Abstract
Purpose
We investigated the factors that influence the reduction in corneal endothelial cells after Ex-Press® surgery.
Methods
This was a retrospective study. We included patients who had undergone Ex-Press surgery and were followed up for > 2. We analyzed the corneal endothelial cell density (ECD) before and after Ex-Press surgery. We investigated the insertion position (Ex-Press device was inserted into cornea or trabecular meshwork (TM)), Ex-Press–iris touch, cornea–iris touch, peripheral anterior synechiae, history of trabeculotomy, history of selective laser trabeculoplasty, type of glaucoma, and simultaneous cataract surgery as influencing factors. We used multivariate analysis to determine the factors influencing the reduction rate of ECD.
Results
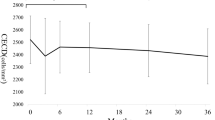
We included 129 eyes. The mean of ECD had decreased 7.0% at 2 years. Ex-Press surgeries significantly decreased the ECD after 2 years (p = 0.0118). As a result of the multivariate analysis, the factor that led to a significantly faster reduction in ECD was the insertion position of the Ex-Press (p < 0.0001). The reduction rate of ECD after 2 years in cases of insertion into the cornea (27 eyes) was 15.1 ± 3.6%, and in cases of insertion into a TM (102 eyes), it was 5.2 ± 1.4%.
Conclusions
Insertion into the cornea was a risk factor for rapid ECD loss. The Ex-Press should be inserted into a TM for long-term protection of the corneal endothelial cells.


Similar content being viewed by others
References
Gonzalez-Rodriguez JM, Trope GE, Drori-Wagschal L, Jinapriya D, Buys YM (2016) Comparison of trabeculectomy versus Ex-PRESS: 3-year follow-up. Br J Ophthalmol 100:1269–1273. https://doi.org/10.1136/bjophthalmol-2015-307161
Chen G, Li W, Jiang F, Mao S, Tong Y (2014) Ex-PRESS implantation versus trabeculectomy in open-angle glaucoma: a meta-analysis of randomized controlled clinical trials. PLOS One 9:e86045. https://doi.org/10.1371/journal.pone.0086045
Netland PA, Sarkisian SR Jr, Moster MR, Ahmed II, Condon G, Salim S, Sherwood MB, Siegfried CJ (2014) Randomized, prospective, comparative trial of EX-PRESS glaucoma filtration device versus trabeculectomy (XVT study). Am J Ophthalmol 157(433–440):e433. https://doi.org/10.1016/j.ajo.2013.09.014
Arimura S, Takihara Y, Miyake S, Iwasaki K, Gozawa M, Matsumura T, Tomomatsu T, Takamura Y, Inatani M (2016) Randomized clinical trial for early postoperative complications of Ex-PRESS implantation versus trabeculectomy: complications postoperatively of Ex-PRESS versus trabeculectomy study (CPETS). Sci Rep 6:26080. https://doi.org/10.1038/srep26080
Mishima S (1982) Clinical investigations on the corneal endothelium. Ophthalmology 89:525–530. https://doi.org/10.1016/s0161-6420(82)34755-7
Arimura S, Miyake S, Iwasaki K, Gozawa M, Matsumura T, Takamura Y, Inatani M (2018) Randomised clinical trial for postoperative complications after Ex-PRESS implantation versus trabeculectomy with 2-Year follow-up. Sci Rep 8:16168. https://doi.org/10.1038/s41598-018-34627-w
Higashide T, Nishino T, Sakaguchi K, Yamada Y, Sugiyama K (2019) Determinants of corneal endothelial cell loss after trabeculectomy with mitomycin C. J Glaucoma 28:61–67. https://doi.org/10.1097/IJG.0000000000001108
Ishida K, Moroto N, Murata K, Yamamoto T (2017) Effect of glaucoma implant surgery on intraocular pressure reduction, flare count, anterior chamber depth, and corneal endothelium in primary open-angle glaucoma. Jpn J Ophthalmol 61:334–346. https://doi.org/10.1007/s10384-017-0512-2
Omatsu S, Hirooka K, Nitta E, Ukegawa K (2018) Changes in corneal endothelial cells after trabeculectomy and EX-PRESS shunt: 2-year follow-up. BMC Ophthalmol 18:243. https://doi.org/10.1186/s12886-018-0913-0
Tojo N, Hayashi A, Otsuka M (2018) Factors influencing the filtration-bleb volume after Ex-PRESS((R)) surgery. Clin Ophthalmol 12:1675–1683. https://doi.org/10.2147/OPTH.S172400
Varadaraj V, Sengupta S, Palaniswamy K, Srinivasan K, Kader MA, Raman G, Reddy S, Ramulu PY, Venkatesh R (2017) Evaluation of angle closure as a risk factor for reduced corneal endothelial cell density. J Glaucoma 26:566–570. https://doi.org/10.1097/Ijg.0000000000000669
