Abstract
Purpose
To assess the effect of streptozotocin induced hyperglycemia on germ cell integrity, DNA ploidy and methylation status for a period of two spermatogenesis cycles in adult male Swiss albino mice.
Methods
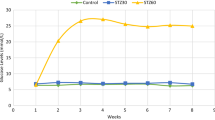
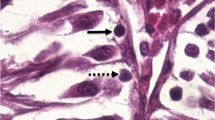
Streptozotocin injected mice were monitored for hyperglycemia at a regular interval for a period of 36 and 72 days. The DNA integrity in epididymal spermatozoa was determined by the comet assay. Flow cytometric analysis was done in germ cells to assess the DNA ploidy. The global methylation analysis in germ cells was done by 5-methyl cytosine immunostaining.
Results
Streptozotocin administration successfully resulted in hyperglycemic response which significantly affected serum testosterone level, sperm DNA integrity and DNA ploidy at the end of 36 days. However, no changes were observed in either epididymal sperm concentration or germ cell methylation status. In contrast, at the end of 76 days, although serum testosterone level, sperm DNA integrity and DNA ploidy status were unperturbed significantly in hyperglycemic group, the epididymal sperm concentration and methylation status of preleptotene/zygotene cells were significantly altered. Importantly, an attempt to find out the association between the blood glucose levels and the abnormalities in hyperglycemic group failed to demonstrate any correlation.
Conclusions
The germ cell abnormalities observed in hyperglycemic group could be interpreted as a primary effect of streptozotocin and not due to hyperglycemia. Our results call for further evaluation of streptozotocin before its application to study the hyperglycemic responses on male germ cells.





Similar content being viewed by others
References
Ballester J, Muñoz MC, Domínguez J, Rigau T, Guinovart JJ, Rodríguez-Gil JE. Insulin-dependent diabetes affects testicular function by FSH- and LH-linked mechanisms. J Androl. 2004;25:706–19.
Agbaje IM, Rogers DA, McVicar CM, McClure N, Atkinson AB, Mallidis C, Lewis SE. Insulin dependent diabetes mellitus: implications for male reproductive function. Hum Reprod. 2007;22:1871–7.
La Vignera S, Condorelli R, Vicari E, D’Agata R, Calogero AE. Diabetes mellitus and sperm parameters: a brief review. J Androl. 2012;33:145–53.
Adiga SK, Upadhya D, Kalthur G, Bola Sadashiva SR, Kumar P. Transgenerational changes in somatic and germ line genetic integrity of first-generation offspring derived from the DNA damaged sperm. Fertil Steril. 2010;93:2486–90.
Goll MG, Bestor TH. Eukaryotic cytosine methyltransferases. Annu Rev Biochem. 2005;74:481–514.
Williams KT, Garrow TA, Schalinske KL. Type I diabetes leads to tissue-specific DNA hypomethylation in male rats. J Nutr. 2008;138:2064–9.
Raketien N, Raketien ML, Nadkarmi M. Studies on the diabetogenic action of Streptozotocin. Cancer Chemother Rep. 1963;29:91–8.
Seethalakshmi L, Menon M, Diamond D. The effect of streptozotocin-induced diabetes on the neuroendocrine-male reproductive tract axis of the adult rat. J Urol. 1987;138:190–4.
Soudamani S, Malini T, Balasubramanian K. Effects of streptozotocin-diabetes and insulin replacement on the epididymis of prepubertal rats: histological and histomorphometric studies. Endocr Res. 2005;31:81–98.
Weiss RB. Streptozocin: a review of its pharmacology, efficacy, and toxicity. Cancer Treat Rep. 1982;66:427–38.
Bolzán AD, Bianchi MS. Genotoxicity of streptozotocin. Mutat Res. 2002;512:121–34.
Singh NP, Stephens RE. X-ray induced DNA double-strand breaks in human sperm. Mutagenesis. 1998;13:75-9.
Krishnamurthy H, Danilovich N, Morales C, Sairam MR. Qualitative and quantitative decline in spermatogenesis of the follicle-stimulating hormone receptor knockout (FORKO) mouse. Biol Reprod. 2000;62:1146–59.
Adiga SK, Ehmcke J, Schlatt S, Kliesch S, Westernströer B, Luetjens CM, Wistuba J, Gromoll J. Reduced expression of DNMT3B in the germ cells of patients with bilateral spermatogenic arrest does not lead to changes in the global methylation status. Mol Hum Reprod. 2011;17:545–9.
Clermont Y, Trott M. Duration of the cycle of the seminiferous epithelium in the mouse and hamster determined by means of 3 H-thymidine and radioautography. Fertil Steril. 1969;20:805–17.
Hassan AA, Hassouna MM, Taketo T, Gagnon C, Elhilali MM. The effect of diabetes on sexual behavior and reproductive tract function in male rats. J Urol. 1993;149:148–54.
Scarano WR, Messias AG, Oliva SU, Klinefelter GR, Kempinas WG. Sexual behaviour, sperm quantity and quality after short-term streptozotocin-induced hyperglycaemia in rats. Int J Androl. 2006;29:482–8.
Jelodar G, Razmi N, Gholampour V. Arginase alteration in the reproductive system of alloxan-diabetic dogs. J Reprod Dev. 2007;53:317–21.
Pontes DA, Fernandes GS, Piffer RC, Gerardin DC, Pereira OC, Kempinas WG. Ejaculatory dysfunction in streptozotocin-induced diabetic rats: the role of testosterone. Pharmacol Rep. 2011;63:130–8.
Murata M, Takahashi A, Saito I, Kawanishi S. Site-specific DNA methylation and apoptosis: induction by diabetogenic streptozotocin. Biochem Pharmacol. 1999;57:881–7.
Kaneda M, Okano M, Hata K, Sado T, Tsujimoto N, Li E, Sasaki H. Essential role for de novo DNA methyltransferase Dnmt3a in paternal and maternal imprinting. Nature. 2004;429:900–03.
Shrilatha B, Muralidhara. Early oxidative stress in testis and epididymal sperm in streptozotocin-induced diabetic mice: its progression and genotoxic consequences. Reprod Toxicol. 2007;23:578–87.
Imaeda A, Kaneko T, Aoki T, Kondo Y, Nagase H. DNA damage and the effect of antioxidants in streptozotocin-treated mice. Food Chem Toxicol. 2002;40(7):979–87.
O’Neill J, Czerwiec A, Agbaje I, Glenn J, Stitt A, McClure N, Mallidis C. Differences in mouse models of diabetes mellitus in studies of male reproduction. Int J Androl. 2010;33:709–16.
Mallidis C, Czerwiec A, Filippi S, O’Neill J, Maggi M, McClure N. Spermatogenic and sperm quality differences in an experimental model of metabolic syndrome and hypogonadal hypogonadism. Reproduction. 2011;142:63–71.
Acknowledgment
Authors would like to acknowledge technical support from Ms. Jayalaxmi Pai and Ms. Kirthi Patil (Clinical Embryology, Kasturba Medical College, Manipal).
This work was partially supported by the intramural funding from Kasturba Medical College, Manipal to RB (Grant # PGR-012).
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule
The germ cell abnormalities observed in streptozotocin induced hyperglycemic mice suggest possible effect of the drug and not due to hyperglycemic response.
Rights and permissions
About this article
Cite this article
Bose, R., Adiga, S.K., D’Souza, F. et al. Germ cell abnormalities in streptozotocin induced diabetic mice do not correlate with blood glucose level. J Assist Reprod Genet 29, 1405–1413 (2012). https://doi.org/10.1007/s10815-012-9873-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-012-9873-0