Abstract
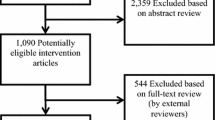
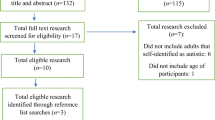
Provider referral is one of the most influential factors in research recruitment. To ease referral burden on providers, we adapted the Best Practice Alert (BPA) in the EPIC Electronic Health Record and assessed its utility in recruiting pediatric patients with autism spectrum disorder for the national SPARK study. During a year-long surveillance, 1203 (64.0%) patients were Interested in SPARK and 223 enrolled. Another 754 participants not recruited via the BPA also enrolled; 35.5% of these participants completed their participation compared to 58.3% of BPA-referred participants. Results suggest that (a) a BPA can successfully engage providers in the study-referral process and (b) families who learn about research through their providers may be more engaged and effectively retained.




Similar content being viewed by others
References
Ahmed, K. L., Simon, A. R., Dempsey, J. R., Samaco, R. C., & Goin-Kochel, R. P. (2020). Radio vs. Facebook: Evaluating two common strategies for research-participant recruitment into autism studies. Journal of Medical Internet Research. https://doi.org/10.2196/16752
Applied Clinical Trials. (2016, January 26). Tufts CSDD Report on New Patient Recruitment/Retention Approaches. Retrieved from http://www.appliedclinicaltrialsonline.com/tufts-csdd-report-new-patient-recruitmentretention-approaches
Baer, A. R., Michaels, M., Good, M. J., & Schapira, L. (2012). Engaging referring physicians in the clinical trial process. Journal of Oncology Practice, 8(1), e8. https://doi.org/10.1200/JOP.2011.000476
Baquet, C. R., Commiskey, P., Mullins, C. D., & Mishra, S. I. (2006). Recruitment and participation in clinical trials: Socio-demographic, rural/urban, and health care access predictors. Cancer Detection and Prevention, 30(1), 24–33. https://doi.org/10.1016/j.cdp.2005.12.001
Carlisle, B., Kimmelman, J., Ramsay, T., & Mackinnon, N. (2014). Unsuccessful trial accrual and human subjects protections: An empirical analysis of recently closed trials. Clinical Trials: Journal of the Society for Clinical Trials, 12(1), 77–83. https://doi.org/10.1177/1740774514558307
Clinical Trial Transformation Initiative. (2018, August 10). Recruitment. Retrieved from https://www.ctti-clinicaltrials.org/projects/recruitment
Devoe, C., Gabbidon, H., Schussler, N., Cortese, L., Caplan, E., Gorman, C., Jethwani, K., Kvedar, J., & Agboola, S. (2019). Use of electronic health records to develop and implement a silent best practice alert notification system for patient recruitment in clinical research: Quality improvement initiative. Journal of Medical Internet Research Medical Informatics, 7(2), e10020. https://doi.org/10.2196/10020
Duhon, G. F., Simon, A. R., Limon, D. L., Ahmed, K. L., Marzano, G., & Goin-Kochel, R. P. (2022). Use of a best practice alert (BPA) to increase diversity within a US-based autism research cohort. Journal of Autism and Developmental Disorders. https://doi.org/10.1007/s10803-021-05407-9
Embi, P. J., Jain, A., Clark, J., Bizjack, S., Hornung, R., & Harris, C. M. (2005). Effect of a clinical trial alert system on physician participation in trial recruitment. Archives of Internal Medicine, 165(19), 2272. https://doi.org/10.1001/archinte.165.19.2272
Embi, P. J., & Leonard, A. C. (2012). Evaluating alert fatigue over time to EHR-based clinical trial alerts: Findings from a randomized controlled study. Journal of the American Medical Informatics Association. https://doi.org/10.1136/amiajnl-2011-000743
Feliciano, P., Daniels, A. M., Snyder, L. A. G., Beaumont, A., Camba, A., Esler, A., Gulsrud, A. G., Mason, A., Gutierrez, A., Nicholson, A., Paolicelli, A. M., McKenzie, A. P., Rachubinski, A. L., Stephens, A. N., Simon, A. R., Stedman, A., Shocklee, A. D., Swanson, A., Finucane, B., et al. (2018). SPARK: A US cohort of 50,000 families to accelerate autism research. Neuron, 97(3), 488–493. https://doi.org/10.1016/j.neuron.2018.01.015
