Abstract
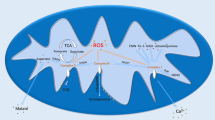
Neutrophil survival and oxidative stress during inflammatory conditions are linked to tissue damage. The present study explores less understood role of catalase, the enzyme catalysing hydrogen peroxide decomposition, in neutrophil survival/death. Importantly, inhibition of catalase activity following S-glutathionylation in the PMA, NO, or zymosan-activated neutrophils or treatment with catalase inhibitor led to neutrophil death. On the contrary, introducing reducing environment by TCEP rescued catalase activity and significantly improved neutrophil survival. Furthermore, augmentation in ROS generation by NOX-2 activation or induction of mitochondrial ROS by Antimycin-A induced catalase S-glutathionylation and cell death, which was prevented in the neutrophil cytosolic factor1 (NCF-1-/-) cells or was rescued by MitoTEMPO, a mitochondrial ROS scavenger, thus, suggesting a correlation between catalase S-glutathionylation/activity inhibition and reduced neutrophil survival. Altogether, enhanced NOX2 activation/mitochondrial dysfunction led to reduced survival of human and mice neutrophils, due to H2O2 accumulation, S-glutathionylation of catalase, and reduction in its enzymatic activity. The present study thus demonstrated mitigation of catalase activity under oxidative stress-impacted neutrophil survival.




Similar content being viewed by others
References
McCracken, J.M., and L.A. Allen. 2014. Regulation of human neutrophil apoptosis and lifespan in health and disease. Journal of Cell Death 7: 15–23.
Albright, C.D., R.I. Salganik, C.N. Craciunescu, M.H. Mar, and S.H. Zeisel. 2003. Mitochondrial and microsomal derived reactive oxygen species mediate apoptosis induced by transforming growth factor-beta1 in immortalized rat hepatocytes. Journal of Cellular Biochemistry 89: 254–261.
Carneiro, M.B.H., E.H. Roma, A.J. Ranson, N.A. Doria, A. Debrabant, D.L. Sacks, L.Q. Vieira, and N.C. Peters. 2018. NOX2-derived reactive oxygen species control inflammation during Leishmania amazonensis infection by mediating infection-induced neutrophil apoptosis. Journal of Immunology 200: 196–208.
Slater, A.F., C.S. Nobel, and S. Orrenius. 1995. The role of intracellular oxidants in apoptosis. Biochimica et Biophysica Acta 1271: 59–62.
Xu, Y., F. Loison, and H.R. Luo. 2010. Neutrophil spontaneous death is mediated by down-regulation of autocrine signaling through GPCR, PI3Kgamma, ROS, and actin. Proceedings of the National Academy of Sciences of the United States of America 107: 2950–2955.
Johnson, T.M., Z.X. Yu, V.J. Ferrans, R.A. Lowenstein, and T. Finkel. 1996. Reactive oxygen species are downstream mediators of p53-dependent apoptosis. Proceedings of the National Academy of Sciences of the United States of America 93: 11848–11852.
Awasthi, D., S. Nagarkoti, A. Kumar, M. Dubey, A.K. Singh, P. Pathak, T. Chandra, M.K. Barthwal, and M. Dikshit. 2016. Oxidized LDL induced extracellular trap formation in human neutrophils via TLR-PKC-IRAK-MAPK and NADPH-oxidase activation. Free Radical Biology & Medicine 93: 190–203.
Abdel-Daim, M.M., N.I. Zakhary, L. Aleya, S.G. Bungau, R.A. Bohara, and N.J. Siddiqi. 2018. Aging, metabolic, and degenerative disorders: biomedical value of antioxidants. Oxidative Medicine and Cellular Longevity 2018: 2098123.
