfer from the mother to the fetus via the placenta. Abnormal placental development and function have been correlated with abnormal expression of imprinted genes, which are regulated by epigenetic modifications at imprinting control regions (ICRs). In this study, we analyzed the expression of imprinted genes known to be involved in fetal growth and epigenetic regulators involved in DNA methylation, as well as DNA methylation at the KvDMR1 imprinting control region and global levels of DNA hydroxymethylation, in IUGR cases.
Methods
Expression levels of imprinted genes and epigenetic regulators were analyzed in term placental samples from 21 IUGR cases and 9 non-IUGR (control) samples, by RT-qPCR. Additionally, KvDMR1 methylation was analyzed by bisulfite sequencing and combined bisulfite restriction analysis (COBRA) techniques. Moreover, global DNA methylation and hydroxymethylation levels were also measured.
Results
We observed increased expression of PHLDA2, CDKN1C, and PEG10 imprinted genes and of DNMT1, DNMT3A, DNMT3B, and TET3 epigenetic regulators in IUGR placentas. No differences in methylation levels at the KvDMR1 were observed between the IUGR and control groups; similarly, no differences in global DNA methylation and hydromethylation were detected.
Conclusion
Our study shows that deregulation of epigenetic mechanisms, namely increased expression of imprinted genes and epigenetic regulators, might be associated with IUGR etiology. Therefore, this study adds knowledge to the molecular mechanisms underlying IUGR, which may contribute to novel prediction tools and future therapeutic options for the management of IUGR pregnancies.






Similar content being viewed by others
Abbreviations
- 5-hmC:
-
5-Hydroxymethylcytosine
- 5-mC:
-
5-Methylcytosine
- DNMT:
-
DNA methyltransferase
- ES cells:
-
Embryonic stem cells
- ICR:
-
Imprinting control region
- IUGR:
-
Intrauterine growth restriction
- TET:
-
Ten eleven translocation
References
Rhon-Calderon EA, Vrooman LA, Riesche L, Bartolomei MS. The effects of assisted reproductive technologies on genomic imprinting in the placenta. Placenta. 2019;84:37–43. https://doi.org/10.1016/j.placenta.2019.02.013.
Gude NM, Roberts CT, Kalionis B, King RG. Growth and function of the normal human placenta. Thromb Res. 2004;114:397–407. https://doi.org/10.1016/j.thromres.2004.06.038.
Maccani MA, Marsit CJ. Epigenetics in the placenta. Am J Reprod Immunol (New York, NY : 1989). 2009;62:78–89. https://doi.org/10.1111/j.1600-0897.2009.00716.x.
Calkins KL, Devaskar SU. Intrauterine growth restriction. Fanaroff Martin's Neonatal-Perinatal Med. 2015;2-Volume Set:227–35. https://doi.org/10.1016/B978-1-4557-5617-9.00016-6.
Bressan FF, De Bem THC, Perecin F, Lopes FLL, Ambrosio CE, Meirelles FVV, et al. Unearthing the roles of imprinted genes in the placenta. Placenta. 2009;30:823–34. https://doi.org/10.1016/j.placenta.2009.07.007.
Monk D. Genomic imprinting in the human placenta. Am J Obstet Gynecol. 2015;213(4, Supplement):S152–S62. https://doi.org/10.1016/j.ajog.2015.06.032.
Pilvar D, Reiman M, Pilvar A, Laan M. Parent-of-origin-specific allelic expression in the human placenta is limited to established imprinted loci and it is stably maintained across pregnancy. Clin Epigenetics. 2019;11(1):94. https://doi.org/10.1186/s13148-019-0692-3.
Moore T. Genomic imprinting in mammalian development: a parental tug-of-war. Trends Genet. 1991;7:45–9. https://doi.org/10.1016/0168-9525(91)90230-N.
Cassidy FC, Charalambous M. Genomic imprinting, growth and maternal–fetal interactions. J Exp Biol. 2018;221(Suppl 1):jeb164517. https://doi.org/10.1242/jeb.164517.
Reik W, Walter J. Genomic imprinting: parental influence on the genome. Nat Rev Genet. 2001;2(1):21–32. https://doi.org/10.1038/35047554.
Santiago M, Antunes C, Guedes M, Sousa N, Marques CJ. TET enzymes and DNA hydroxymethylation in neural development and function—how critical are they? Genomics. 2014;104(5):334–40. https://doi.org/10.1016/j.ygeno.2014.08.018.
