Abstract
Since air pollution compromise the respiratory system and COVID-19 disease is caused by a respiratory virus, it is expected that air pollution plays an important role in the current COVID-19 pandemic. Exploratory studies have observed positive associations between air pollution and COVID-19 cases, deaths, fatality, and mortality rate. However, no study focused on Brazil, one of the most affected countries by the pandemic. Thus, this study aimed to understand how long-term exposure to PM10, PM2.5, and NO2 contributed to COVID-19 fatality and mortality rates in São Paulo state in 2020. Air quality data between 2015 and 2019 in 64 monitoring stations within 36 municipalities were considered. The COVID-19 fatality was calculated considering cases and deaths from the government’s official data and the mortality rate was calculated considering the 2020 population. Linear regression models were well-fitted for PM2.5 concentration and fatality (R2 = 0.416; p = 0.003), NO2 concentration and fatality (R2 = 0.232; p = 0.005), and NO2 concentration and mortality (R2 = 0.273; p = 0.002). This study corroborates other authors’ findings and enriches the discussion for having considered a longer time series to represent long-term exposure to the pollutants and for having considered one of the regions with the highest incidence of COVID-19 in the world. Thus, it reinforces measures to reduce the concentration of air pollutants which are essential for public health and will increase the chance to survive in future respiratory disease epidemics.
Similar content being viewed by others
Introduction
The current coronavirus disease (COVID-19) pandemic through the spreading of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has triggered serious consequences to global health, healthcare systems, and economics, resulting in millions of human lives losses and huge social costs. As of December 31st, 2021, COVID-19 has caused more than 5.4 million deaths worldwide, with an average case fatality of 1.8%, varying by region (López-Feldman et al., 2021; WHO, 2021a; Worldometers, 2021).
At the beginning of the COVID-19 pandemic, human-to-human transmission was set as the main form of contagion. As the disease spread around the world and data from the most affected locations were studied, it was possible to note the great contribution of weather conditions and also of air pollution in the spread of the SARS-CoV-2 virus. Low wind speed associated with elevated concentrations of air pollutants favors the virus permanence in the air, so cities with these conditions are more likely to present high transmission rates (Coccia, 2021a, b). According to Coccia (2020), the analysis of 55 Italian cities reveals that air pollution-to-human transmission (airborne viral infectivity) seemed to be more relevant than human-to-human transmission. Besides wind speed and air pollutants concentration, the SARS-CoV-2 infectivity has already been related to temperature, relative humidity, and precipitation (Srivastava, 2021). In this sense, higher temperatures and relative humidity reduce the virus viability, and lower temperatures, the presence of drew or frost points, and precipitation increase the virus infectivity (Sarkodie & Owusu, 2020).
COVID‐19 symptoms differ among patients and may include fever, cough, breathing difficulties, loss of smell, multiple organ dysfunction, and asymptomatic cases may also occur, according to the World Health Organization (WHO, 2021b). Moreover, older age, obesity, immunodeficiency, pre-existing chronic non-communicable diseases, and respiratory disorders are the major risk factors for mortality (Noor & Islam, 2020; Rothan & Byrareddy, 2020; Simonnet et al., 2020). Given the complexity of this new disease, it is challenging to understand the multiple factors involved in its development and spread.
Ambient air pollution is a well-known threat to global health. Many previous studies support the close relationship between exposure to air pollutants and several adverse health impacts, such as morbidity and mortality related to neurodevelopmental and neurodegenerative disorders, heart disease, stroke, asthma, bronchitis, chronic obstructive pulmonary disease, and lung cancer (Chen et al., 2017; Gharibvand et al., 2016; Landrigan et al., 2018; Lim et al., 2018). Moreover, it is important to highlight the association with infectious diseases and ambient air pollutants, observed in epidemic events, such as influenza seasons (Feng et al., 2016; Liang et al., 2014) and the 2003 Severe Acute Respiratory Syndrome (SARS) outbreak (Cui et al., 2003), in China. Besides SARS-CoV-2 being highly transmissible, COVID-19 is primarily a respiratory disease; therefore, understanding how air pollution might be either a contributing factor to this disease outcome or susceptibility is a topic of growing interest for this current global health crisis.
The influence of air pollution on public health can be understood from two different perspectives: short-term and long-term exposure. The health effects resulting from short-term exposure were described first, often associated with acute episodes of air pollution in the initial decades of the twentieth century. A classical description of these health effects occurred after the London Smog in 1952 (Wilkins, 1954). Currently, in this type of study, models such as Generalized Linear or Generalized Additive Models (GLM and GAM) are fitted to associate the increase in health outcomes such as death or hospitalization with episodes of worsening air quality. More recently, the long-term exposure effects of air pollution (i.e., living for years in an urban center) have been widely described. For instance, long-term exposure to air pollutants from vehicles (living near to traffic roads) has already been associated with lung cancer death, increased mediators of systemic inflammation in the bloodstream of adults, lower cognitive development in primary school children, and a higher probability of developing dementia (in the elderly) and asthma (in children) (Bidoli et al., 2016; Lanki et al., 2015; McConnell et al., 2010; Sunyer et al., 2015).
The relationship between air quality and COVID-19 was first described by Conticini et al. (2020) in Northern Italy and, according to the authors, the high levels of air pollution in Lombardy and Emilia Romagna might explain why these regions registered the highest level of virus fatality in the world at the beginning of the pandemic. After this study, similar ones were conducted in different regions of the world (Table 1). The effects of air pollution in the COVID-19 pandemic have been described both in terms of short-term exposure (using air quality data from the epidemic period) and long-term exposure (using air quality data from past periods).
Table 1 summarizes the most relevant results discussed in the systematic review published by Copat et al. (2020), as well as including more recent studies that were published until August 2021. Most authors focused their attention to examine the effects of air pollution on COVID-19 outcomes, in terms of PM2.5, PM10, and NO2 exposures. PM2.5 was the most explored pollutant, as it was the object of investigation in all studies. These studies support the evidence that exposure to PM2.5 and NO2 exerts a greater influence on COVID-19 outcomes, such as case, fatality rate, and mortality rate. The contribution of PM10 seems to be less significant and other pollutants, such as O3, show controversial results. China, the USA, Italy, and some locations of the Latin America and the Caribbean (LAC) Region were the main explored areas. However, studies that specifically investigated Brazilian data were not found.
