Abstract
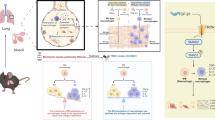
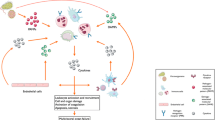
The role of programmed death ligand 1 (PD-L1) has been extensively investigated in adaptive immune system. However, increasing data show that innate immune responses are also affected by the immune checkpoint molecule. It has been demonstrated that regulation of PD-L1 signaling in macrophages may be a potential therapeutic method for acute respiratory distress syndrome (ARDS). However, the PD-L1 expression pattern in local macrophages and whole lung tissues remains mysterious, hindering optimization of the potential treatment program. Therefore, we aim to determine the PD-L1 expression pattern during ARDS. Our findings show that PD-L1 levels are markedly increased in lipopolysaccharide (LPS)-stimulated lung tissues, which might be attributable to an increase in the gene expression by immune cells, including macrophages and neutrophils. In vitro experiments are performed to explore the mechanism involved in LPS-induced PD-L1 production. We find that PD-L1 generation is controlled by transcription factors early growth response 1 (Egr-1) and CCAAT/enhancer binding protein delta (C/EBPδ). Strikingly, PD-L1 production is enhanced by phosphoinositide-3 kinase (PI3K)–protein kinase B (AKT) signaling pathway via up-regulation of Egr-1 and C/EBPδ expressions. Additionally, we observe that expressions of Egr-1 and C/EBPδ mutually reinforce each other. Moreover, we observe that PD-L1 is protective for ARDS due to its regulatory role in macrophage-associated inflammatory response. In summary, during LPS-induced ARDS, PD-L1 expression, which is beneficial for the disease, is increased via the PI3K-AKT1-Egr-1/C/EBPδ signaling pathway, providing theoretical basis for application of methods controlling PD-L1 signaling in macrophages for ARDS treatment in clinic.















Similar content being viewed by others
Data Availability
The data generated in the current study and material-related information are available from the authors on reasonable request.
References
Mowery, N.T., W.T.H. Terzian, and A.C. Nelson. 2020. Acute lung injury. Current Problems in Surgery 57: 100777.
Day, C.L., D.E. Kaufmann, P. Kiepiela, J.A. Brown, E.S. Moodley, S. Reddy, E.W. Mackey, J.D. Miller, A.J. Leslie, C. DePierres, Z. Mncube, J. Duraiswamy, B. Zhu, Q. Eichbaum, M. Altfeld, E.J. Wherry, H.M. Coovadia, P.J. Goulder, P. Klenerman, R. Ahmed, G.J. Freeman, and B.D. Walker. 2006. PD-1 expression on HIV-specific T cells is associated with T-cell exhaustion and disease progression. Nature 443: 350–354.
Fourcade, J., Z. Sun, M. Benallaoua, P. Guillaume, I.F. Luescher, C. Sander, J.M. Kirkwood, V. Kuchroo, and H.M. Zarour. 2010. Upregulation of Tim-3 and PD-1 expression is associated with tumor antigen-specific CD8+ T cell dysfunction in melanoma patients. Journal of Experimental Medicine 207: 2175–2186.
Wherry, E.J., S.J. Ha, S.M. Kaech, W.N. Haining, S. Sarkar, V. Kalia, S. Subramaniam, J.N. Blattman, D.L. Barber, and R. Ahmed. 2007. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity 27: 670–684.
Akbay, E.A., S. Koyama, J. Carretero, A. Altabef, J.H. Tchaicha, C.L. Christensen, O.R. Mikse, A.D. Cherniack, E.M. Beauchamp, T.J. Pugh, M.D. Wilkerson, P.E. Fecci, M. Butaney, J.B. Reibel, M. Soucheray, T.J. Cohoon, P.A. Janne, M. Meyerson, D.N. Hayes, G.I. Shapiro, T. Shimamura, L.M. Sholl, S.J. Rodig, G.J. Freeman, P.S. Hammerman, G. Dranoff, and K.K. Wong. 2013. Activation of the PD-1 pathway contributes to immune escape in EGFR-driven lung tumors. Cancer Discovery 3: 1355–1363.
Zajac, A.J., J.N. Blattman, K. Murali-Krishna, D.J. Sourdive, M. Suresh, J.D. Altman, and R. Ahmed. 1998. Viral immune evasion due to persistence of activated T cells without effector function. Journal of Experimental Medicine 188: 2205–2213.
