Abstract
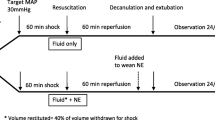
Hemorrhage is a common cause of death in the battlefield. Valproic acid (VPA) has been associated with improved outcomes in multiple models of trauma, when combined with isotonic fluid resuscitation. However, isotonic fluid administered in this setting is logistically impractical and may be associated with complications. In this study, we sought to evaluate the feasibility and immunologic impact of combining VPA treatment with low-volume hypertonic saline (HTS). In vivo: female Yorkshire swine were subjected to hemorrhage (40% total blood volume) and polytrauma (rib fracture and delayed liver injury). Animals were kept in shock for 30 minutes and resuscitated with (1) normal saline (NS, 3× hemorrhaged volume), (2) HTS (7.5% saline, 4 mL/kg), or (3) HTS + VPA (4 mg/kg; 150 mg/kg; n = 3/cohort). After 18 hours of observation, animals were euthanized and the lungs evaluated for acute injury and expression of myeloperoxidase (MPO) and caveolin-1 (Cav-1). In vitro: human umbilical vein endothelial cells (HUVECs) were exposed to anoxic conditions (5% CO2, 95% N2) for 16 hours in (1) normosmotic, (2) hyperosmotic (400 mOsm), or (3) hyperosmotic + VPA (4 mM) media. Immunohistochemistry and Western blots were performed to determine Cav-1 expression. Lungs from VPA-treated animals demonstrated decreased acute injury, MPO expression, and endothelial expression of Cav-1 when compared to lungs from animals resuscitated with NS or HTS alone. Similarly, HUVECs cultured in hyperosmotic media containing VPA demonstrated decreased expression of Cav-1. This study demonstrates that combined treatment with VPA and HTS is a viable strategy in hemorrhagic shock and polytrauma. Attenuation of lung injury following VPA treatment may be related to modulation of the inflammatory response.





Similar content being viewed by others
References
Kelly, J.F., A.E. Ritenour, D.F. McLaughlin, et al. 2008. Injury severity and causes of death from operation Iraqi freedom and operation enduring freedom: 2003-2004 versus 2006. The Journal of Trauma 64 (2 Suppl): S21–S26 discussion S6-7.
Shackford, S.R., R.C. Mackersie, T.L. Holbrook, et al. 1993. The epidemiology of traumatic death. A population-based analysis. Archives of Surgery 128 (5): 571–575.
Holcomb, J.B., B.C. Tilley, S. Baraniuk, et al. 2015. Transfusion of plasma, platelets, and red blood cells in a 1:1:1 vs a 1:1:2 ratio and mortality in patients with severe trauma: The PROPPR randomized clinical trial. Journal of the American Medical Association 313 (5): 471–482.
Neal, M.D., J.B. Brown, E.E. Moore, et al. 2014. Prehospital use of nonsteroidal anti-inflammatory drugs (NSAIDs) is associated with a reduced incidence of trauma-induced coagulopathy. Annals of Surgery 260 (2): 378–382.
Park, P.K., J.W. Cannon, W. Ye, et al. 2013. Transfusion strategies and development of acute respiratory distress syndrome in combat casualty care. Journal of Trauma and Acute Care Surgery 75 (2 Suppl 2): S238–S246.
Balogh, Z.J., W. Lumsdaine, E.E. Moore, and F.A. Moore. 2014. Postinjury abdominal compartment syndrome: From recognition to prevention. Lancet 384 (9952): 1466–1475.
Gunst, M., V. Ghaemmaghami, A. Gruszecki, J. Urban, H. Frankel, and S. Shafi. 2010. Changing epidemiology of trauma deaths leads to a bimodal distribution. Proc (Bayl Univ Med Cent). 23 (4): 349–354.
Gerhordt, R.T., and F.K. Butler. 2012. CAPT U. Fundamentals of Combat Casualty Care. Combat Casualty Care: Lessons Learned from OEF and OIF. 9:85.
Bulger, E.M., and D.B. Hoyt. 2012. Hypertonic resuscitation after severe injury: Is it of benefit? Advances in Surgery 46: 73–85.
Champion, H.R. 2003. Combat fluid resuscitation: Introduction and overview of conferences. The Journal of Trauma 54 (5 Suppl): S7–12.
Rhee, P., E. Koustova, and H.B. Alam. 2003. Searching for the optimal resuscitation method: Recommendations for the initial fluid resuscitation of combat casualties. The Journal of Trauma 54 (5 Suppl): S52–S62.
Halaweish, I., V. Nikolian, P. Georgoff, Y. Li, and H.B. Alam. 2015. Creating a "Prosurvival phenotype" through histone deacetylase inhibition: Past, present, and future. Shock 44 (Suppl 1): 6–16.