Abdel Daim, M., O. Eltawil, G. Md Ashraf, S. Bungau, and A. Atanasov. 2018. Applications of antioxidants in metabolic disorders and degenerative diseases: mechanistic approach. Oxidative Medicine and Cellular Longevity 2019. https://doi.org/10.1155/2019/4179676
Yeung, A.W.K., N.T. Tzvetkov, O.S. El-Tawil, S.G. Bungau, M.M. Abdel-Daim, and A.G. Atanasov. 2019. Antioxidants: scientific literature landscape analysis. Oxidative Medicine and Cellular Longevity 2019: 8278454.
Hawkins, R.A., K. Sangster, and M.J. Arends. 1998. Apoptotic death of pancreatic cancer cells induced by polyunsaturated fatty acids varies with double bond number and involves an oxidative mechanism. The Journal of Pathology 185: 61–70.
Takahashi, H., N. Kosaka, and S. Nakagawa. 1998. Alpha-tocopherol protects PC12 cells from hyperoxia-induced apoptosis. Journal of Neuroscience Research 52: 184–191.
Salganik, R.I., C.D. Albright, J. Rodgers, J. Kim, S.H. Zeisel, M.S. Sivashinskiy, and T. van Dyke. 2000. Dietary antioxidant depletion: enhancement of tumor apoptosis and inhibition of brain tumor growth in transgenic mice. Carcinogenesis 21: 909–914.
Abdel-Daim, M.M., K. Abo-El-Sooud, L. Aleya, S.G. Bungau, A. Najda, and R. Saluja. 2018. Alleviation of drugs and chemicals toxicity: biomedical value of antioxidants. Oxidative Medicine and Cellular Longevity 2018: 6276438.
Raducan, A., A.R. Cantemir, M. Puiu, and D. Oancea. 2012. Kinetics of hydrogen peroxide decomposition by catalase: hydroxylic solvent effects. Bioprocess and Biosystems Engineering 35: 1523–1530.
Kinnula, V.L., Y. Soini, K. Kvist-Makela, E.R. Savolainen, and P. Koistinen. 2002. Antioxidant defense mechanisms in human neutrophils. Antioxidants & Redox Signaling 4: 27–34.
Maianski, N.A., J. Geissler, S.M. Srinivasula, E.S. Alnemri, D. Roos, and T.W. Kuijpers. 2004. Functional characterization of mitochondria in neutrophils: a role restricted to apoptosis. Cell Death and Differentiation 11: 143–153.
van Raam, B.J., W. Sluiter, E. de Wit, D. Roos, A.J. Verhoeven, and T.W. Kuijpers. 2008. Mitochondrial membrane potential in human neutrophils is maintained by complex III activity in the absence of supercomplex organisation. PLoS One 3: e2013.
Li, X., P. Fang, J. Mai, E.T. Choi, H. Wang, and X.F. Yang. 2013. Targeting mitochondrial reactive oxygen species as novel therapy for inflammatory diseases and cancers. Journal of Hematology & Oncology 6: 19.
Orrenius, S., V. Gogvadze, and B. Zhivotovsky. 2007. Mitochondrial oxidative stress: implications for cell death. Annual Review of Pharmacology and Toxicology 47: 143–183.
Kalogeris, T., Y. Bao, and R.J. Korthuis. 2014. Mitochondrial reactive oxygen species: a double edged sword in ischemia/reperfusion vs preconditioning. Redox Biology 2: 702–714.
Cairns, R.A., I.S. Harris, and T.W. Mak. 2011. Regulation of cancer cell metabolism. Nature Reviews Cancer 11: 85–95.
Sanz, A. 2016. Mitochondrial reactive oxygen species: Do they extend or shorten animal lifespan? Biochimica et Biophysica Acta 1857: 1116–1126.
Madamanchi, N.R., and M.S. Runge. 2007. Mitochondrial dysfunction in atherosclerosis. Circulation Research 100: 460–473.
Ohashi, M., M.S. Runge, F.M. Faraci, and D.D. Heistad. 2006. MnSOD deficiency increases endothelial dysfunction in ApoE-deficient mice. Arteriosclerosis, Thrombosis, and Vascular Biology 26: 2331–2336.
