Abstract
Purpose
To report the therapeutic efficacy and safety of topical 0.1% lodoxamide in the long-term treatment of superior limbic keratoconjunctivitis.
Methods
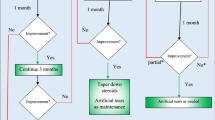
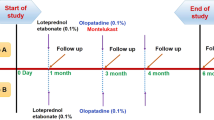
Sixty-seven eyes of 34 patients with active SLK were studied. Therapeutic response was analyzed according to modified-Ohashi parameters. All eyes were treated with 0.1% lodoxamide twice daily, and those with moderate or severe inflammation received a short course (7–14 days) of 0.1% fluorometholone acetate at presentation and during a relapse. Patients were evaluated at regular intervals and followed up for ≥3 months on continuous therapy. Primary endpoints included inflammatory response; rates of inflammatory control and remission; relapses while on therapy or on remission; and therapeutic failure rate.
Results
The mean follow-up time on lodoxamide therapy was 15.3 months. The majority of eyes (82.0%) achieved control of inflammation in a mean time of 2.2 months. Of these, 42 (76.3%) eyes remained under control while on therapy for 13.8 months. There was a significant improvement of SLK-related signs by the third month on therapy (p < 0.05). A total of 24 (35.8%) eyes achieved remission. Relapses presented in 12 (18.0%) treated eyes and in 4 (16.6%) eyes on remission. Only 5 (7.4%) eyes failed to respond to therapy. In the majority of cases (95.3%), lodoxamide 0.1% was well tolerated and minor adverse effects not requiring stopping the medication were reported in only 4.7% of patients.
Conclusions
Lodoxamide 0.1% is an efficacious therapeutic alternative for the treatment of active and chronic SLK. This medication has proved to be safe and well tolerated.


Similar content being viewed by others
References
Corwin ME (1968) Superior limbic keratoconjunctivitis. Am J Ophthalmol 66:338–340
Theodore FH (1963) Superior limbic keratoconjunctivitis. Eye Ear Nose Throat 42:25–28
Wright P (1972) Superior limbic keratoconjunctivitis. Trans Ophthalmol Soc UK 92:555–560
Nelson JD (1989) Superior limbic keratoconjunctivitis (SLK). Eye Lond 3:180–189
Theodore FH, Ferry AP (1970) Superior limbic keratoconjunctivitis: clinical and pathologic correlations. Arch Ophthalmol 84:481–484
Mendoza-Adam G, Rodriguez-Garcia A (2013) Superior limbic keratoconjunctivitis (SLK) and its association to systemic diseases. Rev Mex Oftalmol 87:93–99
Kadrmas EF, Bartley GB (1995) Superior limbic keratoconjunctivitis: a prognostic sign for severe Grave´s ophthalmopathy. Ophthalmology 102:1472–1475
Cher I (2000) Superior limbic keratoconjunctivitis: multifactorial mechanical pathogenesis. Clin Exp Ophthalmol 28:181–184
Eiferman RA, Wilkins EL (1979) Immunological aspects of superior limbic keratoconjunctivitis. Can J Ophthalmol 14:85–87
Sun YC, Hsiao CH, Chen WL, Wang IJ, Hou YC, Hu FR (2008) Conjunctival resection combined with Tenon layer excision and the involvement of mast cells in superior limbic keratoconjunctivitis. Am J Ophthalmol 145:445–452
Goto E, Shimmura S, Shimazaki J, Tsubota K (2001) Treatment of superior limbic keratoconjunctivitis by application of autologous serum. Cornea 20:807–810
Ohashi Y, Watanabe H, Kinoshita S, Hosotani H, Umemoto M, Manabe R (1998) Vitamin-A eye drops for superior limbic keratoconjunctivitis. Am J Ophthalmol 105:523–527
Donshik PC, Collin HB, Foster CS, Cavanagh HD, Boruchoff SA (1978) Conjunctival resection treatment and ultrastructural histopathology of superior limbic keratoconjunctivitis. Am J Ophthalmol 85:101–110
Passons GA, Wood TO (1984) Conjunctival resection for superior limbic keratoconjunctivitis. Ophthalmology 91:966–968
