Abstract
Objective
To investigate whether glucocorticoids, the hallmark medication for systemic lupus erythematosus (SLE), could prevent the development of neuropsychiatric SLE (NPSLE).
Methods
The protective effects of prednisone on NPSLE were tested using the open field, object recognition/placement, forced swim, tail suspension, and sucrose preference tests in MRL/lpr mice. Auto-antibody titres and the weight of lymph nodes were also measured.
Results
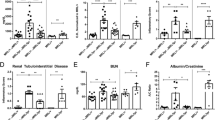
MRL/lpr mice exhibited mild depression at the age of 8 weeks before progressing with spatial cognitive impairment and severe depression-like behaviour at the age of 16 weeks. Treating MRL/lpr mice with prednisone (5 mg/kg) from the age of 8 weeks decreased anti-cardiolipin and anti-N-methyl-d-aspartate (NMDA) receptor antibody titres in the brain, reduced the weight of lymph nodes, and prolonged the floating latency in the forced swim test. However, prednisone (3 or 5 mg/kg) had no preventive effect on the development of spatial cognitive impairment and other depression-like behaviours in MRL/lpr mice. The dose of prednisone had a positive correlation with the floating latency in the forced swim test, while it offered no effects on all other behavioural tests.
Conclusion
Our results provide evidence that early treatment with prednisone had a limited effect on the development of neuropsychiatric symptoms in MRL/lpr mice. Further work is needed in other models beyond NPSLE in MRL/lpr mice before any definitive conclusions are made on the efficacy of prednisone in human NPSLE.






Similar content being viewed by others
Abbreviations
- ACA:
-
Anti-cardiolipin antibody
- ANOVA:
-
One-way analysis of variance
- Anti-NMDAR:
-
Anti-N-methyl-d-aspartate receptor
- ELISA:
-
Enzyme-linked immunosorbent assays
- EULAR:
-
European league against rheumatism
- i.g.:
-
Intragastrically
- LPR-8w:
-
8-Week-old MRL/lpr mice
- NPSLE:
-
Neuropsychiatric systemic lupus erythematosus
- NMDAR:
-
N-Methyl-D-aspartate receptor
- PRE:
-
Prednisone
- PRE-3 mg:
-
Prednisone at 3 mg/kg
- PRE-5 mg:
-
Prednisone at 5 mg/kg
- SLE:
-
Systemic lupus erythematosus
- WT:
-
Wild type
References
Beger E, Deocharan B, Edelman M, Erblich B, Gu Y, Putterman C (2002) A peptide DNA surrogate accelerates autoimmune manifestations and nephritis in lupus-prone mice. J Immunol 168(7):3617–3626. https://doi.org/10.4049/jimmunol.168.7.3617
Bennett SA, Roberts DC (2003) Analysis of protein expression in brain tissue by ELISA. Methods Mol Med 79:283–295
Bertsias GK, Ioannidis JP, Aringer M, Bollen E, Bombardieri S, Bruce IN et al (2010) EULAR recommendations for the management of systemic lupus erythematosus with neuropsychiatric manifestations: report of a task force of the EULAR standing committee for clinical affairs. Ann Rheum Dis 69(12):2074–2082. https://doi.org/10.1136/ard.2010.130476
Bhangle SD, Kramer N, Rosenstein ED (2013) Corticosteroid-induced neuropsychiatric disorders: review and contrast with neuropsychiatric lupus. Rheumatol Int 33(8):1923–1932. https://doi.org/10.1007/s00296-013-2750-z
Bonfa E, Golombek SJ, Kaufman LD, Skelly S, Weissbach H, Brot N et al (1987) Association between lupus psychosis and anti-ribosomal p protein antibodies. N Engl J Med 317(5):265–271. https://doi.org/10.1056/Nejm198707303170503
Da Mesquita S, Louveau A, Vaccari A, Smirnov I, Cornelison RC, Kingsmore KM et al (2018) Functional aspects of meningeal lymphatics in ageing and Alzheimer’s disease. Nature 560(7717):185–191. https://doi.org/10.1038/s41586-018-0368-8
Dale RC, Gorman MP, Lim M (2017) Autoimmune encephalitis in children: clinical phenomenology, therapeutics, and emerging challenges. Curr Opin Neurol 30(3):334–344. https://doi.org/10.1097/WCO.0000000000000443
Denburg SD, Carbotte RM, Denburg JA (1994) Corticosteroids and neuropsychological functioning in patients with systemic lupus-erythematosus. Arthritis Rheum 37(9):1311–1320. https://doi.org/10.1002/art.1780370907
Ehrenreich H (2017) Autoantibodies against the N-methyl-d-aspartate receptor subunit NR1: untangling apparent inconsistencies for clinical practice. Front Immunol 8:181. https://doi.org/10.3389/fimmu.2017.00181
