Abstract
Purpose
Our study aimed to make a bibliometric analysis on Sjögren's syndrome-related dry eye disease (SS-DED), explore its potential research hotspots, and provide critical information for future research interest and undeveloped topics in this field, which can benefit clinicians and researchers.
Methods
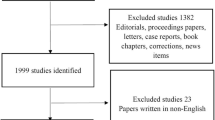
We extracted all publications relating to SS-DED from 2003 to 2022 from the Web of Science Core Collection database. Original articles and reviews in English were included. The contributions of different countries, institutions, journals, and authors were compared, and the research hotspots were visualized for network analysis through GraphPad Prism, CiteSpace, and VOSviewer.
Results
We enrolled a total of 987 publications. The United States contributed the most publications (281, 28.5%), followed by China (157, 15.9%) and Japan (80, 8.11%). Publications from the United States were cited more frequently (13,060 citations), with the highest H-index of 57. China ranked second in the total number of publications, the papers were not cited frequently (3790 citations), and the H-index ranked second (H-index = 31). PLoS One (32, 3.24%) published the most papers, and the University of California system had the highest number of publications (45, 4.56%). Bootsma H from the Netherlands published the most papers. The trend of research hotspots evolved mainly from the basic manifestation to pathogenesis and treatment of SS-DED and paid more attention to distinguishing SS-DED from that dry eye disease without SS.
Conclusions
Based on the bibliometric, co-citation, and network analyses in this study, we obtained the annual publications and citations, the growth trends of publications, the productivity of countries, organizations, journals, and authors, high-quality publications, and the emerging hotspots of SS-DED, which may open new doors for promising research directions.






Similar content being viewed by others
References
Helmick CG, Felson DT, Lawrence RC, Gabriel S, Hirsch R, Kwoh CK, Liang MH, Kremers HM, Mayes MD, Merkel PA, Pillemer SR, Reveille JD, Stone JH (2008) Estimates of the prevalence of arthritis and other rheumatic conditions in the United States Part I. Arthritis Rheum 58(1):15–25. https://doi.org/10.1002/art.23177
Vehof J, Utheim TP, Bootsma H, Hammond CJ (2020) Advances, limitations and future perspectives in the diagnosis and management of dry eye in Sjögren’s syndrome. Clin Exp Rheumatol 38(4):301–309
Li R, Sun X, Liu X, Yang Y, Li Z (2019) Autoimmune diseases in China. Adv Immunol 144:173–216. https://doi.org/10.1016/bs.ai.2019.09.002
Pflugfelder SC, Huang AJ, Feuer W, Chuchovski PT, Pereira IC, Tseng SC (1990) Conjunctival cytologic features of primary Sjögren’s syndrome. Ophthalmology 97(8):985–991. https://doi.org/10.1016/s0161-6420(90)32478-8
Caban M, Omulecki W, Latecka-Krajewska B (2022) Dry eye in Sjögren’s syndrome - characteristics and therapy. Eur J Ophthalmol 32(6):3174–3184. https://doi.org/10.1177/11206721221091375
Ou JI, Manche EE (2007) Corneal perforation after conductive keratoplasty in a patient with previously undiagnosed Sjögren syndrome. Arch Ophthalmol 125(8):1131–1132. https://doi.org/10.1001/archopht.125.8.1131
Murtagh P, Comer R, Fahy G (2018) Corneal perforation in undiagnosed Sjögren’s syndrome following topical NSAID and steroid drops post routine cataract extraction. BMJ case reports 2018:bcr--2018. https://doi.org/10.1136/bcr-2018-225428