Wang, F., X. Huang, C.S. Chung, Y. Chen, N.A. Hutchins, and A. Ayala. 2016. Contribution of programmed cell death receptor (PD)-1 to Kupffer cell dysfunction in murine polymicrobial sepsis. American Journal of Physiology. Gastrointestinal and Liver Physiology 311: G237–G245.
Jia, L., K. Liu, T. Fei, Q. Liu, X. Zhao, L. Hou, and W. Zhang. 2021. Programmed cell death-1/programmed cell death-ligand 1 inhibitors exert antiapoptosis and antiinflammatory activity in lipopolysaccharide stimulated murine alveolar macrophages. Experimental and Therapeutic Medicine 21: 400.
Xu, J., J.H. Wang, X.L. Wang, R.M. Tan, X.L. Qi, Z.J. Liu, H.P. Qu, T.T. Pan, Q.Y. Zhan, Y. Zuo, W. Yang, and J.L. Liu. 2020. Soluble PD-L1 improved direct ARDS by reducing monocyte-derived macrophages. Cell Death & Disease 11: 934.
Cerezo, M., R. Guemiri, S. Druillennec, I. Girault, H. Malka-Mahieu, S. Shen, D. Allard, S. Martineau, C. Welsch, S. Agoussi, C. Estrada, J. Adam, C. Libenciuc, E. Routier, S. Roy, L. Desaubry, A.M. Eggermont, N. Sonenberg, J.Y. Scoazec, A. Eychene, S. Vagner, and C. Robert. 2018. Translational control of tumor immune escape via the eIF4F-STAT1-PD-L1 axis in melanoma. Nature Medicine 24: 1877–1886.
Huang, G., Q. Wen, Y. Zhao, Q. Gao, and Y. Bai. 2013. NF-kappaB plays a key role in inducing CD274 expression in human monocytes after lipopolysaccharide treatment. PLoS ONE 8: e61602.
Barsoum, I.B., C.A. Smallwood, D.R. Siemens, and C.H. Graham. 2014. A mechanism of hypoxia-mediated escape from adaptive immunity in cancer cells. Cancer Research 74: 665–674.
Jiang, X., J. Zhou, A. Giobbie-Hurder, J. Wargo, and F.S. Hodi. 2013. The activation of MAPK in melanoma cells resistant to BRAF inhibition promotes PD-L1 expression that is reversible by MEK and PI3K inhibition. Clinical Cancer Research 19: 598–609.
Bu, L.L., G.T. Yu, L. Wu, L. Mao, W.W. Deng, J.F. Liu, A.B. Kulkarni, W.F. Zhang, L. Zhang, and Z.J. Sun. 2017. STAT3 induces immunosuppression by upregulating PD-1/PD-L1 in HNSCC. Journal of Dental Research 96: 1027–1034.
Yan, C., P.F. Johnson, H. Tang, Y. Ye, M. Wu, and H. Gao. 2013. CCAAT/enhancer-binding protein delta is a critical mediator of lipopolysaccharide-induced acute lung injury. American Journal of Pathology 182: 420–430.
Yan, C., F. Guan, Y. Shen, H. Tang, D. Yuan, H. Gao, and X. Feng. 2016. Bigelovii A protects against lipopolysaccharide-induced acute lung injury by blocking NF-kappaB and CCAAT/enhancer-binding protein delta pathways. Mediators of Inflammation 2016: 9201604.
Gao, H.W., R.F. Guo, C.L. Speyer, J. Reuben, T.A. Neff, L.M. Hoesel, N.C. Riedemann, S.A. McClintock, J.V. Sarma, N. Van Rooijen, F.S. Zetoune, and P.A. Ward. 2004. Stat3 activation in acute lung injury. Journal of Immunology 172: 7703–7712.
Lim, D., W. Kim, C. Lee, H. Bae, and J. Kim. 2018. Macrophage depletion protects against cigarette smoke-induced inflammatory response in the mouse colon and lung. Frontiers in Physiology 9: 47.
Misharin, A.V., L. Morales-Nebreda, G.M. Mutlu, G.R. Budinger, and H. Perlman. 2013. Flow cytometric analysis of macrophages and dendritic cell subsets in the mouse lung. American Journal of Respiratory Cell and Molecular Biology 49: 503–510.
Zhang, X., R. Goncalves, and D.M. Mosser. 2008. The isolation and characterization of murine macrophages. Current Protocols in Immunology 14: 14.1.1–14.1.14.