Gao HX, Campbell SR, Cui MH, Zong P, Hee-Hwang J, Gulinello M et al (2009) Depression is an early disease manifestation in lupus-prone MRL/lpr mice. J Neuroimmunol 207(1–2):45–56. https://doi.org/10.1016/j.jneuroim.2008.11.009
Govoni M, Bortoluzzi A, Padovan M, Silvagni E, Borrelli M, Donelli F et al (2016) The diagnosis and clinical management of the neuropsychiatric manifestations of lupus. J Autoimmun 74:41–72. https://doi.org/10.1016/j.jaut.2016.06.013
Hahn BH, McMahon MA, Wilkinson A, Wallace WD, Daikh DI, Fitzgerald JD et al (2012) American College of Rheumatology guidelines for screening, treatment, and management of lupus nephritis. Arthritis Care Res (Hoboken) 64(6):797–808. https://doi.org/10.1002/acr.21664
Hanly JG, Cassell K, Fisk JD (1997) Cognitive function in systemic lupus erythematosus: results of a 5-year prospective study. Arthritis Rheum 40(8):1542–1543. https://doi.org/10.1002/1529-0131(199708)40:8%3c1542:AID-ART26%3e3.0.CO;2-9
Ho RC, Thiaghu C, Ong H, Lu Y, Ho CS, Tam WW et al (2016) A meta-analysis of serum and cerebrospinal fluid autoantibodies in neuropsychiatric systemic lupus erythematosus. Autoimmun Rev 15(2):124–138. https://doi.org/10.1016/j.autrev.2015.10.003
Huang X, Magder LS, Petri M (2016) Predictors of incident seizure in systemic lupus erythematosus. J Rheumatol 43(3):565–575. https://doi.org/10.3899/jrheum.150135
Huang L, Xie D, Yu Y, Liu H, Shi Y, Shi T et al (2018) TCMID 2.0: a comprehensive resource for TCM. Nucleic Acids Res 46(D1):D1117–D1120. https://doi.org/10.1093/nar/gkx1028
Jeltsch-David H, Muller S (2014) Neuropsychiatric systemic lupus erythematosus and cognitive dysfunction: the MRL-lpr mouse strain as a model. Autoimmun Rev 13(9):963–973. https://doi.org/10.1016/j.autrev.2014.08.015
Jia C, Brown RW, Malone HM, Burgess KC, Gill WD, Keasey MP et al (2018) Ciliary neurotrophic factor is a key sex-specific regulator of depressive-like behavior in mice. Psychoneuroendocrinology 100:96–105. https://doi.org/10.1016/j.psyneuen.2018.09.038
Kabadi S, Yeaw J, Bacani AK, Tafesse E, Bos K, Karkare S et al (2018) Healthcare resource utilization and costs associated with long-term corticosteroid exposure in patients with systemic lupus erythematosus. Lupus 27(11):1799–1809. https://doi.org/10.1177/0961203318790675
Kapadia M, Bijelic D, Zhao H, Ma D, Stojanovich L, Milosevic M et al (2017) Effects of sustained i.c.v. infusion of lupus CSF and autoantibodies on behavioral phenotype and neuronal calcium signaling. Acta Neuropathol Commun 5(1):70. https://doi.org/10.1186/s40478-017-0473-1
Kaul A, Gordon C, Crow MK, Touma Z, Urowitz MB, van Vollenhoven R et al (2016) Systemic lupus erythematosus. Nat Rev Dis Primers 2:16039. https://doi.org/10.1038/nrdp.2016.39
Kozora E, Ellison MC, West S (2006) Depression, fatigue, and pain in systemic lupus erythematosus (SLE): relationship to the American College of Rheumatology SLE neuropsychological battery. Arthritis Rheum 55(4):628–635. https://doi.org/10.1002/art.22101
Kozora E, Arciniegas DB, Zhang L, West S (2007) Neuropsychological patterns in systemic lupus erythematosus patients with depression. Arthritis Res Ther 9(3):R48. https://doi.org/10.1186/ar2203
Lei HW, Wang JY, Dang QJ, Yang F, Liu X, Zhang JH et al (2017) Neuropsychiatric involvement in lupus is associated with the Nogo-a/NgR1 pathway. J Neuroimmunol 311:22–28. https://doi.org/10.1016/j.jneuroim.2017.06.008
Magro-Checa C, Zirkzee EJ, Huizinga TW, Steup-Beekman GM (2016) Management of neuropsychiatric systemic lupus erythematosus: current approaches and future perspectives. Drugs 76(4):459–483. https://doi.org/10.1007/s40265-015-0534-3
McLaurin EY, Holliday SL, Williams P, Brey RL (2005) Predictors of cognitive dysfunction in patients with systemic lupus erythematosus. Neurology 64(2):297–303. https://doi.org/10.1212/01.WNL.0000149640.78684.EA
Mike EV, Makinde HM, Der E, Stock A, Gulinello M, Gadhvi GT et al (2018) Neuropsychiatric systemic lupus erythematosus is dependent on sphingosine-1-phosphate signaling. Front Immunol. https://doi.org/10.3389/fimmu.2018.02189
Monahan RC, Beaart-van de Voorde LJJ, Steup-Beekman GM, Magro-Checa C, Huizinga TWJ, Hoekman J et al (2017) Neuropsychiatric symptoms in systemic lupus erythematosus: impact on quality of life. Lupus 26(12):1252–1259. https://doi.org/10.1177/0961203317694262
