Abstract
Intravenous inotropic therapy can be used in patients with advanced heart failure, as palliative therapy or as a bridge to cardiac transplantation or mechanical circulatory support, as well as in cardiogenic shock. Their use is limited to increasing cardiac output in low cardiac output states and reducing ventricular filling pressures to alleviate patient symptoms and improve functional class. Many advanced heart failure patients have sinus tachycardia as a compensatory mechanism to maintain cardiac output. However, excessive sinus tachycardia caused by intravenous inotropes can increase myocardial oxygen consumption, decrease coronary perfusion, and at extreme heart rates decrease ventricular filling and stroke volume. The limited available hemodynamic studies support the hypothesis that adding ivabradine, a rate control agent without negative inotropic effect, may blunt inotrope-induced tachycardia and its associated deleterious effects, while optimizing cardiac output by increasing stroke volume. This review analyzes the intriguing pathophysiology of combined intravenous inotropes and ivabradine to optimize the hemodynamic profile of patients in advanced heart failure.

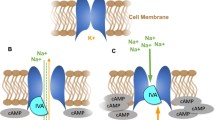
Illustration of the beneficial and deleterious hemodynamic effects of intravenous inotropes in advanced heart failure, and the positive effects of adding ivabradine.
Similar content being viewed by others
Data availability
Not applicable
Abbreviations
- LV:
-
Left ventricle
- cAMP:
-
Cyclic adenosine monophosphate
- HCN:
-
Hyperpolarization-activated cyclic nucleotide-gated
References
Metra M, Ponikowski P, Dickstein K, McMurray JJV, Gavazzi A, Bergh C-H et al (2007) Advanced chronic heart failure: a position statement from the Study Group on Advanced Heart Failure of the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail 9:684–694. https://doi.org/10.1016/j.ejheart.2007.04.003
Hunt SA, Abraham WT, Chin MH, Feldman AM, Francis GS, Ganiats TG et al (2009) 2009 focused update incorporated into the ACC/AHA 2005 guidelines for the diagnosis and management of heart failure in adults: a report of the Aamerican College of Cardiology Foundation/American Heart Association Task Force on practice guidelines: developed in collaboration with the International Society for Heart and Lung Transplantation. Circulation 119. https://doi.org/10.1161/CIRCULATIONAHA.109.192065
Yancy CW, Jessup M, Chair V, Bozkurt B, Butler J, Casey DE et al (2013) 2013 ACCF/AHA Guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. JAC 62:1495–1539. https://doi.org/10.1016/j.jacc.2013.05.020
Aranda JM, Schofield RS, Pauly DF, Cleeton TS, Walker TC, Monroe VS et al (2003) Comparison of dobutamine versus milrinone therapy in hospitalized patients awaiting cardiac transplantation: a prospective, randomized trial. Am Heart J 145:324–329. https://doi.org/10.1067/mhj.2003.50
Brozena SC, Twomey C, Goldberg LR, Desai SS, Drachman B, Kao A et al (2004) A prospective study of continuous intravenous milrinone therapy for status IB patients awaiting heart transplant at home. J Heart Lung Transplant 23:1082–1086. https://doi.org/10.1016/j.healun.2003.08.017
Hershberger RE, Nauman D, Walker TL, Dutton D, Burgess D (2003) Care processes and clinical outcomes of continuous outpatient support with inotropes (COSI) in patients with refractory endstage heart failure. J Card Fail 9:180–187. https://doi.org/10.1054/jcaf.2003.24