Rowsey JJ, Gaylor JR (1980) Intraocular lens disasters: peripheral anterior synechia. Ophthalmology 87:646–664. https://doi.org/10.1016/s0161-6420(80)35189-0
Hasegawa Y, Nejima R, Mori Y, Sakisaka T, Minami K, Miyata K, Oshika T (2016) Risk factors for corneal endothelial cell loss by cataract surgery in eyes with pseudoexfoliation syndrome. Clin Ophthalmol 10:1685–1689. https://doi.org/10.2147/OPTH.S106661
Bourne RR, Minassian DC, Dart JK, Rosen P, Kaushal S, Wingate N (2004) Effect of cataract surgery on the corneal endothelium: modern phacoemulsification compared with extracapsular cataract surgery. Ophthalmology 111:679–685. https://doi.org/10.1016/j.ophtha.2003.07.015
Soro-Martinez MI, Villegas-Perez MP, Sobrado-Calvo P, Ruiz-Gomez JM, de Imperial Miralles, Mora-Figueroa J (2010) Corneal endothelial cell loss after trabeculectomy or after phacoemulsification, IOL implantation and trabeculectomy in 1 or 2 steps. Graefe’s Arch Clin Exp Ophthalmol 248:249–256. https://doi.org/10.1007/s00417-009-1185-4
Gagnon MM, Boisjoly HM, Brunette I, Charest M, Amyot M (1997) Corneal endothelial cell density in glaucoma. Cornea 16:314–318
Smith DL, Skuta GL, Lindenmuth KA, Musch DC, Bergstrom TJ (1991) The effect of glaucoma filtering surgery on corneal endothelial cell density. Ophthalmic Surg 22:251–255
Ayaki M, Noda Y, Yaguchi S, Koide R, Iwasawa A, Inoue T, Inoue Y (2009) Cytotoxicity of antiglaucoma ophthalmic solutions for human corneal endothelial cells. Nippon Ganka Gakkai zasshi 113:576–582
Yamamoto Y, Uno T, Shisida K, Xue LQ, Shiraishi A, Zheng X, Ohashi Y (2006) Demonstration of aqueous streaming through a laser iridotomy window against the corneal endothelium. Arch Ophthalmol Chic 124:387–393. https://doi.org/10.1001/archopht.124.3.387
Sihota R, Sharma T, Agarwal HC (1998) Intraoperative mitomycin C and the corneal endothelium. Acta Ophthalmol Scand 76:80–82
Storr-Paulsen T, Norregaard JC, Ahmed S, Storr-Paulsen A (2008) Corneal endothelial cell loss after mitomycin C-augmented trabeculectomy. J Glaucoma 17:654–657. https://doi.org/10.1097/IJG.0b013e3181659e56
Macdonald JM, Geroski DH, Edelhauser HF (1987) Effect of inflammation on the corneal endothelial pump and barrier. Curr Eye Res 6:1125–1132
Sagoo P, Chan GL, Larkin DFR, George AJT (2004) Inflammatory cytokines induce apoptosis of corneal endothelium through nitric oxide. Investig Ophthalmol Vis Sci 45:3964–3973. https://doi.org/10.1167/iovs.04-0439
Tojo N, Hayashi A, Miyakoshi A (2015) Corneal decompensation following filtering surgery with the Ex-PRESS® mini glaucoma shunt device. Clin Ophthalmol 9:499–502. https://doi.org/10.2147/OPTH.S81050
Hamanaka T, Kasahara K, Takemura T (2011) Histopathology of the trabecular meshwork and Schlemm’s canal in primary angle-closure glaucoma. Investig Ophthalmol Vis Sci 52:8849–8861. https://doi.org/10.1167/iovs.11-7591
Wu KY, Wang HZ, Hong SJ (2008) Mechanism of mitomycin-induced apoptosis in cultured corneal endothelial cells. Mol Vis 14:1705–1712
Zarei R, Zarei M, Fakhraie G, Eslami Y, Moghimi S, Mohammadi M, Abdollahi A (2015) Effect of mitomycin-C augmented trabeculectomy on corneal endothelial cells. J Ophthalmic Vis Res 10:257–262. https://doi.org/10.4103/2008-322X.170345
Leahy KE, Madigan MC, Sarris M, Watson SL, McCluskey P, White AJR (2018) Investigation of corneal endothelial changes post selective laser trabeculoplasty. Clin Exp Ophthalmol 46:730–737. https://doi.org/10.1111/ceo.13172
Kasahara M, Shoji N, Matsumura K (2019) The influence of trabectome surgery on corneal endothelial cells. J Glaucoma 28:150–153. https://doi.org/10.1097/Ijg.0000000000001128
Funding
No funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Human and animals rights
All procedures performed were in accordance with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards, and ethical approval was obtained from the Institutional Review Board of the University of Toyama.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tojo, N., Numata, A. & Hayashi, A. Factors influencing the reduction in corneal endothelial cells after Ex-Press® surgery. Int Ophthalmol 40, 1201–1208 (2020). https://doi.org/10.1007/s10792-020-01286-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01286-8