Abstract
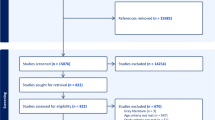
Many evidence-based treatments (EBTs) have been identified for specific child mental health disorders, but there is limited research on the use of EBTs in community-based settings. This study used administrative data from a statewide system of care to examine 1) the extent to which EBTs were provided congruent with the child’s primary diagnosis, 2) whether there were differences in effectiveness of EBTs that were congruent or incongruent with the child’s primary diagnosis, and 3) whether comorbidity moderated the effectiveness of EBTs for children based on congruence with their primary diagnosis. The sample consisted of 23,895 children ages 3–17 with at least one of the most common diagnoses (attention-deficit/hyperactivity disorder, conduct problems, depressive disorders, anxiety disorders, and post-traumatic stress disorder) who received outpatient psychotherapy. Data were collected as part of routine care, including child demographic characteristics, diagnosis, treatment type, and problem severity. Forty-two percent of children received an EBT congruent with their diagnosis, and these children showed greater improvement than the 35% of children who received no EBT (ES = 0.14–0.16) or the 23% who received an EBT incongruent with their diagnosis (ES = 0.06–0.15). For children with comorbid diagnoses, the use of EBTs congruent with the primary diagnosis was also associated with the greatest improvement, especially when compared to no EBT (ES = 0.22–0.24). Results of the current study support the use of EBTs in community-based settings, and suggest that clinicians should select EBTs that match the child’s primary diagnosis to optimize treatment outcomes, especially for children with comorbidity.

Similar content being viewed by others
Notes
For simplicity, “comorbidity” is used in this paper to refer to children with more than one diagnosis.
References
Alisic, E., Zalta, A. K., Van Wesel, F., Larsen, S. E., Hafstad, G. S., Hassanpour, K., & Smid, G. E. (2014). Rates of post-traumatic stress disorder in trauma-exposed children and adolescents: Meta-analysis. The British Journal of Psychiatry, 204(5), 335–340. https://doi.org/10.1192/bjp.bp.113.131227
Baker-Ericzén, M. J., Hurlburt, M. S., Brookman-Frazee, L., Jenkins, M. M., & Hough, R. L. (2010). Comparing child, parent, and family characteristics in usual care and empirically supported treatment research samples for children with disruptive behavior disorders. Journal of Emotional and Behavioral Disorders, 18(2), 82–99. https://doi.org/10.1177/1063426609336956
Barkley, R. A. (2013). Defiant children: A clinician’s manual for assessment and parent training. The Guilford Press.
Cary, C. E., & McMillen, J. C. (2012). The data behind the dissemination: A systematic review of trauma-focused cognitive behavioral therapy for use with children and youth. Children and Youth Services Review, 34(4), 748–757. https://doi.org/10.1016/j.childyouth.2012.01.003
Chorpita, B. F., Daleiden, E. L., & Weisz, J. R. (2005). Identifying and selecting the common elements of evidence based interventions: A distillation and matching model. Mental Health Services Research, 7(1), 5–20. https://doi.org/10.1007/s11020-005-1962-6
Chorpita, B. F., Daleiden, E. L., Ebesutani, C., Young, J., Becker, K. D., Nakamura, B. J., Phillips, L., Ward, A., Lynch, R., Trent, L., Smith, R. L., Okamura, K., & Starace, N. (2011). Evidence-based treatments for children and adolescents: An updated review of indicators of efficacy and effectiveness. Clinical Psychology: Science and Practice, 18(2), 154–172. https://doi.org/10.1111/j.1468-2850.2011.01247.x
Chorpita, B. F., Daleiden, E. L., Park, A. L., Ward, A. M., Levy, M. C., Cromley, T., Chiu, A. W., Letamendi, A. M., Tsai, K. H., & Krull, J. L. (2017). Child STEPs in California: A cluster randomized effectiveness trial comparing modular treatment with community implemented treatment for youth with anxiety, depression, conduct problems, or traumatic stress. Journal of Consulting and Clinical Psychology, 85(1), 13–25. https://doi.org/10.1037/ccp0000133
Chorpita, B. F., Weisz, J. R., Daleiden, E. L., Schoenwald, S. K., Palinkas, L. A., Miranda, J., Higa-McMillan, C. K., Nakamura, B. J., Austin, A. A., Borntrager, C. F., Ward, A., Wells, K. C., Gibbons, R., & Research Network on Youth Mental Health. (2013). Long-term outcomes for the Child STEPs randomized effectiveness trial: A comparison of modular and standard treatment designs with usual care. Journal of Consulting and Clinical Psychology, 81(6), 999–1099. https://doi.org/10.1037/a0034200
Cohen, J. A., Mannarino, A. P., & Deblinger, E. (2017). Treating trauma and traumatic grief in children and adolescents. The Guilford Press.