Rasmussen, T.E., D.G. Baer, A.P. Cap, and B.C. Lein. 2015. Ahead of the curve: Sustained innovation for future combat casualty care. Journal of Trauma and Acute Care Surgery 79 (4 Suppl 2): S61–S64.
Georgoff, P., Halaweish, I., Nikolian, V. et al. 2016. Alterations in the human proteome following administration of valproic acid. Journal of Trauma and Acute Care Surgery.
Li, Y., and H.B. Alam. 2011. Modulation of acetylation: Creating a pro-survival and anti-inflammatory phenotype in lethal hemorrhagic and septic shock. Journal of Biomedicine & Biotechnology 2011: 523481.
Sailhamer, E.A., Y. Li, E.J. Smith, et al. 2008. Acetylation: A novel method for modulation of the immune response following trauma/hemorrhage and inflammatory second hit in animals and humans. Surgery 144 (2): 204–216.
Alam, H.B., K.B. Hamwi, M. Duggan, et al. 2011. Hemostatic and pharmacologic resuscitation: Results of a long-term survival study in a swine polytrauma model. The Journal of Trauma 70 (3): 636–645.
Alam, H.B., F. Shuja, M.U. Butt, et al. 2009. Surviving blood loss without blood transfusion in a swine poly-trauma model. Surgery 146 (2): 325–333.
Liu, Z., Y. Li, B. Liu, et al. 2013. Synergistic effects of hypertonic saline and valproic acid in a lethal rat two-hit model. Journal of Trauma and Acute Care Surgery 74 (4): 991–997 discussion 7-8.
Halaweish, I., T. Bambakidis, W. He, et al. 2015. Early resuscitation with fresh frozen plasma for traumatic brain injury combined with hemorrhagic shock improves neurologic recovery. Journal of the American College of Surgeons 220 (5): 809–819.
Souto, F.O., J.C. Alves-Filho, W.M. Turato, M. Auxiliadora-Martins, A. Basile-Filho, and F.Q. Cunha. 2011. Essential role of CCR2 in neutrophil tissue infiltration and multiple organ dysfunction in sepsis. American Journal of Respiratory and Critical Care Medicine 183 (2): 234–242.
Williams, T.M., F. Medina, I. Badano, et al. 2004. Caveolin-1 gene disruption promotes mammary tumorigenesis and dramatically enhances lung metastasis in vivo. Role of Cav-1 in cell invasiveness and matrix metalloproteinase (MMP-2/9) secretion. The Journal of Biological Chemistry 279 (49): 51630–51646.
Halaweish, I., T. Bambakidis, Z. Chang, et al. 2015. Addition of low-dose valproic acid to saline resuscitation provides neuroprotection and improves long-term outcomes in a large animal model of combined traumatic brain injury and hemorrhagic shock. Journal of Trauma and Acute Care Surgery 79 (6): 911–919.
Jin, G., M. Duggan, A. Imam, et al. 2012. Pharmacologic resuscitation for hemorrhagic shock combined with traumatic brain injury. Journal of Trauma and Acute Care Surgery 73 (6): 1461–1470.
Sillesen, M., L.S. Rasmussen, G. Jin, et al. 2014. Assessment of coagulopathy, endothelial injury, and inflammation after traumatic brain injury and hemorrhage in a porcine model. Journal of Trauma and Acute Care Surgery 76 (1): 12–19 discussion 9-20.
Findlay, L.J., P. El-Mallakh, and R.S. El-Mallakh. 2015. Management of bipolar I depression: Clinical utility of lurasidone. Therapeutics and Clinical Risk Management 11: 75–81.
Loscher, W. 1999. Valproate: A reappraisal of its pharmacodynamic properties and mechanisms of action. Progress in Neurobiology 58 (1): 31–59.
Lennartsson, A., E. Arner, M. Fagiolini, et al. 2015. Remodeling of retrotransposon elements during epigenetic induction of adult visual cortical plasticity by HDAC inhibitors. Epigenetics & Chromatin 8: 55.
Wanczyk, M., K. Roszczenko, K. Marcinkiewicz, K. Bojarczuk, M. Kowara, and M. Winiarska. 2011. HDACi--going through the mechanisms. Front Biosci (Landmark Ed) 16: 340–359.
Das, C., and T.K. Kundu. 2005. Transcriptional regulation by the acetylation of nonhistone proteins in humans -- a new target for therapeutics. IUBMB Life 57 (3): 137–149.
Bulger, E.M., S. May, J.D. Kerby, et al. 2011. Out-of-hospital hypertonic resuscitation after traumatic hypovolemic shock: A randomized, placebo controlled trial. Annals of Surgery 253 (3): 431–441.