Bourque DKK, Avila L, Peñaherrera M, von Dadelszen P, Robinson WPP. Decreased placental methylation at the H19/IGF2 imprinting control region is associated with normotensive intrauterine growth restriction but not preeclampsia. Placenta. 2010;31:197–202. https://doi.org/10.1016/j.placenta.2009.12.003.
Cordeiro A, Neto AP, Carvalho F, Ramalho C, Dória S. Relevance of genomic imprinting in intrauterine human growth expression of CDKN1C, H19, IGF2, KCNQ1 and PHLDA2 imprinted genes. J Assist Reprod Genet. 2014;31:1361–8. https://doi.org/10.1007/s10815-014-0278-0.
Chiesa N, De Crescenzo A, Mishra K, Perone L, Carella M, Palumbo O, et al. The KCNQ1OT1 imprinting control region and non-coding RNA: new properties derived from the study of Beckwith-Wiedemann syndrome and Silver-Russell syndrome cases. Hum Mol Genet. 2012;21:10–25. https://doi.org/10.1093/hmg/ddr419.
Jensen AB, Tunster SJ, John RM. The significance of elevated placental PHLDA2 in human growth restricted pregnancies. Placenta. 2014;35:528–32. https://doi.org/10.1016/j.placenta.2014.04.018.
Jin F, Qiao C, Luan N, Shang T. The expression of the imprinted gene pleckstrin homology-like domain family A member 2 in placental tissues of preeclampsia and its effects on the proliferation, migration and invasion of trophoblast cells JEG-3. Clin Exp Pharmacol Physiol. 2015;42(11):1142–51. https://doi.org/10.1111/1440-1681.12468.
Lee MH, Reynisdottir I, Massague J. Cloning of p57KIP2, a cyclin-dependent kinase inhibitor with unique domain structure and tissue distribution. Genes Dev. 1995;9(6):639–49. https://doi.org/10.1101/gad.9.6.639.
Jacob K, Robinson W, Lefebvre L. Beckwith–Wiedemann and Silver–Russell syndromes: opposite developmental imbalances in imprinted regulators of placental function and embryonic growth. Clin Genet. 2013;84(4):326–34. https://doi.org/10.1111/cge.12143.
Frost JM, Moore GE. The importance of imprinting in the human placenta. PLoS Genet. 2010;6(7):e1001015. https://doi.org/10.1371/journal.pgen.1001015.
Kotzot D, Schmitt S, Bernasconi F, Robinson WP, Lurie IW, Ilyina H, et al. Uniparental disomy 7 in Silver—Russell syndrome and primordial growth retardation. Hum Mol Genet. 1995;4(4):583–7. https://doi.org/10.1093/hmg/4.4.583.
Mayer W, Hemberger M, Frank HG, Grümmer R, Winterhager E, Kaufmann P, et al. Expression of the imprinted genes MEST/Mest in human and murine placenta suggests a role in angiogenesis. Dev Dyn. 2000;217(1):1–10. https://doi.org/10.1002/(sici)1097-0177(200001)217:1<1::Aid-dvdy1>3.0.Co;2-4.
Chen H, Sun M, Liu J, Tong C, Meng T. Silencing of paternally expressed gene 10 inhibits trophoblast proliferation and invasion. PLoS One. 2015;10(12):e0144845. https://doi.org/10.1371/journal.pone.0144845.
Carraca T, Ferraz T, Machado L, Bessa Monteiro S, Rodrigues T, Montengro N. Restrição de crescimento fetal- Rastreio, diagnóstico e orientação clínica. In: Lidel, editor. Protocolos de medicina materno-fetal. 3ª ed. Lisboa: Lidel; 2008. p. 133–4.
Figueras F, Gratacós E. Update on the diagnosis and classification of fetal growth restriction and proposal of a stage-based management protocol. Fetal Diagn Ther. 2014;36(2):86–98. https://doi.org/10.1159/000357592.
Pidoux G, Gerbaud P, Laurendeau I, Guibourdenche J, Bertin G, Vidaud M, et al. Large variability of trophoblast gene expression within and between human normal term placentae. Placenta. 2004;25(5):469–73. https://doi.org/10.1016/j.placenta.2003.10.016.