Nizamic T, Murad MH, Allen LA, McIlvennan CK, Wordingham SE, Matlock DD et al (2018) Ambulatory inotrope infusions in advanced heart failure: a systematic review and meta-analysis. JACC Hear Fail 6:757–767. https://doi.org/10.1016/j.jchf.2018.03.019
Hauptman PJ, Mikolajczak P, George A, Mohr CJ, Hoover R, Swindle J et al (2006) Chronic inotropic therapy in end-stage heart failure. Am Heart J 152:1096.e1–1096.e8. https://doi.org/10.1016/j.ahj.2006.08.003
Feneck RO, Sherry KM, Withington PS, Oduro-Dominah A (2001) Comparison of the hemodynamic effects of milrinone with dobutamine in patients after cardiac surgery. J Cardiothorac Vasc Anesth 15:306–315. https://doi.org/10.1053/jcan.2001.23274
Cuffe MS, Califf RM, Adams KF, Benza R, Bourge R, Colucci WS et al (2002) Short-term intravenous milrinone for acute exacerbation of chronic heart failure: a randomized controlled trial. J Am Med Assoc 287:1541–1547. https://doi.org/10.1001/jama.287.12.1541
Felker GM, Benza RL, Chandler AB, Leimberger JD, Cuffe MS, Califf RM et al (2003) Heart failure etiology and response to milrinone in decompensated heart failure: results from the OPTIME-CHF study. J Am Coll Cardiol 41:997–1003. https://doi.org/10.1016/S0735-1097(02)02968-6
O’Connor CM, Gattis WA, Uretsky BF, Adams KF, McNulty SE, Grossman SH et al (1999) Continuous intravenous dobutamine is associated with an increased risk of death in patients with advanced heart failure: insights from the Flolan International Randomized Survival Trial (FIRST). Am Heart J 138:78–86. https://doi.org/10.1016/s0002-8703(99)70250-4
Elkayam U, Tasissa G, Binanay C, Stevenson LW, Gheorghiade M, Warnica JW et al (2007) Use and impact of inotropes and vasodilator therapy in hospitalized patients with severe heart failure. Am Heart J 153:98–104. https://doi.org/10.1016/j.ahj.2006.09.005
Abraham WT, Adams KF, Fonarow GC, Costanzo MR, Berkowitz RL, Lejemtel TH et al (2005) In-hospital mortality in patients with acute decompensated heart failure requiring intravenous vasoactive medications: an analysis from the Acute Decompensated Heart Failure National Registry (ADHERE). J Am Coll Cardiol 46:57–64. https://doi.org/10.1016/j.jacc.2005.03.051
Mebazaa A, Motiejunaite J, Gayat E, Crespo-Leiro MG, Lund LH, Maggioni AP et al (2018) Long-term safety of intravenous cardiovascular agents in acute heart failure: results from the European Society of Cardiology Heart Failure Long-Term Registry. Eur J Heart Fail 20:332–341. https://doi.org/10.1002/ejhf.991
Papp Z, Édes I, Fruhwald S, De Hert SG, Salmenperä M, Leppikangas H et al (2012) Levosimendan: molecular mechanisms and clinical implications: consensus of experts on the mechanisms of action of levosimendan. Int J Cardiol 159:82–87. https://doi.org/10.1016/j.ijcard.2011.07.022
Silvetti S, Belletti A, Fontana A, Pollesello P (2017) Rehospitalization after intermittent levosimendan treatment in advanced heart failure patients: a meta-analysis of randomized trials. ESC Hear Fail 4:595–604. https://doi.org/10.1002/ehf2.12177
Comín-Colet J, Manito N, Segovia-Cubero J, Delgado J, García Pinilla JM, Almenar L et al (2018) Efficacy and safety of intermittent intravenous outpatient administration of levosimendan in patients with advanced heart failure: the LION-HEART multicentre randomised trial. Eur J Heart Fail 20:1128–1136. https://doi.org/10.1002/ejhf.1145
Silvetti S, Nieminen MS (2016) Repeated or intermittent levosimendan treatment in advanced heart failure: an updated meta-analysis. Int J Cardiol 202:138–143. https://doi.org/10.1016/j.ijcard.2015.08.188
