Abstract
Purpose
This prospective observational case series study aimed to observe the clinical characteristics of acute zonal occult outer retinopathy (AZOOR) and its prognosis in Chinese Han patients.
Methods
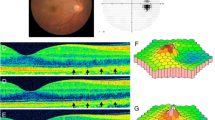
Six eyes of 5 female patients diagnosed with AZOOR were followed up for 4 months to observe the natural disease course. All enrolled subjects underwent a series of ocular examinations at the onset and each return visit, including best corrected visual acuity (BCVA), split lamp microscopy, fundus photography, optical coherence tomography (OCT), perimetry, multifocal electroretinogram and fundus fluorescein angiography.
Results
Over the follow-up, all enrolled patients recovered on BCVA, perimetry and OCT in different degrees. Among them, one patient recovered completely since the ocular examination results returned to normal.
Conclusion
AZOOR is a rare ocular disorder in Chinese population. Our results demonstrated that visual functions of enrolled patients significantly improved spontaneously, indicating that Chinese female Han patients with AZOOR have good visual outcomes during the follow-up period without any specific managements.





Similar content being viewed by others
References
Gass JD (1993) Acute zonal occult outer retinopathy. Donders Lecture: The Netherlands Ophthalmological Society, Maastricht, Holland, June 19, 1992. J Clin Neuroophthalmol 13(2):79–97
Li D, Kishi S (2007) Loss of photoreceptor outer segment in acute zonal occult outer retinopathy. Arch Ophthalmol 125(9):1194–1200. doi:10.1001/archopht.125.9.1194
Tsunoda K, Fujinami K, Miyake Y (2011) Selective abnormality of cone outer segment tip line in acute zonal occult outer retinopathy as observed by spectral-domain optical coherence tomography. Arch Ophthalmol 129(8):1099–1101. doi:10.1001/archophthalmol.2011.217
Gass JD, Agarwal A, Scott IU (2002) Acute zonal occult outer retinopathy: a long-term follow-up study. Am J Ophthalmol 134(3):329–339
Monson DM, Smith JR (2011) Acute zonal occult outer retinopathy. Surv Ophthalmol 56(1):23–35. doi:10.1016/j.survophthal.2010.07.004
Fujiwara T, Imamura Y, Giovinazzo VJ, Spaide RF (2010) Fundus autofluorescence and optical coherence tomographic findings in acute zonal occult outer retinopathy. Retina 30(8):1206–1216. doi:10.1097/IAE.0b013e3181e097f0
Matsui Y, Matsubara H, Ueno S, Ito Y, Terasaki H, Kondo M (2014) Changes in outer retinal microstructures during 6 month period in eyes with acute zonal occult outer retinopathy-complex. PLoS ONE 9(10):e110592. doi:10.1371/journal.pone.0110592
Arai M, Nao-i N, Sawada A, Hayashida T (1998) Multifocal electroretinogram indicates visual field loss in acute zonal occult outer retinopathy. Am J Ophthalmol 126(3):466–469
Spaide RF, Koizumi H, Freund KB (2008) Photoreceptor outer segment abnormalities as a cause of blind spot enlargement in acute zonal occult outer retinopathy-complex diseases. Am J Ophthalmol 146(1):111–120. doi:10.1016/j.ajo.2008.02.027
Fine HF, Spaide RF, Ryan EH Jr, Matsumoto Y, Yannuzzi LA (2009) Acute zonal occult outer retinopathy in patients with multiple evanescent white dot syndrome. Arch Ophthalmol 127(1):66–70. doi:10.1001/archophthalmol.2008.530
Neutzner RV, Jager M, Friedburg C, Deeg CA, Lorenz B (2011) Blind spot enlargement syndrome in acute zonal occult outer retinopathy with detection of autoantibodies against the retinal antigens CRALBP and S-Ag. Der Ophthalmologe: Zeitschrift der Deutschen Ophthalmologischen Gesellschaft 108(11):1045–1049. doi:10.1007/s00347-011-2406-x
Tagami M, Matsumiya W, Imai H, Kusuhara S, Honda S, Azumi A (2014) Autologous antibodies to outer retina in acute zonal occult outer retinopathy. Jpn J Ophthalmol 58(6):462–472. doi:10.1007/s10384-014-0347-z
Song ZM, Sheng YJ, Chen QS, Xue AQ, Lin B, Li YZ, Fu XY (2008) Clinical characteristics of acute zonal occult outer retinopathy in Chinese patients. Ophthalmologica Journal international d’ophtalmologie International journal of ophthalmology Zeitschrift fur Augenheilkunde 222(3):149–156. doi:10.1159/000126076
Chen SN, Yang CH, Yang CM (2015) Systemic corticosteroids therapy in the management of acute zonal occult outer retinopathy. J Ophthalmol 2015:793026. doi:10.1155/2015/793026
Gass JD (2003) Acute zonal occult outer retinopathy: Donders Lecture: The Netherlands Ophthalmological Society, Maastricht, Holland, June 19, 1992. 1993. Retina 23(6 Suppl):79–97
Gass JD (2000) The acute zonal outer retinopathies. Am J Ophthalmol 130(5):655–657
Jacobson SG, Morales DS, Sun XK, Feuer WJ, Cideciyan AV, Gass JD, Milam AH (1995) Pattern of retinal dysfunction in acute zonal occult outer retinopathy. Ophthalmology 102(8):1187–1198
Spaide RF, Yannuzzi LA, Freund KB (1991) Linear streaks in multifocal choroiditis and panuveitis. Retina 11(2):229–231
Watzke RC, Shults WT (2002) Clinical features and natural history of the acute idiopathic enlarged blind spot syndrome. Ophthalmology 109(7):1326–1335
Liu X, Chen B, Zhang M, Huang H (2014) Clinical features and differential diagnosis of acute idiopathic blind spot enlargement syndrome. Eye Sci 29(3):143–150
Piri N, Kaplan HJ, Sigford DK, Tezel TH (2014) High-definition optical coherence tomography findings in acute idiopathic blind spot enlargement (AIBSE) syndrome. Ocular Immunol Inflamm 22(6):494–496. doi:10.3109/09273948.2013.872802
Volpe NJ, Rizzo JF 3rd, Lessell S (2001) Acute idiopathic blind spot enlargement syndrome: a review of 27 new cases. Arch Ophthalmol 119(1):59–63
Acknowledgements
We are grateful to Dr. Yanbo Shi (Jiaxing Traditional Chinese Medicine Hospital Affiliated to Zhejiang Chinese Medical University) and Ms. Julie Qiaojin Lin (Department of Physiology, Development and Neuroscience, University of Cambridge) for editing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Si, S., Song, W., Song, Y. et al. The clinical characteristics and prognosis of acute zonal occult outer retinopathy. Int Ophthalmol 38, 1177–1185 (2018). https://doi.org/10.1007/s10792-017-0580-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-017-0580-9