Abstract
Neu1 is a glycosidase that releases sialic acids from the non-reducing ends of glycoconjugates, and its enzymatic properties are conserved among vertebrates. Recently, Neu1-KO zebrafish were generated using genome editing technology, and the KO fish showed abnormal emotional behavior, such as low schooling, low aggressiveness, and excess exploratory behavior, accompanied by the downregulation of anxiety-related genes. To examine the alteration of neuronal and glial cells in Neu1-KO zebrafish, we analyzed the molecular profiles in the zebrafish brain, focusing on the midbrain and telencephalon. Using immunohistochemistry, we found that signals of Maackia amurensis (MAM) lectin that recognizes Sia α2-3 linked glycoconjugates were highly increased in Neu1-KO zebrafish brains, accompanied by an increase in Lamp1a. Neu1-KO zebrafish suppressed the gene expression of AMPA-type glutamate receptors such as gria1a, gria2a, and gria3b, and vesicular glutamate transporter 1. Additionally, Neu1-KO zebrafish induced the hyperactivation of astrocytes accompanied by an increase in Gfap and phosphorylated ERK levels, while the mRNA levels of astrocyte glutamate transporters (eaat1a, eaat1c, and eaat2) were downregulated. The mRNA levels of sypb and ho1b, which are markers of synaptic plasticity, were also suppressed by Neu1 deficiency. Abnormal activity of microglia was also revealed by IHC, and the expressions of iNOS and IL-1β, an inflammatory cytokine, were increased in Neu1-KO zebrafish. Furthermore, drastic neuronal degeneration was detected in Neu1-KO zebrafish using Fluoro-Jade B staining. Collectively, the neuronal and glial abnormalities in Neu1-KO zebrafish may be caused by changes in the excitatory neurotransmitter glutamate and involved in the emotional abnormalities.






Similar content being viewed by others
References
Tringali, C., Anastasia, L., Papini, N., Bianchi, A., Ronzoni, L., Cappellini, M.D., Monti, E., Tettamanti, G., Venerando, B.: Modification of sialidase levels and sialoglycoconjugate pattern during erythroid and erytroleukemic cell differentiation. Glycoconj. J. 24, 67–79 (2006). https://doi.org/10.1007/s10719-006-9013-0
Ryuzono, S., Takase, R., Kamada, Y., Ikenaga, T., Chigwechokha, P.K., Komatsu, M., Shiozaki, K.: Suppression of Neu1 sialidase delays the absorption of yolk sac in medaka (Oryzias latipes) accompanied with the accumulation of α2-3 sialo-glycoproteins. Biochimie 135, 63–71 (2017). https://doi.org/10.1016/j.biochi.2017.01.008
Creek, K.E., Walter, V.P., Evers, D., Yeo, E., Elliott, W.L., Heinstein, P.F., Morré, D.M., Morré, D.J.: Sialoglycoconjugate changes during 2-acetylaminofluorene-induced hepatocarcinogenesis in the rat. Biochim. Biophys. Acta - Lipids Lipid Metab. 793, 133–140 (1984). https://doi.org/10.1016/0005-2760(84)90314-X
Takahashi, Y., Yajima, A., Cisar, J.O., Konishi, K.: Functional analysis of the Streptococcus gordonii DL1 sialic acid-binding adhesin and its essential role in bacterial binding to platelets. Infect. Immun. 72, 3876–3882 (2004). https://doi.org/10.1128/IAI.72.7.3876-3882.2004
Shiozaki, K., Oishi, K., Honda, A.: Functional characterization of fish sialidases and their diversity among different orders. Trends Glycosci. Glycotechnol. 31, E7–E13 (2019). https://doi.org/10.4052/tigg.1518.1E
Miyagi, T., Wada, T., Yamaguchi, K., Hata, K.: Sialidase and malignancy: A minireview. Glycoconj. J. 20, 189–198 (2003). https://doi.org/10.1023/B:GLYC.0000024250.48506.bf
Uemura, T., Shiozaki, K., Yamaguchi, K., Miyazaki, S., Satomi, S., Kato, K., Sakuraba, H., Miyagi, T.: Contribution of sialidase NEU1 to suppression of metastasis of human colon cancer cells through desialylation of integrin β4. Oncogene 28, 1218–1229 (2009). https://doi.org/10.1038/onc.2008.471
