Abstract
Purpose
To identify genetic variation associated to premature ovarian insufficiency (POI).
Methods
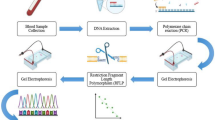
A total of 74 women with POI (group POI), 45 women with increased FSH levels (group high FSH), and 88 controls (non-POI) were studied. Genotyping of BMP15:c.-9C>G (rs3810682), BMP15:c.328+905A>G (rs3897937), and BMP15:c.852C>T (rs17003221); and GDF9:c.134-694G>A (rs4705974), GDF9:c.-31-951G>A (rs11748063), GDF9:c.-152G>C (rs30177), and GDF9:g.1073C>T (rs803224) was performed by the TaqMan methodology. Chi-square and Fisher’s exact tests were performed to evaluate the distribution of genotypes, alleles, odds ratio, and the Hardy-Weinberg equilibrium of each variation. Haplotype analysis was performed for each gene considering the case and control groups. Bonferroni’s correction was applied to chi-square and Fisher’s exact test data, and p values < 0.007 for genotypes and alleles and < 0.006 for haplotypes were considered significant.
Results
It was observed a statistically significant difference in genotype distribution of BMP15:c.852C>T between group POI and controls (p < 0.001). TT and TC genotypes were more frequently observed in group POI. Genotype distribution in case group POI, however, was not in the Hardy-Weinberg equilibrium, due to the increased number of heterozygotes in the sample. Concerning GDF9, no association was found among the studied genetic variants and POI or high FSH groups.
Conclusion
It is concluded from the present study that the genotypes CT and TT from BMP15:c.852C>T variation may be risk factors for the development of POI.
Similar content being viewed by others
References
Silva AA, Arent A, Petracco A, Mancebo AC, Bastos AM, Fraga AM, et al. Tratado de Reprodução Assistida. 1ª. Ed. São Paulo: Abril 2010.
Goswami D, Conway GS. Premature ovarian failure. Hum Reprod Update. 2005;11(4):391–410.
European Society for Human Reproduction and Embryology (ESHRE) Guideline Group on POI, Webber L, Davies M, Anderson R, Bartlett J, Braat D, et al. ESHRE guideline: management of women with premature ovarian insufficiency. Hum Reprod. 2016;31(5):926–37.
Vegetti W, Marozzi A, Manfredini E, Testa G, Alagna F, Nicolosi A, et al. Premature ovarian failure. Mol Cell Endocrinol. 2000;161(1–2):53–7.
Mattison DR, Evans MI, Schwimmer WB, White BJ, Jensen B, Schulman JD. Familial premature ovarian failure. Am J Hum Genet. 1984;36:1341–8.
Alper MM, Garner PR, Seibel MM. Premature ovarian failure. Current concepts. J Reprod Med. 1986;31:699–708.
Anasti JN. Premature ovarian failure: an update. Fertil Steril. 1998;70:1–15.
Conway GS. Premature ovarian failure. Curr Opin Obstet Gynecol. 1997;9:202–6.
Kovanci E, Simpson JL, Amato P, Rohozinski J, Heard MJ, Bishop CE, et al. Oocyte specific G protein coupled receptor-3 (GPR3) gene perturbations are not commonly involved in premature ovarian failure. Fertil Steril. Published online October 20, 2007.
Paulini F, Melo EO. The role of oocyte-secreted factors GDF9 and BMP15 in follicular development and oogenesis. Reprod Domest Anim. 2011;46:354–61.
Trombly DJ, Woodruff TK, Mayo KE. Roles for transforming growth factor beta superfamily proteins in early folliculogenesis. Semin Reprod Med. 2009;27:14–23.
Kedem A, Fisch B, Garor R, Ben-Zaken A, Gizunterman T, Felz C, et al. Growth differentiating factor 9 (GDF9) and bone morphogenetic protein 15 both activate development of human primordial follicles in vitro, with seemingly more beneficial effects of GDF9. J Clin Endocrinol Metab. 2011;96:1246–54.
Vilodre LC, Moretto M, Kohek MB, Spritzer PM. Premature ovarian failure: present aspects. Arq Bras Endocrinol Metabol. 2007;51(6):920–9.
Pennetier S, Uzbekova S, Perreau C, Papillier P, Mermillod P, Dalbies-Tran R. Spatio-temporal expression of the germ cell marker genes MATER, ZAR1, GDF9, BMP15, and VASA in adult bovine tissues, oocytes, and preimplantation embryos. Biol Reprod. 2004;71:1359–66.
Lahiri DK, Numberger JI. A rapid non-enzymatic method for Q2 preparation of HMW DNA from blood for RFLP studies. Nucleic Acids Res. 1991;19:5444.
Naslavsky MS, Yamamoto GL, de Almeida TF, Ezquina SAM, Sunaga DY, Pho N, et al. Exomic variants of an elderly cohort of Brazilians in the ABraOM database. Hum Mutat. 2017;38(7):751–63.
Galloway SM, McNatty KP, Cambridge LM, Laitinen MP, Juengel JL, Jokiranta TS, et al. Mutations in an oocyte-derived growth factor gene (BMP15) cause increased ovulation rate and infertility in a dosage-sensitive manner. Nat Genet. 2000;25(3):279–83.
