Abstract
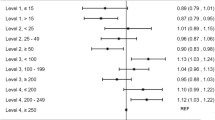
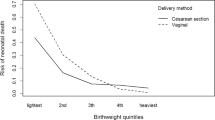
Objective Regionalised perinatal care with antenatal transfer of high risk pregnancies to Level III centres is beneficial. However, levels of care are usually not linked to caseload requirements, which remain a point for discussion. We aimed to investigate the impact of annual delivery volume on early neonatal mortality among very preterm births. Methods All neonates with gestational age 24–30 weeks, born 1991–1999 in Lower Saxony were included into this population-based cohort study (n = 5,083). Large units were defined as caring for more than 1,000 deliveries/year, large NICUs as those with at least 36 annual very low birthweight (<1,500 g, VLBW) admissions. Main outcome criterion was mortality until day 7. Adjusted Odds Ratios (adj. OR) and 95% confidence intervals (CI) were calculated based on generalised estimating equation models, accounting for correlation of individuals within units. Results Within the first week of life, 20.6% of all neonates deceased; 10.2% were stillbirths, 3.7% died in the delivery unit, and 6.7% in the NICU. The crude OR for early neonatal mortality after having been delivered in a small delivery unit (excluding stillbirths) was 1.36 (95%CI 1.04–1.78; adj. OR 1.16 (0.82–1.63)). It increased to 1.96 (1.54–2.48; adj. OR 1.21 (0.86–1.70)) after the inclusion of stillbirths. Conclusion This study has shown a slight, but non-significant association between obstetrical volume and early neonatal mortality. In future studies the impact of caseload on outcome may become more evident when referring to high-risk patients instead of to the overall number of deliveries.

Similar content being viewed by others
Abbreviations
- Adj.:
-
Adjusted
- AGA:
-
Appropriate weight for gestational age
- CI:
-
Confidence interval
- GA:
-
Gestational age
- GEE:
-
General estimating equation
- LGA:
-
Large for gestational age
- MV:
-
Missing value
- NICU:
-
Neonatal intensive care unit
- OR:
-
Odds ratio
- RDS:
-
Respiratory distress syndrome
- SGA:
-
Small for gestational age
- VLBW:
-
Very low birthweight (<1,500 g)
References
Sanderson M, Sappenfield WM, Jespersen KM, Liu Q, Baker SL. Association between level of delivery hospital and neonatal outcomes among South Carolina Medicaid recipients. Am J Obstet Gynecol 2000;183(6):1504–11.
Halm EA, Lee C, Chassin MR. Is volume related to outcome in health care? A systematic review and methodologic critique of the literature. Ann Intern Med 2002;137(6):511–20.
Stark AR, Couto J. Levels of neonatal care. Pediatrics 2004;114(5):1341–7.
Perkins BB. Rethinking perinatal policy: history and evaluation of minimum volume and level-of-care standards. J Public Health Policy 1993;14(3):299–319.
Cifuentes J, Bronstein J, Phibbs CS, Phibbs RH, Schmitt SK, Carlo WA. Mortality in low birth weight infants according to level of neonatal care at hospital of birth. Pediatrics 2002;109(5):745–51.
Phibbs CS, Bronstein JM, Buxton E, Phibbs RH. The effects of patient volume and level of care at the hospital of birth on neonatal mortality. Jama 1996;276(13):1054–9.
Samuelson JL, Buehler JW, Norris D, Sadek R. Maternal characteristics associated with place of delivery and neonatal mortality rates among very-low-birthweight infants, Georgia. Paediatr Perinat Epidemiol 2002;16(4):305–13.
Bartels DB, Wypij D, Wenzlaff P, Dammann O, Poets CF. Hospital volume and neonatal mortality among very low birth weight infants. Pediatrics 2006;117(6):2206–14.
Center for Quality Management. NPExtra 1996. Hannover: Druckerei L. Lindenhain; 1997.
Bartels D, Kreienbrock L, Dammann O, Wenzlaff P, Poets CF. Population-based study on the outcome of small for gestational age newborns. Arch Dis Child Fetal Neonatal Ed 2005;90:F53–F9.
Moster D, Lie RT, Markestad T. Neonatal mortality rates in communities with small maternity units compared with those having larger maternity units. Bjog 2001;108(9):904–9.
Voigt M, Schneider KT, Jahrig K. [Analysis of a 1992 birth sample in Germany. 1: New percentile values of the body weight of newborn infants]. Geburtshilfe Frauenheilkd. 1996;56(10):550–8.