Seyrantepe, V., Poupetova, H., Froissart, R., Zabot, M., Maire, I., Pshezhetsky, A.V.: Molecular pathology of NEU1 gene in sialidosis. Hum. Mutat. 22, 343–352 (2003). https://doi.org/10.1002/humu.10268
Khan, A., Sergi, C.: Sialidosis: A review of morphology and molecular biology of a rare pediatric disorder. Diagnostics. 8, 29 (2018). https://doi.org/10.3390/diagnostics8020029
Wang, D., Bonten, E.J., Yogalingam, G., Mann, L., d’Azzo, A.: Short-term, high dose enzyme replacement therapy in sialidosis mice. Mol. Genet. Metab. 85, 181–189 (2005). https://doi.org/10.1016/j.ymgme.2005.03.007
Arora, V., Setia, N., Dalal, A., Vanaja, M.C., Gupta, D., Razdan, T., Phadke, S.R., Saxena, R., Rohtagi, A., Verma, I.C., Puri, R.D.: Sialidosis type II: Expansion of phenotypic spectrum and identification of a common mutation in seven patients. Mol. Genet. Metab. Reports. 22, 100561 (2020). https://doi.org/10.1016/j.ymgmr.2019.100561
de Geest, N., Bonten, E., Mann, L., de Sousa-Hitzler, J., Hahn, C., d’Azzo, A.: Systemic and neurologic abnormalities distinguish the lysosomal disorders sialidosis and galactosialidosis in mice. Hum. Mol. Genet. 11, 1455–1464 (2002). https://doi.org/10.1093/hmg/11.12.1455
Annunziata, I., Patterson, A., Helton, D., Hu, H., Moshiach, S., Gomero, E., Nixon, R., d’Azzo, A.: Lysosomal NEU1 deficiency affects amyloid precursor protein levels and amyloid-β secretion via deregulated lysosomal exocytosis. Nat. Commun. 4, 2734 (2013). https://doi.org/10.1038/ncomms3734
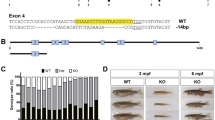
Okada, K., Takase, R., Hamaoka, Y., Honda, A., Ikeda, A., Hokazono, Y., Maeda, Y., Hayasaka, O., Kotani, T., Komatsu, M., Shiozaki, K.: Establishment and characterization of Neu1-knockout zebrafish and its abnormal clinical phenotypes. Biochem. J. 477, 2841–2857 (2020). https://doi.org/10.1042/bcj20200348
Ryuzono, S., Takase, R., Oishi, K., Ikeda, A., Chigwechokha, P.K., Funahashi, A., Komatsu, M., Miyagi, T., Shiozaki, K.: Lysosomal localization of Japanese medaka (Oryzias latipes) Neu1 sialidase and its highly conserved enzymatic profiles with human. Gene 575, 513–523 (2016). https://doi.org/10.1016/j.gene.2015.09.028
Honda, A., Chigwechokha, P.K., Takase, R., Hayasaka, O., Fujimura, K., Kotani, T., Komatsu, M., Shiozaki, K.: Novel Nile tilapia Neu1 sialidases: Molecular cloning and biochemical characterization of the sialidases Neu1a and Neu1b. Gene 742, 144538 (2020). https://doi.org/10.1016/j.gene.2020.144538
Shiozaki, K., Uezono, K., Hirai, G., Honda, A., Minoda, M., Wakata, R.: Identification of novel fish sialidase genes responsible for KDN-cleaving activity. Glycoconj. J. 37, 745–753 (2020). https://doi.org/10.1007/s10719-020-09948-6
Patton, E.E., Zon, L.I., Langenau, D.M.: Zebrafish disease models in drug discovery: from preclinical modelling to clinical trials. Nat. Rev. Drug Discov. 20, 611–628 (2021). https://doi.org/10.1038/s41573-021-00210-8
Ikeda, A., Komamizu, M., Hayashi, A., Yamasaki, C., Okada, K., Kawabe, M., Komatsu, M., Shiozaki, K.: Neu1 deficiency induces abnormal emotional behavior in zebrafish. Sci. Rep. 11, 13477 (2021). https://doi.org/10.1038/s41598-021-92778-9
Rosa, S.G., Quines, C.B., Stangherlin, E.C., Nogueira, C.W.: Diphenyl diselenide ameliorates monosodium glutamate induced anxiety-like behavior in rats by modulating hippocampal BDNF-Akt pathway and uptake of GABA and serotonin neurotransmitters. Physiol. Behav. 155, 1–8 (2016). https://doi.org/10.1016/j.physbeh.2015.11.038
Pollack, M.H., Jensen, J.E., Simon, N.M., Kaufman, R.E., Renshaw, P.F.: High-field MRS study of GABA, glutamate and glutamine in social anxiety disorder: Response to treatment with levetiracetam. Prog. Neuro-Psychopharmacol. Biol. Psychiatry. 32, 739–743 (2008). https://doi.org/10.1016/j.pnpbp.2007.11.023
Sild, M., Ruthazer, E.S., Booij, L.: Major depressive disorder and anxiety disorders from the glial perspective: Etiological mechanisms, intervention and monitoring. Neurosci. Biobehav. Rev. 83, 474–488 (2017). https://doi.org/10.1016/j.neubiorev.2017.09.014