Garrett, P., & Seidman, J. (2011, January 4). EMR vs HER—What's the difference? Retrieved from https://www.healthit.gov/buzz-blog/electronic-health-and-medical-records/emr-vs-ehr-difference
Getz, K. A. (2017). Examining and enabling the role of health care providers as patient engagement facilitators in clinical trials. Clinical Therapeutics, 39(11), 2203–2213. https://doi.org/10.1016/j.clinthera.2017.09.014
Huang, G. D., Bull, J., Mckee, K. J., Mahon, E., Harper, B., & Roberts, J. N. (2018). Clinical trials recruitment planning: A proposed framework from the Clinical Trials Transformation Initiative. Contemporary Clinical Trials, 66, 74–79. https://doi.org/10.1016/j.cct.2018.01.003
Kadam, R., Borde, S., Madas, S., Salvi, S., & Limaye, S. (2016). Challenges in recruitment and retention of clinical trial subjects. Perspectives in Clinical Research, 7(3), 137. https://doi.org/10.4103/2229-3485.184820
Kruse, C. S., Stein, A., Thomas, H., & Kaur, H. (2018). The use of electronic health records to support population health: A systematic review of the literature. Journal of Medical Systems. https://doi.org/10.1007/s10916-018-1075-6
Lai, Y. S., & Afseth, J. D. (2019). A review of the impact of utilising electronic medical records for clinical research recruitment. Clinical Trials, 16(2), 194–203. https://doi.org/10.1177/1740774519829709
Raman, S. R., Curtis, L. H., Temple, R., Andersson, T., Ezekowitz, J., Ford, I., James, S., Marsolo, K., Mirhaji, P., Rocca, M., Rothman, R. L., Sethuraman, B., Stockbridge, N., Terry, S., Wasserman, S. M., Peterson, E. D., & Hernandez, A. F. (2018). Leveraging electronic health records for clinical research. American Heart Journal, 202, 13–19. https://doi.org/10.1016/j.ahj.2018.04.015
Rollman, B. L., Fischer, G. S., Zhu, F., & Belnap, B. H. (2008). Comparison of electronic physician prompts versus waitroom case-finding on clinical trial enrollment. Journal of General Internal Medicine, 23, 447–450. https://doi.org/10.1007/s11606-007-0449-0
Tufts University. (2020, January 28). Drug developers are making strides in streamlining patient recruitment and retention for clinical trials, according to tufts center for the study of drug development [Press release]. Retrieved from https://csdd.tufts.edu/csddnews
Acknowledgments
The authors express their thanks to the SPARK team at the Simons Foundation, the SPARK clinical sites, and the SPARK cohort participants. Although the authors contribute to SPARK as a clinical site (#385052, RPG-K), this project was initiated by the authors without specific or supplemental funding. The sponsors played no role in designing, executing, or writing up the results of this analysis. We are also grateful to Ms. Robin Barton and the EPIC-support team at Texas Children’s Hospital for their collaboration in developing the BPA and exporting the data described in this study. This work was partially supported by the Intellectual and Developmental Disabilities Research Center (1U54 HD083092) at Baylor College of Medicine.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by ARS, KLA, GFD, and RPG. The first draft of the manuscript was written by ARS and KLA, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Robin P. Goin-Kochel has served as a paid consultant in the design of clinical trials for Yamo Pharmaceuticals. All other authors have no known conflicts of interest to disclose.
Ethical Approval
The research reported herein was approved by the Internal Review Board (IRB) of Baylor College of Medicine. Human participants were involved and the IRB approved a waiver of informed consent because of the chartreview methodology.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Simon, A.R., Ahmed, K.L., Limon, D.L. et al. Utilization of a Best Practice Alert (BPA) at Point-of-Care for Recruitment into a US-Based Autism Research Study. J Autism Dev Disord 53, 359–369 (2023). https://doi.org/10.1007/s10803-022-05444-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-022-05444-y