In 2020, Brazil was the 2nd country with more COVID-19 deaths (194,149 deaths) and the 23rd considering deaths per population rate (917 deaths per million) (Our world in data, 2021). Despite this being a tragic scenario, it makes Brazil a propitious place to study the COVID-19 disease. According to Rosario et al. (2020), Brazilian solar radiation is a climatic factor that suppresses the spread of COVID-19. Even so, Brazil was one of the countries that stood out the most during the first year of the pandemic (including placing the emergence of new variants of the SARS-COV-2 virus). Brazil was analyzed in two previous studies mentioned in Table 1. Neither Yu et al. (2021) nor Bolaño-Ortiz et al. (2020) investigated the air pollution influence on COVID-19 fatality or mortality rates, focusing on the number of cases and deaths separately. Yu et al. (2021) studied the effects of long-term exposure to PM2.5 in a global analysis. They noticed that there is a positive correlation between deaths per million population and PM2.5 concentration. However, it cannot be understood as higher COVID-19 fatality since they also found a positive correlation between cases per million population and PM2.5 concentration (Yu et al., 2021). Bolaño-Ortiz et al. (2020) studied the effects of short-term exposure to PM2.5, PM10, and NO2 pollutants and found a positive correlation between these pollutants and COVID-19 cases and mortality in São Paulo, Brazil.
Considering that long-term exposure to air pollutants may have a significant influence on COVID-19 fatality and mortality rates since it compromises the respiratory system and that this association has not been yet demonstrated in Brazil, which is one of the pandemic hotspots, this study aimed to understand how long-term exposure to air pollutants contributed to COVID-19 fatality and mortality rates in São Paulo, the most populous Brazilian state.
Materials and methods
Study area
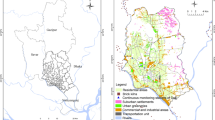
Brazil is the 5th largest country in the world with 8.36 million km2 and has 212 million inhabitants (The World Bank, 2021). In this study, only São Paulo state was considered, because it is the only Brazilian state with a robust air quality monitoring network, with 64 automatic stations and 22 manual monitoring points across the 248,209 Km2 state area (Fig. 1) (CETESB, 2021).
The first case of COVID-19 in Brazil was registered in the city of São Paulo (capital of the state) in a person who had been in Italy. As the main Brazilian airport is located in the São Paulo state, people from different areas pass through the region. This fact has favored both the spread of the disease at the beginning of the pandemic and the spread of new variants of SARS-CoV-2. In 2020, 24% of all COVID-19 deaths registered in Brazil occurred in São Paulo state. If São Paulo state was a country, it would be the 12th country with more COVID-19 deaths in 2020 (Our world in data, 2021; SEADE, 2021a).
São Paulo state occupies only 2.9% of the Brazilian area. However, it is the most populous, presenting 22% of its population. The projection based on the last Brazilian census estimates that 44.9 million people are living in the 645 municipalities of São Paulo state (SEADE, 2021b). In 2020, São Paulo’s Gross Domestic Product (GDP) was about US$ 447,447 million, representing 31% of Brazilian GDP (SEADE, 2021c).
Data sources and considerations
To investigate the association between previous exposure to air pollutants and COVID-19, it was considered air quality data from 2015 to 2019. The air quality in 2020 was not considered because social isolation implied lower levels of air pollution in some regions and these lower levels are uncharacteristic of the population’s daily exposure through the years (Debone et al., 2020).
The pollutants considered were the particulate matter with less than 10 µm of diameter (PM10), particulate matter with less than 2.5 µm of diameter (PM2.5), and nitrogen dioxide (NO2). These are the pollutants more frequently considered in the previous studies conducted in other countries (see Table 1) and they are also consistently monitored in the state. Between 2015 and 2019, PM10 was monitored at 36 municipalities (60 monitoring stations), PM2.5 at 19 municipalities (31 monitoring stations), and NO2 at 32 municipalities (51 monitoring stations). The annual mean concentration of each pollutant was consulted on the São Paulo’s environmental agency database (named QUALAR). When there was more than one monitoring station in the same city, the annual air quality was considered as the mean. The population exposure to the pollutants through the years was considered as the mean concentration between 2015 and 2019 in each municipality.
COVID-19 data (cases and deaths) were consulted in the official São Paulo state report of December 31st, 2020. The COVID-19 fatality was considered as the rate between all death registered in each city until December, 31st and all cases in the same period. The mortality rate was defined as the ratio between all deaths registered in 2020 and the official estimated population for the same year. The year 2021 was not considered, because Brazilian Health System collapsed. There was a list of patients who needed hospitalization with people from all over the state and they were transported according to the availability of lays. So, deaths registered in one city were not necessarily of inhabitants of this specific city. Another consequence of the collapse was that there were deaths as a result of lack of medical care, which considerably increased the COVID-19 fatality and mortality rates.
Statistical analysis
Six independent linear regression analyses were performed in order to investigate the association between fatality rate and the previous exposure to PM10, PM2.5 and NO2 and between mortality rate and the exposure to these three pollutants. The dependent variable was considered as the COVID-19 fatality or mortality rate in each city and the independent variable was considered as the mean pollutant concentration in the previous years. The linear regression model is presented in Eq. (1).
In which \({Y}_{i}\) is the response variable; \({\beta }_{0}\) is the intercept; \({\beta }_{1}\) is the inclination; \({X}_{1}\) is the predictor variable; and \({\varepsilon }_{i}\) is the aleatory error.
Besides the regression model, a Pearson coefficient analysis was performed to measure the extent of the relationship between the variables.
Both analyses were performed in the IBM SPSS Statistics 20 Software and p-value < 0.05 was considered as statistically significant.