Pollesello P, Parissis J, Kivikko M, Harjola VP (2016) Levosimendan meta-analyses: is there a pattern in the effect on mortality? Int J Cardiol 209:77–83. https://doi.org/10.1016/j.ijcard.2016.02.014
Follath F, Cleland JGF, Just H, Papp JGY, Scholz H, Peuhkurinen K et al (2002) Efficacy and safety of intravenous levosimendan compared with dobutamine in severe low-output heart failure (the LIDO study): a randomised double-blind trial. Lancet 360:196–202. https://doi.org/10.1016/S0140-6736(02)09455-2
Bonios MJ, Terrovitis JV, Drakos SG, Katsaros F, Pantsios C, Nanas SN et al (2012) Comparison of three different regimens of intermittent inotrope infusions for end stage heart failure. Int J Cardiol 159:225–229. https://doi.org/10.1016/j.ijcard.2011.03.013
Pölzl G, Allipour Birgani S, Comín-Colet J, Delgado JF, Fedele F, García-Gonzáles MJ et al (2019) Repetitive levosimendan infusions for patients with advanced chronic heart failure in the vulnerable post-discharge period. ESC Hear Fail 6:174–181. https://doi.org/10.1002/ehf2.12366
Packer M, Colucci W, Fisher L, Massie BM, Teerlink JR, Young J et al (2013) Effect of levosimendan on the short-term clinical course of patients with acutely decompensated heart failure. JACC Hear Fail 1:103–111. https://doi.org/10.1016/j.jchf.2012.12.004
Mebazaa A, Nieminen MS, Packer M, Cohen-Solal A, Kleber FX, Pocock SJ et al (2007) Levosimendan vs dobutamine for patients with acute decompensated heart failure: the SURVIVE randomized trial. J Am Med Assoc 297:1883–1891. https://doi.org/10.1001/jama.297.17.1883
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS et al (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail 18:891–975. https://doi.org/10.1002/ejhf.592
Vanoverschelde JL, Wijns W, Essamri B, Bol A, Robert A, Labar D et al (1993) Hemodynamic and mechanical determinants of myocardial O2 consumption in normal human heart: effects of dobutamine. Am J Phys 265:H1884–H1892. https://doi.org/10.1152/ajpheart.1993.265.6.H1884
Motwani M, Kidambi A, Sourbron S, Fairbairn TA, Uddin A, Kozerke S et al (2014) Quantitative three-dimensional cardiovascular magnetic resonance myocardial perfusion imaging in systole and diastole. J Cardiovasc Magn Reson 16. https://doi.org/10.1186/1532-429X-16-19
Pieske B, Maier LS, Piacentino V, Weisser J, Hasenfuss G, Houser S (2002) Rate dependence of [Na+]i and contractility in nonfailing and failing human myocardium. Circulation 106:447–453. https://doi.org/10.1161/01.cir.0000023042.50192.f4
Gierula J, Paton MF, Lowry JE, Jamil HA, Byrom R, Drozd M et al (2018) Rate-response programming tailored to the force-frequency relationship improves exercise tolerance in chronic heart failure. JACC Hear Fail 6:105–113. https://doi.org/10.1016/j.jchf.2017.09.018
Flannery G, Gehrig-Mills R, Billah B, Krum H (2008) Analysis of randomized controlled trials on the effect of magnitude of heart rate reduction on clinical outcomes in patients with systolic chronic heart failure receiving beta-blockers. Am J Cardiol 101:865–869. https://doi.org/10.1016/j.amjcard.2007.11.023
Metra M, Nodari S, D’Aloia A, Muneretto C, Robertson AD, Bristow MR et al (2002) Beta-blocker therapy influences the hemodynamic response to inotropic agents in patients with heart failure: a randomized comparison of dobutamine and enoximone before and after chronic treatment with metoprolol or carvedilol. J Am Coll Cardiol 40:1248–1258. https://doi.org/10.1016/s0735-1097(02)02134-4
Bucchi A, Baruscotti M, Difrancesco D (2002) Current-dependent block of rabbit sino-atrial node If channels by ivabradine. J Gen Physiol 120:1–13. https://doi.org/10.1085/jgp.20028593