Di Pasquale E, Beck-Peccoz P, Persani L. Hypergonadotropic ovarian failure associated with an inherited mutation of human bone morphogenetic protein-15 (BMP15) gene. Am J Hum Genet. 2004;75(1):106–11.
Qin Y, Jiao X, Simpson JL, Chen ZJ. Genetics of primary ovarian insufficiency: new developments and opportunities. Hum Reprod Update. 2015;21(6):787–808.
Kumar R, Alwani M, Kosta S, Kaur R, Agarwal S. BMP15 and GDF9 gene mutations in premature ovarian failure. J Reprod Infertil. 2017;18(1):185–9.
Ma L, Chen Y, Mei S, Liu C, Ma X, Li Y, et al. Single nucleotide polymorphisms in premature ovarian failure-associated genes in a Chinese Hui population. Mol Med Rep. 2015;12(2):2529–38.
Tiotiu D, Alvaro Mercadal B, Imbert R, Verbist J, Demeestere I, De Leener A, et al. Variants of the BMP15 gene in a cohort of patients with premature ovarian failure. Hum Reprod. 2010;25(6):1581–7.
Wang B, Wen Q, Ni F, Zhou S, Wang J, Cao Y, et al. Analyses of growth differentiation factor 9 (GDF9) and bone morphogenetic protein 15 (BMP15) mutation in Chinese women with premature ovarian failure. Clin Endocrinol. 2010;72(1):135–6.
Rossetti R, Di Pasquale E, Marozzi A, Bione S, Toniolo D, Grammatico P, et al. BMP15 mutations associated with primary ovarian insufficiency cause a defective production of bioactive protein. Hum Mutat. 2009;30(5):804–10.
Ledig S, Röpke A, Haeusler G, Hinney B, Wieacker P. BMP15 mutations in XX gonadal dysgenesis and premature ovarian failure. Am J Obstet Gynecol. 2008;198(1):84.e1–5.
Zhang P, Shi YH, Wang LC, Chen ZJ. Sequence variants in exons of the BMP-15 gene in Chinese patients with premature ovarian failure. Acta Obstet Gynecol Scand. 2007;86(5):585–9.
Laissue P, Christin-Maitre S, Touraine P, Kuttenn F, Ritvos O, Aittomaki K, et al. Mutations and sequence variants in GDF9 and BMP15 in patients with premature ovarian failure. Eur J Endocrinol. 2006;154(5):739–44.
Dixit H, Rao LK, Padmalatha V, Kanakavalli M, Deenadayal M, Gupta N, et al. Mutational screening of the coding region of growth differentiation factor 9 gene in Indian women with ovarian failure. Menopause. 2005;12(6):749–54.
Dixit H, Rao LK, Padmalatha VV, Kanakavalli M, Deenadayal M, Gupta N, et al. Missense mutations in the BMP15 gene are associated with ovarian failure. Hum Genet. 2006;119(4):408–15.
Di Pasquale E, Rossetti R, Marozzi A, Bodega B, Borgato S, Cavallo L, et al. Identification of new variants of human BMP15 gene in a large cohort of women with premature ovarian failure. J Clin Endocrinol Metab. 2006 May;91(5):1976–9.
Peluso C, Goldman C, Cavalcanti V, Gastaldo G, Trevisan CM, Christofolini DM, et al. Use of bone morphogenetic protein 15 polymorphisms to predict ovarian stimulation outcomes in infertile Brazilian women. Genet Test Mol Biomarkers. 2017;21(5):328–33.
Duarte CW, Vaughan LK, Beasley TM, Tiwari HK. Multifactorial Inheritance and Complex Diseases. Emery and Rimoin’s principles and practice of medical genetics, 6th edn. 2013; chapter 12: 1–15. ISBN: 978–0–12-383834-6.
Voorhuis M, Broekmans FJ, Fauser BC, Onland-Moret NC, van der Schouw YT. Genes involved in initial follicle recruitment may be associated with age at menopause. J Clin Endocrinol Metab. 2011;96(3):E473–9.
Carvalho-Silva DR, Santos FR, Rocha J, Pena SD. The phylogeography of Brazilian Y-chromosome lineages. Am J Hum Genet. 2001;68(1):281–6.
Chand AL, Ponnampalam AP, Harris SE, Winship IM, Shelling AN. Mutational analysis of BMP15 and GDF9 as candidate genes for premature ovarian failure. Fertil Steril. 2006;86(4):1009–12.
Takebayashi K, Takakura K, Wang H, Kimura F, Kasahara K, Noda Y. Mutation analysis of the growth differentiation factor-9 and -9B genes in patients with premature ovarian failure and polycystic ovary syndrome. Fertil Steril. 2000;74(5):976–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The research project was approved by the FMABC’s Ethics Committee and all patients read and signed the informed consent form.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Santos, M., Cordts, E.B., Peluso, C. et al. Association of BMP15 and GDF9 variants to premature ovarian insufficiency. J Assist Reprod Genet 36, 2163–2169 (2019). https://doi.org/10.1007/s10815-019-01548-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-019-01548-0