Akpek EK, Mathews P, Hahn S, Hessen M, Kim J, Grader-Beck T, Birnbaum J, Baer AN (2015) Ocular and systemic morbidity in a longitudinal cohort of Sjögren’s syndrome. Ophthalmology 122(1):56–61. https://doi.org/10.1016/j.ophtha.2014.07.026
Shan SJ, Wu EI, Akpek EK (2009) Sterile corneal melt after descemet stripping endothelial keratoplasty in patients with previously undiagnosed Sjogren syndrome. Arch Ophthalmol 127(2):219–220. https://doi.org/10.1001/archophthalmol.2008.601
Erickson S, Sullivan AG, Barabino S, Begovic E, Benitez-Del-Castillo JM, Bonini S, Borges JS, Brzheskiy V, Bulat N, Cerim A, Craig JP, Cușnir V, Cușnir V Jr, Cușnir V, Doan S, Dülger E, Farrant S, Geerling G, Goldblum D, Golubev S, Gomes JAP, González-Méijome JM, Grupcheva CN, Gündüz ÖU, Horwath-Winter J, Källmark F, Karanadze N, Karcic HH, Karcic S, Kontadakis G, Messmer EM, Mrugacz M, Murphy C, O’Leary OE, Procopciuc V, Pult H, Raus P, Şahin A, Setälä N, Stanila A, Stanila DM, Utheim TP, Vehof J, Versura P, Villani E, Willcox MDP, Wolffsohn JS, Zagórski Z, Zoega GM, Sullivan DA (2020) TFOS European Ambassador meeting: unmet needs and future scientific and clinical solutions for ocular surface diseases. Ocul Surf 18(4):936–962. https://doi.org/10.1016/j.jtos.2020.05.006
Akpek EK, Klimava A, Thorne JE, Martin D, Lekhanont K, Ostrovsky A (2009) Evaluation of patients with dry eye for presence of underlying Sjögren syndrome. Cornea 28(5):493–497. https://doi.org/10.1097/ICO.0b013e31818d3846
Akpek EK, Bunya VY, Saldanha IJ (2019) Sjögren’s syndrome: more than just dry eye. Cornea 38(5):658–661. https://doi.org/10.1097/ico.0000000000001865
Stefanski AL, Tomiak C, Pleyer U, Dietrich T, Burmester GR, Dörner T (2017) The diagnosis and treatment of Sjögren’s syndrome. Deutsches Arzteblatt Int 114(20):354–361. https://doi.org/10.3238/arztebl.2017.0354
Kassan SS, Moutsopoulos HM (2004) Clinical manifestations and early diagnosis of Sjögren syndrome. Arch Intern Med 164(12):1275–1284. https://doi.org/10.1001/archinte.164.12.1275
Bjordal O, Norheim KB, Rødahl E, Jonsson R, Omdal R (2020) Primary Sjögren’s syndrome and the eye. Surv Ophthalmol 65(2):119–132. https://doi.org/10.1016/j.survophthal.2019.10.004
Aragona P, Stilo A, Ferreri F, Mobrici M (2005) Effects of the topical treatment with NSAIDs on corneal sensitivity and ocular surface of Sjögren’s syndrome patients. Eye (Lond) 19(5):535–539. https://doi.org/10.1038/sj.eye.6701537
Avunduk AM, Avunduk MC, Varnell ED, Kaufman HE (2003) The comparison of efficacies of topical corticosteroids and nonsteroidal anti-inflammatory drops on dry eye patients: a clinical and immunocytochemical study. Am J Ophthalmol 136(4):593–602. https://doi.org/10.1016/s0002-9394(03)00326-x
Lin T, Gong L (2015) Topical fluorometholone treatment for ocular dryness in patients with Sjögren syndrome: a randomized clinical trial in China. Medicine (Baltimore) 94(7):e551. https://doi.org/10.1097/md.0000000000000551
Devecı H, Kobak S (2014) The efficacy of topical 0.05 % cyclosporine A in patients with dry eye disease associated with Sjögren’s syndrome. Int ophthalmol 34(5):1043–1048. https://doi.org/10.1007/s10792-014-9901-4
Moscovici BK, Holzchuh R, Sakassegawa-Naves FE, Hoshino-Ruiz DR, Albers MB, Santo RM, Hida RY (2015) Treatment of Sjögren’s syndrome dry eye using 0.03% tacrolimus eye drop: prospective double-blind randomized study. Contact Lens Anterior Eye J Br Contact Lens Assoc 38(5):373–378. https://doi.org/10.1016/j.clae.2015.04.004
Aragona P, Bucolo C, Spinella R, Giuffrida S, Ferreri G (2005) Systemic omega-6 essential fatty acid treatment and pge1 tear content in Sjögren’s syndrome patients. Invest Ophthalmol Vis Sci 46(12):4474–4479. https://doi.org/10.1167/iovs.04-1394