Yan, C., C. Deng, X. Liu, Y. Chen, J. Ye, R. Cai, Y. Shen, and H. Tang. 2018. TNF-alpha induction of IL-6 in alveolar type II epithelial cells: Contributions of JNK/c-Jun/AP-1 element, C/EBPdelta/C/EBP binding site and IKK/NF-kappaB p65/kappaB site. Molecular Immunology 101: 585–596.
Yan, C., M. Zhu, J. Staiger, P.F. Johnson, and H. Gao. 2012. C5a-regulated CCAAT/enhancer-binding proteins beta and delta are essential in Fcgamma receptor-mediated inflammatory cytokine and chemokine production in macrophages. Journal of Biological Chemistry 287: 3217–3230.
Yan, C., J. Chen, Y. Ding, Z. Zhou, B. Li, C. Deng, D. Yuan, Q. Zhang, and X. Wang. 2021. The crucial role of PPARgamma-Egr-1-pro-inflammatory mediators axis in IgG immune complex-induced acute lung injury. Frontiers in Immunology 12: 634889.
Muthumani, K., D.J. Shedlock, D.K. Choo, P. Fagone, O.U. Kawalekar, J. Goodman, C.B. Bian, A.A. Ramanathan, P. Atman, P. Tebas, M.A. Chattergoon, A.Y. Choo, and D.B. Weiner. 2011. HIV-mediated phosphatidylinositol 3-kinase/serine-threonine kinase activation in APCs leads to programmed death-1 ligand upregulation and suppression of HIV-specific CD8 T cells. The Journal of Immunology 187: 2932–2943.
Shao, R., Y. Fang, H. Yu, L. Zhao, Z. Jiang, and C.S. Li. 2016. Monocyte programmed death ligand-1 expression after 3–4 days of sepsis is associated with risk stratification and mortality in septic patients: A prospective cohort study. Critical Care 20: 124.
Venet, F., and G. Monneret. 2018. Advances in the understanding and treatment of sepsis-induced immunosuppression. Nature Reviews. Nephrology 14: 121–137.
Tsai, J.C., L. Liu, B.C. Cooley, M.R. DiChiara, J.N. Topper, and W.C. Aird. 2000. The Egr-1 promoter contains information for constitutive and inducible expression in transgenic mice. The FASEB Journal 14: 1870–1872.
Leyva-Illades, D., R.P. Cherla, C.L. Galindo, A.K. Chopra, and V.L. Tesh. 2010. Global transcriptional response of macrophage-like THP-1 cells to Shiga toxin type 1. Infection and Immunity 78: 2454–2465.
Thiel, G., and G. Cibelli. 2002. Regulation of life and death by the zinc finger transcription factor Egr-1. Journal of Cellular Physiology 193: 287–292.
Min, I.M., G. Pietramaggiori, F.S. Kim, E. Passegue, K.E. Stevenson, and A.J. Wagers. 2008. The transcription factor EGR1 controls both the proliferation and localization of hematopoietic stem cells. Cell Stem Cell 2: 380–391.
Dinkel, A., K. Warnatz, B. Ledermann, A. Rolink, P.F. Zipfel, K. Burki, and H. Eibel. 1998. The transcription factor early growth response 1 (Egr-1) advances differentiation of pre-B and immature B cells. Journal of Experimental Medicine 188: 2215–2224.
Pignatelli, M., R. Luna-Medina, A. Perez-Rendon, A. Santos, and A. Perez-Castillo. 2003. The transcription factor early growth response factor-1 (EGR-1) promotes apoptosis of neuroblastoma cells. The Biochemical Journal 373: 739–746.
Pang, Z., R. Raudonis, C. McCormick, and Z. Cheng. 2019. Early Growth Response 1 Deficiency Protects the Host against Pseudomonas aeruginosa Lung Infection. Infection and Immunity 88: e00678–19.
Reynolds, P.R., M.G. Cosio, and J.R. Hoidal. 2006. Cigarette smoke-induced Egr-1 upregulates proinflammatory cytokines in pulmonary epithelial cells. American Journal of Respiratory Cell and Molecular Biology 35: 314–319.
Chu, L., T. Wang, Y. Hu, Y. Gu, Z. Su, and H. Jiang. 2013. Activation of Egr-1 in human lung epithelial cells exposed to silica through MAPKs signaling pathways. PLoS ONE 8: e68943.
