Summary
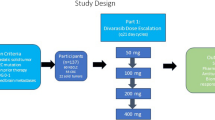
Background Overcoming resistance to anti-epidermal growth factor receptor (EGFR) monoclonal antibodies (mAbs) in patients with KRAS wildtype (WT) metastatic colorectal cancer (mCRC) could help meet the needs of patients with limited treatment options. Methods In this phase 1b study, patients with N/KRAS WT, MET-positive mCRC who had progressed following anti-EGFR mAb treatment received escalating oral doses of capmatinib (150, 300, and 400 mg) twice daily plus weekly intravenous cetuximab (at the approved dose). The primary objective was to establish a recommended dose for expansion (RDE) of capmatinib in combination with cetuximab. Safety, preliminary activity, pharmacokinetics, and pharmacodynamics were also explored. Results Thirteen patients were enrolled. No patients experienced a dose-limiting toxicity at investigated doses; the RDE was established as capmatinib 400 mg twice daily plus cetuximab. All patients experienced adverse events (AEs) suspected to be related to the study treatment. Five patients (38.5%) reported study-drug–related AEs of grade 3/4 in severity. No patients achieved a complete or partial response according to RECIST v1.1; however, tumor shrinkage of 29–44% was observed in 4 patients. Conclusions Capmatinib plus cetuximab was well tolerated. Preliminary signs of activity were observed. Further investigation is warranted to obtain efficacy data and refine predictive biomarkers of response. Clinical trial registration NCT02205398.


Similar content being viewed by others
Data availability
Novartis is committed to sharing with qualified external researchers, access to patient-level data and supporting clinical documents from eligible studies. These requests are reviewed and approved by an independent review panel on the basis of scientific merit. All data provided are anonymized to respect the privacy of patients who have participated in the trial in line with applicable laws and regulations.
This trial data availability is according to the criteria and process described on www.clinicalstudydatarequest.com.
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA Cancer J Clin 65(2):87–108
Van Cutsem E, Cervantes A, Adam R et al (2016) ESMO consensus guidelines for the management of patients with metastatic colorectal cancer. Ann Oncol 27(8):1386–1422
Van Cutsem E, Köhne CH, Hitre E et al (2009) Cetuximab and chemotherapy as initial treatment for metastatic colorectal cancer. N Engl J Med 360(14):1408–1417
Van Cutsem E, Köhne CH, Láng I et al (2011) Cetuximab plus irinotecan, fluorouracil, and leucovorin as first-line treatment for metastatic colorectal cancer: updated analysis of overall survival according to tumor KRAS and BRAF mutation status. J Clin Oncol 29(15):2011–2019
Douillard JY, Siena S, Cassidy J et al (2010) Randomized, phase III trial of panitumumab with infusional fluorouracil, leucovorin, and oxaliplatin (FOLFOX4) versus FOLFOX4 alone as first-line treatment in patients with previously untreated metastatic colorectal cancer: the PRIME study. J Clin Oncol 28(31):4697–4705
Van Cutsem E, Lenz HJ, Köhne CH et al (2015) Fluorouracil, leucovorin, and irinotecan plus cetuximab treatment and RAS mutations in colorectal cancer. J Clin Oncol 33(7):692–700
Hurwitz H, Fehrenbacher L, Novotny W et al (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350(23):2335–2342
Saltz LB, Clarke S, Díaz-Rubio E et al (2008) Bevacizumab in combination with oxaliplatin-based chemotherapy as first-line therapy in metastatic colorectal cancer: a randomized phase III study. J Clin Oncol 26(12):2013–2019
Sorich MJ, Wiese MD, Rowland A, Kichenadasse G, McKinnon RA, Karapetis CS (2015) Extended RAS mutations and anti-EGFR monoclonal antibody survival benefit in metastatic colorectal cancer: a meta-analysis of randomized, controlled trials. Ann Oncol 26(1):13–21
Chong CR, Jänne PA (2013) The quest to overcome resistance to EGFR-targeted therapies in cancer. Nat Med 19(11):1389–1400
Engelman JA, Zejnullahu K, Mitsudomi T et al (2007) MET amplification leads to gefitinib resistance in lung cancer by activating ERBB3 signaling. Science 316(5827):1039–1043
Bean J, Brennan C, Shih JY et al (2007) MET amplification occurs with or without T790M mutations in EGFR mutant lung tumors with acquired resistance to gefitinib or erlotinib. Proc Natl Acad Sci U S A 104(52):20932–20937
Bardelli A, Corso S, Bertotti A et al (2013) Amplification of the MET receptor drives resistance to anti-EGFR therapies in colorectal cancer. Cancer Discov 3(6):658–673
Siravegna G, Mussolin B, Buscarino M et al (2015) Clonal evolution and resistance to EGFR blockade in the blood of colorectal cancer patients. Nat Med 21(7):795–801
Bertotti A, Papp E, Jones S et al (2015) The genomic landscape of response to EGFR blockade in colorectal cancer. Nature 526(7572):263–267