Gottenberg JE, Ravaud P, Puéchal X, Le Guern V, Sibilia J, Goeb V, Larroche C, Dubost JJ, Rist S, Saraux A, Devauchelle-Pensec V, Morel J, Hayem G, Hatron P, Perdriger A, Sene D, Zarnitsky C, Batouche D, Furlan V, Benessiano J, Perrodeau E, Seror R, Mariette X (2014) Effects of hydroxychloroquine on symptomatic improvement in primary Sjögren syndrome: the JOQUER randomized clinical trial. JAMA 312(3):249–258. https://doi.org/10.1001/jama.2014.7682
Ibrahim OM, Dogru M, Kawashima S, Wakamatsu TH, Tsubota K, Fujishima H (2013) Visante optical coherence tomography and tear function test evaluation of cholinergic treatment response in patients with Sjögren syndrome. Cornea 32(5):653–657. https://doi.org/10.1097/ICO.0b013e318261eb4a
Willeke P, Schlüter B, Becker H, Schotte H, Domschke W, Gaubitz M (2007) Mycophenolate sodium treatment in patients with primary Sjögren syndrome: a pilot trial. Arthritis Res Ther 9(6):R115. https://doi.org/10.1186/ar2322
Yavuz S, Asfuroğlu E, Bicakcigil M, Toker E (2011) Hydroxychloroquine improves dry eye symptoms of patients with primary Sjogren’s syndrome. Rheumatol Int 31(8):1045–1049. https://doi.org/10.1007/s00296-010-1415-4
Avila MY (2014) Restoration of human lacrimal function following platelet-rich plasma injection. Cornea 33(1):18–21. https://doi.org/10.1097/ico.0000000000000016
Güerrissi JO, Belmonte J (2004) Surgical treatment of dry eye syndrome: conjunctival graft of the minor salivary gland. J Craniofac Surg 15(1):6–10. https://doi.org/10.1097/00001665-200401000-00004
Qiu W, Liu Z, Ao M, Li X, Wang W (2013) Punctal plugs versus artificial tears for treating primary Sjögren’s syndrome with keratoconjunctivitis SICCA: a comparative observation of their effects on visual function. Rheumatol Int 33(10):2543–2548. https://doi.org/10.1007/s00296-013-2769-1
La Porta WS, Becco de Souza R, Gomes JÁP, Hofling-Lima AL (2016) The use of the Esclera Scleral contact lens in the treatment of moderate to severe dry eye disease. Am J Ophthalmol 163:167-173.e161. https://doi.org/10.1016/j.ajo.2015.11.034
Tauqeer Z, Bunya VY, Macchi I, Massaro-Giordano M (2021) Ocular pathophysiology of Sjögren’s syndrome. Ocul Immunol Inflamm 29(4):796–802. https://doi.org/10.1080/09273948.2021.1903935
Bron AJ, de Paiva CS, Chauhan SK, Bonini S, Gabison EE, Jain S, Knop E, Markoulli M, Ogawa Y, Perez V, Uchino Y, Yokoi N, Zoukhri D, Sullivan DA (2017) TFOS DEWS II pathophysiology report. Ocul Surf 15(3):438–510. https://doi.org/10.1016/j.jtos.2017.05.011
Ogawa Y, Takeuchi T, Tsubota K (2021) Autoimmune epithelitis and chronic inflammation in Sjögren’s syndrome-related dry eye disease. Int J Mol Sci 22(21):11820. https://doi.org/10.3390/ijms222111820
Reyes JL, Vannan DT, Eksteen B, Avelar IJ, Rodríguez T, González MI, Mendoza AV (2018) Innate and adaptive cell populations driving inflammation in dry eye disease. Mediators Inflamm 2018:2532314. https://doi.org/10.1155/2018/2532314
Ushio A, Arakaki R, Eguchi H, Hotta F, Yamada A, Kudo Y, Ishimaru N (2017) Pathological analysis of ocular lesions in a murine model of Sjögren’s syndrome. Int J Mol Sci 18(6):1209. https://doi.org/10.3390/ijms18061209
Tao Z, Zhou S, Yao R, Wen K, Da W, Meng Y, Yang K, Liu H, Tao L (2020) COVID-19 will stimulate a new coronavirus research breakthrough: a 20-year bibliometric analysis. Ann Transl Med 8(8):528. https://doi.org/10.21037/atm.2020.04.26
Chen W, Geng Y, Zhong S, Zhuang M, Pan H (2020) A bibliometric analysis of ecosystem services evaluation from 1997 to 2016. Environ Sci Pollut Res Int 27(19):23503–23513. https://doi.org/10.1007/s11356-020-08760-x
