Abstract
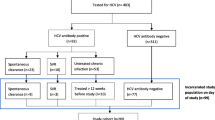
To determine hepatitis C incidence and the demographic and behavioural predictors in seronegative drug injecting prisoners. Prisoners in New South Wales, Australia who: were aged 18 years and over; reported IDU; had been continuously imprisoned; had a documented negative HCV antibody test result in prison in the last 12 months; provided written informed consent. Subjects were interviewed about their demographic characteristics and detailed risk factors for transmission prior to, and since, imprisonment. A blood sample was collected to screen for HCV antibodies by ELISA and RNA by PCR. Of 253 inmates recruited, 120 were continuously imprisoned and included in this analysis. Sixteen acquired HCV infection indicating an incidence of 34.2 per 100 person years (CI: 19.6–55.6). Risk factors for transmission included prior imprisonment, methadone treatment and greater than 10 years of education. Although the frequency of injecting was reduced in prison, 33.6% continued to inject drugs, most commonly methamphetamine, and 90% of these reported sharing injecting equipment. Prison inmates were at high risk of HCV infection, despite some reduction in high-risk behaviours and access to prevention services. To prevent HCV transmission in prisons, better prevention strategies are required.
Similar content being viewed by others
Abbreviations
- HCV:
-
Hepatitis C virus
- IDU:
-
Injecting drug use(rs)
- NSW:
-
New South Wales
References
Shepard CW, Finelli L, Alter MJ. Global epidemiology of hepatitis C virus infection. Lancet Infect Dis. 2005;5(9):558–67.
Jurgens R, Ball A, Verster A. Interventions to reduce HIV transmission related to injecting drug use in prison. Lancet Infect Dis. 2009;9:57–66.
Correctional Service Canada. 1995 National inmate survey: Final report [No. SR-02]. Ottawa: Correctional Service Canada; 1996.
Gore SM, Bird AG, Burns SM, Goldberg DJ, Ross AJ, Macgregor J. Drug injection and HIV prevalence in inmates of Glenochil prison. Brit Med J. 1995;310(6975):293–6.
O’Sullivan BG, Levy MH, Dolan KA, Post JJ, Barton SG, Dwyer DE, et al. Hepatitis C transmission and HIV post-exposure prophylaxis after needle- and syringe-sharing in Australian prisons. Med J Aust. 2003;178(11):546–9.
Post JJ, Dolan KA, Whybin LR, Carter IW, Haber PS, Lloyd AR. Acute hepatitis C virus infection in an Australian prison inmate: tattooing as a possible transmission route. Med J Aust. 2001;174(4):183–4.
Rosen HR. Acquisition of hepatitis C by a conjunctival splash. Am J Infect Control. 1997;25:242–7.
Haber PS, Parsons SJ, Harper SE, White PA, Rawlinson WD, Lloyd AR. Transmission of hepatitis C within Australian prisons. Med J Aust. 1999;171(1):31–4.
Neaigus A, Gyarmathy VA, Zhao M, Miller M, Friedman SR, Des Jarlais DC. Sexual and other noninjection risks for HBV and HCV seroconversions among non-injecting heroin users. J Infect Dis. 2007;195(7):1052–61.
Macalino GE, et al. Prevalence and incidence of HIV, hepatitis B virus, and hepatitis C virus infections among males in Rhode Island prisons. Am J Public Health. 2004;94(7):1218–23.
Vlahov D, Nelson KE, Quinn TC, Kendig N. Prevalence and incidence of hepatitis C virus infection among male prison inmates in Maryland. Eur J Epidemiol. 1993;9(5):566–9.
Arrada A, Zak Dit Zbar O, Vasseur V. Prevalence of HBV and HCV infections and incidence of HCV infection after 3, 6 and 12 months detention in La Sante prison, Paris. Ann Med Interne (Paris). 2001;152(Suppl 7):6–8.
Crofts N, Stewart T, Hearne P, Ping XY, Breshkin AM, Locarnini SA. Spread of bloodborne viruses among Australian prison entrants. Brit Med J. 1995;310(6975):285–8.
Christensen PB, Krarup HB, Niesters HG, Norder H, Georgsen J. Prevalence and incidence of bloodborne viral infections among Danish prisoners. Eur J Epidemiol. 2000;16(11):1043–9.