Results
The municipalities considered in this study and the descriptive data about the COVID-19 fatality and mortality rates, air quality, population, and GDP are presented in Table 2. The 36 cities altogether summed more than 925,000 cases and almost 32,000 deaths in 2020. The population of these cities varied from 26,572 to 11,914,851 inhabitants, representing 66% of the state population, performing a GDP from US$340,193,079 to US$137,439,108,165, about 66% of the state production, evidencing the relevance and representativeness of the chosen municipalities. The average fatality rate in these municipalities was 2.9%. The COVID-19 disease was the least lethal in Araraquara city (1.15%) and the most lethal in Guarulhos (6.10%). The average mortality rate was 110.9 deaths per 105 inhabitants. The highest mortality rate was registered in Santos city (210.6 deaths per 105 inhabitants) and the lowest was registered in Araraquara (39.3 deaths per 105 inhabitants). Regarding air quality, the mean annual concentrations of PM10 ranged between 19.7 and 53.0 µg/m3 (average = 28.7 ± 7.4), PM2.5 between 10.0 and 22.0 µg/m3 (average = 15.6 ± 2.8), and NO2 between 9.0 and 46.4 µg/m3 (average = 22.4 ± 9.5).
The Pearson correlation analyses revealed positive relationships between COVID-19 fatality rate and the concentrations of pollutants PM2.5 and NO2 (p = 0.001 and p = 0.003, respectively). The correlation was stronger for PM2.5 than NO2 (R2 = 0. 416 and R2 = 0.232, respectively). Between COVID-19 mortality rate and the pollutants’ concentrations, the Pearson correlation was significant for the pollutants PM10 and NO2 (p = 0.03 and p = 0.001, respectively). The relation was considered very low between PM10 exposure and mortality rate (R2 = 0.097) and low between NO2 exposure and mortality rate (R2 = 0.273).
The linear regression models were well-fitted in the relationships between the fatality and PM2.5 and NO2 concentrations (ANOVA test p = 0.003 for PM2.5 and p = 0.005 for NO2) and between mortality rate and NO2 concentration (ANOVA test p = 0.002). The model did not fit into the relationship between COVID-19 fatality and PM10 concentration (ANOVA test p = 0.520) and between COVID-19 mortality and PM10 and PM2.5 concentrations (ANOVA test p = 0.065 for MP10 and p = 0.202 for MP2.5). Figure 2 presents the graphs which illustrate each model.
Scatter plots showing the relation between COVID-19 fatality or mortality rates and PM10, PM2.5, and NO2 concentrations in the previous years in the 36 Brazilian municipalities. The numbers signed in the graphs represent the municipalities presented in Table 2. Figure elaborated by the authors in the IBM SPSS Statistics 20 Software
Some municipalities presented fatality or mortality rates that could not be explained by the models (exceeding the 95% confidence interval). The fatality rate registered in Guarulhos city (6.10%) did not fit in any of the three performed models and the one registered in Mogi das Cruzes city (4.73%) did not fit into the NO2 model. Regarding mortality rates, the cities of Santos and São José do Rio Preto (210.63 and 203.61 deaths per 105 inhabitants, respectively) did not fit into the NO2 model.
Discussion
Ambient air pollution is widely recognized as a risk factor for all-cause of deaths and cardiopulmonary diseases (Beelen et al., 2014; Gharibvand et al., 2016; Landrigan et al., 2018; Zhao et al., 2020; Zhu et al., 2019). However, the relationship between air pollutants exposure and viral respiratory infections has been poorly investigated. Cui et al. (2003) found that Chinese regions with a moderate long-term air pollution index (API) were related with a 126% case fatality rate higher than locations with low API, during the 2003 SARS outbreak. In a similar vein, Liang et al. (2014) and Feng et al. (2016) reported that PM2.5 concentrations were significantly related to cases and influenza-like illness (ILI) risk, respectively, during the flu season of Beijing.
Several works are now emerging, reporting close relation between air pollutants exposure and COVID-19 outcomes, such as deaths, fatality, and mortality rates (Table 1). PM2.5 was the most explored among the authors. Furthermore, these studies support the evidence that the long-term exposure of PM2.5 exerts an important influence on COVID-19 outcomes, as shown in Yu et al. (2021) that found that deaths per million population were positive correlated with PM2.5 (r = 0.419, p < 0.01), using a satellite-derived PM2.5 concentration of 251 countries, from 2016. Páez-Osuna et al. (2021) carried a study in Mexico and showed a significant relationship between cumulative mortality rates and PM2.5 emissions from vehicles (r = 0.616, p < 0.005), considering data from the last 37 years. Borro et al. (2020) reported positive correlations between PM2.5 and mortality rate (r = 0.65, p < 0.0001) and case fatality rate (r = 0.7, p < 0.0001), considering PM2.5 data of days before the first reported cases in Italy. In opposite to what was found in our study, Vasquez-Apestegui et al. (2021) estimated a significant association between long-term exposure to PM2.5 and COVID-19 mortality in Peru; however, they did not observe this relationship for the lethality rate. The discrepant results between the investigations suggest that the better variable (fatality or mortality rate) to have the relationship with long-term exposure to air pollutants depends on the specific characteristics as which are the analyzed cities, socioeconomic indicators, quality of healthcare services, etc.
In several instances, the results related to long-term exposure of NO2 also has shown a close relation between COVID-19 outcomes, as evidenced by Travaglio et al. (2021) that reported that a 1-µg/m3 increase in NO2 was associated with 3.1% more deaths, but 1-µg/m3 increase in PM2.5 was associated with 12% more cases, considering air pollution data from 2018 of England. Konstantinoudis et al. (2021) found that a 1-µg/m3 increase in PM2.5 and NO2 was associated with a 1.4% and 0.5% increase in mortality risk in England, respectively, considering air pollution data from 2014 to 2018. Chakraborty et al. (2020), using the pollution data from the year before the COVID-19 pandemic, found a positive correlation between NO2 and both the absolute number of deaths (r = 0.79, p < 0.05) and case fatality rate (r = 0.74, p < 0.05), in India.