Wyatt SM, Kraus FT, Roh CR, Elchalal U, Nelson DM, Sadovsky Y. The correlation between sampling site and gene expression in the term human placenta. Placenta. 2005;26(5):372–9. https://doi.org/10.1016/j.placenta.2004.07.003.
Marques CJ, Joao Pinho M, Carvalho F, Bieche I, Barros A, Sousa M. DNA methylation imprinting marks and DNA methyltransferase expression in human spermatogenic cell stages. Epigenetics. 2011;6(11):1354–61. https://doi.org/10.4161/epi.6.11.17993.
Hellemans J, Mortier G, De Paepe A, Speleman F, Vandesompele J. qBase relative quantification framework and software for management and automated analysis of real-time quantitative PCR data. Genome Biol. 2007;8:R19. https://doi.org/10.1186/gb-2007-8-2-r19.
Khoueiry R, Ibala-Romdhane S, Al-Khtib M, Blachere T, Lornage J, Guerin JF, et al. Abnormal methylation of KCNQ1OT1 and differential methylation of H19 imprinting control regions in human ICSI embryos. Zygote. 2013;21(2):129–38. https://doi.org/10.1017/s0967199411000694.
Xiong Z, Laird PW. COBRA: a sensitive and quantitative DNA methylation assay. Nucleic Acids Res. 1997;25(12):2532–4. https://doi.org/10.1093/nar/25.12.2532.
Marques CJ, Costa P, Vaz B, Carvalho F, Fernandes S, Barros A, et al. Abnormal methylation of imprinted genes in human sperm is associated with oligozoospermia. Mol Hum Reprod. 2008;14(2):67–74. https://doi.org/10.1093/molehr/gam093.
Gong S, Johnson MD, Dopierala J, Gaccioli F, Sovio U, Constância M, et al. Genome-wide oxidative bisulfite sequencing identifies sex-specific methylation differences in the human placenta. Epigenetics. 2018;13(3):228–39. https://doi.org/10.1080/15592294.2018.1429857.
Martin E, Smeester L, Bommarito PA, Grace MR, Boggess K, Kuban K, et al. Sexual epigenetic dimorphism in the human placenta: implications for susceptibility during the prenatal period. Epigenomics. 2017;9(3):267–78. https://doi.org/10.2217/epi-2016-0132.
Bock C, Reither S, Mikeska T, Paulsen M, Walter J, Lengauer T. BiQ Analyzer: visualization and quality control for DNA methylation data from bisulfite sequencing. Bioinformatics. 2005;21:4067–8. https://doi.org/10.1093/bioinformatics/bti652.
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods. 2001;25(4):402–8. https://doi.org/10.1006/meth.2001.1262.
Ishida M, Moore GE. The role of imprinted genes in humans. Mol Asp Med. 2013;34:826–40. https://doi.org/10.1016/j.mam.2012.06.009.
Piedrahita JA. The role of imprinted genes in fetal growth abnormalities. Birth Defects Res A, Clin Molec Teratol. 2011;91:682–92. https://doi.org/10.1002/bdra.20795.
McMinn J, Wei M, Schupf N, Cusmai J, Johnson EB, Smith AC, et al. Unbalanced placental expression of imprinted genes in human intrauterine growth restriction. Placenta. 2006;27:540–9. https://doi.org/10.1016/j.placenta.2005.07.004.
López-Abad M, Iglesias-Platas I, Monk D. Epigenetic characterization of CDKN1C in placenta samples from non-syndromic intrauterine growth restriction. Front Genet. 2016;7:62. https://doi.org/10.3389/fgene.2016.00062.
Diplas AI, Lambertini L, Lee M-J, Sperling R, Lee YL, Wetmur J, et al. Differential expression of imprinted genes in normal and IUGR human placentas. Epigenetics. 2009;4:235–40.
Janssen AB, Tunster SJ, Heazell AEP, John RM. Placental PHLDA2 expression is increased in cases of fetal growth restriction following reduced fetal movements. BMC Med Genet. 2016;17:17. https://doi.org/10.1186/s12881-016-0279-1.
Apostolidou S, Abu-Amero S, O’Donoghue K, Frost J, Olafsdottir O, Chavele KM, et al. Elevated placental expression of the imprinted PHLDA2 gene is associated with low birth weight. J Mol Med. 2007;85:379–87. https://doi.org/10.1007/s00109-006-0131-8.