Conners, C. K. (2002). Forty years of methylphenidate treatment in attention-deficit/ hyperactivity disorder. Journal of Attention Disorders, 6(Suppl. 1), S17–S30. https://doi.org/10.1177/070674370200601S04
Deighton, J., Argent, R., De Francesco, D., Edbrooke-Childs, J., Jacob, J., Fleming, I., Ford, T., & Wolpert, M. (2016). Associations between evidence-based practice and mental health outcomes in child and adolescent mental health services. Clinical Child Psychology and Psychiatry, 21(2), 287–296. https://doi.org/10.1177/1359104515589637
Dorsey, S., McLaughlin, K. A., Kerns, S. E., Harrison, J. P., Lambert, H. K., Briggs, E. C., Cox, J. R., & Amaya-Jackson, L. (2017). Evidence base update for psychosocial treatments for children and adolescents exposed to traumatic events. Journal of Clinical Child & Adolescent Psychology, 46(3), 303–330. https://doi.org/10.1080/15374416.2016.1220309
Durlak, J. A. (2009). How to select, calculate, and interpret effect sizes. Journal of Pediatric Psychology, 34(9), 917–928. https://doi.org/10.1093/jpepsy/jsp004
Evans, S. W., Owens, J. S., & Bunford, N. (2014). Evidence-based psychosocial treatments for children and adolescents with attention-deficit/hyperactivity disorder. Journal of Clinical Child & Adolescent Psychology, 43(4), 527–551. https://doi.org/10.1080/15374416.2013.850700
Evans, S. W., Owens, J. S., & Power, T. J. (2019). Attention-deficit/hyperactivity disorder. In M. J. Prinstein, E. A. Youngstrom, E. J. Mash, & R. A. Barkley (Eds.), Treatment of disorders in childhood and adolescence (pp. 47–101). The Guilford Press.
Finkelhor, D., Turner, H. A., Shattuck, A., & Hamby, S. L. (2015). Prevalence of childhood exposure to violence, crime, and abuse: Results from the national survey of children’s exposure to violence. JAMA Pediatrics, 169(8), 746–754. https://doi.org/10.1001/jamapediatrics.2015.0676
Garland, A. F., Accurso, E. C., Haine-Schlagel, R., Brookman-Frazee, L., Roesch, S., & Zhang, J. J. (2014). Searching for elements of evidence-based practices in children’s usual care and examining their impact. Journal of Clinical Child & Adolescent Psychology, 43(2), 201–215. https://doi.org/10.1080/15374416.2013.869750
Garland, A. F., Brookman-Frazee, L., Hurlburt, M. S., Accurso, E. C., Zoffness, R. J., Haine-Schlagel, R., & Ganger, W. (2010). Mental health care for children with disruptive behavior problems: A view inside therapists’ offices. Psychiatric Services, 61(8), 788–795. https://doi.org/10.1176/ps.2010.61.8.788
Garland, A. F., Hough, R. L., McCabe, K. M., Yeh, M. A. Y., Wood, P. A., & Aarons, G. A. (2001). Prevalence of psychiatric disorders in youths across five sectors of care. Journal of the American Academy of Child & Adolescent Psychiatry, 40(4), 409–418. https://doi.org/10.1097/00004583-200104000-00009
Ghandour, R. M., Sherman, L. J., Vladutiu, C. J., Ali, M. M., Lynch, S. E., Bitsko, R. H., & Blumberg, S. J. (2019). Prevalence and treatment of depression, anxiety, and conduct problems in US children. The Journal of Pediatrics, 206, 256–267. https://doi.org/10.1016/j.jpeds.2018.09.021
Higa-McMillan, C. K., Francis, S. E., Rith-Najarian, L., & Chorpita, B. F. (2016). Evidence base update: 50 years of research on treatment for child and adolescent anxiety. Journal of Clinical Child & Adolescent Psychology, 45(2), 91–113. https://doi.org/10.1080/15374416.2015.1046177
Hunsley, J. (2007). Addressing key challenges in evidence-based practice in psychology. Professional Psychology: Research and Practice, 38(2), 113–121. https://doi.org/10.1037/0735-7028.38.2.113
Kaminski, J. W., & Claussen, A. H. (2017). Evidence base update for psychosocial treatments for disruptive behaviors in children. Journal of Clinical Child & Adolescent Psychology, 46(4), 477–499. https://doi.org/10.1080/15374416.2017.1310044
Kendall, P. C., & Hedtke, K. A. (2006). Cognitive-behavioral therapy for anxious children: Therapist manual (3rd ed.). Workbook Publishing.