Cho, S.J., M.J. Kang, R.J. Homer, H.R. Kang, X. Zhang, P.J. Lee, J.A. Elias, and C.G. Lee. 2006. Role of early growth response-1 (Egr-1) in interleukin-13-induced inflammation and remodeling. Journal of Biological Chemistry 281: 8161–8168.
Russo, M.W., B.R. Sevetson, and J. Milbrandt. 1995. Identification of NAB1, a repressor of NGFI-A- and Krox20-mediated transcription. Proceedings of the National Academy of Sciences USA 92: 6873–6877.
Qu, Z., L.A. Wolfraim, J. Svaren, M.U. Ehrengruber, N. Davidson, and J. Milbrandt. 1998. The transcriptional corepressor NAB2 inhibits NGF-induced differentiation of PC12 cells. Journal of Cell Biology 142: 1075–1082.
Cantwell, C.A., E. Sterneck, and P.F. Johnson. 1998. Interleukin-6-specific activation of the C/EBPdelta gene in hepatocytes is mediated by Stat3 and Sp1. Molecular and Cellular Biology 18: 2108–2117.
Carpenter, C.L., B.C. Duckworth, K.R. Auger, B. Cohen, B.S. Schaffhausen, and L.C. Cantley. 1990. Purification and characterization of phosphoinositide 3-kinase from rat liver. Journal of Biological Chemistry 265: 19704–19711.
Cantley, L.C. 2002. The phosphoinositide 3-kinase pathway. Science 296: 1655–1657.
Datler, H., A. Vogel, M. Kerndl, C. Baumgartinger, L. Musiejovsky, N. Makivic, S. Frech, B. Niederreiter, T. Haider, M. Puhringer, J.S. Brunner, O. Sharif, and G. Schabbauer. 2019. PI3K activity in dendritic cells exerts paradoxical effects during autoimmune inflammation. Molecular Immunology 111: 32–42.
Diaz-Guerra, M.J., A. Castrillo, P. Martin-Sanz, and L. Bosca. 1999. Negative regulation by phosphatidylinositol 3-kinase of inducible nitric oxide synthase expression in macrophages. The Journal of Immunology 162: 6184–6190.
Lee, J.S., W.M. Nauseef, A. Moeenrezakhanlou, L.M. Sly, S. Noubir, K.G. Leidal, J.M. Schlomann, G. Krystal, and N.E. Reiner. 2007. Monocyte p110alpha phosphatidylinositol 3-kinase regulates phagocytosis, the phagocyte oxidase, and cytokine production. Journal of Leukocyte Biology 81: 1548–1561.
Guha, M., and N. Mackman. 2002. The phosphatidylinositol 3-kinase-Akt pathway limits lipopolysaccharide activation of signaling pathways and expression of inflammatory mediators in human monocytic cells. Journal of Biological Chemistry 277: 32124–32132.
Luyendyk, J.P., G.A. Schabbauer, M. Tencati, T. Holscher, R. Pawlinski, and N. Mackman. 2008. Genetic analysis of the role of the PI3K-Akt pathway in lipopolysaccharide-induced cytokine and tissue factor gene expression in monocytes/macrophages. The Journal of Immunology 180: 4218–4226.
Hutchins, N.A., J. Unsinger, R.S. Hotchkiss, and A. Ayala. 2014. The new normal: Immunomodulatory agents against sepsis immune suppression. Trends in Molecular Medicine 20: 224–233.
Laudanski, K., C. Miller-Graziano, W. Xiao, M.N. Mindrinos, D.R. Richards, A. De, L.L. Moldawer, R.V. Maier, P. Bankey, H.V. Baker, B.H. Brownstein, J.P. Cobb, S.E. Calvano, R.W. Davis, and R.G. Tompkins. 2006. Cell-specific expression and pathway analyses reveal alterations in trauma-related human T cell and monocyte pathways. Proceedings of the National Academy of Sciences USA 103: 15564–15569.
Funding
This work is supported by the National Natural Science Foundation of China (grant numbers 81971858 and 31400751).
Author information
Authors and Affiliations
Contributions
C.Y., Q.Z., X.X., and X.W. designed the project. C.Y., J.C., B.W., J.W., M.L., and J.T. performed experiments. C.Y., Q.Z., and X.W. prepared the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yan, C., Chen, J., Wang, B. et al. PD-L1 Expression Is Increased in LPS-Induced Acute Respiratory Distress Syndrome by PI3K-AKT-Egr-1/C/EBPδ Signaling Pathway. Inflammation (2024). https://doi.org/10.1007/s10753-024-01988-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10753-024-01988-6