Our findings are consistent with previous studies, since we also showed a significant positive correlation between COVID-19 fatality rate and air pollutants long-term exposure, considering PM2.5 and NO2 concentrations (R2 = 0.416 and R2 = 0.232, respectively) and between COVID-19 mortality rate and previous exposure to NO2 (R2 = 0.273). Specifically, our model for PM2.5 resulted in metrics with a similar range of values to those presented by Borro et al. (2020). Regarding the association between NO2 concentration and COVID-19 fatality rate, our results were more moderate than those presented by Chakraborty et al. (2020); however, it is important to highlight that India has one of the highest rates of air pollution in the world and the authors had data available from 207 air quality monitoring stations in 128 cities, which may justify a lower value metric for our model.
The relationship between PM10 concentration and COVID-19 (cases, deaths, or fatalities) was explored by fewer authors (Table 1). Since this pollutant penetrates less deeply into the airways than smaller diameter PM and gases, the concentration of PM10 is often used in models that assess the health effects of short-term exposure. In this context, the increase in the concentration of this pollutant is especially associated with an increase in daily hospitalizations or deaths of people with chronic diseases or those affecting the cardiorespiratory system (Anderson et al., 2012). In this vein, Zhu et al. (2020) and Bolaño-Ortiz et al. (2020) noted the effects of short-term exposure to PM10 on the number of COVID-19 cases and mortality, respectively. The analysis of health effects resulting from long-term exposure to PM10 is present in the bibliography, although it is not included in the main models recommended by the WHO (Ostro, 2004; Pascal et al., 2011). Positive associations between prior and systemic exposure to PM10 and the increase in COVID-19 cases and fatality were described by Travaglio et al. (2021) and Yao et al. (2020), respectively. However, these associations were lower than those found between the exposure to PM2.5 and the same outcomes. It is noteworthy that the concentration of PM2.5 is usually between 50 and 70% of the concentration of PM10 (Ostro, 2004; Pascal et al., 2011); thus, given the existence of a relationship between PM2.5 long-term exposure and health outcomes, it is also possible to have similar results concerning PM10, even if such outcomes are not a direct consequence of this pollutant, but rather of PM2.5. In the present study, neither the Pearson correlation nor the regression model fitted the relationship between COVID-19 fatality and previous exposure to PM10. Regarding the COVID-19 mortality rate, it was found an almost insignificant Pearson correlation with previous PM10 exposure (R2 = 0.097; p = 0.033) and the linear regression model did not fit into the variables (ANOVA test p = 0.065).
Moreover, it is important to point out that the effect of exposure to air pollutants on COVID‐19 outcomes varied within regions. Several factors can explain the divergences, such as differences in lockdown policies and strategies, socioeconomic indicators, quality of healthcare services, geographical location, and meteorological parameters (Ali et al., 2021). For instance, a comparative study among China, England, Germany, and Japan indicated that the population density and absolute humidity influence both the SARS-COV-2 spread and the decay duration of the pandemic (Diao et al., 2021).
In our analysis, Guarulhos city presented the higher COVID-19 fatality rate, which could not be explained either by PM2.5 or NO2 previous exposure. However, the COVID-19 mortality rate did not configure an outlier in the COVID-19 mortality rate models. It suggests that Guarulhos inhabitants were less tested for the disease in 2020. In this sense, the major tests were performed in people which needed medical care, so the observed fatality rate was very higher than the predicted one. Furthermore, the mortality rate in Santos and São José do Rio Preto municipalities could not be explained by NO2 previous exposure. Despite presenting a lower population density compared to the others (1494 and 945 inhabitants per km2 in Santos and São José do Rio Preto respectively), these cities are, respectively, the 1st and the 3rd cities with the higher proportion of elderly people in the population. In Santos, 21.50% of the inhabitants are older than 60 years; in São José do Rio Preto, the proportion is 15.40%. So, the elevated mortality rate registered in these cities is probably related to their population age structure. According to Coccia (2021c), high expenditures in the health sector (> 7.5% of GDP) may reduce the fatality rates even in places with a great percentage of elderly people.
Climatic and meteorological factors seem to be less related to the high rates described for these municipalities. Santos, for example, is a coastal city with high averages of temperature, relative humidity, and wind speed throughout the year. São José do Rio Preto is among the three cities with the highest annual thermal average.
Besides small airborne particulate matter being widely recognized as more dangerous to human health since it can penetrate deeply into the respiratory tract, chronic exposure to PM2.5 has been related to overexpression of the angiotensin-converting enzyme 2 (ACE-2) in mice (Aztatzi-Aguilar et al., 2015; Lin et al., 2018). ACE-2 was reported as an important entry receptor for SARS-CoV-2 since the S1 subunit of the viral spike (S) protein binds to human ACE-2 in the alveoli (Babadaei et al., 2020; Beyerstedt et al., 2021). Considering that the alveolar level only can be reached by small airborne particulate matter, the link between chronic exposure to air pollution and COVID-19 fatality can be explained, since high levels of PM2.5 could overexpress ACE-2 facilitating viral penetration (Frontera et al., 2020).
The effects of the air pollution on the COVID-19 pandemic may go beyond the increased fatality rate due to pulmonary impairment, especially in the most susceptible population. Recent studies have been demonstrating that aerosols are capable of carrying the SARS-CoV-2 virus (Asadi et al., 2020; Greenhalgh et al., 2021). In this way, in regions with high local levels of aerosols in the atmosphere, disease transmission can be optimized. In Mexico, during June 2020 Saharan dust event, it was possible to find a positive association between PM levels and the daily number of COVID-19 cases and deaths (Kutralam-Muniasamy et al., 2021).
Furthermore, in predominantly urban regions, such as most municipalities analyzed in this study, exposure to PM2.5 is accompanied by NO2, as they are generally positively correlated, emitted from a common source. In Sao Paulo, vehicles are responsible for 62.5% of nitrogen oxides and 37% of PM2.5 emissions (CETESB, 2021). Considering that NO2 is a deep lung irritant with high oxidative potential, that increases inflammatory response and cellular injury, chronic exposure to this pollutant may promote viral activity due to the lung defense disruption and tissue damage caused by oxidative stress, increasing the COVID-19 patients’ vulnerability (Frontera et al., 2020).