Lang, J. M., Franks, R. P., Epstein, C., Stover, C., & Oliver, J. A. (2015). Statewide dissemination of an evidence-based practice using Breakthrough Series Collaboratives. Children and Youth Services Review, 55, 201–209. https://doi.org/10.1016/j.childyouth.2015.06.005
Lang, J. M., Lee, P., Connell, C. M., Marshall, T., & Vanderploeg, J. J. (2021). Outcomes, evidence-based treatments, and disparities in a statewide outpatient children’s behavioral health system. Children and Youth Services Review, 120, Article 105729. https://doi.org/10.1016/j.childyouth.2020.105729
Lang, J. M., Randall, K., Delaney, M., & Vanderploeg, J. J. (2017). A Model for Sustaining Evidence-Based Practices in a Statewide System. Families in Society, 98(1), 18–26. https://doi.org/10.1606/1044-3894.2017.5
McCart, M. R., & Sheidow, A. J. (2016). Evidence-based psychosocial treatments for adolescents with disruptive behavior. Journal of Clinical Child & Adolescent Psychology, 45(5), 529–563. https://doi.org/10.1080/15374416.2016.1146990
Milette-Winfree, M., & Mueller, C. W. (2018). Treatment-as-usual therapy targets for comorbid youth disproportionately focus on externalizing problems. Psychological Services, 15(1), 65–77. https://doi.org/10.1037/ser0000162
Miller, M., & Hinshaw, S. P. (2012). Attention-deficit/hyperactivity disorder. In P. C. Kendall (Ed.), Child and adolescent therapy: Cognitive-behavioral procedures (pp. 61–91). The Guilford Press.
Mueller, C. W., Tolman, R., Higa-McMillan, C. K., & Daleiden, E. L. (2010). Longitudinal predictors of youth functional improvement in a public mental health system. The Journal of Behavioral Health Services & Research, 37(3), 350–362. https://doi.org/10.1007/s11414-009-9172-4
Ogles, B. M., Melendez, G., Davis, D. C., & Lunnen, K. M. (1999). The Ohio Youth Problems, Functioning, and Satisfaction Scales (Short Form): User's Manual. Columbus, OH: Ohio Department of Mental Health, Office of Program Evaluation and Research.
Ogles, B. M., Melendez, G., Davis, D. C., & Lunnen, K. M. (2000). The Ohio Youth Problem, Functioning, and Satisfaciton Scales: Technical Manual. Columbus, OH: Ohio Department of Mental Health.
Park, A. L., Moskowitz, A. L., & Chorpita, B. F. (2018). Community-based providers’ selection of practices for children and adolescents with comorbid mental health problems. Journal of Clinical Child & Adolescent Psychology, 47(5), 796–807. https://doi.org/10.1080/15374416.2016.1188706
Prinstein, M. J., Youngstrom, E. A., Mash, E. J., & Barkley, R. A. (Eds.). (2019). Treatment of disorders in childhood and adolescence. The Guilford Press.
