Abstract
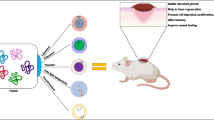
Several species of the genus Ocotea are used in traditional medicine due to their anti-inflammatory and analgesic properties. In this work we sought to investigate the effects of biseugenol, the main component of the hexane extract from the leaves of Ocotea cymbarum (Lauraceae), during a chronic inflammatory process induced by polyester-polyurethane sponge in mice. In addition to the inflammatory component, sponge discs also allowed us to evaluate parameters associated with the formation of new blood vessels and the deposition and organization of the extracellular matrix, processes that are related to the chronification of the inflammatory response. Daily treatment with biseugenol (0.1, 1 or 10 µg in 10 µl of 0.5% DMSO) inhibited the synthesis of inflammatory cytokines (TNF-α, CXCL-1 and CCL2) and the neutrophil and macrophage infiltrate into to the implants, indirectly evaluated by the activity of myeloperoxidase and N-acetyl-β-d-glycosaminidase enzymes, respectively. In implants treated with biseugenol, we observed a reduction in angiogenesis, assessed through histological quantification of mean number of blood vessels, the levels of the pro-angiogenic cytokines FGF and VEGF and the activity of metalloproteinases. Except for VEGF levels, all mentioned parameters showed significant reductions after treatment with biseugenol. Finally, the administration of the compound also reduced TGF-β1 levels, collagen synthesis and deposition, in addition to modifying the organization of the newly formed matrix, presenting a potential anti-fibrotic effect. Therefore, our results demonstrate the potential therapeutic use of biseugenol for the treatment of a series of pathological conditions, where parameters associated with inflammation, angiogenesis and fibrogenesis are deregulated.








Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Andrade SP, Ferreira MAND (2016) The sponge implant model of angiogenesis. pp 333–343
Barcelos LS, Talvani A, Teixeira AS et al (2005) Impaired inflammatory angiogenesis, but not leukocyte influx, in mice lacking TNFR1. J Leukoc Biol 78:352–358. https://doi.org/10.1189/jlb.1104682
Beirith A, Santos ARS, Calixto JB et al (1999) Study of the antinociceptive action of the ethanolic extract and the triterpene 24-hydroxytormentic acid isolated from the stem bark of Ocotea suaveolens. Planta Med 65:050–055. https://doi.org/10.1055/s-1999-13962
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473:298–307. https://doi.org/10.1038/nature10144
Cheresh P, Kim S-J, Tulasiram S, Kamp DW (2013) Oxidative stress and pulmonary fibrosis. Biochim Biophys Acta Mol Basis Dis 1832:1028–1040. https://doi.org/10.1016/j.bbadis.2012.11.021
Coussens LM, Werb Z (2002) Inflammation and cancer. Nature 420:860–867. https://doi.org/10.1038/nature01322
Cross MJ, Claesson-Welsh L (2001) FGF and VEGF function in angiogenesis: signalling pathways, biological responses and therapeutic inhibition. Trends Pharmacol Sci 22:201–207. https://doi.org/10.1016/S0165-6147(00)01676-X
Cui N, Hu M, Khalil RA (2017) Biochemical and biological attributes of matrix metalloproteinases. pp 1–73
Duran CL, Howell DW, Dave JM, et al (2017) Molecular regulation of sprouting angiogenesis. In: comprehensive physiology. Wiley, pp 153–235
Eming SA, Wynn TA, Martin P (2017) Inflammation and metabolism in tissue repair and regeneration. Science (80- ) 356:1026–1030. https://doi.org/10.1126/science.aam7928
Euler M, Hoffmann MH (2019) The double-edged role of neutrophil extracellular traps in inflammation. Biochem Soc Trans 47:1921–1930. https://doi.org/10.1042/BST20190629
Fathy M, Okabe M, Saad Eldien HM, Yoshida T (2020) AT-MSCs antifibrotic activity is improved by eugenol through modulation of TGF-β/Smad signaling pathway in rats. Molecules 25:348. https://doi.org/10.3390/molecules25020348
Ferreira BA, Silva RF, de Moura FBR et al (2021) α-zingiberene, a sesquiterpene from essential oil from leaves of Casearia sylvestris, suppresses inflammatory angiogenesis and stimulates collagen deposition in subcutaneous implants in mice. Nat Prod Res. https://doi.org/10.1080/14786419.2021.2019729
Folkman J (2006) Angiogenesis. Annu Rev Med 57:1–18. https://doi.org/10.1146/annurev.med.57.121304.131306
Fournet A, Ferreira ME, Rojas de Arias A et al (2007) Phytochemical and antiprotozoal activity of Ocotea lancifolia. Fitoterapia 78:382–384. https://doi.org/10.1016/j.fitote.2007.03.003