Abdel-Daim, M.M., Y.M. Moustafa, M. Umezawa, K.V. Ramana, and E. Azzini. 2017. Applications of antioxidants in ameliorating drugs and xenobiotics toxicity: mechanistic approach. Oxidative Medicine and Cellular Longevity 2017: 4565127.
Nagarkoti, S., M. Dubey, D. Awasthi, V. Kumar, T. Chandra, S. Kumar, and M. Dikshit. 2018. S-Glutathionylation of p47phox sustains superoxide generation in activated neutrophils. Biochimica et Biophysica Acta 1865: 444–454.
Ivanovic-Matic, S., D. Bogojevic, V. Martinovic, A. Petrovic, S. Jovanovic-Stojanov, G. Poznanovic, et al. 2014. Catalase inhibition in diabetic rats potentiates DNA damage and apoptotic cell death setting the stage for cardiomyopathy. Journal of Physiology and Biochemistry 70: 947–959.
Wang, W., M. Adachi, R. Kawamura, H. Sakamoto, T. Hayashi, T. Ishida, K. Imai, and Y. Shinomura. 2006. Parthenolide-induced apoptosis in multiple myeloma cells involves reactive oxygen species generation and cell sensitivity depends on catalase activity. Apoptosis : an international journal on programmed cell death 11: 2225–2235.
Gurgul, E., S. Lortz, M. Tiedge, A. Jorns, and S. Lenzen. 2004. Mitochondrial catalase overexpression protects insulin-producing cells against toxicity of reactive oxygen species and proinflammatory cytokines. Diabetes 53: 2271–2280.
Izawa, S., Y. Inoue, and A. Kimura. 1996. Importance of catalase in the adaptive response to hydrogen peroxide: analysis of acatalasaemic Saccharomyces cerevisiae. The Biochemical Journal 320 (Pt 1): 61–67.
Goth, L., A. Lenkey, and W.N. Bigler. 2001. Blood catalase deficiency and diabetes in Hungary. Diabetes Care 24: 1839–1840.
Ogata, M., D.H. Wang, and K. Ogino. 2008. Mammalian acatalasemia: the perspectives of bioinformatics and genetic toxicology. Acta Medica Okayama 62: 345–361.
Komosinska-Vassev, K., K. Olczyk, P. Olczyk, and K. Winsz-Szczotka. 2005. Effects of metabolic control and vascular complications on indices of oxidative stress in type 2 diabetic patients. Diabetes Research and Clinical Practice 68: 207–216.
Sethi, S., and M. Dikshit. 2000. Modulation of polymorphonuclear leukocytes function by nitric oxide. Thrombosis Research 100: 223–247.
Cowland, J.B., and N. Borregaard. 1999. Isolation of neutrophil precursors from bone marrow for biochemical and transcriptional analysis. Journal of Immunological Methods 232: 191–200.
Dubey, M., S. Nagarkoti, D. Awasthi, A.K. Singh, T. Chandra, J. Kumaravelu, M.K. Barthwal, and M. Dikshit. 2016. Nitric oxide-mediated apoptosis of neutrophils through caspase-8 and caspase-3-dependent mechanism. Cell Death & Disease 7: e2348.
Li, Y., and H.E. Schellhorn. 2007. Rapid kinetic microassay for catalase activity. Journal of Biomolecular Techniques 18: 185–187.
Pillai, D.N., and J.W. Earl. 1991. Quality assurance for biogenic amines with authentic patient specimens. Pathology 23: 11–16.
Lugli, E., L. Troiano, R. Ferraresi, E. Roat, N. Prada, M. Nasi, et al. 2005. Characterization of cells with different mitochondrial membrane potential during apoptosis. Cytometry Part A : the Journal of the International Society for Analytical Cytology 68: 28–35.