Odaka, H., Numakawa, T., Soga, M., Kido, J., Matsumoto, S., Kajihara, R., Okumiya, T., Tani, N., Tanoue, Y., Fukuda, T., Furuya, H., Inoue, T., Era, T.: An iPSC-based neural model of sialidosis uncovers glycolytic impairment-causing presynaptic dysfunction and deregulation of Ca2+ dynamics. Neurobiol. Dis. 152, 105279 (2021). https://doi.org/10.1016/j.nbd.2021.105279
Oheda, Y., Kotani, M., Murata, M., Sakuraba, H., Kadota, Y., Tatano, Y., Kuwahara, J., Itoh, K.: Elimination of abnormal sialylglycoproteins in fibroblasts with sialidosis and galactosialidosis by normal gene transfer and enzyme replacement. Glycobiology 16, 271–280 (2006). https://doi.org/10.1093/glycob/cwj069
Brandão, M.L., Troncoso, A.C., de Souza Silva, M.A., Huston, J.P.: The relevance of neuronal substrates of defense in the midbrain tectum to anxiety and stress: empirical and conceptual considerations. Eur. J. Pharmacol. 463, 225–233 (2003). https://doi.org/10.1016/S0014-2999(03)01284-6
Tsubokawa, T., Saito, K., Kawano, H., Kawamura, K., Shinozuka, K., Watanabe, S.: Pharmacological effects on mirror approaching behavior and neurochemical aspects of the telencephalon in the fish, medaka (Oryzias latipes). Soc. Neurosci. 4, 276–286 (2009). https://doi.org/10.1080/17470910802625215
Yogalingam, G., Bonten, E.J., van de Vlekkert, D., Hu, H., Moshiach, S., Connell, S.A., d’Azzo, A.: Neuraminidase 1 is a negative regulator of lysosomal exocytosis. Dev. Cell. 15, 74–86 (2008). https://doi.org/10.1016/j.devcel.2008.05.005
Daniels, R.W., Collins, C.A., Chen, K., Gelfand, M.V., Featherstone, D.E., DiAntonio, A.: A single vesicular glutamate transporter is sufficient to fill a synaptic vesicle. Neuron 49, 11–16 (2006). https://doi.org/10.1016/j.neuron.2005.11.032
Song, I., Huganir, R.L.: Regulation of AMPA receptors during synaptic plasticity. Trends Neurosci. 25, 578–588 (2002). https://doi.org/10.1016/S0166-2236(02)02270-1
Gao, L., Penglee, R., Huang, Y., Yi, X., Wang, X., Liu, L., Gong, X., Bao, B.: CRISPR/Cas9-induced nos2b mutant zebrafish display behavioral abnormalities. Genes, Brain Behav. 20, (2021). https://doi.org/10.1111/gbb.12716
Norden, D.M., Trojanowski, P.J., Villanueva, E., Navarro, E., Godbout, J.P.: Sequential activation of microglia and astrocyte cytokine expression precedes increased iba-1 or GFAP immunoreactivity following systemic immune challenge. Glia 64, 300–316 (2016). https://doi.org/10.1002/glia.22930
Li, D., Tong, L., Kawano, H., Liu, N., Yan, H., Zhao, L., Li, H.: Regulation and role of ERK phosphorylation in glial cells following a nigrostriatal pathway injury. Brain Res. 1648, 90–100 (2016). https://doi.org/10.1016/j.brainres.2016.07.008
Kyrkanides, S., Olschowka, J.A., Williams, J.P., Hansen, J.T., O’Banion, M.K.: TNFα and IL-1β mediate intercellular adhesion molecule-1 induction via microglia–astrocyte interaction in CNS radiation injury. J. Neuroimmunol. 95, 95–106 (1999). https://doi.org/10.1016/S0165-5728(98)00270-7
Tang, Y., Le, W.: Differential roles of M1 and M2 microglia in neurodegenerative diseases. Mol. Neurobiol. 53, 1181–1194 (2016). https://doi.org/10.1007/s12035-014-9070-5
Cheng, X., Xie, Y., Zhou, B., Huang, N., Farfel-Becker, T., Sheng, Z.: Characterization of LAMP1-labeled nondegradative lysosomal and endocytic compartments in neurons. J. Cell Biol. 217, 3127–3139 (2018). https://doi.org/10.1083/jcb.201711083
Arantes, R.M.E., Andrews, N.W.: A role for synaptotagmin VII-regulated exocytosis of lysosomes in neurite outgrowth from primary sympathetic neurons. J. Neurosci. 26, 4630–4637 (2006). https://doi.org/10.1523/JNEUROSCI.0009-06.2006
Ibata, K., Yuzaki, M.: Destroy the old to build the new: Activity-dependent lysosomal exocytosis in neurons. Neurosci. Res. 167, 38–46 (2021). https://doi.org/10.1016/j.neures.2021.03.011
