Abstract
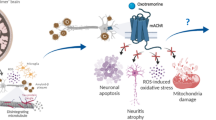
Alzheimer’s disease (AD) is a major neurological disease affecting elderly individuals worldwide. Existing drugs only reduce the symptoms of the disease without addressing the underlying causes. Commonly, Aβ25–35 peptide aggregation is the main reason for AD development. Recently, the discovery of multiple protein-targeting molecules has provided a new strategy for treating AD. This study demonstrates the neuroprotective potential of oxymatrine against multiple mechanisms, such as acetylcholinesterase, mitochondrial damage, and β-amyloid-induced cell toxicity. The in vitro cell culture studies showed that oxymatrine possesses significant potential to inhibit acetylcholine esterase and promotes antioxidant, antiapoptotic effects while preventing Aβ25–35 peptide aggregation in PC12 cells. Furthermore, oxymatrine protects PC12 cells against Aβ25–35-induced cytotoxicity and down-regulates the reactive oxygen species generation. The in vivo acute toxicological studies confirm the safety of oxymatrine without causing organ damage or death in animals. Overall, this study provided evidence that oxymatrine is an efficient neuroprotective agent, with a potential to be a multifunctional drug for Alzheimer’s disease treatment. These findings present a reliable and synergistic approach for treating AD.










Similar content being viewed by others
Data availability
Not applicable.
References
Abeysinghe AADT, Deshapriya RDUS, Udawatte C (2020) Alzheimer’s disease; a review of the pathophysiological basis and therapeutic interventions. Life Sci 256:117996
Al-Afifi NA, Alabsi AM, Bakri MM, Ramanathan A (2018) Acute and sub-acute oral toxicity of Dracaena cinnabari resin methanol extract in rats. BMC Complement Altern Med 18(1):1–14
AI-Atroshi C, Rene Beulah J, Singamaneni KK, Pretty Diana Cyril C, Neelakandan S, Velmurugan S (2022) Automated speech-based evaluation of mild cognitive impairment and Alzheimer’s disease detection using with deep belief network model. Int J Healthc Manag. https://doi.org/10.1080/20479700.2022.2097764
Alexander GC, Karlawish J (2021) The problem of aducanumab for the treatment of Alzheimer disease. Ann Intern Med 174(9):1303–1304
Arbo BD, Andre-Miral C, Nasre-Nasser RG, Schimith LE, Santos MG, Costa-Silva D, Hort MA (2020) Resveratrol derivatives as potential treatments for Alzheimer’s and Parkinson’s disease. Front Aging Neurosci 12:103
Calvo-Rodriguez M, Bacskai BJ (2021) Mitochondria and calcium in Alzheimer’s disease: from cell signaling to neuronal cell death. Trends Neurosci 44(2):136–151
Caruso G, Godos J, Privitera A, Lanza G, Castellano S, Chillemi A, Grosso G (2022) Phenolic acids and prevention of cognitive decline: polyphenols with a neuroprotective role in cognitive disorders and Alzheimer’s disease. Nutrients 14(4):819
Chu Q, Zhu Y, Cao T, Zhang Y, Chang Z, Liu Y, Zhang Y (2020) Studies on the neuroprotection of osthole on glutamate-induced apoptotic cells and an Alzheimer’s disease mouse model via modulation oxidative stress. Appl Biochem Biotechnol 190(2):634–644
El-Ganainy SO, Gowayed MA, Agami M, Mohamed P, Belal M, Farid RM, Hanafy AS (2021) Galantamine nanoparticles outperform oral galantamine in an Alzheimer’s rat model: pharmacokinetics and pharmacodynamics. Nanomedicine 16(15):1281–1296
Folch J, Petrov D, Ettcheto M, Abad S, Sánchez-Lopez E, Garcia ML, Camins A (2016) Current research therapeutic strategies for Alzheimer’s disease treatment. Neural Plast 2016:1–15
Franchini S, Linciano P, Puja G, Tait A, Borsari C, Denora N, Sorbi C (2020) Novel dithiolane-based ligands combining sigma and NMDA receptor interactions as potential neuroprotective agents. ACS Med Chem Lett 11(5):1028–1034
Gomes LM, Bataglioli JC, Storr T (2020) Metal complexes that bind to the amyloid-β peptide of relevance to Alzheimer’s disease. Coord Chem Rev 412:213255
Good PF, Werner P, Hsu A, Olanow CW, Perl DP (1996) Evidence of neuronal oxidative damage in Alzheimer’s disease. Am J Pathol 149(1):21
Gul R, Jan H, Lalay G, Andleeb A, Usman H, Zainab R, Abbasi BH (2021) Medicinal plants and biogenic metal oxide nanoparticles: a paradigm shift to treat Alzheimer’s disease. Coatings 11(6):717