Chen XJ, Chen F, Lv PP, Zhang D, Ding GL, Hu XL, et al. Maternal high estradiol exposure alters CDKN1C and IGF2 expression in human placenta. Placenta. 2018;61:72–9. https://doi.org/10.1016/j.placenta.2017.11.009.
Moore GGE, Ishida M, Demetriou C, Al-Olabi L, Leon LJ, Thomas AC, et al. The role and interaction of imprinted genes in human fetal growth. Philos Trans R Soc Lond Ser B Biol Sci. 2015;370:20140074. https://doi.org/10.1098/rstb.2014.0074.
Gou C, Liu X, Shi X, Chai H, He ZM, Huang X, et al. Placental expressions of CDKN1C and KCNQ1OT1 in monozygotic twins with selective intrauterine growth restriction. Twin Res Hum Genet. 2017;20(5):389–94. https://doi.org/10.1017/thg.2017.41.
Shi X, He Z, Gao Y, Luo Y, Gou C, Fang Q. Placental expression of PHLDA2 in selective intrauterine growth restriction in monozygotic twins. Placenta. 2014;35(6):428–30. https://doi.org/10.1016/j.placenta.2014.03.006.
Jin F, Qiao C, Luan N, Li H. Lentivirus-mediated PHLDA2 overexpression inhibits trophoblast proliferation, migration and invasion, and induces apoptosis. Int J Mol Med. 2016;42016:949–57.
Hannula-Jouppi K, Muurinen M, Lipsanen-Nyman M, Reinius LE, Ezer S, Greco D, et al. Differentially methylated regions in maternal and paternal uniparental disomy for chromosome 7. Epigenetics. 2014;9(3):351–65. https://doi.org/10.4161/epi.27160.
Vasconcelos S, Ramalho C, Marques CJ, Doria S. Altered expression of epigenetic regulators and imprinted genes in human placenta and fetal tissues from second trimester spontaneous pregnancy losses. Epigenetics. 2019;14:1–11. https://doi.org/10.1080/15592294.2019.1634988.
Miranda Furtado CL, Salomão KB, Verruma CG, Paulino Leite SB, Lopes Rios ÁF, Bialecka M, et al. Variation in DNA methylation in the KvDMR1 (ICR2) region in first-trimester human pregnancies. Fertil Steril. 2019;111(6):1186–93. https://doi.org/10.1016/j.fertnstert.2019.01.036.
Ishida M, Monk D, Duncan Andrew J, Abu-Amero S, Chong J, Ring Susan M, et al. Maternal inheritance of a promoter variant in the imprinted PHLDA2 gene significantly increases birth weight. Am J Hum Genet. 2012;90(4):715–9. https://doi.org/10.1016/j.ajhg.2012.02.021.
Li Y, Meng G, Guo QN. Changes in genomic imprinting and gene expression associated with transformation in a model of human osteosarcoma. Exp Mol Pathol. 2008;84(3):234–9. https://doi.org/10.1016/j.yexmp.2008.03.013.
Wang R, Su L, Yu S, Ma X, Jiang C, Yu Y. Inhibition of PHLDA2 transcription by DNA methylation and YY1 in goat placenta. Gene. 2020;739:144512. https://doi.org/10.1016/j.gene.2020.144512.
De Crescenzo A, Sparago A, Cerrato F, Palumbo O, Carella M, Miceli M, et al. Paternal deletion of the 11p15.5 centromeric-imprinting control region is associated with alteration of imprinted gene expression and recurrent severe intrauterine growth restriction. J Med Genet. 2013;50:99–103. https://doi.org/10.1136/jmedgenet-2012-101352.
He Z, Lu H, Luo H, Gao F, Wang T, Gao Y, et al. The promoter methylomes of monochorionic twin placentas reveal intrauterine growth restriction-specific variations in the methylation patterns. Sci Rep. 2016;6:20181. https://doi.org/10.1038/srep20181.
Piyasena C, Reynolds RM, Khulan B, Seckl JR, Menon G, Drake AJ. Placental 5-methylcytosine and 5-hydroxymethylcytosine patterns associate with size at birth. Epigenetics. 2015;10:692–7. https://doi.org/10.1080/15592294.2015.1062963.
Zhang Y, Zheng D, Fang Q, Zhong M. Aberrant hydroxymethylation of ANGPTL4 is associated with selective intrauterine growth restriction in monochorionic twin pregnancies. Epigenetics. 2020;15:1–13. https://doi.org/10.1080/15592294.2020.1737355.