Gu X, Xie M, Jia R, Ge S (2021) Publication trends of research on retinoblastoma during 2001–2021: a 20-year bibliometric analysis. Front Med 8:675703. https://doi.org/10.3389/fmed.2021.675703
Chen J, He Q, Jiang B, Song W, Wu Z, Yang J, Huang Z, Yu X, Luo J, Tao Q (2022) Research on primary Sjögren’s syndrome in 2004–2021: a Web of Science-based cross-sectional bibliometric analysis. Rheumatol Int. https://doi.org/10.1007/s00296-022-05138-9
Akyol A, Kocyigit BF (2021) Publication activity in the field of Sjögren’s syndrome: a ten-year Web of Science based analysis. Rheumatol Int 41(4):763–769. https://doi.org/10.1007/s00296-020-04714-1
Hirsch JE (2005) An index to quantify an individual’s scientific research output. Proc Natl Acad Sci USA 102(46):16569–16572. https://doi.org/10.1073/pnas.0507655102
Whitcher JP, Shiboski CH, Shiboski SC, Heidenreich AM, Kitagawa K, Zhang S, Hamann S, Larkin G, McNamara NA, Greenspan JS, Daniels TE, Sjögren's International Collaborative Clinical Alliance Research Groups (2010) A simplified quantitative method for assessing keratoconjunctivitis sicca from the Sjögren's Syndrome International Registry. Am J Ophthalmol 149(3):405–415. https://doi.org/10.1016/j.ajo.2009.09.013
Ogawa Y (2018) Sjögren’s syndrome, non-Sjögren’s syndrome, and graft-versus-host disease related dry eye. Invest Ophthalmol Vis Sci 59(14):Des71-des79. https://doi.org/10.1167/iovs.17-23750
Vriezekolk JE, Geenen R, Hartkamp A, Godaert GL, Bootsma H, Kruize AA, Bijlsma JW, Derksen RH (2005) Psychological and somatic predictors of perceived and measured ocular dryness of patients with primary Sjögren’s syndrome. J Rheumatol 32(12):2351–2355
van Leeuwen N, Bossema ER, Vermeer RR, Kruize AA, Bootsma H, Vingerhoets AJ, Bijlsma JW, Geenen R (2016) Crying without tears: dimensions of crying and relations with ocular dryness and mental well-being in patients with Sjögren’s syndrome. J Clin Psychol Med Settings 23(1):77–87. https://doi.org/10.1007/s10880-015-9432-9
de Monchy I, Gendron G, Miceli C, Pogorzalek N, Mariette X, Labetoulle M (2011) Combination of the Schirmer I and phenol red thread tests as a rescue strategy for diagnosis of ocular dryness associated with Sjögren’s syndrome. Invest Ophthalmol Vis Sci 52(8):5167–5173. https://doi.org/10.1167/iovs.10-6671
Wakamatsu TH, Sato EA, Matsumoto Y, Ibrahim OM, Dogru M, Kaido M, Ishida R, Tsubota K (2010) Conjunctival in vivo confocal scanning laser microscopy in patients with Sjögren syndrome. Invest Ophthalmol Vis Sci 51(1):144–150. https://doi.org/10.1167/iovs.08-2722
Ogawa Y, Shimizu E, Tsubota K (2018) Interferons and dry eye in Sjögren’s syndrome. Int J Mol Sci 19(11):3548. https://doi.org/10.3390/ijms19113548
Fox RI (2005) Sjögren’s syndrome. Lancet 366(9482):321–331. https://doi.org/10.1016/s0140-6736(05)66990-5
Shiboski CH, Shiboski SC, Seror R, Criswell LA, Labetoulle M, Lietman TM, Rasmussen A, Scofield H, Vitali C, Bowman SJ, Mariette X, International Sjögren's Syndrome Criteria Working Group (2017) 2016 American College of Rheumatology/European League Against Rheumatism Classification Criteria for Primary Sjögren's Syndrome: A Consensus and Data-Driven Methodology Involving Three International Patient Cohorts. Arthritis Rheumatol 69(1):35–45. https://doi.org/10.1002/art.39859
Akpek EK, Mathews P, Hahn S, Hessen M, Kim J, Grader-Beck T, Birnbaum J, Baer AN (2015) Ocular and systemic morbidity in a longitudinal cohort of Sjögren's syndrome. Ophthalmology 122(1):56–61. https://doi.org/10.1016/j.ophtha.2014.07.026