The present study corroborates the main findings on the relationship between long-term exposure to PM2.5 and NO2 and COVID-19. It also reveals that, in São Paulo state (Brazil), the fatality rate is a better variable to explore its association with air pollutants’ exposure than mortality rate and that PM2.5 is the best pollutant for such model. The study relevance is highlighted by the use of statistical models, which support the first descriptive associations on the theme (such as that by Conticini et al. in 2020), by using a longer time series to demonstrate the long-term exposure and by the studied area, which has consolidated among the regions with the highest incidence of COVID-19 in the world. Despite this, some limitations should be mentioned. The first is the scarcity of air quality monitoring stations in Brazil. This limited the area of analysis to the state of São Paulo. The second limitation is the evident underreporting of COVID-19 cases and deaths. At the beginning of the pandemic, tests to detect the disease were scarce and they were used only in hospitalized patients. The fact that only patients with complications were tested may have resulted in a generally overestimated fatality. We suppose that Guarulhos city presented the higher fatality rate because, in the city, the tests were applyed mostly in hospitalized people. This supposition could not be verified, because Brazilian Health Ministry does not disclose the number of tested people per city. Even among the deceased, underreporting throughout 2020 is evident. The lack of tests and the government’s pressure to minimize the severity of the COVID-19 pandemic led many health professionals to attribute deaths that were possibly due to COVID-19 to other causes. In the state of São Paulo, deaths due to respiratory distress syndrome (ICD-10 J80) between 2017 and 2019 were 71, 106, and 94 and, in 2020, they increased to 377 (DATASUS, 2021). Regarding deaths from acute respiratory failure (ICD-10 J96), they were 359, 334, 327 in 2017, 2018, and 2019 respectively, and, in 2020, they increased to 643 (DATASUS, 2021). The historical series of deaths from severe acute respiratory syndrome (SARS; ICD-10 U04) were hidden from the official platform of the Ministry of Health of Brazil, revealing the lack of government transparency about the pandemic. Considering the notary’s office data, deaths registered by SARS in Brazil jumped from 293 in 2019 to 2422 in 2020 (Cartórios de Registro Civil do Brasil, 2021). The National Council of Health Departments estimates that, in 2020, there were 275,587 exceed deaths in Brazil probably due to COVID-19, but reported due to other causes (CONASS, 2021).
Our work, by presenting a significant correlation between COVID-19 fatality and long-term exposure to air pollutants, reinforces the relevant debate on the urgency of improving strategies for sustainable practices in urban centers, especially regarding air pollution control measures, since it can bring direct benefits to human health, especially in the context of this current global health crisis.
Conclusion
The COVID-19 pandemic is bringing a lot of learning to the world. In the search for an understanding of how the disease behaves and what are the associated risk factors, one more harmful effect of air pollution is perceived. The present study found a positive correlation between long-term exposure to PM2.5 and NO2 pollutants in the 5 years previous to the pandemic and COVID-19 fatality rate (R2 = 0.416 and R2 = 0.232, respectively). It was also found a positive correlation between long-term exposure to NO2 pollutant in the 5 years previous to the pandemic and COVID-19 mortality rate (R2 = 0.273). These results reinforce that measures to reduce the concentration of pollutants are essential for public health and will increase the chance of survival in future epidemics of respiratory diseases.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Ali, N., Fariha, K. A., Islam, F., Mishu, M. A., Mohanto, N. C., Hosen, M. J., & Hossain, K. (2021). Exposure to air pollution and COVID-19 severity: A review of current insights, management, and challenges. Integrated Environmental Assessment and Management. https://doi.org/10.1002/ieam.4435
Anderson, J. O., Thundiyil, J. G., & Stolbach, A. (2012). Clearing the air: A review of the effects of particulate matter air pollution on human health. Journal of Medical Toxicology, 8(2), 166–175. https://doi.org/10.1007/s13181-011-0203-1
Asadi, S., Bouvier, N., Wexler, A. S., & Ristenpart, W. D. (2020). The coronavirus pandemic and aerosols: Does COVID-19 transmit via expiratory particles?. Aerosol Science and Technology, 54(6), 635–638. https://doi.org/10.1080/02786826.2020.1749229
Aztatzi-Aguilar, O. G., Uribe-Ramírez, M., Arias-Montaño, J. A., Barbier, O., & De Vizcaya-Ruiz, A. (2015). Acute and subchronic exposure to air particulate matter induces expression of angiotensin and bradykinin-related genes in the lungs and heart: Angiotensin-II type-I receptor as a molecular target of particulate matter exposure. Particle and Fibre Toxicology, 12(1), 1–18. https://doi.org/10.1186/s12989-015-0094-4
Babadaei, M. M. N., Hasan, A., Bloukh, S. H., Edis, Z., Sharifi, M., Kachooei, E., & Falahati, M. (2020). The expression level of angiotensin-converting enzyme 2 determines the severity of COVID-19: Lung and heart tissue as targets. Journal of Biomolecular Structure and Dynamics. https://doi.org/10.1080/07391102.2020.1767211
Beelen, R., Raaschou-Nielsen, O., Stafoggia, M., Andersen, Z. J., Weinmayr, G., Hoffmann, B., Wolf, K., Samoli, E., Fischer, P., Nieuwenhuijsen, M., Vineis, P., Xun, W. W., Katsouyanni, K., Dimakopoulou, K., Oudin, A., Forsberg, B., Modig, L., Havulinna, A. S., Lanki, T., & Hoek, G. (2014). Effects of long-term exposure to air pollution on natural-cause mortality: An analysis of 22 European cohorts within the multicentre ESCAPE project. The Lancet, 383(9919), 785–795. https://doi.org/10.1016/S0140-6736(13)62158-3
Beyerstedt, S., Casaro, E. B., & Rangel, É. B. (2021). COVID-19: Angiotensin-converting enzyme 2 (ACE2) expression and tissue susceptibility to SARS-CoV-2 infection. European Journal of Clinical Microbiology and Infectious Diseases, 40(5), 905–919. https://doi.org/10.1007/s10096-020-04138-6
Bidoli, E., Pappagallo, M., Birri, S., Frova, L., Zanier, L., & Serraino, D. (2016). Residential proximity to major roadways and lung cancer mortality. Italy, 1990–2010: An observational study. International Journal of Environmental Research and Public Health, 13(2), 1–9. https://doi.org/10.3390/ijerph13020191
Bolaño-Ortiz, T. R., Camargo-Caicedo, Y., Puliafito, S. E., Ruggeri, M. F., Bolaño-Diaz, S., Pascual-Flores, R., Saturno, J., Ibarra-Espinosa, S., Mayol-Bracero, O. L., Torres-Delgado, E., & Cereceda-Balic, F. (2020). Spread of SARS-CoV-2 through Latin America and the Caribbean region: A look from its economic conditions, climate and air pollution indicators. Environmental Research, 191, 109938. https://doi.org/10.1016/j.envres.2020.109938
Borro, M., Di Girolamo, P., Gentile, G., De Luca, O., Preissner, R., Marcolongo, A., Ferracuti, S., & Simmaco, M. (2020). Evidence-based considerations exploring relations between SARS-CoV-2 pandemic and air pollution: Involvement of PM2.5-mediated up-regulation of the viral receptor ace-2. International Journal of Environmental Research and Public Health, 17(15), 1–13. https://doi.org/10.3390/ijerph17155573
Cartórios de Registro Civil do Brasil. (2021). Painel registral. Especial Covid.
