Abstract
Rosacea is a chronic facial inflammatory skin disease that occurs with dysfunction of the immune system. Colchicine was reported to have anti-inflammatory properties. However, the impact of colchicine on rosacea remains unclear. In the present study, the phenotype of rosacea lesions was evaluated by the redness score, inflammatory biomarkers were analyzed by reverse transcription PCR (RT‒PCR), and the infiltration of inflammatory cells was assessed by IHC analysis and immunofluorescence in a rosacea-like mouse model. In vitro, RT‒PCR was used to identify the inflammatory factors that Toll-like receptor 2 (TLR2) agonist caused neutrophils to produce, and immunofluorescence and coimmunoprecipitation were used to identify putative signalling pathways. We found that skin erythema and histopathological alterations, as well as elevated proinflammatory factors (IL-1β, IL-6, TNFα, CXCL2) and CAMP, were significantly ameliorated by colchicine treatment in LL37-induced rosacea-like mice. In addition, colchicine reduced the colocalization of TLR2 and neutrophils and the formation of neutrophil extracellular trap networks (NET) in mouse lesions. In neutrophils, colchicine markedly reduced TLR2 agonist-induced inflammatory biomarker expression, NET formation, and ROS production. Moreover, we found that LL37 could bind to TLR2 upon activation of TLR2 in neutrophils. Importantly, colchicine could repress the combination of TLR2 and LL37 in vivo. Finally, bioinformatics methods further validated the key molecules of neutrophil-related inflammation in rosacea, which is consistent with our experimental findings. Collectively, colchicine ameliorated rosacea-like dermatitis by regulating the neutrophil immune response activated by the TLR2 pathway, indicating that it could be an effective therapeutic option for patients with rosacea.





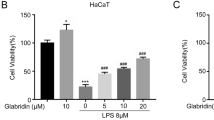
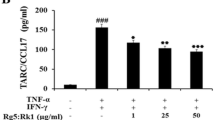
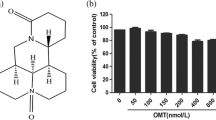
Similar content being viewed by others
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Two, A.M., W. Wu, R.L. Gallo, and T.R. Hata. 2015. Rosacea: part I. Introduction, categorization, histology, pathogenesis, and risk factors. Journal of the American Academy of Dermatology 72: 749–758; quiz 759–760.
van Zuuren, E.J. 2017. Rosacea. New England Journal of Medicine 377: 1754–1764.
Rainer, B.M., S. Kang, and A.L. Chien. 2017. Rosacea: Epidemiology, pathogenesis, and treatment. Dermatoendocrinol 9: e1361574.
Deng, Y., Q. Peng, S. Yang, D. Jian, B. Wang, Y. Huang, H. Xie, and J. Li. 2018. The Rosacea-specific Quality-of-Life instrument (RosQol): Revision and validation among Chinese patients. PLoS ONE 13: e0192487.
Yamasaki, K., A. Di Nardo, A. Bardan, M. Murakami, T. Ohtake, A. Coda, R.A. Dorschner, C. Bonnart, P. Descargues, A. Hovnanian, et al. 2007. Increased serine protease activity and cathelicidin promotes skin inflammation in rosacea. Nature Medicine 13: 975–980.
Yamasaki, K., K. Kanada, D.T. Macleod, A.W. Borkowski, S. Morizane, T. Nakatsuji, A.L. Cogen, and R.L. Gallo. 2011. TLR2 expression is increased in rosacea and stimulates enhanced serine protease production by keratinocytes. The Journal of Investigative Dermatology 131: 688–697.
Gallo, R.L., R.D. Granstein, S. Kang, M. Mannis, M. Steinhoff, J. Tan, and D. Thiboutot. 2018. Standard classification and pathophysiology of rosacea: The 2017 update by the National Rosacea Society Expert Committee. Journal of the American Academy of Dermatology 78: 148–155.
Steinhoff, M., J. Buddenkotte, J. Aubert, M. Sulk, P. Novak, V.D. Schwab, C. Mess, F. Cevikbas, M. Rivier, I. Carlavan, et al. 2011. Clinical, cellular, and molecular aspects in the pathophysiology of rosacea. The Journal of Investigative Dermatology. Symposium Proceedings 15: 2–11.
Zhang, J., P. Jiang, L. Sheng, Y. Liu, Y. Liu, M. Li, M. Tao, L. Hu, X. Wang, Y. Yang, et al. 2021. A novel mechanism of carvedilol efficacy for rosacea treatment: Toll-like receptor 2 inhibition in macrophages. Frontiers in Immunology 12: 609615.
Reinholz, M., T. Ruzicka, and J. Schauber. 2012. Cathelicidin LL-37: An antimicrobial peptide with a role in inflammatory skin disease. Annals of Dermatology 24: 126–135.
Steinhoff, M., J. Schauber, and J.J. Leyden. 2013. New insights into rosacea pathophysiology: A review of recent findings. Journal of the American Academy of Dermatology 69: S15-26.
Buhl, T., M. Sulk, P. Nowak, J. Buddenkotte, I. McDonald, J. Aubert, I. Carlavan, S. Déret, P. Reiniche, M. Rivier, et al. 2015. Molecular and morphological characterization of inflammatory infiltrate in rosacea reveals activation of Th1/Th17 pathways. The Journal of Investigative Dermatology 135: 2198–2208.
Jiang, Y., Y. Huang, G. Ma, T. Liu, Q. Li, H. Wu, and J. Li. 2023. Granulomatous rosacea in Chinese patients: clinical-histopathological analysis and pathogenesis exploration. Journal of Dermatology.