Furman D, Campisi J, Verdin E et al (2019) Chronic inflammation in the etiology of disease across the life span. Nat Med 25:1822–1832. https://doi.org/10.1038/s41591-019-0675-0
Golia E, Limongelli G, Natale F et al (2014) Inflammation and cardiovascular disease: from pathogenesis to therapeutic target. Curr Atheroscler Rep 16:435. https://doi.org/10.1007/s11883-014-0435-z
Grecco SS, Costa-Silva TA, Jerz G et al (2017) Antitrypanosomal activity and evaluation of the mechanism of action of dehydrodieugenol isolated from Nectandra leucantha (Lauraceae) and its methylated derivative against Trypanosoma cruzi. Phytomedicine 24:62–67. https://doi.org/10.1016/j.phymed.2016.11.015
Hu H-H, Chen D-Q, Wang Y-N et al (2018) New insights into TGF-β/Smad signaling in tissue fibrosis. Chem Biol Interact 292:76–83. https://doi.org/10.1016/j.cbi.2018.07.008
Junqueira LCU, Bignolas G, Brentani RR (1979) Picrosirius staining plus polarization microscopy, a specific method for collagen detection in tissue sections. Histochem J 11:447–455. https://doi.org/10.1007/BF01002772
Karsdal MA, Nielsen SH, Leeming DJ et al (2017) The good and the bad collagens of fibrosis—their role in signaling and organ function. Adv Drug Deliv Rev 121:43–56. https://doi.org/10.1016/j.addr.2017.07.014
Kim KM, Kim NS, Kim J et al (2013) Magnolol suppresses vascular endothelial growth factor-induced angiogenesis by inhibiting Ras-dependent mitogen-activated protein kinase and phosphatidylinositol 3-kinase/Akt signaling pathways. Nutr Cancer 65:1245–1253. https://doi.org/10.1080/01635581.2013.828082
Legler DF, Thelen M (2016) Chemokines: chemistry. Biochem Biol Funct Chim (aarau) 70:856. https://doi.org/10.2533/chimia.2016.856
Ley K, Hoffman HM, Kubes P et al (2018) Neutrophils: new insights and open questions. Sci Immunol. https://doi.org/10.1126/sciimmunol.aat4579
Li M, Hou Q, Zhong L et al (2021) Macrophage related chronic inflammation in non-healing wounds. Front Immunol. https://doi.org/10.3389/fimmu.2021.681710
Libby P (2008) Inflammatory mechanisms: the molecular basis of inflammation and disease. Nutr Rev 65:S140–S146. https://doi.org/10.1111/j.1753-4887.2007.tb00352.x
Manikandan P, Murugan RS, Priyadarsini RV et al (2010) Eugenol induces apoptosis and inhibits invasion and angiogenesis in a rat model of gastric carcinogenesis induced by MNNG. Life Sci 86:936–941. https://doi.org/10.1016/j.lfs.2010.04.010
Marcos-Ramiro B, García-Weber D, Millán J (2014) TNF-induced endothelial barrier disruption: beyond actin and Rho. Thromb Haemost 112:1088–1102. https://doi.org/10.1160/th14-04-0299
Medzhitov R (2008) Origin and physiological roles of inflammation. Nature 454:428–435. https://doi.org/10.1038/nature07201
Medzhitov R (2010) Inflammation 2010: new adventures of an old flame. Cell 140:771–776. https://doi.org/10.1016/j.cell.2010.03.006
Morikawa M, Derynck R, Miyazono K (2016) TGF-β and the TGF-β family: context-dependent roles in cell and tissue physiology. Cold Spring Harb Perspect Biol 8:a021873. https://doi.org/10.1101/cshperspect.a021873
Murakami Y, Shoji M, Hanazawa S et al (2003) Preventive effect of bis-eugenol, a eugenol ortho dimer, on lipopolysaccharide-stimulated nuclear factor kappa B activation and inflammatory cytokine expression in macrophages. Biochem Pharmacol 66:1061–1066. https://doi.org/10.1016/S0006-2952(03)00419-2
Newman DJ, Cragg GM (2020) Natural products as sources of new drugs over the nearly four decades from 01/1981 to 09/2019. J Nat Prod 83:770–803. https://doi.org/10.1021/acs.jnatprod.9b01285
Niazi A, Kourkinejad Gharaei F, Saebinasab Z et al (2021) Eugenol administration improves liver damage induced by a fructose-rich diet. Adv Biomed Res 10:42. https://doi.org/10.4103/abr.abr_237_20
Page-McCaw A, Ewald AJ, Werb Z (2007) Matrix metalloproteinases and the regulation of tissue remodelling. Nat Rev Mol Cell Biol 8:221–233. https://doi.org/10.1038/nrm2125
Ponci V, Silva RC, Santana FPR et al (2020) Biseugenol exhibited anti-inflammatory and anti-asthmatic effects in an asthma mouse model of mixed-granulocytic asthma. Molecules 25:5384. https://doi.org/10.3390/molecules25225384
Prudovsky I (2021) Cellular mechanisms of FGF-stimulated tissue repair. Cells 10:1830. https://doi.org/10.3390/cells10071830
Pulivendala G, Bale S, Godugu C (2020) Honokiol: a polyphenol neolignan ameliorates pulmonary fibrosis by inhibiting TGF-β/Smad signaling, matrix proteins and IL-6/CD44/STAT3 axis both in vitro and in vivo. Toxicol Appl Pharmacol 391:114913. https://doi.org/10.1016/j.taap.2020.114913