CETESB. (2021). Qualidade do ar no estado de São Paulo 2020.
Chakraborty, P., Jayachandran, S., Padalkar, P., Sitlhou, L., Chakraborty, S., Kar, R., Bhaumik, S., & Srivastava, M. (2020). Exposure to nitrogen dioxide (NO2) from vehicular emission could increase the COVID-19 pandemic fatality in India: A perspective. Bulletin of Environmental Contamination and Toxicology, 105(2), 198–204. https://doi.org/10.1007/s00128-020-02937-3
Chen, H., Kwong, J. C., Copes, R., Tu, K., Villeneuve, P. J., van Donkelaar, A., Hystad, P., Martin, R. V., Murray, B. J., Jessiman, B., Wilton, A. S., Kopp, A., & Burnett, R. T. (2017). Living near major roads and the incidence of dementia, Parkinson’s disease, and multiple sclerosis: A population-based cohort study. The Lancet, 389(10070), 718–726. https://doi.org/10.1016/S0140-6736(16)32399-6
Coccia, M. (2020). Factors determining the diffusion of COVID-19 and suggested strategy to prevent future accelerated viral infectivity similar to COVID. Science of the Total Environment, 729, 138474.
Coccia, M. (2021a). How do low wind speeds and high levels of air pollution support the spread of COVID-19? Atm. Pollut. Res., 12, 437–445.
Coccia, M. (2021b). The effects of atmospheric stability with low wind speed and of air pollution on the accelerated transmission dynamics of COVID-19. International Journal of Environmental Studies, 78(1), 1–27.
Coccia, M. (2021c). High health expenditures and low exposure of population to air pollution as critical factors that can reduce fatality rate in COVID-19 pandemic crisis. Environmental Research, 199, 111339.
CONASS. (2021). Excesso de mortalidade nas regiões do Brazil. Painel de análise do excesso de mortalidade por causas naturais no Brasil.
Conticini, E., Frediani, B., & Caro, D. (2020). Can atmospheric pollution be considered a co-factor in extremely high level of SARS-CoV-2 lethality in Northern Italy?. Environmental Pollution, 261, 114465. https://doi.org/10.1016/j.envpol.2020.114465
Copat, C., Cristaldi, A., Fiore, M., Grasso, A., Zuccarello, P., Signorelli, S. S., Conti, G. O., & Ferrante, M. (2020). The role of air pollution (PM and NO2) in COVID-19 spread and lethality: A systematic review. Environmental Research, 191(July), 110129. https://doi.org/10.1016/j.envres.2020.110129
Cui, Y., Zhang, Z. F., Froines, J., Zhao, J., Wang, H., Yu, S. Z., & Detels, R. (2003). Air pollution and case fatality of SARS in the People’s Republic of China: An ecologic study. Environmental Health: A Global Access Science Source, 2, 1–5. https://doi.org/10.1186/1476-069X-2-1
Dales, R., Blanco-Vidal, C., Romero-Meza, R., Schoen, S., Lukina, A., & Cakmak, S. (2021). The association between air pollution and COVID-19 related mortality in Santiago, Chile: A daily time series analysis. Environmental Research, 198, 111284. https://doi.org/10.1016/j.envres.2021.111284
DATASUS. (2021). Painel de monitoramento da mortalidade CID10. Painies de Monitoramento.
Debone, D., da Costa, M. V., & Miraglia, S. G. E. K. (2020). 90 days of COVID-19 social distancing and its impacts on air quality and health in Sao Paulo, Brazil. Sustainability, 12(18), 7440. https://doi.org/10.3390/su12187440
Diao, Y., Kodera, S., Anzai, D., Gomez-Tames, J., Rashed, E. A., & Hirata, A. (2021). Influence of population density, temperature, and absolute humidity on spread and decay durations of COVID-19: A comparative study of scenarios in China, England, Germany, and Japan. One Health, 12, 100203.
