Abstract
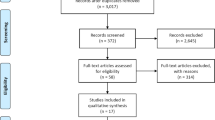
We performed a systematic literature search regarding maternal diabetes before and during pregnancy and the risk of autism spectrum disorders (ASD) in the offspring. Of the 178 potentially relevant articles, 12 articles including three cohort studies and nine case–control studies were included in the meta-analysis. Both the meta-analyses of cohort studies and case–control studies showed significant associations. The pooled relative risk and 95 % confidence interval (CI) among cohort studies was 1.48 (1.25–1.75, p < 0.001). For case–control studies, the pooled odds ratio and 95 % CI was 1.72 (1.24–2.41, p = 0.001). No indication of significant heterogeneity across studies or publication bias was observed. In conclusion, maternal diabetes was significantly associated with a greater risk of ASD in the offspring.




Similar content being viewed by others
Abbreviations
- ADI-R:
-
Autism diagnostic interview-revised
- ADOS:
-
The autism diagnostic observation schedule
- ASD:
-
Autism spectrum disorders
- CARS:
-
The childhood autism rating scale
- CI:
-
Confidence interval
- DSM-IV:
-
The diagnostic and statistical manual of mental disorders, fourth edition
- ICD:
-
International classification of diseases
- OR:
-
Odds ratio
- RR:
-
Relative risk
References
Albrecht, S. S., Kuklina, E. V., Bansil, P., Jamieson, D. J., Whiteman, M. K., Kourtis, A. P., et al. (2010). Diabetes trends among delivery hospitalizations in the US, 1994–2004. Diabetes Care, 33, 768–773.
American Diabetes Association. (2004). Gestational diabetes mellitus. Diabetes Care, 27(Suppl 1), S88–S90.
American Diabetes Association. (2013). Diagnosis and classification of diabetes mellitus. Diabetes Care, 36(Suppl 1), S67–S74.
Anderson, J. L., Waller, D. K., Canfield, M. A., Shaw, G. M., Watkins, M. L., & Werler, M. M. (2005). Maternal obesity, gestational diabetes, and central nervous system birth defects. Epidemiology, 16, 87–92.
Autism and Developmental Disabilities Monitoring Network Surveillance Year 2008 Principal Investigators; Centers for Disease Control and Prevention. (2012). Prevalence of autism spectrum disorders–Autism and Developmental Disabilities Monitoring Network, 14 sites, United States, 2008. MMWR Surveill Summ, 61, 1–19.
Bailey, A., Le Couteur, A., Gottesman, I., Bolton, P., Simonoff, E., Yuzda, E., et al. (1995). Autism as a strongly genetic disorder: evidence from a British twin study. Psychological Medicine, 25, 63–77.
Bardenheier, B. H., Elixhauser, A., Imperatore, G., Devlin, H. M., Kuklina, E. V., Geiss, L. S., et al. (2013). Variation in prevalence of gestational diabetes mellitus among hospital discharges for obstetric delivery across 23 states in the United States. Diabetes Care, 36, 1209–1214.
Bell, R., Bailey, K., Cresswell, T., Hawthorne, G., Critchley, J., & Lewis-Barned, N. (2008). Trends in prevalence and outcomes of pregnancy in women with pre-existing type I and type II diabetes. BJOG: An International Journal of Obstetrics and Gynaecology, 115, 445–452.
Biri, A., Onan, A., Devrim, E., Babacan, F., Kavutcu, M., & Durak, I. (2006). Oxidant status in maternal and cord plasma and placental tissue in gestational diabetes. Placenta, 27, 327–332.
Brimacombe, M., Ming, X., & Lamendola, M. (2007). Prenatal and birth complications in autism. Maternal and Child Health Journal, 11, 73–79.
Buchmayer, S., Johansson, S., Johansson, A., Hultman, C. M., Sparen, P., & Cnattingius, S. (2009). Can association between preterm birth and autism be explained by maternal or neonatal morbidity? Pediatrics, 124, e817–e825.
Burstyn, I., Sithole, F., & Zwaigenbaum, L. (2010). Autism spectrum disorders, maternal characteristics and obstetric complications among singletons born in Alberta, Canada. Chronic Diseases in Canada, 30, 125–134.
Burstyn, I., Wang, X., Yasui, Y., Sithole, F., & Zwaigenbaum, L. (2011). Autism spectrum disorders and fetal hypoxia in a population-based cohort: accounting for missing exposures via Estimation-Maximization algorithm. BMC Medical Research Methodology, 11, 2.
Chauhan, A., Chauhan, V., Brown, W. T., & Cohen, I. (2004). Oxidative stress in autism: increased lipid peroxidation and reduced serum levels of ceruloplasmin and transferrin–the antioxidant proteins. Life Sciences, 75, 2539–2549.
Chen, X., & Scholl, T. O. (2005). Oxidative stress: Changes in pregnancy and with gestational diabetes mellitus. Current Diabetes Reports, 5, 282–288.
Croen, L. A., Grether, J. K., Yoshida, C. K., Odouli, R., & Van de Water, J. (2005). Maternal autoimmune diseases, asthma and allergies, and childhood autism spectrum disorders: A case-control study. Archives of Pediatrics and Adolescent Medicine, 159, 151–157.