Dubey, M., A.K. Singh, D. Awasthi, S. Nagarkoti, S. Kumar, W. Ali, T. Chandra, V. Kumar, M.K. Barthwal, K. Jagavelu, F.J. Sánchez-Gómez, S. Lamas, and M. Dikshit. 2015. L-Plastin S-glutathionylation promotes reduced binding to beta-actin and affects neutrophil functions. Free Radical Biology & Medicine 86: 1–15.
Tsurubuchi, T., Y. Aratani, N. Maeda, and H. Koyama. 2001. Retardation of early-onset PMA-induced apoptosis in mouse neutrophils deficient in myeloperoxidase. Journal of Leukocyte Biology 70: 52–58.
Saito, T., H. Takahashi, H. Doken, H. Koyama, and Y. Aratani. 2005. Phorbol myristate acetate induces neutrophil death through activation of p38 mitogen-activated protein kinase that requires endogenous reactive oxygen species other than HOCl. Bioscience, Biotechnology, and Biochemistry 69: 2207–2212.
Kohnert, K.D., E.J. Freyse, and E. Salzsieder. 2012. Glycaemic variability and pancreatic beta-cell dysfunction. Current Diabetes Reviews 8: 345–354.
Sveinbjornsson, B., R. Olsen, O.M. Seternes, and R. Seljelid. 1996. Macrophage cytotoxicity against murine meth a sarcoma involves nitric oxide-mediated apoptosis. Biochemical and Biophysical Research Communications 223: 643–649.
Shen, X., L. Yang, S. Yan, W. Wei, L. Liang, H. Zheng, and X. Cai. 2014. The effect of FFAR1 on pioglitazone-mediated attenuation of palmitic acid-induced oxidative stress and apoptosis in betaTC6 cells. Metabolism, Clinical and Experimental 63: 335–351.
Wu, J.Z., C.C. Cheng, L.L. Shen, Z.K. Wang, S.B. Wu, W.L. Li, S.H. Chen, R.P. Zhou, and P.H. Qiu. 2014. Synthetic chalcones with potent antioxidant ability on H(2)O(2)-induced apoptosis in PC12 cells. International Journal of Molecular Sciences 15: 18525–18539.
Jawaid, P., M. Rehman, Y. Yoshihisa, P. Li, Q. Zhao, M.A. Hassan, et al. 2014. Effects of SOD/catalase mimetic platinum nanoparticles on radiation-induced apoptosis in human lymphoma U937 cells. Apoptosis : an international journal on programmed cell death 19: 1006–1016.
Song, L.L., Y.Y. Tu, L. Xia, W.W. Wang, W. Wei, C.M. Ma, D.H. Wen, H. Lei, H.Z. Xu, and Y.L. Wu. 2014. Targeting catalase but not peroxiredoxins enhances arsenic trioxide-induced apoptosis in K562 cells. PLoS One 9: e104985.
Goth, L., T. Nagy, and M. Kaplar. 2015. Acatalasemia and type 2 diabetes mellitus. Orvosi Hetilap 156: 393–398.
Wagner, B.A., B.E. Britigan, K.J. Reszka, M.L. McCormick, and C.P. Burns. 2002. Hydrogen peroxide-induced apoptosis of HL-60 human leukemia cells is mediated by the oxidants hypochlorous acid and chloramines. Archives of Biochemistry and Biophysics 401: 223–234.
Ding, G.R., T. Nakahara, H. Hirose, S. Koyama, Y. Takashima, and J. Miyakoshi. 2004. Extremely low frequency magnetic fields and the promotion of H2O2-induced cell death in HL-60 cells. International Journal of Radiation Biology 80: 317–324.
DiPietrantonio, A.M., T. Hsieh, and J.M. Wu. 1999. Activation of caspase 3 in HL-60 cells exposed to hydrogen peroxide. Biochemical and Biophysical Research Communications 255: 477–482.