Nikpour M, Urowitz MB, Ibanez D, Gladman DD (2009) Frequency and determinants of flare and persistently active disease in systemic lupus erythematosus. Arthritis Rheum 61(9):1152–1158. https://doi.org/10.1002/art.24741
Pan H, Oliveira B, Saher G, Dere E, Tapken D, Mitjans M et al (2018) Uncoupling the widespread occurrence of anti-NMDAR1 autoantibodies from neuropsychiatric disease in a novel autoimmune model. Mol Psychiatry. https://doi.org/10.1038/s41380-017-0011-3
Porsolt RD, Bertin A, Jalfre M (1977) Behavioral despair in mice: a primary screening test for antidepressants. Arch Int Pharmacodyn Ther 229(2):327–336
Shimizu Y, Yasuda S, Kako Y, Nakagawa S, Kanda M, Hisada R et al (2016) Post-steroid neuropsychiatric manifestations are significantly more frequent in SLE compared with other systemic autoimmune diseases and predict better prognosis compared with de novo neuropsychiatric SLE. Autoimmun Rev 15(8):786–794. https://doi.org/10.1016/j.autrev.2016.03.017
Stock AD, Wen J, Doerner J, Herlitz LC, Gulinello M, Putterman C (2015) Neuropsychiatric systemic lupus erythematosus persists despite attenuation of systemic disease in MRL/lpr mice. J Neuroinflamm 12:205. https://doi.org/10.1186/s12974-015-0423-4
Toledano P, Sarbu N, Espinosa G, Bargallo N, Cervera R (2013) Neuropsychiatric systemic lupus erythematosus: magnetic resonance imaging findings and correlation with clinical and immunological features. Autoimmun Rev 12(12):1166–1170. https://doi.org/10.1016/j.autrev.2013.07.004
Trune DR, Kempton JB (2001) Aldosterone and prednisolone control of cochlear function in MRL/MpJ-Fas(lpr) autoimmune mice. Hear Res 155(1–2):9–20. https://doi.org/10.1016/S0378-5955(01)00240-4
Wen J, Chen CH, Stock A, Doerner J, Gulinello M, Putterman C (2016a) Intracerebroventricular administration of TNF-like weak inducer of apoptosis induces depression-like behavior and cognitive dysfunction in non-autoimmune mice. Brain Behav Immun 54:27–37. https://doi.org/10.1016/j.bbi.2015.12.017
Wen J, Doerner J, Chalmers S, Stock A, Wang H, Gullinello M et al (2016b) B cell and/or autoantibody deficiency do not prevent neuropsychiatric disease in murine systemic lupus erythematosus. J Neuroinflamm 13(1):73. https://doi.org/10.1186/s12974-016-0537-3
Wu XY, Yang M, Xie YS, Xiao WG, Lin J, Zhou B et al (2018) Causes of death in hospitalized patients with systemic lupus erythematosus: a 10-year multicenter nationwide Chinese cohort. Clin Rheumatol. https://doi.org/10.1007/s10067-018-4259-z
Xiong W, Lahita RG (2014) Pragmatic approaches to therapy for systemic lupus erythematosus. Nat Rev Rheumatol 10(2):97–107. https://doi.org/10.1038/nrrheum.2013.157
Xu Z, Wang Y, Chen B, Xu C, Wu X, Wang Y et al (2016) Entorhinal principal neurons mediate brain-stimulation treatments for epilepsy. EBioMedicine 14:148–160. https://doi.org/10.1016/j.ebiom.2016.11.027
Zhu TY, Tam LS, Lee VW, Lee KK, Li EK (2009) Systemic lupus erythematosus with neuropsychiatric manifestation incurs high disease costs: a cost-of-illness study in Hong Kong. Rheumatology (Oxford) 48(5):564–568. https://doi.org/10.1093/rheumatology/kep031
Acknowledgements
This work was funded by the Zhejiang TCM Science and Technology Plan (2018ZZ007), the National Natural Science Foundation of China (81673623), and partly the Foundation of the Zhejiang Chinese Medical University (ZYX2018002 and 2018ZG24). The authors thank the members of the Laboratory Animal Research Centre of Zhejiang Chinese Medical University for their excellent technical support. The authors also thank Dr. John Hugh Snyder and Dr. Anthony J. Filiano for editing our manuscript. Z. X. also would like to thank all members of Filiano Lab, Kurtzberg Lab and Marcus Centre for Cellular Cures (MC3) at Duke University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lu, F., Lu, H., Xie, M. et al. Limited preventive effect of prednisone on neuropsychiatric symptoms in murine systemic lupus erythematosus. Inflammopharmacol 27, 511–520 (2019). https://doi.org/10.1007/s10787-019-00587-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-019-00587-4