McGregor G. Small for gestational age, term babies, in the first six years of life. Eur J Clin Nutr 1998;52(S1):S59–S64.
Hosmer D, Lemeshow S. Applied logistic regression. New York: John Wiley & Sons; 1989.
Zeger SL, Liang KY, Albert PS. Models for longitudinal data: a generalized estimating equation approach. Biometrics 1988;44(4):1049–60.
LeFevre M, Sanner L, Anderson S, Tsutakawa R. The relationship between neonatal mortality and hospital level. J Fam Pract 1992;35(3):259–64.
Bode MM, O’Shea T M, Metzguer KR, Stiles AD. Perinatal regionalization and neonatal mortality in North Carolina, 1968–1994. Am J Obstet Gynecol. 2001;184(6):1302–7.
Pollack MM, Koch MA. Association of outcomes with organizational characteristics of neonatal intensive care units. Crit Care Med 2003;31(6):1620–9.
Johansson S, Montgomery SM, Ekbom A, Olausson PO, Granath F, Norman M et al. Preterm delivery, level of care, and infant death in sweden: a population-based study. Pediatrics 2004;113(5):1230–5.
Berg CJ, Druschel CM, McCarthy BJ, LaVoie M, Floyd RL. Neonatal mortality in normal birth weight babies: does the level of hospital care make a difference?. Am J Obstet Gynecol 1989;161(1):86–91.
Menard MK, Liu Q, Holgren EA, Sappenfield WM. Neonatal mortality for very low birth weight deliveries in South Carolina by level of hospital perinatal service. Am J Obstet Gynecol 1998;179(2):374–81.
Moster D, Lie RT, Markestad T. Relation between size of delivery unit and neonatal death in low risk deliveries: population based study. Arch Dis Child Fetal Neonatal Ed 1999;80(3):F221–5.
Kramer MS, Liu S, Luo Z, Yuan H, Platt RW, Joseph KS. Analysis of perinatal mortality and its components: time for a change?. Am J Epidemiol 2002;156(6):493–7.
Warner B, Musial MJ, Chenier T, Donovan E. The Effect of Birth Hospital Type on the Outcome of Very Low Birth Weight Infants. Pediatrics 2004;113(1):35–41.
Heller G, Richardson DK, Schnell R, Misselwitz B, Kunzel W, Schmidt S. Are we regionalized enough? Early-neonatal deaths in low-risk births by the size of delivery units in Hesse, Germany 1990–1999. Int J Epidemiol. 2002;31(5):1061–8.
Mayfield JA, Rosenblatt RA, Baldwin LM, Chu J, Logerfo JP. The relation of obstetrical volume and nursery level to perinatal mortality. Am J Public Health 1990;80(7):819–23.
Lee SK, McMillan DD, Ohlsson A, Boulton J, Lee DS, Ting S et al. The benefit of preterm birth at tertiary care centers is related to gestational age. Am J Obstet Gynecol 2003;188(3):617–22.
Phibbs CS, Baker LC, Caughey AB, Danielsen B, Schmitt SK, Phibbs RH. Level and volume of neonatal intensive care and mortality in very-low-birth-weight infants. N Engl J Med 2007;356(21):2165–75.
American Academy of Pediatrics & American College of Obstetricians and Gynecologists. Guidelines for perinatal care. 4th ed. Washington: American Academy of Pediatrics and The American College of Obstetricians and Gynecologists; 1997.
Haberland CA, Phibbs CS, Baker LC. Effect of opening midlevel neonatal intensive care units on the location of low birth weight births in California. Pediatrics 2006;118(6):e1667–79.
Chien LY, Whyte R, Aziz K, Thiessen P, Matthew D, Lee SK. Improved outcome of preterm infants when delivered in tertiary care centers. Obstet Gynecol 2001;98(2):247–52.
Stevenson DK, Verter J, Fanaroff AA, Oh W, Ehrenkranz RA, Shankaran S et al. Sex differences in outcomes of very low birthweight infants: the newborn male disadvantage. Arch Dis Child Fetal Neonatal Ed 2000;83(3):F182–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bartels, D.B., Wenzlaff, P. & Poets, C.F. Obstetrical volume and early neonatal mortality in preterm infants. Eur J Epidemiol 22, 791–798 (2007). https://doi.org/10.1007/s10654-007-9182-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-007-9182-6