Yamakawa, H., Y. Ito, T. Naganawa, Y. Banno, S. Nakashima, S. Yoshimura, M. Sawada, Y. Nishimura, Y. Nozawat, and N. Sakai. 2000. Activation of caspase-9 and -3 during H2O2-induced apoptosis of PC12 cells independent of ceramide formation. Neurological Research 22: 556–564.
Aoshiba, K., Y. Nakajima, S. Yasui, J. Tamaoki, and A. Nagai. 1999. Red blood cells inhibit apoptosis of human neutrophils. Blood 93: 4006–4010.
Lizcano, A., I. Secundino, S. Dohrmann, R. Corriden, C. Rohena, S. Diaz, et al. 2017. Erythrocyte sialoglycoproteins engage Siglec-9 on neutrophils to suppress activation. Blood 129: 3100–3110.
Li, L., Y.G. Zhang, and C.L. Chen. 2013. Anti-apoptotic role of peroxiredoxin III in cervical cancer cells. FEBS Open Bio 3: 51–54.
Gruss-Fischer, T., and I. Fabian. 2002. Protection by ascorbic acid from denaturation and release of cytochrome c, alteration of mitochondrial membrane potential and activation of multiple caspases induced by H(2)O(2), in human leukemia cells. Biochemical Pharmacology 63: 1325–1335.
Nijs, J., F. Almond, P. De Becker, S. Truijen, and L. Paul. 2008. Can exercise limits prevent post-exertional malaise in chronic fatigue syndrome? An uncontrolled clinical trial. Clinical Rehabilitation 22: 426–435.
Palomba, L., P. Sestili, and O. Cantoni. 1999. The antioxidant butylated hydroxytoluene induces apoptosis in human U937 cells: the role of hydrogen peroxide and altered redox state. Free Radical Research 31: 93–101.
Jing, Y., J. Dai, R.M. Chalmers-Redman, W.G. Tatton, and S. Waxman. 1999. Arsenic trioxide selectively induces acute promyelocytic leukemia cell apoptosis via a hydrogen peroxide-dependent pathway. Blood 94: 2102–2111.
Sagara, Y., R. Dargusch, D. Chambers, J. Davis, D. Schubert, and P. Maher. 1998. Cellular mechanisms of resistance to chronic oxidative stress. Free Radical Biology & Medicine 24: 1375–1389.
Bai, J., and A.I. Cederbaum. 2003. Catalase protects HepG2 cells from apoptosis induced by DNA-damaging agents by accelerating the degradation of p53. The Journal of Biological Chemistry 278: 4660–4667.
Finkel, T. 2012. Signal transduction by mitochondrial oxidants. The Journal of Biological Chemistry 287: 4434–4440.
Nieborowska-Skorska, M., P.K. Kopinski, R. Ray, G. Hoser, D. Ngaba, S. Flis, K. Cramer, M.M. Reddy, M. Koptyra, T. Penserga, E. Glodkowska-Mrowka, E. Bolton, T.L. Holyoake, C.J. Eaves, S. Cerny-Reiterer, P. Valent, A. Hochhaus, T.P. Hughes, H. van der Kuip, M. Sattler, W. Wiktor-Jedrzejczak, C. Richardson, A. Dorrance, T. Stoklosa, D.A. Williams, and T. Skorski. 2012. Rac2-MRC-cIII-generated ROS cause genomic instability in chronic myeloid leukemia stem cells and primitive progenitors. Blood 119: 4253–4263.
Turrens, J.F., B.A. Freeman, J.G. Levitt, and J.D. Crapo. 1982. The effect of hyperoxia on superoxide production by lung submitochondrial particles. Archives of Biochemistry and Biophysics 217: 401–410.
Schon, E.A., and S. Przedborski. 2011. Mitochondria: the next (neurode)generation. Neuron 70: 1033–1053.
Finkel, T. 2011. Signal transduction by reactive oxygen species. The Journal of Cell Biology 194: 7–15.
