Abstract
Purpose
Description of a novel modified technique known as haptic-twist method for placing a trailing haptic into a 27 G needle during double-needle intrascleral haptic fixation (Yamane technique) in the absence and/or inadequacy of capsular support.
Methods
The trailing haptic was threaded into the needle lumen using a haptic-twist method in 12 eyes of 11 patients with aphakia. The haptic was grasped by a forceps 2–3 mm from the tip, while the forceps was rotated by 180° counter-clockwise around its own axis. This maneuver enabled the trailing haptic to be slightly twisted without any deformation and to coordinate with the needle in the proper angle. The surgical technique has also been mentioned in a surgical video.
Results
Mean age of the patients was 62 years ± 18 (range 46–78 years). Although the mean pre-operative best-corrected visual acuity was 0.70 ± 0.35 logarithm of the minimum angle of resolution (logMAR) (range 1.30–0.20 logMAR), an improvement of up to 0.40 ± 0.32 logMAR (range 1.0–0.1 logMAR) was observed 3 months after surgery. No trailing haptic bending or breakage was observed during the process. Furthermore, no optical tilting or decentralization was observed post-operatively.
Conclusions
Although threading the leading haptic into the needle is reasonably straightforward, the trailing haptic positioning can be difficult due to an inappropriate gesture of both the haptic and the needle. We fervently believe that this novel haptic-twist method can provide a much simpler and easier approach, and thus contribute to better surgical outcomes.





Similar content being viewed by others
References
Gimbel HV, Sun R, Ferensowicz M, Anderson Penno E, Kamal A (2001) Intraoperative management of posterior capsule tears in phacoemulsification and intraocular lens implantation. Ophthalmology 108:2186–2189. https://doi.org/10.1016/s0161-6420(01)00716-3
Por YM, Lavin MJ (2005) Techniques of intraocular lens suspension in the absence of capsular/zonular support. Surv Ophthalmol 50:429–462. https://doi.org/10.1016/j.survophthal.2005.06.010
Chang DF (2004) Siepser slipknot for McCannel iris-suture fixation of subluxated intraocular lenses. J Cataract Refract Surg 30:1170–1176. https://doi.org/10.1016/j.jcrs.2003.10.025
Teichmann KD (1994) Pars plana fixation of posterior chamber intraocular lenses. Ophthalmic Surg 25:549–553
Apple DJ, Price FW, Gwin T, Imkamp E, Daun M, Casanova R, Hansen S, Carlson AN (1989) Sutured retropupillary posterior chamber intraocular lenses for exchange or secondary implantation. The 12th annual Binkhorst lecture, 1988. Ophthalmology 96:1241–1247. https://doi.org/10.1016/s0161-6420(89)32745-x
Wagoner MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL, American Academy of Ophthalmology (2003) Intraocular lens implantation in the absence of capsular support: a report by the American Academy of Ophthalmology. Ophthalmology 110:840–859. https://doi.org/10.1016/s0161-6420(02)02000-6
Gabor SG, Pavlidis MM (2007) Sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 33:1851–18544. https://doi.org/10.1016/j.jcrs.2007.07.013
Agarwal A, Kumar DA, Jacob S, Baid C, Agarwal A, Srinivasan S (2008) Fibrin glue-assisted sutureless posterior chamber intraocular lens implantation in eyes with deficient posterior capsules. J Cataract Refract Surg 34:1433–1438. https://doi.org/10.1016/j.jcrs.2008.04.040
Yamane S, Sato S, Maruyama-Inoue M, Kadonosono K (2017) Flanged intrascleral intraocular lens fixation with double-needle technique. Ophthalmology 124:1136–1142. https://doi.org/10.1016/j.ophtha.2017.03.036
Haszcz D, Nowomiejska K, Oleszczuk A, Forlini C, Forlini M, Moneta-Wielgos J, Maciejewski R, Michalska-Malecka K, Jünemann AG, Rejdak R (2016) Visual outcomes of posterior chamber intraocular lens intrascleral fixation in the setting of postoperative and posttraumatic aphakia. BMC Ophthalmol 16:50. https://doi.org/10.1186/s12886-016-0228-y
Chantarasorn Y, Techalertsuwan S, Siripanthong P, Tamerug A (2018) Reinforced scleral fixation of foldable intraocular lens by double sutures: comparison with intrascleral intraocular lens fixation. Jpn J Ophthalmol 62:365–372. https://doi.org/10.1007/s10384-018-0579-4
Sindal MD, Nakhwa CP, Sengupta S (2016) Comparison of sutured versus sutureless scleral-fixated intraocular lenses. J Cataract Refract Surg 42:27–34. https://doi.org/10.1016/j.jcrs.2015.09.019
Narang P, Narang S (2013) Glue-assisted intrascleral fixation of posterior chamber intraocular lens. Indian J Ophthalmol 61:163–167. https://doi.org/10.4103/0301-4738.112160
Kumar DA, Agarwal A, Packiyalakshmi S, Jacob S, Agarwal A (2013) Complications and visual outcomes after glued foldable intraocular lens implantation in eyes with inadequate capsules. J Cataract Refract Surg 39:1211–1218. https://doi.org/10.1016/j.jcrs.2013.03.004
