Abstract
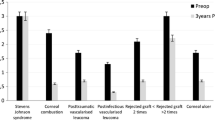
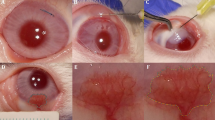
The purpose of this study is to investigate whether subconjunctival and/or intrastromal Bevacizumab injections could help to prevent graft failure in high-risk keratoplasties. Twenty seven eyes of 27 patients, affected by high immune rejection risk and corneal neovascularization, were involved in this prospective interventional case–control series (case group: 14 eyes and control group: 13 eyes). Case group was submitted to a cycle of three subconjunctival and/or intrastromal injections of 5 mg/0.2 ml Bevacizumab. After a mean period of 6.36 months ± 3.38 SD from the last injection, all patients underwent keratoplasty. An adjunctive injection was performed intraoperatively at the end of the surgical procedure. Control group did not receive any Bevacizumab injection, but directly underwent keratoplasty. Each patient was submitted to a complete eye examination and corneal confocal microscopy. The absence of immune rejection signs in the graft, at clinical and confocal microscopy examination, was considered as main outcome measure. All cases showed less ocular inflammation and activity of vessels. No side effects were detected after the injection procedure. No corneal graft rejection was seen during the follow-up (mean 26.1 months ± 5.7 SD) in the case group. Six eyes of the control group showed graft rejection 3.8 months ± 1.4 SD after keratoplasty. As a conclusion, Bevacizumab injection may represent a preconditioning treatment to improve prognosis in high-risk corneal transplantation. The procedure seems to be safe and it may help to reduce the inflammatory stimulus that plays a key role in corneal graft rejection.



Similar content being viewed by others
References
Chang Jin-Hong, Garg Nitin K, Lunde Elisa et al (2012) Corneal neovascularization: an anti-VEGF therapy review. Surv Ophtahalmol 57(5):415–429
Awadein A (2007) Subconjunctival bevacizumab for vascularized rejected corneal grafts. J Cataract Refract Surg 33:1991–1993
Patel HY, Ormonde S, Brookes NH et al (2011) The New Zeland National Eye Bank: survival and visual outcome 1 year after penetrating keratoplasty. Cornea 30(7):760–764
Panda A, Vanathi M, Kumar A, Dash Y, Priya S (2007) Corneal graft rejection. Surv Ophthalmol 52(4):375–396
Vassileva PI, Hergeldzhieva TG (2009) Avastin use in high risk corneal transplantation. Graefes Arch Clin Exp Ophthalmol 247:1701–1706
Amano S, Rohan R, Kuroki M et al (1998) Requirement for vascular endothelial growth factor in wound and inflammation related corneal neovascularization. Invest Ophthalmol Vis Sci 39:18–22
Niederkorn JY (2007) Immune mechanisms of corneal allograft rejection. Curr Eye Res 32:1005–1016
Pleyer U, Schlickeiser S (2009) The taming of the shrew? The immunology of corneal transplantation. Acta Ophthalmol 87:488–497
Mosca L, Fasciani R, Mosca L et al (2011) Graft rejection after Femtosecond-assisted deep anterior lamellar keratoplasty: report of 3 cases. Cornea 30(8):912–916
Alessio G, L’Abbate M, Boscia F et al (2010) Excimer laser-assisted keratoplasty and the corneal endothelium. Am J Ophthalmol 150:88–96
Joussen AM, Kruse FE, Volcker HE et al (1999) Topical application of methotrexate for inhibition of corneal angiogenesis. Graefes Arch Clin Exp Ophthalmol 237:920–927
Lipman RM, Epstein RJ, Hendricks RL (1992) Suppression of corneal neovascularization with cyclosporine. Arch Ophthalmol 110:405–407
D’Amato RJ, Loughnan MS, Flynn E et al (1994) Thalidomide is an inhibitor of angiogenesis. Proc Natl Acad Sci USA 91:4082–4085
Kvanta A, Sarman S, Fagerholm P et al (2000) Expression of matrix metalloproteinase-2 (MMP-2) and vascular endothelial growth factor (VEGF) in inflammation associated corneal neovascularization. Exp Eye Res 70:419–428
Gan L, Fagerholm P, Palmblad J (2004) Vascular endothelial growth factor (VEGF) and its receptor VEGFR-2 in the regulation of corneal neovascularization and wound healing. Acta Ophthalmol Scand 82:557–563
Edelman JL, Castro MR, Wen Y (1999) Correlation of VEGF expression by leukocytes with the growth and regression of blood vessels in the rat cornea. Invest Ophthalmol Vis Sci 40:1112–1123
Benayoun Y, Adenis JP, Casse G et al (2012) Effects of subconjunctival bevacizumab on corneal neovascularization: results of a prospective study. Cornea 31(8):934–944
Symes RJ, Poole TRG (2010) Corneal graft surgery combined with subconjunctival bevacizumab (Avastin). Cornea 29:691–693
Acar BT, Halili E, Acar S (2013) The effect of different doses of subconjunctival bevacizumab injection on corneal neovascularization. Int Ophthalmol 33(5):507–513
Petsoglou C, Balaggan KS, Dart JKG et al (2013) Subconjunctival bevacizumab induces regression of corneal neovascularisation: a pilot randomized placebo-controlled double-masked trial. Br J Ophthalmol 97:28–32
Stevenson W, Cheng SF, Dastjerdi MH et al (2012) Corneal neovascularization and the utility of topical VEGF inhibition: ranibizumab (Lucentis) vs bevacizumab (Avastin). Ocul Surf 10(2):67–83
Ferrara N, Leung DW, Phillips HS (1991) Molecular characterization and distribution of vascular endothelial growth factor. In: Muller EE, MacLeod RB (eds) Neuroendocrine Perspectives. Springer-Verlag, New York, p 127
Breier G, Albrecht U, Sterrer S et al (1992) Expression of vascular endothelial growth factor during embryonic angiogenesis and endothelial cell differentiation. Development 114:521–532
Dastjerdi NH, Saban DN, Okanobo A et al (2010) Effects of topical and subconjunctival bevacizumab in high-risk corneal transplant survival. Invest Ophthalmol Vis Sci 51(5):2411–2417
Niederer LR, Sherwin T, McGhee CNJ (2007) In vivo confocal microscopy of subepithelial infiltrates in human corneal transplant rejection. Cornea 26:501–504
Cursiefen C, Chen Lu, Borges LP et al (2004) VEGF-A stimulates lymphangiogenesis and hemangiogenesis in inflammatory neovascularization via macrophages recruitment. J Clin Invest 113:1040–1050
Traversi C, Nuti E, Bovone C (2009) Principi di immunologia. Newsletter S.I.TRA.C. No 3, 1–2 Oct 2009
Cursiefen C, Küchle M (1998) Naumann GOH: angiogenesis in corneal diseases: histopathologic evaluation of 254 human corneal buttons with neovascularisation. Cornea 17:611–613
Rama P, Insacco C (2009). Rigetto nel trapianto di cornea perforante. Newsletter S.I.TRA.C.No 3, 3–4 Oct 2009
Fontana L, Parente G, Tassinari G (2009). Reazioni di rigetto dopo cheratoplastica lamellare anteriore profonda, aspetti clinici. Newsletter S.I.TRA.C.No 3, 3 Oct 2009
Funding/Support
None.
Financial Disclosure
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fasciani, R., Mosca, L., Giannico, M.I. et al. Subconjunctival and/or intrastromal bevacizumab injections as preconditioning therapy to promote corneal graft survival. Int Ophthalmol 35, 221–227 (2015). https://doi.org/10.1007/s10792-014-9938-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-014-9938-4