Bucchi A, Tognati A, Milanesi R, Baruscotti M, DiFrancesco D (2006) Properties of ivabradine-induced block of HCN1 and HCN4 pacemaker channels. J Physiol 572:335–346. https://doi.org/10.1113/jphysiol.2005.100776
Koruth JS, Lala A, Pinney S, Reddy VY, Dukkipati SR (2017) The clinical use of ivabradine
Manz M, Reuter M, Lauck G, Omran H, Jung W (2003) A single intravenous dose of ivabradine, a (novel If inhibitor, lowers heart rate but does) not depress left ventricular function in patients with left ventricular dysfunction. Cardiology 100:149–155. https://doi.org/10.1159/000073933
Herrmann S, Layh B, Ludwig A (2011) Novel insights into the distribution of cardiac HCN channels: an expression study in the mouse heart. J Mol Cell Cardiol 51:997–1006. https://doi.org/10.1016/j.yjmcc.2011.09.005
Colin P, Ghaleh B, Monnet X, Hittinger L, Berdeaux A (2004) Effect of graded heart rate reduction with ivabradine on myocardial oxygen consumption and diastolic time in exercising dogs. J Pharmacol Exp Ther 308:236–240. https://doi.org/10.1124/jpet.103.059717
Mulder P, Barbier S, Chagraoui A, Richard V, Henry JP, Lallemand F et al (2004) Long-term heart rate reduction induced by the selective if current inhibitor ivabradine improves left ventricular function and intrinsic myocardial structure in congestive heart failure. Circulation 109:1674–1679. https://doi.org/10.1161/01.CIR.0000118464.48959.1C
Dedkov EI, Zheng W, Christensen LP, Weiss RM, Mahlberg-Gaudin F, Tomanek RJ (2007) Preservation of coronary reserve by ivabradine-induced reduction in heart rate in infarcted rats is associated with decrease in perivascular collagen. Am J Physiol Heart Circ Physiol 293. https://doi.org/10.1152/ajpheart.00047.2007
Fang Y, Debunne M, Vercauteren M, Brakenhielm E, Richard V, Lallemand F et al (2012) Heart rate reduction induced by the if current inhibitor ivabradine improves diastolic function and attenuates cardiac tissue hypoxia. J Cardiovasc Pharmacol 59:260–267. https://doi.org/10.1097/FJC.0b013e31823e5e01
Swedberg K, Komajda M, Böhm M, Borer JS, Ford I, Dubost-Brama A et al (2010) Ivabradine and outcomes in chronic heart failure (SHIFT): a randomised placebo-controlled study. Lancet 376:875–885. https://doi.org/10.1016/S0140-6736(10)61198-1
Reil JC, Tardif JC, Ford I, Lloyd SM, O’Meara E, Komajda M et al (2013) Selective heart rate reduction with ivabradine unloads the left ventricle in heart failure patients. J Am Coll Cardiol 62:1977–1985. https://doi.org/10.1016/j.jacc.2013.07.027
Tardif J-C, O’Meara E, Komajda M, Böhm M, Borer JS, Ford I et al (2011) Effects of selective heart rate reduction with ivabradine on left ventricular remodelling and function: results from the SHIFT echocardiography substudy. Eur Heart J 32:2507–2515
Bakkehaug JP, Næsheim T, Torgersen Engstad E, Kildal AB, Myrmel T, How OJ (2016) Reversing dobutamine-induced tachycardia using ivabradine increases stroke volume with neutral effect on cardiac energetics in left ventricular post-ischaemia dysfunction. Acta Physiol 218:78–88. https://doi.org/10.1111/apha.12704
Rønning L, Bakkehaug JP, Rødland L, Kildal AB, Myrmel T, How OJ (2018) Opposite diastolic effects of omecamtiv mecarbil versus dobutamine and ivabradine co-treatment in pigs with acute ischemic heart failure. Phys Rep 6:e13879. https://doi.org/10.14814/phy2.13879