Feng, C., Li, J., Sun, W., Zhang, Y., & Wang, Q. (2016). Impact of ambient fine particulate matter (PM2.5) exposure on the risk of influenza-like-illness: A time-series analysis in Beijing, China. Environmental Health: A Global Access Science Source, 15(1), 1–12. https://doi.org/10.1186/s12940-016-0115-2
Frontera, A., Cianfanelli, L., Vlachos, K., Landoni, G., & Cremona, G. (2020). Severe air pollution links to higher mortality in COVID-19 patients: The “double-hit” hypothesis. Journal of Infection, 81(2), 255–259. https://doi.org/10.1016/j.jinf.2020.05.031
Gharibvand, L., Shavlik, D., Ghamsary, M., Beeson, W. L., Soret, S., Knutsen, R., & Knutsen, S. F. (2016). The association between ambient fine particulate air pollution and lung cancer incidence: Results from the AHSMOG-2 study. Environmental Health Perspectives. https://doi.org/10.1289/EHP124
Greenhalgh, T., Jimenez, J. L., Prather, K. A., Tufekci, Z., Fisman, D., & Schooley, R. (2021). Ten scientific reasons in support of airborne transmission of SARS-CoV-2. The Lancet, 397(10285), 1603–1605. https://doi.org/10.1016/S0140-6736(21)00869-2
Hendryx, M., & Luo, J. (2020). COVID-19 prevalence and fatality rates in association with air pollution emission concentrations and emission sources. Environmental Pollution, 265, 115126. https://doi.org/10.1016/j.envpol.2020.115126
Jiang, Y., Wu, X. J., & Guan, Y. J. (2020). Effect of ambient air pollutants and meteorological variables on COVID-19 incidence. Infection Control and Hospital Epidemiology, 41(9), 1011–1015. https://doi.org/10.1017/ice.2020.222
Konstantinoudis, G., Padellini, T., Bennett, J., Davies, B., Ezzati, M., & Blangiardo, M. (2021). Long-term exposure to air-pollution and COVID-19 mortality in England: A hierarchical spatial analysis. Environment International, 146, 106316. https://doi.org/10.1016/j.envint.2020.106316
Kutralam-Muniasamy, G., Pérez-Guevara, F., Martínez, I. E., & Chari, S. V. (2021). Particulate matter concentrations and their association with COVID-19-related mortality in Mexico during June 2020 Saharan dust event. Environmental Science and Pollution Research. https://doi.org/10.1007/s11356-021-14168-y
Landrigan, P. J., Fuller, R., Acosta, N. J. R., Adeyi, O., Arnold, R., Basu, N., Baldé, A. B., Bertollini, R., Bose-O’Reilly, S., Boufford, J. I., Breysse, P. N., Chiles, T., Mahidol, C., Coll-Seck, A. M., Cropper, M. L., Fobil, J., Fuster, V., Greenstone, M., Haines, A., & Zhong, M. (2018). The Lancet Commission on pollution and health. The Lancet, 391(10119), 462–512. https://doi.org/10.1016/S0140-6736(17)32345-0
Lanki, T., Hampel, R., Tiittanen, P., Andrich, S., Beelen, R., Brunekreef, B., Dratva, J., de Faire, U., Fuks, K. B., Hoffmann, B., Imboden, M., Jousilahti, P., Koenig, W., Mahabadi, A. A., Künzli, N., Pedersen, N. L., Penell, J., Pershagen, G., Probst-Hensch, N. M., & Peters, A. (2015). Air pollution from road traffic and systemic inflammation in adults: A cross-sectional analysis in the european escape project. Environmental Health Perspectives, 123(8), 785–791. https://doi.org/10.1289/ehp.1408224
Liang, D., Liuhua, S., Zhao, J., Liu, P., Sarnat, J. A., Gao, S., Schwartz, J., Liu, Y., Ebelt, S. T., Scovronick, N., & Chang, H. (2020). Urban air pollution may enhance COVID-19 case-fatality and mortality rates in the United States. The Innovation, January, 19–21.
Liang, Y., Fang, L., Pan, H., Zhang, K., Kan, H., Brook, J. R., & Sun, Q. (2014). PM 2.5 in Beijing – Temporal pattern and its association with influenza. Environmental Health, 1–8.
Lim, C. C., Hayes, R. B., Ahn, J., Shao, Y., Silverman, D. T., Jones, R. R., Garcia, C., & Thurston, G. D. (2018). Association between long-term exposure to ambient air pollution and diabetes mortality in the US. Environmental Research, 165, 330–336. https://doi.org/10.1016/j.envres.2018.04.011
Lin, C. I., Tsai, C. H., Sun, Y. L., Hsieh, W. Y., Lin, Y. C., Chen, C. Y., & Lin, C. S. (2018). Instillation of particulate matter 2.5 induced acute lung injury and attenuated the injury recovery in ACE2 knockout mice. International Journal of Biological Sciences, 14(3), 253–265. https://doi.org/10.7150/ijbs.23489
López-Feldman, A., Heres, D., & Marquez-Padilla, F. (2021). Air pollution exposure and COVID-19: A look at mortality in Mexico City using individual-level data. Science of the Total Environment, 756, 143929. https://doi.org/10.1016/j.scitotenv.2020.143929
McConnell, R., Islam, K. T., Shankardass, K., Jerrett, M., Lurmann, F., Gilliland, F. D., Gauderman, J., Avol, E., Künzli, N., Yao, L., Peters, J. M., & Berhane, K. (2010). Childhood incident asthma and traffic-related air pollution at home and school. Environmental Health Perspectives, 118(7), 1021–1026. https://doi.org/10.1289/ehp.0901232
Noor, F. M., & Islam, M. M. (2020). Prevalence and associated risk factors of mortality among COVID-19 patients: A meta-analysis. Journal of Community Health, 45(6), 1270–1282. https://doi.org/10.1007/s10900-020-00920-x
Ostro, B. (2004). Outdoor air pollution: Assessing the environmental burden of disease at national and local levels. In Environmental Burden of Disease Series (Issue 5). ISBN 92 4 159146 3.
Our world in data. (2021). Coronavirus country profiles. Coronavirus.
Páez-Osuna, F., Valencia-Castañeda, G., & Rebolledo, U. A. (2021). The link between COVID-19 mortality and PM2.5 emissions in rural and medium-size municipalities considering population density, dust events, and wind speed. Chemosphere. https://doi.org/10.1016/j.chemosphere.2021.131634
Pascal, M., Corso, M., Ung, A., Declercq, C., & Medina, S. (2011). Guidelines for assessing the health impacts of air pollution in European cities.
Rosario, D. K. A., Mutz Yhan, S., Bernardes, P. C., & Conte-Junior, C. A. (2020). Relationship between COVID-19 and weather: Case study in a tropical country. International Journal of Hygiene and Environmental Health, 229, 113587.