Udell IJ, Kenyon KR, Sawa M, Dohlman CH (1986) Treatment of superior limbic keratoconjunctivitis by thermocauterization of the superior bulbar conjunctiva. Ophthalmology 93:162–166
Mondino BJ, Zaidman GW, Salamon SW (1982) Use of pressure patching and soft contact lenses in superior limbic keratoconjunctivitis. Arch Ophthalmol 100:1932–1934
Yang HY, Fujishima H, Toda I, Shimazaki J, Tsubota K (1997) Lacrimal punctal occlusion for the treatment of superior limbic keratoconjunctivitis. Am J Ophthalmol 124:80–87
Kabat AG (1998) Lacrimal occlusion therapy for the treatment of superior limbic keratoconjunctivitis. Optom Vis Sci 75:714–718
Shen YC, Wang CY, Tsai HY, Lee YF (2007) Supratarsal triamcinolone injection in the treatment of superior limbic keratoconjunctivitis. Cornea 26:423–426
Fraunfelder FW (2009) Liquid nitrogen cryotherapy of superior limbic keratoconjunctivitis. Am J Ophthalmol 147:234–238
Chun YS, Kim JC (2014) Treatment of superior limbic keratoconjunctivitis using botulinum toxin A. Korean J Optom Vis SCi 13:46–52
Liu J, Sheha H, Fu Y, John T, Tseng SC (2011) A new surgical approach of amniotic membrane transplantation for superior limbic keratoconjunctivitis. Techn Ophthalmol 9:41–43
Gris O, Plazas A, Lerma E, Güell JL, Pelegrín L, Elíes D (2010) Conjunctival resection with and without amniotic membrane graft for the treatment of superior limbic keratoconjunctivitis. Cornea 29:1025–1030
Ahn JM, Choi CY, Seo KY (2014) Surgical approach with high-frequency radiowave electrosurgery for superior limbic keratoconjunctivitis. Cornea 33:210–214
Kim WS, Wee SW, Kim JC (2014) Two cases of superior limbic keratoconjunctivitis treated with bevacizumab and triamcinolone injection. J Korean Ophthalmol Soc 55:443–448
Sanchez JC, Mesa D, Avendafio E (2013) Superior limbic keratoconjunctivitis. In: Benitez del Castillo JM, Lemp MA (eds) Ocular surface disorders, vol 25. JP Medical, LTD, New Delhi, pp 215–219
Bonini S, Schiavone M, Bonini S, Magrini L, Lischetti P, Lambiase A, Bucci MG (1997) Efficacy of lodoxamide eye drops on mast cells and eosinophils after allergen challenge in allergic conjunctivitis. Ophthalmology 104:849–853
Yanni JM, Weimer LK, Glaser RL, Lang LS, Robertson SM, Spellman JM (1993) Effect of lodoxamide on in vitro and in vivo conjunctival immediate hypersensitivity responses in rats. Int Arch Allergy Immunol 101:102–106
Caldwell DR, Verin P, Hartwich-Young R (1992) Efficacy and safety of lodoxamide 0.1% versus cromolyn sodium 4% in patients with vernal keratoconjunctivitis. Am J Ophthalmol 113:632–637
Denis D, Bloch-Michel E, Verin P, Sebastiani A, Tazartes M, Helleboid L, Di Giovanni A, Lecorvec M (1998) Treatment of common ocular allergic disorders; a comparison of lodoxamide and NAAGA. Br J Ophthalmol 82:1135–1138
Grutzmacher RD, Foster RS, Feiler LS (1995) Lodoxamide tromethamine treatment for superior limbic keratoconjunctivitis. Am J Ophthalmol 120:400–402
Khalil M, Malik TG, Munawar S (2013) Use of silver nitrate in superior limbic keratoconjunctivitis. Pak J Ophthalmol 29:181–182
Takahashi Y, Ichinose A, Kakizaki H (2014) Topical rebamipide treatment for superior limbic keratoconjunctivitis in patients with thyroid eye disease. Am J Ophthalmol 157:807–812
Yokoi N, Komuro A, Maruyama K, Tsuzuki M, Miyajima S, Kinoshita S (2003) New surgical treatment for superior limbic keratoconjunctivitis and its association with conjunctivochalasis. Am J Ophthalmol 135:303–308
Sun YC, Hsiao CH, Chen WL, Hu FR (2011) Overexpression of matrix metalloproteinase-1 (MMP-1) and MMP-3 in superior limbic keratoconjunctivitis. Invest Ophthalmol Vis Sci 52:3701–3705