Dolan KA, Shearer J, White B, Zhou J, Wodak A. Four-year follow-up of imprisoned male heroin users and methadone treatment: mortality, reincarceration and hepatitis C infection. Addiction. 2005;100(6):820–8.
Marsch LA. The efficacy of methadone maintenance interventions in reducing illicit opiate use, HIV risk behaviour and criminality: a meta-analysis. Addiction. 1998;93:515–32.
Gowing L, Farrell M, Bornemann R, Ali R. Substitution treatment of injecting opioid users for prevention of HIV infection. Cochrane Database Syst Rev. 2004;4:CD0041453.
Dolan KA, Shearer J, MacDonald M, Mattick RP, Hall W, Wodak AD. A randomised controlled trial of methadone maintenance treatment versus wait list control in an Australian prison system. Drug Alcohol Depend. 2003;72(1):59–65.
Barnett PG, Hui SS. The cost-effectiveness of methadone maintenance. Mt Sinai J Med. 2000;67:365–74.
Amato L, Davoli M, Perucci CA, Ferri M, Faggiano F, Mattick RP. An overview of systematic reviews of the effectiveness of opiate maintenance therapies: available evidence to inform clinical practice and research. J Subst Abuse Treat. 2005;28:321–9.
Dolan K, Wodak A. An international review of methadone provision in prisons. Addict Res. 1996;4(1):85–97.
Larney S, Dolan K. A literature review of international implementation of opioid substitution treatment in prisons: equivalence of care? Euro Addict Res. 2009;15:107–12.
Clayton D, Hills M. Statistical models in epidemiology. Oxford: Oxford University Press; 1993.
Goldberg D, Taylor A. Preventing transmission of bloodborne virus infections in prisons. Commun Dis Public Health. 2000;3(2):84–5.
Power KG, Markova I, Rowlands A, McKee KJ, Anslow PJ, Kilfedder C. Intravenous drug use and HIV transmission amongst inmates in Scottish prisons. Br J Addict. 1992;87(1):35–45.
Hallinan R, Byrne A, Amin J, Dore G. Hepatitis C virus prevalence and outcomes among IDUs on opioid replacement therapy. J Gastroenterol Hepatol. 2005;20:1082–6.
Dolan K, Hall W, Wodak A. Methadone maintenance reduces injecting in prison. Brit Med J. 1996;312:1162.
New South Wales Opioid Treatment Program. Clinical guidelines for methadone and buprenorphine treatment of opioid dependence. New South Wales Health. 2006. Available at www.nsw.health.gov.au.
Australian Bureau of Statistics, Prisoners in Australia. 2008. http://www.abs.gov.au/ausstats/abs@.nsf/cat/4517.0 accessed 8 Dec 2009).
National Centre in HIV Epidemiology and Clinical Research. Return on Investment 2: Evaluating the cost-effectiveness of needle and syringe programs in Australia, 2009. Sydney. 2009.
Dolan K, Larney S, Jacka B, Rawlinson W. Presence of hepatitis C virus in syringes confiscated in prisons in Australia. J Gastroenterol Hepatol. 2009;24(10):1655–7.
Dolan K, Hall W, Wodak A, Gaughwin M. Evidence of HIV transmission in an Australian prison. Letter Med J Aust. 1994;160:734.
Larney S, Dolan K. Increased access to opioid substitution treatment in prisons is needed to ensure equivalence of care. Aust NZ J Pub Health. 2008;32:86–7.
Dolan K, Kite B, Black E, Aceijas C, Stimson GV. HIV in prison in low-income and middle-income countries. Lancet Infect Dis. 2007;7:32–41.
Barroon LH. Subjects or objects? Prisoners and human experimentation. New England J Med. 2007;356:1806–7.
Acknowledgments
All authors have contributed to the design, data analysis and write up of the paper. We have no conflict of interest. This work was supported by a Project Grant from the National Health and Medical Research Council of Australia (No. 222877) and by the University of New South Wales Hepatitis C Vaccine Initiative. The authors are independent of the funders. The study protocol was approved by the Human Research Ethics Committees of Justice Health, and the Department of Corrective Services, New South Wales, Australia.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dolan, K., Teutsch, S., Scheuer, N. et al. Incidence and risk for acute hepatitis C infection during imprisonment in Australia. Eur J Epidemiol 25, 143–148 (2010). https://doi.org/10.1007/s10654-009-9421-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-009-9421-0