Southam-Gerow, M. A., & Prinstein, M. J. (2014). Evidence base updates: The evolution of the evaluation of psychological treatments for children and adolescents. Journal of Clinical Child & Adolescent Psychology, 43(1), 1–6. https://doi.org/10.1080/15374416.2013.855128
Stewart, R. E., Stirman, S. W., & Chambless, D. L. (2012). A qualitative investigation of practicing psychologists’ attitudes toward research-informed practice: Implications for dissemination strategies. Professional Psychology: Research and Practice, 43(2), 100–109. https://doi.org/10.1037/a0025694
Tam, K. K. (2006). Reliable change and clinical significance for outcomes instruments. Columbus, OH: Ohio Department of Mental Health, Office of Program Evaluation and Research. http://mha.ohio.gov/Portals/0/assets/Planning/OutcomesResearch/reports/quarterly-12.pdf
Tam, K. K., & Healy, J. (2006). Benchmarks for reliable change and clinical significance on the Ohio Scales for Youth - Problem and Functioning Scales. Columbus, OH: Ohio Department of Mental Health, Office of Program Evaluation and Research. http://mha.ohio.gov/Portals/0/assets/Planning/OutcomesResearch/reports/quarterly-16.pdf
Vidal, S., & Connell, C. M. (2019). Treatment Effects of Parent-Child Focused Evidence-Based Programs on Problem Severity and Functioning among Children and Adolescents with Disruptive Behavior. Journal of Clinical Child & Adolescent Psychology, 48(sup1), S326–S336. https://doi.org/10.1080/15374416.2018.1469092
Warren, J. S., Nelson, P. L., Mondragon, S. A., Baldwin, S. A., & Burlingame, G. M. (2010). Youth psychotherapy change trajectories and outcomes in usual care: Community mental health versus managed care settings. Journal of Consulting and Clinical Psychology, 78(2), 144–155. https://doi.org/10.1037/a0018544
Weersing, V. R., Jeffreys, M., Do, M. C. T., Schwartz, K. T., & Bolano, C. (2017). Evidence base update of psychosocial treatments for child and adolescent depression. Journal of Clinical Child & Adolescent Psychology, 46(1), 11–43. https://doi.org/10.1080/15374416.2016.1220310
Weisz, J. R., Chorpita, B. F., Palinkas, L. A., Schoenwald, S. K., Miranda, J., Bearman, S. K., Daleiden, E. L., Ugueto, A. M., Ho, A., Martin, J., Gray, J., Alleyne, A., Langer, D. A., Southam-Gerow, M. A., Gibbons, R. D., & the Research Network on Youth Mental Health. (2012). Testing standard and modular designs for psychotherapy treating depression, anxiety, and conduct problems in youth: A randomized effectiveness trial. Archives of General Psychiatry, 69(3), 274–282. https://doi.org/10.1001/archgenpsychiatry.2011.147
Weisz, J. R., Doss, A. J., & Hawley, K. M. (2005). Youth psychotherapy outcome research: A review and critique of the evidence base. Annual Review of Psychology, 56, 337–363. https://doi.org/10.1146/annurev.psych.55.090902.141449
Weisz, J. R., Kuppens, S., Eckshtain, D., Ugueto, A. M., Hawley, K. M., & Jensen-Doss, A. (2013a). Performance of evidence-based youth psychotherapies compared with usual clinical care: A multilevel meta-analysis. JAMA Psychiatry, 70(7), 750–761. https://doi.org/10.1001/jamapsychiatry.2013.1176
Weisz, J. R., Kuppens, S., Ng, M. Y., Eckshtain, D., Ugueto, A. M., Vaughn-Coaxum, R., Jensen-Doss, A., Hawley, K. M., Krumholz Marchette, L. S., Chu, B. C., Weersing, V. R., & Fordwood, S. R. (2017). What five decades of research tells us about the effects of youth psychological therapy: A multilevel meta-analysis and implications for science and practice. American Psychologist, 72(2), 79–117. https://doi.org/10.1037/a0040360
Weisz, J. R., Southam-Gerow, M. A., Gordis, E. B., Connor-Smith, J. K., Chu, B. C., Langer, D. A., McLeod, B. D., Jensen-Doss, A., Updegraff, A., & Weiss, B. (2009). Cognitive–behavioral therapy versus usual clinical care for youth depression: An initial test of transportability to community clinics and clinicians. Journal of Consulting and Clinical Psychology, 77(3), 383–396. https://doi.org/10.1037/a0013877
Weisz, J. R., Ugueto, A. M., Cheron, D. M., & Herren, J. (2013b). Evidence-based youth psychotherapy in the mental health ecosystem. Journal of Clinical Child & Adolescent Psychology, 42(2), 274–286. https://doi.org/10.1080/15374416.2013.764824
Acknowledgements
The authors would like to acknowledge and thank Yvette Cortez, Jack Lu, Kellie Randall, Bethany Zorba, and all of the Connecticut outpatient providers.
Funding
This was an unfunded study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
This study used de-identified archived administrative data that was determined not to qualify as human subjects research by the Eastern Connecticut State University IRB.
Informed Consent
Consent/assent for treatment was originally obtained by each provider as part of their routine intake and treatment process.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lee, P., Lang, J.M., Vanderploeg, J.J. et al. Evidence-Based Treatments in Community Mental Health Settings: Use and Congruence With Children’s Primary Diagnosis and Comorbidity. Res Child Adolesc Psychopathol 50, 417–430 (2022). https://doi.org/10.1007/s10802-021-00877-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10802-021-00877-y