Izco MP, Ramírez-Carracedo R, Navarro IH, Ruiz ÁO, Navarro BC, Berrocal IC et al (2020) Ivabradine in acute heart failure: effects on heart rate and hemodynamic parameters in a randomized and controlled swine trial. Cardiol J 27:62–71. https://doi.org/10.5603/CJ.a2018.0078
De Ferrari GM, Mazzuero A, Agnesina L, Bertoletti A, Lettino M, Campana C et al (2008) Favourable effects of heart rate reduction with intravenous administration of ivabradine in patients with advanced heart failure☆. Eur J Heart Fail 10:550–555. https://doi.org/10.1016/j.ejheart.2008.04.005
Cavusoglu Y, Mert U, Nadir A, Mutlu F, Morrad B, Ulus T (2015) Ivabradine treatment prevents dobutamine-induced increase in heart rate in patients with acute decompensated heart failure. J Cardiovasc Med 16:603–609. https://doi.org/10.2459/JCM.0000000000000033
Mert KU, Mert GÖ, Morrad B, Tahmazov S, Mutlu F, Çavuşoglu Y (2017) Effects of ivabradine and beta-blocker therapy on dobutamine-induced ventricular arrhythmias. Kardiol Pol 75:786–793. https://doi.org/10.5603/KP.a2017.0094
Porcile R, Levin R (2016) Safety, tolerability and efficacy of ivabradine for control of sinus tachycardia in patients undergoing inotropic therapy. Curr Res Cardiol 3. https://doi.org/10.4172/2368-0512.1000056
Nguyen LS, Squara P, Amour J, Carbognani D, Bouabdallah K, Thierry S et al (2018) Intravenous ivabradine versus placebo in patients with low cardiac output syndrome treated by dobutamine after elective coronary artery bypass surgery: a phase 2 exploratory randomized controlled trial. Crit Care 22:193. https://doi.org/10.1186/s13054-018-2124-8
Gallet R, Ternacle J, Damy T, Guendouz S, Bremont C, Seemann A et al (2014) Hemodynamic effects of Ivabradine in addition to dobutamine in patients with severe systolic dysfunction. Int J Cardiol 176:450–455. https://doi.org/10.1016/j.ijcard.2014.07.093
Chiu MH, Howlett JG, Sharma NC (2019) Initiation of ivabradine in cardiogenic shock. ESC Hear Fail 6:1088–1091. https://doi.org/10.1002/ehf2.12499
Lofrano-Alves MS, Issa VS, Biselli B, Chizzola P, Ayub-Ferreira SM, Bocchi EA (2016) Control of sinus tachycardia as an additional therapy in patients with decompensated heart failure (CONSTATHE-DHF): a randomized, double-blind, placebo-controlled trial. J Heart Lung Transplant 35:1260–1264. https://doi.org/10.1016/j.healun.2016.06.005
Nuding S, Schröder J, Presek P, Wienke A, Müller-Werdan U, Ebelt H et al (2018) Reducing elevated heart rates in patients with multiple organ dysfunction syndrome with the i f (Funny Channel Current) Inhibitor Ivabradine. Shock 49:402–411. https://doi.org/10.1097/SHK.0000000000000992
Cervetto L, Demontis GC, Gargini C (2007) Cellular mechanisms underlying the pharmacological induction of phosphenes. Br J Pharmacol 150:383–390. https://doi.org/10.1038/sj.bjp.0706998
Author information
Authors and Affiliations
Contributions
Juan Aranda and Juan Vilaro had the idea for the article.
Mohammed Elzeneini and Mohammad Al-Ani contributed to the literature review.
Mohammed Elzeneini contributed to the data analysis.
All authors contributed to the drafting and/or critical revision of the work.
All authors approved the final manuscript for submission.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Code availability
Not applicable
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Elzeneini, M., Aranda, J., Al-Ani, M. et al. Hemodynamic effects of ivabradine use in combination with intravenous inotropic therapy in advanced heart failure. Heart Fail Rev 26, 355–361 (2021). https://doi.org/10.1007/s10741-020-10029-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-020-10029-x