Abstract
Purpose
To systematic analysis of domestic and foreign literature on the incidence and related factors of glaucomatous optic nerve damage (GOND) in patients with Glaucomatocyclitic Crisis (PSS).
Methods
A computerized literature search was carried out in PubMed database, Wanfang Medical Database, China National Knowledge Infrastructure to collected domestic and foreign research studies on the incidence and related factors of glaucomatous optic nerve damage of Glaucomatocyclitic Crisis. Using Stata 15.1 software, select the indicators: incidence, gender, age, single/double eyes, duration of disease, and intraocular pressure (IOP) at onset for meta-analysis. OR (odds risk) was used as the effect variable for the binary variables, and mean difference was used as the effect variable for the continuous variables. The results are expressed by each effect amount and its 95% Confidence interval (CI). If there was heterogeneity among the original studies, a random effects model was used; otherwise, a fixed effects model was used.
Results
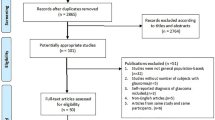
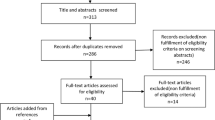
A total of 13 studies were included. The incidence of GOND in PSS was 0.251 (95%CI: 0.175–0.327). Three studies include the relevant factor analysis and the results showed: there was a statistically significant difference in age, and duration of disease in PSS patients with/without GOND (p = 0.000, p = 0.000), there was no statistical difference between the two groups in gender, single /double eyes, and IOP at onset (p = 0.468, 0.053, 0.065).
Conclusion
Glaucomatocyclitic Crisis can cause glaucomatous optic nerve damage. GOND is more likely to occur in patients who are older, and have a long course of the disease. For such patients, special attention should be paid to the detailed examination of visual function and follow-up.






Similar content being viewed by others
Change history
10 May 2022
A Correction to this paper has been published: https://doi.org/10.1007/s10792-022-02248-y
References
Posner A, Schlossman A (1948) Syndrome of unilateral recurrent attacks of glaucoma with cyclitic symptoms. Arch Ophthalmol 39:517–520
Li Z, Zuan X, Chen S et al (1982) Long-term follow-up observation of Glaucomatocyclitic Crisis syndrome. Chin J Ophthalmol 18:306–308
Lu D, Yan R (1982) Analysis of 177 cases of Glaucomatocyclitic Crisis syndrome. Chin J Ophthalmol 18:34–37
Kris M, Becher B, Knlker AE (1973) Glaucomatocyclitic crisis syndrome and primary open angle glaucoma. A J Ophthalmol 75:673–688
Jap A, Sivakumar M, Chee SP (2001) Is Passer-Schlossman syndrome benign? Ophthalmology 108:913–918
Maruyama K (2017) Characteristics of cases needing advanced treatment for intractable Posner-Schlossman syndrome. BMC Ophthalmol 17(1):45. https://doi.org/10.1186/s12886-017-0438-y
Liu Z, Zheng R (2012) The clinical analysis of Glaucomatocyclitic Crisis syndrome. Chin J Pract Ophthalmol 30(8):998–1000
Zhou H, Du Y, Song Y (2002) Related factors of visual field damage in glaucomatocyclitic crisis syndrome. Chin J Pract Ophthalmol 20(10):768–769
Wang H, Ma Z (2017) Analysis of factors related to visual field damage in Posner-Schlossman syndrome. Chin J Chin Ophthalmol 27(5):325–327
Gu S, Liu D, Li J (2018) Curative effect observation of Posner-Schlossman syndrome. J Mil Surg Southwest China 20(2):134–137
Fu P, Hong H (2004) Heterochromic iris as a risk factor for the damage of optic nerve in Posner Schlossman syndrome. Chin J Pract Ophthalmol 22(3):193–195. https://doi.org/10.3760/cma.j.issn.1006-4443.2004.03.012
Luo Q, Cheng Y, Yang Y (2009) Clinical analysis of Posner–Schlossman's syndrome on 32 cases. Int Eye Sci 9(7):1292–1293
Sun L, Guo Z, Li N (2017) Clinical analysis of Posner–Schlossman's syndrome. Women's Health Res 16:93–94
Qiao J (2015) Clinical analysis of Glaucomatocyclitic syndrome. Chin Health Stand Manag 6:156–157
Tang Y (2010) Clinical analysis of damage of visual field with Posner Schlossman's syndrome. Int Eye Sci 10(6):1204–1205
Xu X, Sun J (2014) Clinical analysis of glaucoma cyclitis syndrome. Jilin Med J 35(1):50–53
Wang S, Yin J, Xue C (2005) Clinical analysis of 48 cases of glaucoma cyclitis syndrome. Jiangsu Med J 31(3):215–216
Tran VT, Auer C, Guex Crosier Y et al (1994) Epidemiological characteristics of uveitis in Switzerland. Int Ophthalmol 18(5):293–298
Paivonsalo-Hietanen T, Tuominen J, Vaahtoranta-Lehtonen H et al (1997) Incidence and prevalence of different uveitis entities in Finland. Acta Ophthalmol Scand 75(1):76–81
Bro T, Tallstdet L (2020) Epidemiology of uveitis in a region of southern Sweden. Acta Ophthalmol 98(1):32–35
Shirahama S, Kaburaki T, Nakahara H et al (2018) Epidemiology of uveitis (2013–2015) and changes in the patterns of uveitis (2004–2015) in the central Tokyo area: a retrospective study. BMC Ophthalmol 18(1):189
Sia KJ, Jansen A, Waduthantri S et al (2017) The pattern of uveitis among Chinese, Malays, and Indians in Singapore. Ocul Immunol Inflamm 25(suppl):s81–s93
陆道平, 孙襄男, 乐伊娣, 等, 应用周边前房深度检查法普查 青光眼. 中华眼科杂志1980, 16(3): 204–205
Jiang JH, Zhang SD, Dai ML et al (2017) Posner Schlossman syndrome in Wenzhou, China: a retrospective review study. Br J Ophathalmol 101(12):1638–1642
Raitta C, Vannas A (1977) Glaucomatocyclitic crisis. Arch Ophthalmol 95(4):608–612
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author Huafang Guo declares that he has no conflict of interest. Author Qian Ye declares that she has no conflict of interest. Author Wenqiang Zhang declares that she has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Human and animal participants
This article does not contain any studies with human participants performed by any of the authors. This retrospective study was objectivity and transparency in research, and accepted principles of ethical and professional conduct have been followed. All the authors of this paper have no financial interest in relation to the submission. Human participants in this research have been informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guo, H., Zhang, W. & Ye, Q. A meta-analysis of the rate and related factors of glaucomatous optic nerve damage in patients with Glaucomatocyclitic Crisis. Int Ophthalmol 40, 3145–3153 (2020). https://doi.org/10.1007/s10792-020-01527-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01527-w