Abstract
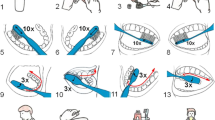
Visual pedagogy and social stories have been widely used to assist children with Autism Spectrum Disorder (ASD) in learning various skills. A toothbrushing visual pedagogy (TBVP) was developed adapting existing toothbrushing social stories for children with ASD. This TBVP consists of 13 toothbrushing steps with scripts describing the toothbrushing technique. To evaluate its feasibility, a review panel was formed to provide feedback on the TBVP and three other published toothbrushing social stories. Effectiveness of the TBVP was further evaluated among 119 preschool children with ASD with significant improvements in toothbrushing skills observed at 3-month and 6-month follow-ups. It is concluded that TBVP is a feasible and an effective educational means that assists children with ASD in learning toothbrushing skills.


Similar content being viewed by others
References
Adams, L., Gouvousis, A., VanLue, M., & Waldron, C. (2004). Social story intervention: Improving communication skills in a child with an autism spectrum disorder. Focus on Autism and Other Developmental Disabilities, 19(2), 87–94.
Al-Batayneh, O., Nazer, T., Khader, Y., & Owais, A. (2019). Effectiveness of a tooth-brushing programme using the picture exchange communication system (PECS) on gingival health of children with autism spectrum disorders. European Archives of Paediatric Dentistry, 1–7.
Annaz, D., Remington, A., Milne, E., Coleman, M., Campbell, R., Thomas, M. S., & Swettenham, J. (2010). Development of motion processing in children with autism. Developmental Science, 13(6), 826–838.
Asma’a, M. S., Badr, S. B., & Rashed, M. A. (2013). Effectiveness of audiovisual modeling on the behavioral change toward oral and dental care in children with autism. Indian Journal of Dentistry, 4(4), 184–190.
Attin, T., & Hornecker, E. (2005). Tooth brushing and oral health: how frequently and when should tooth brushing be performed? Oral Health & Preventive Dentistry, 3(3).
Bäckman, B., & Pilebro, C. (1999). Visual pedagogy in dentistry for children with autism. ASDC Journal of Dentistry for Children, 66(5), 325.
Belmonte, M. K., & Yurgelun-Todd, D. A. (2003). Functional anatomy of impaired selective attention and compensatory processing in autism. Cognitive Brain Research, 17(3), 651–664.
Bennetto, L., Pennington, B. F., & Rogers, S. J. (1996). Intact and impaired memory functions in autism. Child Development, 67(4), 1816–1835.
Bondy, A. S., & Frost, L. A. (1994). The picture exchange communication system. Focus on Autistic Behavior, 9(3), 1–19.
Buzalaf, M., & Levy, S. M. (2011). Fluoride intake of children: considerations for dental caries and dental fluorosis. Monographs in oral science, 22, 1–19. https://doi.org/10.1159/000325101
Chan, D., Chan, S., So, H., Li, A., Ng, R., & Tsang, N. (2014). Dental Health of Preschool Children with Autism Spectrum Disorder in Hong Kong 香港自閉症學前兒童的牙科保健. HK Journal of Paediatrics (new series), 19(3), 161–168.
Chistol, L. T., Bandini, L. G., Must, A., Phillips, S., Cermak, S. A., & Curtin, C. (2018). Sensory sensitivity and food selectivity in children with autism spectrum disorder. Journal of Autism and Developmental Disorders, 48(2), 583–591.
Delano, M., & Snell, M. E. (2006). The effects of social stories on the social engagement of children with autism. Journal of Positive Behavior Interventions, 8(1), 29–42.
Du, R., Yiu, C., & King, N. (2019). Health-and oral health-related quality of life among preschool children with autism spectrum disorders. European Archives of Paediatric Dentistry, 1–9.
El Khatib, A. A., El Tekeya, M. M., El Tantawi, M. A., & Omar, T. (2014). Oral health status and behaviours of children with Autism Spectrum Disorder: a case–control study. International Journal of Paediatric Dentistry, 24(4), 314–323.
Flippin, M., Reszka, S., & Watson, L. R. (2010). Effectiveness of the Picture Exchange Communication System (PECS) on communication and speech for children with autism spectrum disorders: A meta-analysis. American Journal of Speech-Language Pathology.
Ganz, J. B., Kaylor, M., Bourgeois, B., & Hadden, K. (2008). The impact of social scripts and visual cues on verbal communication in three children with autism spectrum disorders. Focus on Autism and Other Developmental Disabilities, 23(2), 79–94.
Geschwind, D. H., & Levitt, P. (2007). Autism spectrum disorders: developmental disconnection syndromes. Current opinion in neurobiology, 17(1), 103–111.
Gray, C. A., & Garand, J. D. (1993). Social stories: Improving responses of students with autism with accurate social information. Focus on Autistic Behavior, 8(1), 1–10.