Kreher, C., Favret, J., Maulik, M., Shin, D.: Lysosomal functions in glia associated with neurodegeneration. Biomolecules 11, 400 (2021). https://doi.org/10.3390/biom11030400
Frischknecht, R., Heine, M., Perrais, D., Seidenbecher, C.I., Choquet, D., Gundelfinger, E.D.: Brain extracellular matrix affects AMPA receptor lateral mobility and short-term synaptic plasticity. Nat. Neurosci. 12, 897–904 (2009). https://doi.org/10.1038/nn.2338
Nordman, J.C.: Anger management: Mechanisms of glutamate receptor-mediated synaptic plasticity underlying animal aggression. Int. J. Biochem. Cell Biol. 142, 106120 (2022). https://doi.org/10.1016/j.biocel.2021.106120
Savotchenko, A., Romanov, A., Isaev, D., Maximyuk, O., Sydorenko, V., Holmes, G.L., Isaeva, E.: Neuraminidase inhibition primes short-term depression and suppresses long-term potentiation of synaptic transmission in the rat hippocampus. Neural Plast. 2015, 908190 (2015). https://doi.org/10.1155/2015/908190
Kawashima, N., Tsuji, D., Okuda, T., Itoh, K., Nakayama, K.: Mechanism of abnormal growth in astrocytes derived from a mouse model of GM2 gangliosidosis. J. Neurochem. 111, 1031–1041 (2009). https://doi.org/10.1111/j.1471-4159.2009.06391.x
Oakley, R.H., Whirledge, S.D., Petrillo, M.G., Riddick, N.V., Xu, X., Moy, S.S., Cidlowski, J.A.: Combinatorial actions of glucocorticoid and mineralocorticoid stress hormone receptors are required for preventing neurodegeneration of the mouse hippocampus. Neurobiol. Stress. 15, 100369 (2021). https://doi.org/10.1016/j.ynstr.2021.100369
Qin, Y., Chen, Y., Yang, J., Wu, F., Zhao, L., Yang, F., Xue, P., Shi, Z., Song, T., Huang, C.: Serum glycopattern and Maackia amurensis lectin-II binding glycoproteins in autism spectrum disorder. Sci. Rep. 7, 46041 (2017). https://doi.org/10.1038/srep46041
Kim, H., Lim, C., Kaang, B.: Neuronal mechanisms and circuits underlying repetitive behaviors in mouse models of autism spectrum disorder. Behav. Brain Funct. 12, 3 (2016). https://doi.org/10.1186/s12993-016-0087-y
Vakilzadeh, G., Falcone, C., Dufour, B., Hong, T., Noctor, S.C., Martínez-Cerdeño, V.: Decreased number and increased activation state of astrocytes in gray and white matter of the prefrontal cortex in autism. Cereb. Cortex. in press (2022). https://doi.org/10.1093/cercor/bhab523
Xiao, L., Yan, J., Feng, D., Ye, S., Yang, T., Wei, H., Li, T., Sun, W., Chen, J.: Critical role of TLR4 on the microglia activation induced by maternal LPS exposure leading to ASD-like behavior of offspring. Front. Cell Dev. Biol. 9, 634837 (2021). https://doi.org/10.3389/fcell.2021.634837
Acknowledgements
We appreciate the support of Dr. Yumiko Yoshizaki, Dr. Shinji Kanda, Dr. Takanori Ikenaga, and the technical assistance of Mika Ishii, Momoko Kawabe, Chihoko Horita, Takumi Nishida, Kanta Miyamoto, Toshiki Hyodo, and Shoji Kodama. The financial support from Sankei Science Foundation is gratefully acknowledged.
Author information
Authors and Affiliations
Contributions
Conceptualization: Asami Ikeda, and Kazuhiro Shiozaki; Methodology: Asami Ikeda, Chiharu Yamasaki, and Kazuhiro Shiozaki; Formal analysis and investigation: Asami Ikeda, Chiharu Yamasaki, Yurina Kubo, Yudai Doi, Mayu Komamizu, and Kazuhiro Shiozaki; Writing -original draft preparation: Asami Ikeda and Kazuhiro Shiozaki; Writing review and editing: Masaharu Komatsu and Kazuhiro Shiozaki; Supervision: Masaharu Komatsu and Kazuhiro Shiozaki.
Corresponding author
Ethics declarations
Competing interests
The authors have no conflicts of interest to declare.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ikeda, A., Yamasaki, C., Kubo, Y. et al. Alteration of the neuronal and glial cell profiles in Neu1-deficient zebrafish. Glycoconj J 39, 499–512 (2022). https://doi.org/10.1007/s10719-022-10074-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10719-022-10074-8