Xiao, W., J. Li, X. Huang, Q. Zhu, T. Liu, H. Xie, Z. Deng, and Y. Tang. 2022. Mediation roles of neutrophils and high-density lipoprotein (HDL) on the relationship between HLA-DQB1 and rosacea. Annals of Medicine 54: 1530–1537.
O’Reilly, N., D. Bergin, E.P. Reeves, N.G. McElvaney, and K. Kavanagh. 2012. Demodex-associated bacterial proteins induce neutrophil activation. British Journal of Dermatology 166: 753–760.
Yousefi, S., D. Stojkov, N. Germic, D. Simon, X. Wang, C. Benarafa, and H.U. Simon. 2019. Untangling “NETosis” from NETs. European Journal of Immunology 49: 221–227.
Riyapa, D., D. Rinchai, V. Muangsombut, C. Wuttinontananchai, M. Toufiq, D. Chaussabel, M. Ato, J.M. Blackwell, and S. Korbsrisate. 2019. Transketolase and vitamin B1 influence on ROS-dependent neutrophil extracellular traps (NETs) formation. PLoS ONE 14: e0221016.
Lee, K.H., A. Kronbichler, D.D. Park, Y. Park, H. Moon, H. Kim, J.H. Choi, Y. Choi, S. Shim, I.S. Lyu, et al. 2017. Neutrophil extracellular traps (NETs) in autoimmune diseases: A comprehensive review. Autoimmunity Reviews 16: 1160–1173.
Robinson, K.P., and J.J. Chan. 2018. Colchicine in dermatology: A review. Australasian Journal of Dermatology 59: 278–285.
Sukeishi, A., K. Isami, H. Hiyama, S. Imai, K. Nagayasu, H. Shirakawa, T. Nakagawa, and S. Kaneko. 2017. Colchicine alleviates acute postoperative pain but delays wound repair in mice: Roles of neutrophils and macrophages. Molecular Pain 13: 1744806917743680.
Zhou, L., H. Zhao, H. Zhao, X. Meng, Z. Zhao, H. Xie, J. Li, Y. Tang, and Y. Zhang. 2023. GBP5 exacerbates rosacea-like skin inflammation by skewing macrophage polarization towards M1 phenotype through the NF-κB signalling pathway. Journal of the European Academy of Dermatology and Venereology 37: 796–809.
Kim, S.W., H. Lee, H.K. Lee, I.D. Kim, and J.K. Lee. 2019. Neutrophil extracellular trap induced by HMGB1 exacerbates damages in the ischemic brain. Acta Neuropathologica Communications 7: 94.
Raup-Konsavage, W.M., Y. Wang, W.W. Wang, D. Feliers, H. Ruan, and W.B. Reeves. 2018. Neutrophil peptidyl arginine deiminase-4 has a pivotal role in ischemia/reperfusion-induced acute kidney injury. Kidney International 93: 365–374.
Yui, S., Y. Nakatani, and M. Mikami. 2003. Calprotectin (S100A8/S100A9), an inflammatory protein complex from neutrophils with a broad apoptosis-inducing activity. Biological &/and Pharmaceutical Bulletin 26: 753–760.
Cribier, B. 2022. Rosacea: Treatment targets based on new physiopathology data. Annales de Dermatologie et de Venereologie 149: 99–107.
Gupta, S., and M.J. Kaplan. 2016. The role of neutrophils and NETosis in autoimmune and renal diseases. Nature Reviews Nephrology 12: 402–413.
Li, G., X. Tang, S. Zhang, Z. Deng, B. Wang, W. Shi, H. Xie, B. Liu, and J. Li. 2022. Aging-conferred SIRT7 decline inhibits rosacea-like skin inflammation by modulating Toll-like receptor 2-NF-κB signaling. The Journal of Investigative Dermatology 142: 2580-2590.e2586.
Mandala, J.P., S. Ahmad, A. Pullagurla, S. Thada, L. Joshi, M.S.S. Ansari, V.L. Valluri, and S.L. Gaddam. 2020. Toll-like receptor 2 polymorphisms and their effect on the immune response to ESAT-6, Pam3CSK4 TLR2 agonist in pulmonary tuberculosis patients and household contacts. Cytokine 126: 154897.
Arzumanyan, G., K. Mamatkulov, Y. Arynbek, D. Zakrytnaya, A. Jevremović, and N. Vorobjeva. 2023. Radiation from UV-A to red light induces ROS-dependent Release of neutrophil extracellular traps. International Journal of Molecular Sciences 24.
Herster, F., Z. Bittner, N.K. Archer, S. Dickhöfer, D. Eisel, T. Eigenbrod, T. Knorpp, N. Schneiderhan-Marra, M.W. Löffler, H. Kalbacher, et al. 2020. Neutrophil extracellular trap-associated RNA and LL37 enable self-amplifying inflammation in psoriasis. Nature Communications 11: 105.
Funding
This work was supported by Guizhou Provincial Science and Technology Projects, ZK[2021] general 421. Guizhou Provincial Science and Technology Projects, ZK[2022] general 250. Fund for Less Developed Regions of the National Natural Science Foundation of China, (Grant: 82160601, GPPH-NSFC-2021-13)
Author information
Authors and Affiliations
Contributions
Xin Yuan and Chengxiang Lian designed research; Xin Yuan, Chengxiang Lian, Liang Sheng, and Guang Shi performed research; Leiwei Jiang contributed new reagents or analytic tools; Leiwei Jiang and Xin Yuan analyzed data; Chengxiang Lian and Xin Yuan wrote the paper.
Corresponding authors
Ethics declarations
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yuan, X., Sheng, L., Shi, G. et al. Colchicine Alleviates Rosacea by Inhibiting Neutrophil Inflammation Activated by the TLR2 Pathway. Inflammation (2024). https://doi.org/10.1007/s10753-023-01956-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10753-023-01956-6