Sadaf, S., A.K. Singh, D. Awasthi, S. Nagarkoti, A.K. Agrahari, R.N. Srivastava, K. Jagavelu, S. Kumar, M.K. Barthwal and M. Dikshit. 2019 Augmentation of iNOS expression in myeloid progenitor cells expedites neutrophil differentiation. J Leukoc Biol 106: 397–415. https://doi.org/10.1002/JLB.1A0918-349RR
Sakai, J., J. Li, K.K. Subramanian, S. Mondal, B. Bajrami, H. Hattori, Y. Jia, B.C. Dickinson, J. Zhong, K. Ye, C.J. Chang, Y.S. Ho, J. Zhou, and H.R. Luo. 2012. Reactive oxygen species-induced actin glutathionylation controls actin dynamics in neutrophils. Immunity 37: 1037–1049.
Acknowledgements
Award of research fellowships to SN and SS from University of Grant commission and to MDY and DA from Council of scientific and Industrial Research, India is acknowledged. Financial Assitance provided to Dr. Madhu Dikshit from the JC Bose National Fellowship (SB/SE/JCB-017/2015). Mr. A L Vishwakarma and Mrs. M Chaturvedi being acknowledged for the excellent technical assistance during the flow cytometry experiments.
Funding
The present study was supported by financial assistance provided to Dr. Madhu Dikshit from the JC Bose National fellowship (SB/SE/JCB-017/2015).
Author information
Authors and Affiliations
Contributions
S.N performed most of the experiments, and was involved in writing of the manuscript. M.DY, S.S and D.A provide experimental help. T.C provided the buffy coat samples. K.J provided the knock-out mice. S.K was involved in the writing of manuscript and also gave suggestions during the experiments. M.D., the corresponding author, guided, designed and conceptualized the work and was involved in finalising the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Fig. S1
A) Cell death was monitored in control and Zymosan or NO treated neutrophils for 4 and 12 h respectively by using Annexin V-PI labelling. B) ROS/RNS generation was measured by DCF-2DA in Zymosan or NO treated human neutrophils. C) Superoxide radical production was measured by DHE using flow cytometry in Zymosan or NO treated human neutrophils. D) Mitochondrial ROS generation was monitored by MitoSOX Red by flow cytometry in Zymosan or NO treated human neutrophils. E) H2O2 production represented in fold change as checked by Amplex RED Kit in Zymosan or NO induced PMNs. F) Zymosan induced cell death was measured in presence of MitoTEMPO; mitochondrial scavenger, mitochondrial complex III inhibitor and catalase inhibitor 3-aminotriazole by Annexin V-FITC/PI labelling. G) NO induced cell death was measured in presence of MitoTEMPO; mitochondrial scavenger, mitochondrial complex III inhibitor and catalase inhibitor 3-aminotriazole by Annexin V-FITC/PI labelling. H) Human PMNs were pre-treated with MitoTEMPO, Antimycin-A or 3-aminotriazole, and then induced with Zymosan. Catalase activity was checked in control and treated neutrophils. I) Human PMNs were pre-treated with MitoTEMPO, Antimycin-A and 3-aminotriazole, and then treated with NO donor. Catalase activity was checked in the control and treated neutrophils. Data have been represented as mean ± SEM from three different experiments. *** p < 0.001, **p < 0.01versus untreated control neutrophils, $$$ p < 0.001, $$p < 0.01, $p < 0.05 versus zymosan treated neutrophils and@@@ p < 0.001, @@p < 0.01, @p < 0.05 versus NO treated neutrophils. (PNG 45.9 kb)
Rights and permissions
About this article
Cite this article
Nagarkoti, S., Dubey, M., Sadaf, S. et al. Catalase S-Glutathionylation by NOX2 and Mitochondrial-Derived ROS Adversely Affects Mice and Human Neutrophil Survival. Inflammation 42, 2286–2296 (2019). https://doi.org/10.1007/s10753-019-01093-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-019-01093-z