DerSimonian, R., & Laird, N. (1986). Meta-analysis in clinical trials. Controlled Clinical Trials, 7, 177–188.
Dodds, L., Fell, D. B., Shea, S., Armson, B. A., Allen, A. C., & Bryson, S. (2011). The role of prenatal, obstetric and neonatal factors in the development of autism. Journal of Autism and Developmental Disorders, 41, 891–902.
Egger, M., Davey Smith, G., Schneider, M., & Minder, C. (1997). Bias in meta-analysis detected by a simple, graphical test. BMJ, 315, 629–634.
Eidelman, A. I., & Samueloff, A. (2002). The pathophysiology of the fetus of the diabetic mother. Seminars in Perinatology, 26, 232–236.
Elhameed, M. A. A., Elbaky, A. E. O. A., & Kamel, E. A. (2011). A controlled study of the risk factors and clinical picture of children with autism in an Egyptian sample. Egypt Journal of Neurology, Neurosurgery and Psychiatry, 48, 271–276.
Fernandez-Morera, J. L., Rodriguez-Rodero, S., Menendez-Torre, E., & Fraga, M. F. (2010). The possible role of epigenetics in gestational diabetes: Cause, consequence, or both. Obstetrics and Gynecology International, 2010, 605163.
Ferrara, A. (2007). Increasing prevalence of gestational diabetes mellitus: A public health perspective. Diabetes Care, 30(Suppl 2), S141–S146.
Gardener, H., Spiegelman, D., & Buka, S. L. (2009). Prenatal risk factors for autism: Comprehensive meta-analysis. British Journal of Psychiatry, 195, 7–14.
Gardener, H., Spiegelman, D., & Buka, S. L. (2011). Perinatal and neonatal risk factors for autism: A comprehensive meta-analysis. Pediatrics, 128, 344–355.
Georgieff, M. K. (2006). The effect of maternal diabetes during pregnancy on the neurodevelopment of offspring. Minnesota Medicine, 89, 44–47.
Gillberg, C. (1999). Neurodevelopmental processes and psychological functioning in autism. Development and Psychopathology, 11, 567–587.
Guinchat, V., Thorsen, P., Laurent, C., Cans, C., Bodeau, N., & Cohen, D. (2012). Pre-, peri- and neonatal risk factors for autism. Acta Obstetricia et Gynecologica Scandinavica, 91, 287–300.
Hayes, D. K., Fan, A. Z., Smith, R. A., & Bombard, J. M. (2011). Trends in selected chronic conditions and behavioral risk factors among women of reproductive age, behavioral risk factor surveillance system, 2001–2009. Preventing Chronic Disease, 8, A120.
Herrera, E., & Ortega-Senovilla, H. (2010). Disturbances in lipid metabolism in diabetic pregnancy: Are these the cause of the problem? Best Practice and Research Clinical Endocrinology and Metabolism, 24, 515–525.
Higgins, J. P., & Thompson, S. G. (2002). Quantifying heterogeneity in a meta-analysis. Statistics in Medicine, 21, 1539–1558.
Huerta, J. M., Tormo, M. J., Egea-Caparros, J. M., Ortola-Devesa, J. B., & Navarro, C. (2009). Accuracy of self-reported diabetes, hypertension and hyperlipidemia in the adult Spanish population. DINO study findings. Revista Espanola de Cardiologia, 62, 143–152.
Hultman, C. M., Sparen, P., & Cnattingius, S. (2002). Perinatal risk factors for infantile autism. Epidemiology, 13, 417–423.
International Diabetes Federation. (2013) IDF Policy Briefing: Diabetes in Pregnancy: Protecting Maternal Health. Accessed July 10, 2013, from http://www.idf.org/sites/default/files/Policy_Briefing_DiabetesInPregancy.pdf.
Juul-Dam, N., Townsend, J., & Courchesne, E. (2001). Prenatal, perinatal, and neonatal factors in autism, pervasive developmental disorder-not otherwise specified, and the general population. Pediatrics, 107, E63.
Keil, A., Daniels, J. L., Forssen, U., Hultman, C., Cnattingius, S., Soderberg, K. C., et al. (2010). Parental autoimmune diseases associated with autism spectrum disorders in offspring. Epidemiology, 21, 805–808.
Kolevzon, A., Gross, R., & Reichenberg, A. (2007). Prenatal and perinatal risk factors for autism: a review and integration of findings. Archives of Pediatrics and Adolescent Medicine, 161, 326–333.
Krakowiak, P., Walker, C. K., Bremer, A. A., Baker, A. S., Ozonoff, S., Hansen, R. L., et al. (2012). Maternal metabolic conditions and risk for autism and other neurodevelopmental disorders. Pediatrics, 129, e1121–e1128.
Leonard, H., de Klerk, N., Bourke, J., & Bower, C. (2006). Maternal health in pregnancy and intellectual disability in the offspring: A population-based study. Annals of Epidemiology, 16, 448–454.
Levy, S. E., Mandell, D. S., & Schultz, R. T. (2009). Autism. Lancet, 374, 1627–1638.
