Abstract
Purpose
The purpose of this study is to present a case of healthy infant born after intracytoplasmic sperm injection-in vitro fertilization (ICSI-IVF) with preimplantation genetic screening (PGS) using sperm from a man with non-mosaic trisomy 21 and a literature review.
Materials and methods
A 26-year-old euploid female and 29-year-old male with non-mosaic trisomy 21 and male factor undergoing ICSI-IVF treatment for primary infertility with embryo biopsy for PGS with comprehensive chromosomal screening (CCS) presented to the Infertility Clinic at Highland Hospital, the Alameda County Medical Center, California, with 6-year history of primary infertility. The outcome measure is a live birth of a healthy child and ploidy status of biopsied blastocysts.
Results
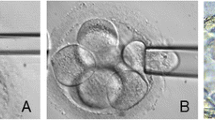
Egg retrieval yielded 33 oocytes, 29 of which underwent ICSI with ejaculated sperm. Twenty-eight 2PN zygotes were cultured, and 13 blastocysts underwent trophectoderm biopsy and vitrification 5 or 6 days after retrieval. CCS analysis revealed that 12 out of 13 (92 %) of blastocysts were euploid and one was a complex abnormal mosaic. Transfer of two grade I hatching blastocysts resulted in a singleton pregnancy with normal prenatal genetic screening and delivery of a healthy male infant at 41 weeks via primary cesarean section for non-reassuring fetal status.
Conclusion
This is the first report of a live birth of a healthy child after ICSI-IVF with PGS using ejaculated sperm from a man with non-mosaic trisomy 21 and male factor infertility.
Similar content being viewed by others
References
Eyman RK, Call TL. Life expectancy of persons with Down syndrome. Am J Ment Retard. 1991;95(6):603–12.
Glasson EJ et al. The changing survival profile of people with Down’s syndrome: implications for genetic counselling. Clin Genet. 2002;62(5):390–3.
Bovicelli L et al. Reproduction in Down syndrome. Obstet Gynecol. 1982;59(6 Suppl):13S–7S.
Hojager B et al. Follicular development in ovaries of children with Down’s syndrome. Acta Paediatr Scand. 1978;67(5):637–43.
Hsiang YH et al. Gonadal function in patients with Down syndrome. Am J Med Genet. 1987;27(2):449–58.
Shobha Rani A et al. Reproduction in Down’s syndrome. Int J Gynaecol Obstet. 1990;31(1):81–6.
Johannisson R et al. Down’s syndrome in the male. Reproductive pathology and meiotic studies. Hum Genet. 1983;63(2):132–8.
Pradhan M et al. Fertility in men with Down syndrome: a case report. Fertil Steril. 2006;86(6):1765.e1–3.
Watson SL et al. Sex and genes, part 1: sexuality and Down, Prader-Willi, and Williams syndromes. Intellect Dev Disabil. 2012;50(2):155–68.
Zuhlke C et al. Down syndrome and male fertility: PCR-derived fingerprinting, serological and andrological investigations. Clin Genet. 1994;46(4):324–6.
Bobrow M et al. Fertility in a male with trisomy 21. J Med Genet. 1992;29(2):141.
Kim ST et al. Successful pregnancy and delivery from frozen-thawed embryos after intracytoplasmic sperm injection using round-headed spermatozoa and assisted oocyte activation in a globozoospermic patient with mosaic Down syndrome. Fertil Steril. 2001;75(2):445–7.
Guerneri S et al. Prevalence and distribution of chromosome abnormalities in a sample of first trimester internal abortions. Hum Reprod. 1987;2(8):735–9.
Nagaishi M et al. Chromosome abnormalities identified in 347 spontaneous abortions collected in Japan. J Obstet Gynaecol Res. 2004;30(3):237–41.
Vogt E et al. Spindle formation, chromosome segregation and the spindle checkpoint in mammalian oocytes and susceptibility to meiotic error. Mutat Res. 2008;651(1–2):14–29.
Kahraman S et al. Results of preimplantation genetic diagnosis in patients with Klinefelter’s syndrome. Reprod Biomed Online. 2003;7(3):346–52.
Staessen C et al. PGD in 47, XXY Klinefelter’s syndrome patients. Hum Reprod Update. 2003;9(4):319–30.
Rives N et al. Assessment of sex chromosome aneuploidy in sperm nuclei from 47, XXY and 46, XY/47, XXY males: comparison with fertile and infertile males with normal karyotype. Mol Hum Reprod. 2000;6(2):107–12.
Mroz K, Hassold TJ, Hunt PA. Meiotic aneuploidy in the XXY mouse: evidence that a compromised testicular environment increases the incidence of meiotic errors. Hum Reprod. 1999;14(5):1151–6.
Scott KL, Hong KH, Scott Jr RT. Selecting the optimal time to perform biopsy for preimplantation genetic testing. Fertil Steril. 2013;100(3):608–14.
McArthur SJ et al. Pregnancies and live births after trophectoderm biopsy and preimplantation genetic testing of human blastocysts. Fertil Steril. 2005;84(6):1628–36.
Scott Jr RT et al. Cleavage-stage biopsy significantly impairs human embryonic implantation potential while blastocyst biopsy does not: a randomized and paired clinical trial. Fertil Steril. 2013;100(3):624–30.
Smith DS. Health care management of adults with Down syndrome. Am Fam Physician. 2001;64(6):1031–8.
Bull MJ, The Committee on Genetics. Health supervision for children with Down syndrome. Pediatrics. 2011;128(2):393–406.
Vintzileos AM et al. Cost-benefit analysis of prenatal diagnosis for Down syndrome using the British or the American approach. Obstet Gynecol. 2000;95(4):577–83.
Skotko BG, Levine SP, Goldstein R. Self-perceptions from people with Down syndrome. Am J Med Genet A. 2011;155A(10):2360–9.
Gath A. Parents as therapists of mentally handicapped children. J Child Psychol Psychiatry. 1979;20(2):165–5.
Gath A. Mentally handicapped people as parents. J Child Psychol Psychiatry. 1988;29(6):739–44.
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule
Healthy life birth after ICSI with PGS in non-mosaic Down syndrome male.
Rights and permissions
About this article
Cite this article
Aghajanova, L., Popwell, J.M., Chetkowski, R.J. et al. Birth of a healthy child after preimplantation genetic screening of embryos from sperm of a man with non-mosaic Down syndrome. J Assist Reprod Genet 32, 1409–1413 (2015). https://doi.org/10.1007/s10815-015-0525-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-015-0525-z