Abstract
Purpose
This study evaluates the effectiveness of a single-dose dexamethasone implant (DI) as an auxiliary therapy to continued intravitreal ranibizumab (IVR) treatment in patients with persistent diabetic macular edema (DME).
Methods
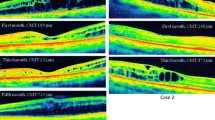
Twenty-five pseudophakic eyes of 25 patients with DME who underwent a single injection of DI as an adjuvant therapy following an IVR loading dose were examined retrospectively. All patients were treatment naive and had a poor response to a loading dose of three consecutive monthly IVR injections. IVR treatments were continued pro re nata after the DI. The main outcome measures were changes in best-corrected visual acuity (BCVA) and central macular thickness (CMT) at 1, 3, 6 and 8 months post-DI treatment.
Results
After the IVR loading dose, the mean BCVA and CMT were 0.9 ± 0.6 LogMAR and 478.2 ± 107.8 µm, respectively. One month after the DI, the mean BCVA and CMT had improved to 0.6 ± 0.4 LogMAR (p = 0.005) and 313.8 ± 62.7 µm (p < 0.001), respectively. This improvement was maintained with mean 0.8 ± 0.8 IVR injections throughout the follow-up period. The final mean BCVA and CMT were 0.5 ± 0.5 LogMAR and 298.4 ± 71.5 µm. Subgroup analyses revealed that different DME types did not have any effect on CMT or BCVA improvement (p = 0.188, p = 0.136; respectively).
Conclusion
Adding DI results in rapid anatomical and visual improvement in patients who respond poorly to an IVR loading dose. Improvements may be maintained with additional IVR in follow-up.





Similar content being viewed by others
References
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL (1984) The Wisconsin epidemiologic study of diabetic retinopathy. IV. Diabetic macular edema. Ophthalmology 91:1464–1474
Do DV, Schmidt-Erfurth U, Gonzalez VH et al (2011) The DA VINCI study: phase 2 primary results of VEGF Trap-Eye in patients with diabetic macular edema. Ophthalmology 118:1819–1826
Cunningham ET Jr, Adamis AP, Altaweel M et al (2005) Macugen Diabetic Retinopathy Study Group. A phase II randomized double-masked trial of pegaptanib, an anti-vascular endothelial growth factor aptamer, for diabetic macular edema. Ophthalmology 112:1747–1757
Cheung N, Wong IY, Wong TY (2014) Ocular anti-VEGF therapy for diabetic retinopathy: over-view of clinical efficacy and evolving applications. Diabetes Care 37:900–905
Nguyen QD, Brown DM, Marcus DM et al (2012) RISE and RIDE Research Group. Ranibizumab for diabetic macular edema: results from 2 phase III randomized trials: RISE and RIDE. Ophthalmology. 119:789–801
Ho AC, Scott IU, Kim SJ et al (2012) Anti-vascular endothelial growth factor pharmacotherapy for diabetic macular edema: a report by the American Academy of Ophthalmology. Ophthalmology 119:2179–2188
Tamura H, Miyamoto K, Kiryu J et al (2005) Intravitreal injection of corticosteroid attenuates leukostasis and vascular leakage in experimental diabetic retina. Invest Ophthalmol Vis Sci 46:1440–1444
Grover D, Li TJ, Chong CC (2008) Intravitreal steroids for macular edema in diabetes. Cochrane Database Syst Rev 1:CD005656
Elman MJ, Aiello LP, Beck RW et al (2010) Diabetic Retinopathy Clinical Research Network. Randomized trial evaluating ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology 117:1064–1077
Smithen LM, Ober MD, Maranan L, Spaide RF (2004) Intravitreal triamcinolone acetonide and intraocular pressure. Am J Ophthalmol 138:740–743
Pacella E, Vestri AR, Muscella R et al (2013) Preliminary results of an intravitreal dexamethasone implant (Ozurdex) in patients with persistent diabetic macular edema. Clin Ophthalmol 7:1423–1428
Boyer DS, Yoon YH, Belfort R Jr et al (2014) Ozurdex MEAD Study Group. Three-year, randomized, sham-controlled trial of dexamethasone intravitreal implant in patients with diabetic macular edema. Ophthalmology 121:1904–1914
Ferris FL III, Maguire MG, Glassman AR, Ying GS, Martin DF (2016) Evaluating effects of switching anti-vascular endothelial growth factor drugs for age-related macular degeneration and diabetic macular edema. JAMA Ophthalmol 1:22. https://doi.org/10.1001/jamaophthalmol.2016.4820
Chatziralli I, Santarelli M, Patrao N et al (2017) Identification of time point to best define ‘sub-optimal response’ following intravitreal ranibizumab therapy for diabetic macular edema based on real-life data. Eye (Lond) 31(11):1594–1599
Maturi RK, Glassman AR, Liu D et al (2017) Diabetic Retinopathy Clinical Research Network. Effect of adding dexamethasone to continued ranibizumab treatment in patients with persistent diabetic macular edema: a DRCR Network Phase 2 randomized clinical trial. JAMA Ophthalmol Nov:11. https://doi.org/10.1001/jamaophthalmol.2017.4914
Ying GS, Maguire MG, Daniel E et al (2015) Comparison of Age-Related Macular Degeneration Treatments Trials (CATT) Research Group. Association of baseline characteristics and early vision response with 2-year outcomes in the Comparison of AMD Treatments Trials (CATT). Ophthalmology 122(12):2523.e1–2531.e1
Elman MJ, Aiello LP, Beck RW et al (2010) Diabetic Retinopathy Clinical Research Network. Randomized trial evaluating ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology 117(6):1064.e35–1077.e35
Cicinelli MV, Cavalleri M, Querques L, Rabiolo A, Bandello F, Querques G (2017) Early response to ranibizumab predictive of functional outcome after dexamethasone for unresponsive diabetic macular oedema. Br J Ophthalmol 101(12):1689–1693
Acknowledgements
The authors have no financial interest in any materials used in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any financial/conflicting interests to disclose.
Rights and permissions
About this article
Cite this article
Cakir, A., Erden, B., Bolukbasi, S. et al. Dexamethasone implant as an adjuvant therapy to ranibizumab loading dose in persistent diabetic macular edema. Int Ophthalmol 39, 2179–2185 (2019). https://doi.org/10.1007/s10792-018-1053-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-018-1053-5