Hu KW, Fan HF, Lin HC, Huang JW, Chen YC, Shen CL, Tu LH (2021) Exploring the impact of glyoxal glycation on β-amyloid peptide (Aβ) aggregation in Alzheimer’s disease. J Phys Chem B 125(21):5559–5571
Jeyakumar M, Sathya S, Gandhi S, Tharra P, Suryanarayanan V, Singh SK, Devi KP (2019) α-bisabolol β-D-fucopyranoside as a potential modulator of β-amyloid peptide induced neurotoxicity: an in vitro & in silico study. Bioorg Chem 88:102935
Jeyakumar M, Sathya S, Gandhi S, Tharra P, Aarthy M, Balan DJ, Devi KP (2022) α-bisabolol β-D-fucopyranoside inhibits β-amyloid (Aβ) 25–35 induced oxidative stress in Neuro-2a cells via antioxidant approaches. Process Biochem 121:493–503
Karimi SA, Noorbakhsh M, Komaki H, Reza Nikoo M, Hasanein P, Shahidi S, Komaki A (2022) The interactive effects of verapamil and CB1 cannabinoid receptor antagonist/inverse agonist, AM251 on passive avoidance learning and memory in rat. Behav Pharmacol 33(2–3):222–229
Lao K, Ji N, Zhang X, Qiao W, Tang Z, Gou X (2019) Drug development for Alzheimer’s disease. J Drug Target 27(2):164–173
Long JM, Holtzman DM (2019) Alzheimer disease: an update on pathobiology and treatment strategies. Cell 179(2):312–339
Majdi A, Sadigh-Eteghad S, Aghsan SR, Farajdokht F, Vatandoust SM, Namvaran A, Mahmoudi J (2020) Amyloid-β, tau, and the cholinergic system in Alzheimer’s disease: seeking direction in a tangle of clues. Rev Neurosci 31(4):391–413
Matuszyk MM, Garwood CJ, Ferraiuolo L, Simpson JE, Staniforth RA, Wharton SB (2022) Biological and methodological complexities of beta-amyloid peptide: implications for Alzheimer’s disease research. J Neurochem 160(4):434–453
Michaels TC, Saric A, Curk S, Bernfur K, Arosio P, Meisl G, Knowles TP (2020) Dynamics of oligomer populations formed during the aggregation of Alzheimer’s Aβ42 peptide. Nat Chem 12(5):445–451
Misrani A, Tabassum S, Yang L (2021) Mitochondrial dysfunction and oxidative stress in Alzheimer’s disease. Front Aging Neurosci 13:617588
Nguyen K, Hoffman H, Chakkamparambil B, Grossberg GT (2021) Evaluation of rivastigmine in Alzheimer’s disease. Neurodegener Dis Manag 11(1):35–48
Nirale P, Paul A, Yadav KS (2020) Nanoemulsions for targeting the neurodegenerative diseases: Alzheimer’s, Parkinson’s and Prion’s. Life Sci 245:117394
Okello EJ, Mather J (2020) Comparative kinetics of acetyl-and butyryl-cholinesterase inhibition by green tea catechins| relevance to the symptomatic treatment of Alzheimer’s disease. Nutrients 12(4):1090
Ovais M, Zia N, Ahmad I, Khalil AT, Raza A, Ayaz M, Shinwari ZK (2018) Phyto-therapeutic and nanomedicinal approaches to cure Alzheimer’s disease: present status and future opportunities. Front Aging Neurosci 10:284
Pei X, Hu F, Luo F, Huang X, Li X, Xing S, Long D (2022) The neuroprotective effects of alpha-lipoic acid on an experimental model of Alzheimer’s disease in PC12 cells. J Appl Toxicol 42(2):285–294
Peng Y, Tao H, Wang S, Xiao J, Wang Y, Su H (2021) Dietary intervention with edible medicinal plants and derived products for prevention of Alzheimer’s disease: a compendium of time-tested strategy. J Funct Foods 81:104463
Piemontese L, Tomas D, Hiremathad A, Capriati V, Candeias E, Cardoso SM, Santos MA (2018) Donepezil structure-based hybrids as potential multifunctional anti-Alzheimer’s drug candidates. J Enzyme Inhib Med Chem 33(1):1212–1224
Prabhu R, Anjali R, Archunan G, Prabhu NM, Pugazhendhi A, Suganthy N (2019) Ecofriendly one pot fabrication of methyl gallate@ ZIF-L nanoscale hybrid as pH responsive drug delivery system for lung cancer therapy. Process Biochem 84:39–52
Raju P, Natarajan S (2021) Anticancer, anti-biofilm and antimicrobial activity of fucoidan-loaded zeolitic imidazole framework fabricated by one-pot synthesis method. Appl Nanosci 13:1919–1937
Raju P, Arivalagan P, Natarajan S (2020) One-pot fabrication of multifunctional catechin@ ZIF-L nanocomposite: Assessment of antibiofilm, larvicidal and photocatalytic activities. J Photochem Photobiol B 203:111774