Rothan, H. A., & Byrareddy, S. N. (2020). The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak. Journal of Autoimmunity, 109, 102433. https://doi.org/10.1016/j.jaut.2020.102433
Sarkodie, S. A., & Owusu, P. A. (2020). Impact of meteorological factors on COVID-19 pandemic: Evidence from top 20 countries with confirmed cases. Environmental Research, 191, 110101.
SEADE. (2021a). Boletim Completo. SP Contra o Novo Coronavírus.
SEADE. (2021b). Painel Seade. Portal de Estatísticas Do Estado de São Paulo.
SEADE. (2021c). PIB SP. SEADE PIB + 30.
Simonnet, A., Chetboun, M., Poissy, J., Raverdy, V., Noulette, J., Duhamel, A., Labreuche, J., Mathieu, D., Pattou, F., Jourdain, M., Caizzo, R., Caplan, M., Cousin, N., Duburcq, T., Durand, A., El kalioubie, A., Favory, R., Garcia, B., Girardie, P., & Verkindt, H. (2020). High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation. Obesity, 28(7), 1195–1199. https://doi.org/10.1002/oby.22831
Srivastava, A. (2021). COVID-19 and air pollution and meteorology-an intricate relationship: A review. Chemosphere, 263, 128297.
Sunyer, J., Esnaola, M., Alvarez-Pedrerol, M., Forns, J., Rivas, I., López-Vicente, M., Suades-González, E., Foraster, M., Garcia-Esteban, R., Basagaña, X., Viana, M., Cirach, M., Moreno, T., Alastuey, A., Sebastian-Galles, N., Nieuwenhuijsen, M., & Querol, X. (2015). Association between traffic-related air pollution in schools and cognitive development in primary school children: A prospective cohort study. PLoS Medicine, 12(3), 1–24. https://doi.org/10.1371/journal.pmed.1001792
The World Bank. (2021). Brazil. Data.
Travaglio, M., Yu, Y., Popovic, R., Selley, L., Leal, N. S., & Martins, L. M. (2021). Links between air pollution and COVID-19 in England. Environmental Pollution, 268, 115859. https://doi.org/10.1016/j.envpol.2020.115859
Vasquez-Apestegui, B. V., Parras-Garrido, E., Tapia, V., Paz-Aparicio, V. M., Rojas, J. P., Sanchez-Ccoyllo, O. R., & Gonzales, G. F. (2021). Association between air pollution in Lima and the high incidence of COVID-19: Findings from a post hoc analysis. BMC Public Health, 21(1), 1–13. https://doi.org/10.1186/s12889-021-11232-7
WHO. (2021a). Ambient air pollution. Air quality and health.
WHO. (2021b). Coronavirus. Health topics.
Wilkins, E. T. (1954). Air pollution aspects of the London fog of December 1952. Quarterly Journal of the Royal Meteorological Society, 80(344), 267–271. https://doi.org/10.1002/qj.49708034420
Worldometers. (2021). Worldometers. COVID-19 coronavirus pandemic.
Wu, X., Nethery, R. C., Sabath, M. B., Braun, D., & Dominici, F. (2020). Air pollution and COVID-19 mortality in the United States: Strengths and limitations of an ecological regression analysis. Science Advances., 6(45), eabd4049. https://doi.org/10.1126/sciadv.abd4049
Yao, Y., Pan, J., Wang, W., Liu, Z., Kan, H., Qiu, Y., Meng, X., & Wang, W. (2020). Association of particulate matter pollution and case fatality rate of COVID-19 in 49 Chinese cities. Science of the Total Environment, 741, 140396. https://doi.org/10.1016/j.scitotenv.2020.140396
Yu, X., Wong, M. S., Kwan, M. P., Nichol, J. E., Zhu, R., Heo, J., Chan, P. W., Chin, D. C. W., Kwok, C. Y. T., & Kan, Z. (2021). COVID-19 infection and mortality: Association with PM2.5 concentration and population density-an exploratory study. ISPRS International Journal of Geo-Information. https://doi.org/10.3390/ijgi10030123
Zhao, B., Johnston, F. H., Salimi, F., Kurabayashi, M., & Negishi, K. (2020). Short-term exposure to ambient fine particulate matter and out-of-hospital cardiac arrest: a nationwide casecrossover study in Japan. The Lancet Planetary Health, 4(1), e15–e23. https://doi.org/10.1016/S2542-5196(19)30262-1
Zhu, F., Ding, R., Lei, R., Cheng, H., Liu, J., Shen, C., Zhang, C., Xu, Y., Xiao, C., Li, X., Zhang, J., & Cao, J. (2019). The short-term effects of air pollution on respiratory diseases and lung cancer mortality in Hefei: A time-series analysis. Respiratory Medicine, 146, 57–65. https://doi.org/10.1016/j.rmed.2018.11.019
Zhu, Y., Xie, J., Huang, F., & Cao, L. (2020). Association between short-term exposure to air pollution and COVID-19 infection: Evidence from China. Science of the Total Environment, 727, 138704. https://doi.org/10.1016/j.scitotenv.2020.138704
Funding
The study was financed by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), Brazil. Finance Codes 1808525 and 1808529.
Author information
Authors and Affiliations
Contributions
Luciana F. L. Leirião: conceptualization, methodology, formal analysis, investigation, writing — original draft, writing — review & editing. Daniela Debone: investigation, writing — original draft. Simone G. E. K. Miraglia: writing — review & editing, supervision.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
We confirm that the manuscript has been read and approved by all named authors and that there are no other persons who satisfied the criteria for authorship but are not listed. We further confirm that the order of authors listed in the manuscript has been approved by all of us.
Consent for publication
The authors agree to publish this article in the Environmental Monitoring and Assessment.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Leirião, L.F.L., Debone, D. & Miraglia, S.G.E.K. Does air pollution explain COVID-19 fatality and mortality rates? A multi-city study in São Paulo state, Brazil. Environ Monit Assess 194, 275 (2022). https://doi.org/10.1007/s10661-022-09924-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10661-022-09924-7