Logan PC, Mitchell MD, Lobie PE. DNA methyltransferases and TETs in the regulation of differentiation and invasiveness of extra-villous trophoblasts. Front Genet. 2013;4:265. https://doi.org/10.3389/fgene.2013.00265.
Putiri EL, Tiedemann RL, Thompson JJ, Liu C, Ho T, Choi J-H, et al. Distinct and overlapping control of 5-methylcytosine and 5-hydroxymethylcytosine by the TET proteins in human cancer cells. Genome Biol. 2014;15(6):R81. https://doi.org/10.1186/gb-2014-15-6-r81.
Rakoczy J, Padmanabhan N, Krzak AM, Kieckbusch J, Cindrova-Davies T, Watson ED. Dynamic expression of TET1, TET2, and TET3 dioxygenases in mouse and human placentas throughout gestation. Placenta. 2017;59:46–56. https://doi.org/10.1016/j.placenta.2017.09.008.
Hernandez Mora JR, Sanchez-Delgado M, Petazzi P, Moran S, Esteller M, Iglesias-Platas I, et al. Profiling of oxBS-450 K 5-hydroxymethylcytosine in human placenta and brain reveals enrichment at imprinted loci. Epigenetics. 2018;13(2):182–91. https://doi.org/10.1080/15592294.2017.1344803.
Li W, Liu M. Distribution of 5-hydroxymethylcytosine in different human tissues. J Nucleic Acids. 2011;2011:870726–5. https://doi.org/10.4061/2011/870726.
Nestor CE, Ottaviano R, Reddington J, Sproul D, Reinhardt D, Dunican D, et al. Tissue type is a major modifier of the 5-hydroxymethylcytosine content of human genes. Genome Res. 2012;22(3):467–77. https://doi.org/10.1101/gr.126417.111.
Green BB, Houseman EA, Johnson KC, Guerin DJ, Armstrong DA, Christensen BC, et al. Hydroxymethylation is uniquely distributed within term placenta, and is associated with gene expression. FASEB J. 2016;30(8):2874–84. https://doi.org/10.1096/fj.201600310R.
Chabrun F, Huetz N, Dieu X, Rousseau G, Bouzillé G, Chao de la Barca JM, et al. Data-mining approach on transcriptomics and methylomics placental analysis highlights genes in fetal growth restriction. Front Genet. 2019. https://doi.org/10.3389/fgene.2019.01292.
O'Callaghan JL, Clifton VL, Prentis P, Ewing A, Miller YD, Pelzer ES. Modulation of Placental Gene Expression in Small-for-Gestational-Age Infants. Genes (Basel). 2020;11(1):80. https://doi.org/10.3390/genes11010080.
Acknowledgments
We thank the obstetricians at the Department of Gynecology/Obstetrics of Hospital São João, Porto, Portugal, for collaboration with sample and patients’ data collection. We are also thankful to members of the Genetics Department of FMUP for technical help and insightful discussions.
Funding
This work was partly funded by the Portuguese Foundation for Science and Technology (FCT) – UID/BIM/04293/2013 and FCT Investigator award to CJM (IF/00047/2012; CEECIND/00371/2017). C.C. is a recipient of a PhD studentship by FCT (SFRH/BD/141855/2018). S.V. is a recipient of a PhD studentship by FCT (SFRH/BD/147440/2019).
Author information
Authors and Affiliations
Contributions
C.C. performed the experiments, analyzed the results, and wrote the first draft of the manuscript; S.V. performed experimental work and revised the manuscript; C.R. (MD, Obstetrician) collected placental samples and patients’ data; C.J.M supervised experimental work, analyzed the data, and wrote the final manuscript; S.D. designed the study, analyzed the data, and wrote the final manuscript. All authors revised and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Patient consent
All patients provided a signed informed consent for this study.
Ethics approval
This study was approved by the Health Ethics Committee of Hospital São João/Faculty of Medicine of Porto (N 70/17).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Caniçais, C., Vasconcelos, S., Ramalho, C. et al. Deregulation of imprinted genes expression and epigenetic regulators in placental tissue from intrauterine growth restriction. J Assist Reprod Genet 38, 791–801 (2021). https://doi.org/10.1007/s10815-020-02047-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-020-02047-3