Purnomo Y, Piccart Y, Coenen T et al (2013) Oxidative stress and transforming growth factor-.β1-induced cardiac fibrosis. Cardiovasc Hematol Disord Targets 13:165–172. https://doi.org/10.2174/1871529X11313020010
Rajarathnam K, Schnoor M, Richardson RM, Rajagopal S (2019) How do chemokines navigate neutrophils to the target site: dissecting the structural mechanisms and signaling pathways. Cell Signal 54:69–80. https://doi.org/10.1016/j.cellsig.2018.11.004
Ramani T, Auletta CS, Weinstock D et al (2015) Cytokines. Int J Toxicol 34:355–365. https://doi.org/10.1177/1091581815584918
Ribeiro VP, Arruda C, Abd El-Salam M, Bastos JK (2018) Brazilian medicinal plants with corroborated anti-inflammatory activities: a review. Pharm Biol 56:253–268. https://doi.org/10.1080/13880209.2018.1454480
Roderfeld M (2018) Matrix metalloproteinase functions in hepatic injury and fibrosis. Matrix Biol 68–69:452–462. https://doi.org/10.1016/j.matbio.2017.11.011
Silva SA, Gobbo MG, Pinto-Fochi ME et al (2015) Prostate hyperplasia caused by long-term obesity is characterized by high deposition of extracellular matrix and increased content of MMP-9 and VEGF. Int J Exp Pathol 96:21–30. https://doi.org/10.1111/iep.12107
Soehnlein O, Steffens S, Hidalgo A, Weber C (2017) Neutrophils as protagonists and targets in chronic inflammation. Nat Rev Immunol 17:248–261. https://doi.org/10.1038/nri.2017.10
Souza RAC, Ferreira BA, de Moura FBR et al (2020) Dehydrodieugenol B and hexane extract from Endlicheria paniculata regulate inflammation, angiogenesis, and collagen deposition induced by a murine sponge model. Fitoterapia 147:104767. https://doi.org/10.1016/j.fitote.2020.104767
Stephenson J, Nutma E, van der Valk P, Amor S (2018) Inflammation in CNS neurodegenerative diseases. Immunology 154:204–219. https://doi.org/10.1111/imm.12922
Varfolomeev E, Vucic D (2018) Intracellular regulation of TNF activity in health and disease. Cytokine 101:26–32. https://doi.org/10.1016/j.cyto.2016.08.035
Wang X, Khalil RA (2018) Matrix metalloproteinases, vascular remodeling, and vascular disease. pp 241–330
Weiskirchen R, Weiskirchen S, Tacke F (2019) Organ and tissue fibrosis: molecular signals, cellular mechanisms and translational implications. Mol Aspects Med 65:2–15. https://doi.org/10.1016/j.mam.2018.06.003
Wynn TA, Ramalingam TR (2012) Mechanisms of fibrosis: therapeutic translation for fibrotic disease. Nat Med 18:1028–1040. https://doi.org/10.1038/nm.2807
Zhao R, Liang H, Clarke E et al (2016) Inflammation in chronic wounds. Int J Mol Sci 17:2085. https://doi.org/10.3390/ijms17122085
Zschocke S, Drewes S, Paulus K et al (2000) Analytical and pharmacological investigation of Ocotea bullata (black stinkwood) bark and leaves. J Ethnopharmacol 71:219–230. https://doi.org/10.1016/S0378-8741(00)00159-8
Acknowledgements
Authors thank the Rede de Biotérios de Roedores from the Federal University of Uberlândia (REBIR/UFU).
Funding
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico—CNPq (446480/2014-2; 301354-2019-7 and 150814/2021-6), Fundação de Amparo à Pesquisa de Minas Gerais—FAPEMIG (APQ-04436-10 and APQ-02238-14), Instituto Nacional de Ciência e Tecnologia—INCT/NanoBiofar, Fundação de Amparo à Pesquisa do Estado de São Paulo—FAPESP (2021/02789-7), and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior—CAPES (financial code 001).
Author information
Authors and Affiliations
Contributions
BAF: Conceptualization, methodology, formal analysis, investigation, writing-original draft preparation. FBRM: Methodology, formal analysis, investigation. KSG: Methodology, formal analysis, investigation. DCSS: Methodology, formal analysis, investigation. JHGL: Conceptualization, supervision, writing—review & editing, funding acquisition, project administration. FAA: Conceptualization, supervision, writing—review & editing, funding acquisition, project administration.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that there are no known conflicts of interest associated with this publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ferreira, B.A., de Moura, F.B.R., Gomes, K.S. et al. Biseugenol from Ocotea cymbarum (Lauraceae) attenuates inflammation, angiogenesis and collagen deposition of sponge-induced fibrovascular tissue in mice. Inflammopharmacol 31, 1539–1549 (2023). https://doi.org/10.1007/s10787-023-01210-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-023-01210-3