Raju P, Balakrishnan K, Mishra M, Ramasamy T, Natarajan S (2022) Fabrication of pH responsive FU@ Eu-MOF nanoscale metal organic frameworks for lung cancer therapy. J Drug Deliv Sci Technol 70:103223
Roy J, Tsui KC, Ng J, Fung ML, Lim LW (2021) Regulation of Melatonin and Neurotransmission in Alzheimer’s Disease. Int J Mol Sci 22(13):6841
Sinha K, Sun C, Kamari R, Bettermann K (2020) Current status and future prospects of pathophysiology-based neuroprotective drugs for the treatment of vascular dementia. Drug Discov Today 25(4):793–799
Stanciu GD, Luca A, Rusu RN, Bild V, Beschea Chiriac SI, Solcan C, Ababei DC (2019) Alzheimer’s disease pharmacotherapy in relation to cholinergic system involvement. Biomolecules 10(1):40
Sun Y, Kakinen A, Wan X, Moriarty N, Hunt CP, Li Y, Ding F (2021) Spontaneous formation of β-sheet nano-barrels during the early aggregation of Alzheimer’s amyloid beta. Nano Today 38:101125
Tan SJ, Ismail IS (2020) Potency of selected berries, grapes, and citrus fruit as neuroprotective agents. Evid Based Complement Altern Med 2020:1
Terao I, Honyashiki M, Inoue T (2022) Comparative efficacy of lithium and aducanumab for cognitive decline in patients with mild cognitive impairment or Alzheimer’s disease: a systematic review and network meta-analysis. Ageing Res Rev 81:101709
Thakur A, Chun YS, October N, Yang HO, Maharaj V (2019) Potential of South African medicinal plants targeting the reduction of Aβ42 protein as a treatment of Alzheimer’s disease. J Ethnopharmacol 231:363–373
Thoe ES, Fauzi A, Tang YQ, Chamyuang S, Chia AYY (2021) A review on advances of treatment modalities for Alzheimer’s disease. Life Sci 276:119129
Tripathi SS, Singh S, Garg G, Kumar R, Verma AK, Singh AK, Rizvi SI (2022) Metformin ameliorates acetaminophen-induced sub-acute toxicity via antioxidant property. Drug Chem Toxicol 45(1):52–60
Wang Q, Yu X, Li L, Zheng J (2014) Inhibition of amyloid-β aggregation in Alzheimer’s disease. Curr Pharm Des 20(8):1223–1243
Wang CF, Song CY, Wang X, Huang LY, Ding M, Yang H, Bi JZ (2019) Protective effects of melatonin on mitochondrial biogenesis and mitochondrial structure and function in the HEK293-APPswe cell model of Alzheimer’s disease. Eur Rev Med Pharmacol Sci 23(8):3542–3550
Wong KH, Riaz MK, Xie Y, Zhang X, Liu Q, Chen H, Yang Z (2019) Review of current strategies for delivering Alzheimer’s disease drugs across the blood-brain barrier. Int J Mol Sci 20(2):381
Yan Y, Yang H, Xie Y, Ding Y, Kong D, Yu H (2020) Research progress on Alzheimer’s disease and resveratrol. Neurochem Res 45(5):989–1006
Yiannopoulou KG, Papageorgiou SG (2020) Current and future treatments in Alzheimer disease: an update. J Cent Nerv Syst Dis 12:1179573520907397
Yu N, Huang Y, Jiang Y, Zou L, Liu X, Liu S, Zhu Y (2020) Ganoderma lucidum triterpenoids (GLTs) reduce neuronal apoptosis via inhibition of ROCK signal pathway in APP/PS1 transgenic Alzheimer’s disease mice. Oxid Med Cell Longev 2020:1–11
Zhang X, Fu Z, Meng L, He M, Zhang Z (2018) The early events that initiate β-amyloid aggregation in Alzheimer’s disease. Front Aging Neurosci 10:359
Zhang Y, Ding C, Li C, Wang X (2021) Advances in fluorescent probes for detection and imaging of amyloid-β peptides in Alzheimer’s disease. Adv Clin Chem 103:135–190
Zhao J, Xu N, Yang X, Ling G, Zhang P (2022) The roles of gold nanoparticles in the detection of amyloid-β peptide for Alzheimer’s disease. Coll Interface Sci Commun 46:100579
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
All authors contributed to the present study conception and design. YZ and ZW—materials preparation and analysis. CG and LZ—formal analysis and data interpretation and RS—manuscript draft, Reviewing and supervision. All authors read and approved the final version of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, Y., Wang, Z., Gao, C. et al. Oxymatrine-mediated prevention of amyloid β-peptide-induced apoptosis on Alzheimer’s model PC12 cells: in vitro cell culture studies and in vivo cognitive assessment in rats. Inflammopharmacol 31, 2685–2699 (2023). https://doi.org/10.1007/s10787-023-01291-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-023-01291-0