Abstract
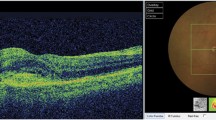
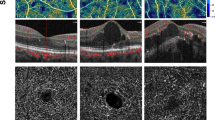
To assess the relationships between visual acuity (VA), fluorescein angiographic parameters and optical coherence tomography (OCT) patterns in exudative age-related macular degeneration (AMD). Fifty eyes with confirmed diagnosis of new exudative AMD who underwent fluorescein angiography (FA) and OCT evaluation were reviewed retrospectively. The greatest linear diameter of lesion (GLD) by FA and central foveal thickness (CFT) by OCT were measured. The OCT scans were evaluated for the presence of diffuse retinal thickening (D), cystic spaces (C), subretinal fluid (S) and pigment epithelial detachment (P) and five OCT patterns were detected (D + S; C; C + S; P + C + S; P + D + S). Angiographic classification of choroidal neovascularizations was performed. Correlations were statistically significant for VA and CFT in all patients whereas VA and GLD correlation was statistically significant only in predominantly classic and minimal classic lesions. The lowest VA values were detected in patients with COCT pattern and/or predominantly classic lesion type by FA. The OCT and FA findings when evaluated simultaneously may provide information regarding visual function in AMD.

Similar content being viewed by others
References
The Eye Diseases Prevalence Research Group (2004) Prevalence of age-related macular degeneration in the United State. Arch Ophthalmol 122:564–572
Bresssler NM, Bressler SB, Fine SL (1988) Age-related macular degeneration macular degeneration. Surv Ophthalmol 32:375–413
Ferris FL 3rd, Fine SL, Hyman L (1984) Age-related macular degeneration and blindness due to neovascular maculopathy. Arch Ophthalmol 102:1640–1642
Macular Photocoagulation Study Group (1991) Subfoveal neovascular lesions in age-related macular degeneration: guidelines for evaluation and treatment in the macular photocoagulation study. Arch Ophthalmol 109:1242–1257
Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) Study Group (1999) Photodynamic therapy of subfoveal choroidal neovascularisation in age-related macular degeneration with verteporfin. One year results of 2 randomized clinical trials-TAP report 1. Arch Ophthalmol 117:1329–1345
Yogonathan P, Deramo VA, Lai JC et al (2006) Visual improvement following intravitreal bevacizumab (Avastin) in exudative age-related macular degeneration. Retina 26:994–998
Chen CY, Wong JY, Heroit WJ et al (2007) İntravitreal bevacizumab (Avastin) for neovascular age-related macular degeneration: a short-term study. Am J Ophthalmol 143:510–512
Salinas-Alman A, Gracia-Layana A, Maldonado MJ et al (2005) Using optical coherence tomography in monitor photodynamic therapy in age related macular degeneration. Am J Ophthalmol 140:23–28
Moutray T, Alarby M, Stevenson M et al (2008) Relationships between clinical measures of visual function, fluorescein angiographic and optical coherence tomography features in patients with subfoveal choroidal neovascularisation. Br J Ophthalmol 92:361–364
Sahni J, Stanga P, Wong D et al (2005) Optical coherence tomography in photodynamic therapy for subfoveal choroidal neovascularisation secondary to age related macular degeneration: a cross sectional study. Br J Ophthalmol 89:316–320
Van de Moere A, Sandhu SS, Talks SJ (2006) Correlation of optical coherence tomography and fundus fluorescein angiography following photodynamic therapy for choroidal neovascular membranes. Br J Ophthalmol 90:304–306
Keane PA, Liakopoulos S, Chang KT et al (2008) Relationships between optical coherence tomography retinal parameters and visual acuity in neovascular age-related macular degeneration. Ophthalmology 115:2206–2214
Conflict of interest
The authors have no proprietary or commercial interest in any materials discussed in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yaylali, S.A., Akcakaya, A.A., Erbil, H.H. et al. The relationship between optical coherence tomography patterns, angiographic parameters and visual acuity in age-related macular degeneration. Int Ophthalmol 32, 25–30 (2012). https://doi.org/10.1007/s10792-012-9519-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-012-9519-3