Bulger, E.M., G.J. Jurkovich, A.B. Nathens, et al. 2008. Hypertonic resuscitation of hypovolemic shock after blunt trauma: A randomized controlled trial. Archives of Surgery 143 (2): 139–148 discussion 49.
Holcroft, J.W., M.J. Vassar, J.E. Turner, R.W. Derlet, and G.C. Kramer. 1987. 3% NaCl and 7.5% NaCl/dextran 70 in the resuscitation of severely injured patients. Annals of Surgery 206 (3): 279–288.
Holcroft, J.W., M.J. Vassar, C.A. Perry, W.L. Gannaway, and G.C. Kramer. 1989. Use of a 7.5% NaCl/6% dextran 70 solution in the resuscitation of injured patients in the emergency room. Progress in Clinical and Biological Research 299: 331–338.
Yang, Y., Q.H. Chen, A.R. Liu, X.P. Xu, J.B. Han, and H.B. Qiu. 2015. Synergism of MSC-secreted HGF and VEGF in stabilising endothelial barrier function upon lipopolysaccharide stimulation via the Rac1 pathway. Stem Cell Research & Therapy 6: 250.
Sun, Y., G. Hu, X. Zhang, and R.D. Minshall. 2009. Phosphorylation of caveolin-1 regulates oxidant-induced pulmonary vascular permeability via paracellular and transcellular pathways. Circulation Research 105 (7): 676–685 15 p following 85.
Jin, Y., S.J. Lee, R.D. Minshall, and A.M. Choi. 2011. Caveolin-1: A critical regulator of lung injury. American Journal of Physiology. Lung Cellular and Molecular Physiology 300 (2): L151–L160.
Bento-Abreu, A., A. Velasco, E. Polo-Hernandez, et al. 2009. Albumin endocytosis via megalin in astrocytes is caveola- and dab-1 dependent and is required for the synthesis of the neurotrophic factor oleic acid. Journal of Neurochemistry 111 (1): 49–60.
Bambakidis, T., Dekker, S.E., Sillensen, M. et al. 2016. Resuscitation with valproic acid alters inflammatory genes in a porcine model of combined traumatic brain injury and hemorrhagic shock. Journal of Neurotrauma.
Bogert, J.N., J.A. Harvin, and B.A. Cotton. 2016. Damage Control Resuscitation. Journal of Intensive Care Medicine 31 (3): 177–186.
Nessen, S.C., B.J. Eastridge, D. Cronk, et al. 2013. Fresh whole blood use by forward surgical teams in Afghanistan is associated with improved survival compared to component therapy without platelets. Transfusion 53 (Suppl 1): 107S–113S.
Acknowledgements
This work was funded by a grant from Department of Defense W81XWH-09-2-0001to YL. Designed study: HBA, YL; performed research: BP, XD, BL; collected data: BP, TM, MJD; analyzed data: BP, PEG, XD; wrote paper: VCN, BP, ISD; revised manuscript: VCN, BP, XW, YL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This research was conducted in compliance with the Animal Welfare Act and other federal statutes and regulations relating experiments involving animals. The study adhered to the principles stated in the Guide for the Care and Use of Laboratory Animals, National Research Council, and was approved by the Institutional Animal Care and Use Committee at Massachusetts General Hospital. All procedures were performed under the supervision of a veterinarian.
Conflict of Interests
The authors declare that they have no conflict of interest.
Additional information
Vahagn C. Nikolian and Baihong Pan contributed equally to project and manuscript. Co-first authorship.
Electronic supplementary material
S1 Fig
VPA decreased anoxia-induced expression of Caveolin-1 (Cav-1) in HUVECs. A, Microscopic images of HUVECs in 100 mm culture dishes; B, Representative immunoblots of Cav-1 in HUVECs cell extract and actin as an internal control of protein-loading; C, Cav-1 protein bands quantified by densitometry and normalized with actin were expressed as mean values ± SD (n = 4/group); *, p ≤ 0.0015 compared to sham group; #, P ≤ 0.001 compared to Anoxia + HTS + VPA group; NS, normal saline; HTS, hypertonic saline; VPA, valproic acid; Sham, no trauma and hemorrhagic shock, no treatment. (GIF 102 kb)
Rights and permissions
About this article
Cite this article
Nikolian, V.C., Pan, B., Mesar, T. et al. Lung Protective Effects of Low-Volume Resuscitation and Pharmacologic Treatment of Swine Subjected to Polytrauma and Hemorrhagic Shock. Inflammation 40, 1264–1274 (2017). https://doi.org/10.1007/s10753-017-0569-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-017-0569-6