London, E. A. (2000). The environment as an etiologic factor in autism: A new direction for research. Environmental Health Perspectives, 108(Suppl 3), 401–404.
Lyall, K., Pauls, D. L., Spiegelman, D., Ascherio, A., & Santangelo, S. L. (2012). Pregnancy complications and obstetric suboptimality in association with autism spectrum disorders in children of the Nurses’ Health Study II. Autism Research, 5, 21–30.
Ming, X., Stein, T. P., Brimacombe, M., Johnson, W. G., Lambert, G. H., & Wagner, G. C. (2005). Increased excretion of a lipid peroxidation biomarker in autism. Prostaglandins Leukotrienes and Essential Fatty Acids, 73, 379–384.
National Institute for Health and Care Excellence. (2009). NICE clinical guidelines 63: Diabetes in pregnancy: Management of diabetes and its complications from pre-conception to the postnatal period. Accessed July 10, 2013, from http://guidance.nice.org.uk/CG63.
Newschaffer, C. J., Croen, L. A., Daniels, J., Giarelli, E., Grether, J. K., Levy, S. E., et al. (2007). The epidemiology of autism spectrum disorders. Annual Review of Public Health, 28, 235–258.
Okura, Y., Urban, L. H., Mahoney, D. W., Jacobsen, S. J., & Rodeheffer, R. J. (2004). Agreement between self-report questionnaires and medical record data was substantial for diabetes, hypertension, myocardial infarction and stroke but not for heart failure. Journal of Clinical Epidemiology, 57, 1096–1103.
Onore, C., Careaga, M., & Ashwood, P. (2012). The role of immune dysfunction in the pathophysiology of autism. Brain, Behavior, and Immunity, 26, 383–392.
Ornoy, A., Ratzon, N., Greenbaum, C., Wolf, A., & Dulitzky, M. (2001). School-age children born to diabetic mothers and to mothers with gestational diabetes exhibit a high rate of inattention and fine and gross motor impairment. Journal of Pediatric Endocrinology and Metabolism, 14(Suppl 1), 681–689.
Piven, J., Simon, J., Chase, G. A., Wzorek, M., Landa, R., Gayle, J., et al. (1993). The etiology of autism: Pre-, peri- and neonatal factors. Journal of the American Academy of Child and Adolescent Psychiatry, 32, 1256–1263.
Rapin, I. (2002). The autistic-spectrum disorders. New England Journal of Medicine, 347, 302–303.
Rizzo, T. A., Dooley, S. L., Metzger, B. E., Cho, N. H., Ogata, E. S., & Silverman, B. L. (1995). Prenatal and perinatal influences on long-term psychomotor development in offspring of diabetic mothers. American Journal of Obstetrics and Gynecology, 173, 1753–1758.
Rodier, P. M., Ingram, J. L., Tisdale, B., Nelson, S., & Romano, J. (1996). Embryological origin for autism: developmental anomalies of the cranial nerve motor nuclei. Journal of Comparative Neurology, 370, 247–261.
Schanen, N. C. (2006). Epigenetics of autism spectrum disorders. Hum Mol Genet, 15(2), R138–R150.
Solomon, C. G., Willett, W. C., Carey, V. J., Rich-Edwards, J., Hunter, D. J., Colditz, G. A., et al. (1997). A prospective study of pregravid determinants of gestational diabetes mellitus. The Journal of the American Medical Association, 278, 1078–1083.
Stern, M. (2011). Insulin signaling and autism. Frontiers in Endocrinology, 2, 54.
Stroup, D. F., Berlin, J. A., Morton, S. C., Olkin, I., Williamson, G. D., Rennie, D., et al. (2000). Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. The Journal of the American Medical Association, 283, 2008–2012.
Van den Bergh, B. R. (2011). Developmental programming of early brain and behaviour development and mental health: a conceptual framework. Developmental Medicine and Child Neurology, 53(Suppl 4), 19–23.
Wells, G. A., Shea, B., O’Connell, D., Peterson, J., Welch, V., Losos, M., et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality if nonrandomized studies in meta-analyses. Accessed January 30, 2013, from http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm.
Wong, V. C., & Hui, S. L. (2008). Epidemiological study of autism spectrum disorder in China. Journal of Child Neurology, 23, 67–72.
Yao, Y., Walsh, W. J., McGinnis, W. R., & Pratico, D. (2006). Altered vascular phenotype in autism: correlation with oxidative stress. Archives of Neurology, 63, 1161–1164.
Acknowledgments
This study was funded by the National Natural Science Foundation of China (No. 81172687) and the Doctoral Fund of Ministry of Education of China (No. 20110171110053). Dr. Wei Bao was supported by the Intramural Research Program of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institutes of Health, USA.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Registration: This review was registered at the PROSPERO as CRD42012003373.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xu, G., Jing, J., Bowers, K. et al. Maternal Diabetes and the Risk of Autism Spectrum Disorders in the Offspring: A Systematic Review and Meta-Analysis. J Autism Dev Disord 44, 766–775 (2014). https://doi.org/10.1007/s10803-013-1928-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-013-1928-2