Hagiwara, T., & Smith Myles, B. (1999). A multimedia social story intervention: Teaching skills to children with autism. Focus on Autism and Other Developmental Disabilities, 14(2), 82–95.
Handsinautism.org. (1995). Time to brush your teeth. http://www.handsinautism.org/.
Happé, F., & Frith, U. (2006). The weak coherence account: detail-focused cognitive style in autism spectrum disorders. Journal of Autism and Developmental Disorders, 36(1), 5–25. https://doi.org/10.1007/s10803-005-0039-0
Jasmin, E., Couture, M., McKinley, P., Reid, G., Fombonne, E., & Gisel, E. (2009). Sensori-motor and daily living skills of preschool children with autism spectrum disorders. Journal of Autism and Developmental Disorders, 39(2), 231–241. https://doi.org/10.1007/s10803-008-0617-z
Johnson, C. P., & Myers, S. M. (2007). Identification and evaluation of children with autism spectrum disorders. Pediatrics, 120(5), 1183–1215. https://doi.org/10.1542/peds.2007-2361
Kang, B. H., Park, S. N., Sohng, K. Y., & Moon, J. S. (2008). Effect of a tooth-brushing education program on oral health of preschool children. Journal of Korean Academy of Nursing, 38(6), 914–922. https://doi.org/10.4040/jkan.2008.38.6.914
Kokina, A., & Kern, L. (2010). Social Story interventions for students with autism spectrum disorders: a meta-analysis. Journal of Autism and Developmental Disorders, 40(7), 812–826. https://doi.org/10.1007/s10803-009-0931-0
Kuoch, H., & Mirenda, P. (2003). Social story interventions for young children with autism spectrum disorders. Focus on Autism and Other Developmental Disabilities, 18(4), 219–227.
Lam, P. P., Du, R., Peng, S., McGrath, C. P., & Yiu, C. K. (2020). Oral health status of children and adolescents with autism spectrum disorder: A systematic review of case-control studies and meta-analysis. Autism, 24(5), 1047–1066. https://doi.org/10.1177/1362361319877337
Landa, R. J., Holman, K. C., O’Neill, A. H., & Stuart, E. A. (2011). Intervention targeting development of socially synchronous engagement in toddlers with autism spectrum disorder a randomized controlled trial. Journal of Child Psychology and Psychiatry, 52(1), 13–21.
Landry, R., & Bryson, S. E. (2004). Impaired disengagement of attention in young children with autism. The Journal of Child Psychology and Psychiatry, 45(6), 1115–1122. https://doi.org/10.1111/j.1469-7610.2004.00304.x
Lopez Cazaux, S., Lefer, G., Rouches, A., & Bourdon, P. (2019). Toothbrushing training programme using an iPad(®) for children and adolescents with autism. European Archives of Paediatric Dentistry, 20(3), 277–284. https://doi.org/10.1007/s40368-018-0396-y
Lord, C., Cook, E. H., Leventhal, B. L., & Amaral, D. G. (2000). Autism spectrum disorders. Neuron, 28(2), 355–363. https://doi.org/10.1016/s0896-6273(00)00115-x
Mesibov, G. B., Shea, V., & Schopler, E. (2005). The TEACCH approach to autism spectrum disorders. Boston: Springer Science & Business Media.
Nilchian, F., Shakibaei, F., & Jarah, Z. T. (2017). Evaluation of Visual Pedagogy in Dental Check-ups and Preventive Practices Among 6–12-Year-Old Children with Autism. Journal of Autism and Developmental Disorders, 47(3), 858–864. https://doi.org/10.1007/s10803-016-2998-8
O’connor, E. . (2009). The use of social story DVDs to reduce anxiety levels: A case study of a child with autism and learning disabilities. Support for Learning, 24(3), 133–136.
Orellana, L. M., Martínez-Sanchis, S., & Silvestre, F. J. (2014). Training adults and children with an autism spectrum disorder to be compliant with a clinical dental assessment using a TEACCH-based approach. Journal of Autism and Developmental Disorders, 44(4), 776–785. https://doi.org/10.1007/s10803-013-1930-8
Pani, S. C., Mubaraki, S. A., Ahmed, Y. T., Alturki, R. Y., & Almahfouz, S. F. (2013). Parental perceptions of the oral health-related quality of life of autistic children in Saudi Arabia. Special Care in Dentistry, 33(1), 8–12. https://doi.org/10.1111/j.1754-4505.2012.00294.x
Pearson, L., & Smit, J. (2003). Xiaohai zenyang xuehui shuaya ne? [How do kids learn to brush their teeth?] Spastics Association of Hong Kong, Trans.