Li DQ, Meller D, Liu Y, Tseng SC (2000) Overexpression of MMP-1 and MMP-3 by cultured conjunctivochalasis fibroblasts. Invest Ophthalmol Vis Sci 41:404–410
Matsuda A, Tagawa Y, Matsuda H (1996) Cytokeratin and proliferative cell nuclear antigen expression in superior limbic keratoconjunctivitis. Curr Eye Res 15:1033–1038
Matsuda A, Tagawa Y, Matsuda H (1999) TGF-beta2, tenascin, and integrin beta1 expression in superior limbic keratoconjunctivitis. Jpn J Ophthalmol 43:251–256
Kinet JP (2007) The essential role of mast cells in orchestrating inflammation. Immunol Rev 217:5–7
Greiner JV, Peace DG, Baird RS, Allansmith MR (1985) Effects of eye rubbing on the conjunctiva as a model of ocular inflammation. Am J Ophthalmol 100:45–50
Murphy GF, Austen KF, Fonferko E, Sheffer AL (1987) Morphologically distinctive forms of cutaneous mast cell degranulation induced by cold and mechanical stimuli: an ultrastructural study. J Allergy Clin Immunol 80:603–611
Allakhverdi Z, Comeau MR, Jessup HK (2007) Thymic stromal lymphopoietin is released by human epithelial cells in response to microbes, trauma, or inflammation and potently activates mast cells. J Exp Med 204:253–258
Sun YC, Liou HM, Shen EP, Hu FR (2015) Stem cell factor and thymic stromal lymphopoietin overexpression with correlation to mast cells in superior limbic keratoconjunctivitis. Cornea 34:1487–1492
Confino J, Brown SI (1987) Treatment of superior limbic keratoconjunctivitis with topical cromolyn sodium. Ann Ophthalmol 19:129–131
Udell IJ, Guidera AC, Madani-Becker J (2002) Ketotifen fumarate treatment of superior limbic keratoconjunctivitis. Cornea 21:778–780
Mantelli F, Santos MS, Petitti T, Sgrulletta R, Cortes M, Lambiase A, Bonini S (2007) Systematic review and meta-analysis of randomised clinical trials on topical treatments for vernal keratoconjunctivitis. Br J Ophthalmol 91:1656–1661
Sahin A, Bozkurt B, Irkec M (2008) Topical cyclosporine-A in the treatment of superior limbic keratoconjunctivitis: a long-term follow-up. Cornea 27:193–195
Perry HD, Doshi-Carnevale S, Donnenfeld ED, Kornstein HS (2003) Topical cyclosporine A 0.5% as a possible new treatment for superior limbic keratoconjunctivitis. Ophthalmology 110:1578–1581
Kymionis GD, Klados NE, Kontadakis GA, Mikropoulos DG (2013) Treatment of superior limbic keratoconjunctivitis with topical tacrolimus 0.03% ointment. Cornea 32:1499–1501
Whitcup SM, Chan CC, Luyo DA, Bo P, Li Q (1996) Topical cyclosporine inhibits mast cell-mediated conjunctivitis. Invest Ophthalmol Vis Sci 37:2686–2693
Acknowledgements
We would like to thank Dr. Luis A. Gonzales for his advice in the design and statistical analysis of the study.
Funding
This study was funded in part by Fundacion Santos y de la Garza-Evia, I.B.P. (a non-profit private charity institution). No other institution participated in funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Alejandro Rodriguez Garcia is a consultant for ALCON (Novartis) laboratories. The rest of the authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants for whom identifying information is included in this article (materials and methods section).
Rights and permissions
About this article
Cite this article
Rodriguez-Garcia, A., Macias-Rodriguez, Y. & Gonzalez-Gonzalez, J.M. Efficacy and safety of 0.1% lodoxamide for the long-term treatment of superior limbic keratoconjunctivitis. Int Ophthalmol 38, 1243–1249 (2018). https://doi.org/10.1007/s10792-017-0588-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-017-0588-1