Karakus S, Baer AN, Akpek EK (2019) Clinical correlations of novel autoantibodies in patients with dry eye. J Immunol Res 2019:7935451. https://doi.org/10.1155/2019/7935451
Bunya VY, Bhosai SJ, Heidenreich AM, Kitagawa K, Larkin GB, Lietman TM, Gaynor BD, Akpek EK, Massaro-Giordano M, Srinivasan M, Porco TC, Whitcher JP, Shiboski SC, Criswell LA, Shiboski CH (2016) Association of dry eye tests with extraocular signs among 3514 participants in the Sjögren’s syndrome international registry. Am J Ophthalmol 172:87–93. https://doi.org/10.1016/j.ajo.2016.09.013
Garcia DM, Reis de Oliveira F, Módulo CM, Faustino J, Barbosa AP, Alves M, Rocha EM (2018) Is Sjögren’s syndrome dry eye similar to dry eye caused by other etiologies? Discriminating different diseases by dry eye tests. PLoS ONE 13(12):e0208420. https://doi.org/10.1371/journal.pone.0208420
Tauqeer Z, Bunya VY, Macchi I, Massaro-Giordano M (2021) Ocular pathophysiology of sjögren's syndrome. Ocul Immunol Inflamm 19;29(4):796–802. https://doi.org/10.1080/09273948.2021.1903935
Mircheff AK (2003) Sjogrens syndrome as failed local immunohomeostasis: prospects for cell-based therapy. Ocul Surf Oct 1(4):160–179. https://doi.org/10.1016/s1542-0124(12)70012-5
Lavie F, Miceli-Richard C, Ittah M, Sellam J, Gottenberg JE, Mariette X (2007) Increase of B cell-activating factor of the TNF family (BAFF) after rituximab treatment: insights into a new regulating system of BAFF production. Ann Rheum Dis 66(5):700–703. https://doi.org/10.1136/ard.2006.060772
Mackay F, Schneider P, Rennert P, Browning J (2003) BAFF AND APRIL: a tutorial on B cell survival. Annu Rev Immunol 21:231–264. https://doi.org/10.1146/annurev.immunol.21.120601.141152
Lee OL, Tepelus TC, Huang J, Irvine AG, Irvine C, Chiu GB, Sadda SR (2018) Evaluation of the corneal epithelium in non-Sjögren's and Sjögren's dry eyes: an in vivo confocal microscopy study using HRT III RCM. BMC Ophthalmol 18(1):309. https://doi.org/10.1186/s12886-018-0971-3
Baudouin C, Aragona P, Messmer EM, Tomlinson A, Calonge M, Boboridis KG, Akova YA, Geerling G, Labetoulle M, Rolando M (2013) Role of hyperosmolarity in the pathogenesis and management of dry eye disease: proceedings of the OCEAN group meeting. Ocul Surf 11(4):246–258. https://doi.org/10.1016/j.jtos.2013.07.003
Acknowledgments
This work was supported by grants from the National Natural Science Foundation of China (82201145).
Funding
This work was supported by grants from the National Natural Science Foundation of China (82201145).
Author information
Authors and Affiliations
Contributions
YJ gave the conception and designed the study. Material preparation, data collection, and analysis were performed by QRW, MYX, and SYL. The first draft of the manuscript was written by QRW and all authors commented on previous versions of the manuscript. SL, LT, and YJ reviewed the manuscript and gave final approval of the version to be submitted. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This is an observational study. The Ethics and Welfare Review of Laboratory Animals in Beijing Tongren Hospital Affiliated to Capital Medical University has confirmed that no ethical approval is required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, Q., Xie, M., Li, S. et al. Mapping the research on Sjögren's syndrome-related dry eye disease: a bibliometric network analysis of the past 20 years. Int Ophthalmol 43, 3115–3130 (2023). https://doi.org/10.1007/s10792-023-02711-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-023-02711-4