Pilebro, C., & Bäckman, B. (2005). Teaching oral hygiene to children with autism. International Journal of Paediatric Dentistry, 15(1), 1–9. https://doi.org/10.1111/j.1365-263X.2005.00589.x
Preston, D., & Carter, M. (2009). A review of the efficacy of the picture exchange communication system intervention. Journal of Autism and Developmental Disorders, 39(10), 1471–1486. https://doi.org/10.1007/s10803-009-0763-y
Provost, B., Crowe, T. K., Acree, K., Osbourn, P. L., & McClain, C. (2009). Sensory behaviors of preschool children with and without autism spectrum disorders. New Zealand Journal of Occupational Therapy, 56(2).
Reichow, B., & Sabornie, E. J. (2009). Brief report: Increasing verbal greeting initiations for a student with autism via a Social StoryTM intervention. Journal of Autism and Developmental Disorders, 39(12), 1740–1743. https://doi.org/10.1007/s10803-009-0814-4
Sansosti, F. J., Powell-Smith, K. A., & Kincaid, D. (2004). A research synthesis of social story interventions for children with autism spectrum disorders. Focus on Autism and Other Developmental Disabilities, 19(4), 194–204.
Scattone, D., Wilczynski, S. M., Edwards, R. P., & Rabian, B. (2002). Decreasing disruptive behaviors of children with autism using social stories. Journal of Autism and Developmental Disorders, 32(6), 535–543. https://doi.org/10.1023/a:1021250813367
Schwartz, I. S., Garfinkle, A. N., & Bauer, J. (1998). The Picture Exchange Communication System: Communicative outcomes for young children with disabilities. Topics in Early Childhood Special Education, 18(3), 144–159.
Seow, W. K., Cheng, E., & Wan, V. (2003). Effects of oral health education and tooth-brushing on mutans streptococci infection in young children. Pediatric Dentistry, 25(3), 223–228.
Stripling, E., Whitney, R., Danquah-Brobby, P. F., & Walton, C. (2013). Healthy Smiles for Autism: Oral Hygiene Tips for Children with Autism Spectrum Disorder. National Museum of Dentistry. . https://vkc.mc.vanderbilt.edu/assets/files/resources/healthy-smiles-for-autism.pdf.
Swaggart, B. L., Gagnon, E., Bock, S. J., Earles, T. L., Quinn, C., Myles, B. S., & Simpson, R. L. (1995). Using social stories to teach social and behavioral skills to children with autism. Focus on Autistic Behavior, 10(1), 1–16.
Thiemann, K. S., & Goldstein, H. (2001). Social stories, written text cues, and video feedback: Effects on social communication of children with autism. Journal of applied behavior analysis, 34(4), 425–446.
Tomchek, S. D., & Dunn, W. (2007). Sensory processing in children with and without autism: a comparative study using the short sensory profile. American Journal of Occupational Therapy, 61(2), 190–200.
Tsang, S. K., Shek, D. T., Lam, L. L., Tang, F. L., & Cheung, P. M. (2007). Brief Report: Application of the TEACCH Program on Chinese Pre-School Children with Autism––Does Culture Make a Difference? Journal of Autism and Developmental Disorders, 37(2), 390–396.
Virues-Ortega, J., Julio, F. M., & Pastor-Barriuso, R. (2013). The TEACCH program for children and adults with autism: A meta-analysis of intervention studies. Clinical Psychology Review, 33(8), 940–953.
Watling, R. L., Deitz, J., & White, O. (2001). Comparison of Sensory Profile scores of young children with and without autism spectrum disorders. American Journal of Occupational Therapy, 55(4), 416–423.
Zhou, N., Wong, H. M., & McGrath, C. (2020). Efficacy of Social Story Intervention in Training Toothbrushing Skills Among Special-Care Children With and Without Autism. Autism Research, 13(4), 666–674. https://doi.org/10.1002/aur.2256
Acknowledgements
We would like to give many thanks to the children and parents who participated in this study. And we also appreciate the teachers, nurses and social workers in the Special Child Care Centres Hong Kong for their time and efforts spent in this study. Last but not least, we would like to thank all the people who contributed in this study, including the panel specialists, technicians, DSAs and librarians.
Funding
The work described was supported by the General Research Fund (GRF) from the Research Grants Council of the Hong Kong Special Administrative Region, China (Project No. 17116014).
Author information
Authors and Affiliations
Contributions
RYD conceptualized, designed and conducted the study. RYD and WY drafted the initial manuscript and reviewed and revised all drafts of the manuscript. CKYY and CPM helped conceptualize the study and provided critical reviews of intellectual content. WY and PPYL provided critical reviews of the manuscript and ensured data represented in tables and text were accurate. All authors approved the final manuscript as submitted.
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Du, R.Y., Yang, W., Lam, P.P.Y. et al. Developing a Toothbrushing Visual Pedagogy (TBVP) for Preschool Children with Autism Spectrum Disorder. J Autism Dev Disord 52, 327–338 (2022). https://doi.org/10.1007/s10803-021-04946-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-021-04946-5