Kumar DA, Agarwal A, Prakash G, Jacob S, Saravanan Y, Agarwal A (2010) Glued posterior chamber IOL in eyes with deficient capsular support: a retrospective analysis of 1-year post-operative outcomes. Eye (London) 24:1143–1148. https://doi.org/10.1038/eye.2010.10
Yang Y, Yao TT, Zhou YL, Wang YX, Wang ZY (2019) A modified intrascleral intraocular lens fixation technique with fewer anterior segment manipulations: 27 G needle-guided procedure with built-in 8–0 absorbable sutures. BMC Ophthalmol 19:234. https://doi.org/10.1186/s12886-019-1239-2
Narang P, Agarwal A (2017) Glued intrascleral haptic fixation of an intraocular lens. Indian J Ophthalmol 65:1370–1380. https://doi.org/10.4103/ijo.IJO_643_17
Narang P, Agarwal A (2019) Handshake riveting flanged technique for Yamane method of intrascleral fixation of an intraocular lens. J Cataract Refract Surg 45:1838–1839. https://doi.org/10.1016/j.jcrs.2019.09.014
Kim DB (2018) Trailing-haptic-first modification of double-needle intrascleral haptic fixation technique. J Cataract Refract Surg 44:424–428. https://doi.org/10.1016/j.jcrs.2018.01.027
Baskaran P, Ganne P, Bhandari S, Ramakrishnan S, Venkatesh R, Gireesh P (2017) Extraocular needle- guided haptic insertion technique of scleral fixation intraocular lens surgeries (X-NIT). Indian J Ophthalmol 65:747–750. https://doi.org/10.4103/ijo.IJO_296_17
Taskin I, Altinbay D, Ozdemir VN (2020) A different surgical approach to cases with zonular weakness or dialysis: sutureless transscleral fixated intraocular lens implantation and stabilization of lens capsule. Int Ophthalmol 40:2315–2323. https://doi.org/10.1007/s10792-020-01416-2
Hoffman RS, Fine IH, Packer M (2006) Scleral fixation without conjunctival dissection. J Cataract Refract Surg 32:1907–1912. https://doi.org/10.1016/j.jcrs.2006.05.029
Crnej A, Hirnschall N, Nishi Y, Gangwani V, Tabernero J, Artal P, Findl O (2011) Impact of intraocular lens haptic design and orientation on decentration and tilt. J Cataract Refract Surg 37:1768–1774. https://doi.org/10.1016/j.jcrs.2011.04.028
Cabeza-Gil I, Ariza-Gracia MÁ, Remón L, Calvo B (2020) Systematic study on the biomechanical stability of C-loop intraocular lenses: approach to an optimal design of the haptics. Ann Biomed Eng 48:1127–1136. https://doi.org/10.1007/s10439-019-02432-9
Funding
Authors declare no public or private financial support or involvement whatsoever in the products, methods or materials referred to in this manuscript.
Author information
Authors and Affiliations
Contributions
TE and HHG were responsible for study design and recruitment of participants; surgery and follow-up of patients; data analysis, reviewing, editing and verifying the accuracy of the manuscript. Complete access to all study data and accountability for data integrity and accuracy of data analysis were performed by TE. Not: TE = Tansu Erakgun; HHG = Hamidu Hamisi Gobeka.
Corresponding author
Ethics declarations
Conflict of interest
The authors claim no conflict of interest. Both authors certify that they have no association or participation with any organization or individual with any financial interest or non-financial interest in the subject matter or materials discussed in this article.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors note that human study participants have given informed consent to the release of the images.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
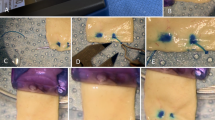
An angled sclerotomy on the left side was made with a 27 G bevel-up needle, 2 mm from the limbus, to engage the leading haptic. The intraocular forceps was used to thread the leading haptic into the needle lumen. After securing the haptic, the needle was removed to externalize the haptic. The second sclerotomy was made with 27 G bevel-up needle 180° away in similar fashion to the first one. The intraocular forceps was inserted through the paracentesis to thread the trailing haptic into the needle lumen. The haptic was slightly twisted around its own axis without deformation and aligned with theneedle lumen in the proper angle. The trailing haptic was then externalized and the tip was heated with a low-temperature cautery to create a flange which was pushed back and fixed intrasclerally. (MP4 177088 kb)
Rights and permissions
About this article
Cite this article
Erakgun, T., Gobeka, H.H. The novel haptic-twist method for a sutureless double-needle intrascleral haptic fixation technique. Int Ophthalmol 41, 3013–3020 (2021). https://doi.org/10.1007/s10792-021-01862-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-01862-6