Raghav K, Morris V, Tang C et al (2016) MET amplification in metastatic colorectal cancer: an acquired response to EGFR inhibition, not a de novo phenomenon. Oncotarget 7(34):54627–54631
Mo H, Liu P (2017) Targeting MET in cancer therapy. Chronic Dis Transl Med 3(3):148–153
Luraghi P, Reato G, Cipriano E et al (2014) MET signaling in colon cancer stem-like cells blunts the therapeutic response to EGFR inhibitors. Cancer Res 74(6):1857–1869
Troiani T, Martinelli E, Napolitano S et al (2013) Increased TGF-α as a mechanism of acquired resistance to the anti-EGFR inhibitor cetuximab through EGFR-MET interaction and activation of MET signaling in colon cancer cells. Clin Cancer Res 19(24):6751–6765
Liu X, Wang Q, Yang G et al (2011) A novel kinase inhibitor, INCB28060, blocks c-MET-dependent signaling, neoplastic activities, and cross-talk with EGFR and HER-3. Clin Cancer Res 17(22):7127–7138
Baltschukat S, Engstler BS, Huang A et al (2019) Capmatinib (INC280) is active against models of non-small cell lung cancer and other cancer types with defined mechanisms of MET activation. Clin Cancer Res 25(10):3164–3175
Schuler MH, Berardi R, Lim W et al (2016) Phase (ph) I study of the safety and efficacy of the cMET inhibitor capmatinib (INC280) in patients (pts) with advanced cMET + non-small cell lung cancer (NSCLC). J Clin Oncol 34(Suppl):9067 (Abstract 9067)
Bang Y, Su W, Nam D et al (2014) Phase I study of the safety and efficacy of INC280 in patients with advanced MET-dependent solid tumors. J Clin Oncol 32(5 Suppl):2520 (Abstract 2520)
Wu Y, Kim D, Felip E et al (2016) Phase (ph) II safety and efficacy results of a single-arm ph ib/II study of capmatinib (INC280) + gefitinib in patients (pts) with EGFR-mutated (mut), cMET-positive (cMET+) non-small cell lung cancer (NSCLC). J Clin Oncol 34(Suppl):9020 (Abstract 9020)
Babb J, Rogatko A, Zacks S (1998) Cancer phase I clinical trials: efficient dose escalation with overdose control. Stat Med 17(10):1103–1120
Neuenschwander B, Branson M, Gsponer T (2008) Critical aspects of the Bayesian approach to phase I cancer trials. Stat Med 27(13):2420–2439
Neuenschwander B, Capkun-Niggli G, Branson M, Spiegelhalter DJ (2010) Summarizing historical information on controls in clinical trials. Clin Trials 7(1):5–18
Wu YL, Zhang L, Kim DW et al (2018) Phase Ib/II study of capmatinib (INC280) plus gefitinib after failure of epidermal growth factor receptor (EGFR) inhibitor therapy in patients with EGFR-mutated, MET factor-dysregulated non-small-cell lung cancer. J Clin Oncol 36(31):3101–3109
Bauer TM, Schuler M, Berardi R et al (2016) MINI01.03: Phase (ph) I study of the safety and efficacy of the cMET inhibitor capmatinib (INC280) in patients with advanced cMET + NSCLC: topic: medical oncology. J Thorac Oncol 11(11 Suppl):S257–S258 (Abstract)
Jonker DJ, O’Callaghan CJ, Karapetis CS et al (2007) Cetuximab for the treatment of colorectal cancer. Engl N J Med 357(20):2040–2048
Gibson TB, Ranganathan A, Grothey A (2006) Randomized phase III trial results of panitumumab, a fully human anti-epidermal growth factor receptor monoclonal antibody, in metastatic colorectal cancer. Clin Colorectal Cancer 6(1):29–31
Pasquini G, Giaccone G (2018) C-MET inhibitors for advanced non-small cell lung cancer. Expert Opin Investig Drugs 27(4):363–375
Iacopetta B (2003) TP53 mutation in colorectal cancer. Hum Mutat 21(3):271–276
Fodde R (2002) The APC gene in colorectal cancer. Eur J Cancer 38(7):867–871
Modest DP, Jung A, Moosmann N et al (2012) The influence of KRAS and BRAF mutations on the efficacy of cetuximab-based first-line therapy of metastatic colorectal cancer: an analysis of the AIO KRK-0104-trial. Int J Cancer 131(4):980–986
Acknowledgements
We would like to thank the capmatinib Early Program Team members at Novartis Pharmaceuticals Corporation, in particular Luigi Manenti, for their significant contribution to the study. O. Alejandro Balbin is thanked for assistance with the analysis of next-generation sequencing data and Angela Tam for generating preclinical combination data. Medical writing assistance was provided by Zoe Crossman, PhD of Articulate Science Ltd. and was funded by Novartis Pharmaceuticals Corporation.
Funding
This work was supported by Novartis Pharmaceuticals Corporation.
Author information
Authors and Affiliations
Contributions
Jean-Pierre Delord, Guillem Argilés, Jerôme Fayette, Lori Wirth, Stefan Kasper, Salvatore Siena, Ricard Mesia, Rossana Berardi, Andrés Cervantes, Jeroen Dekervel, and Lillian L. Siu were involved in the acquisition of data; all authors analyzed and interpreted the data; Yongjian Sun undertook the statistical analysis; Huai-Xiang Hao supervised preclinical experiments of cetuximab + capmatinib combination; all authors were involved in the writing, review and/or revision of the manuscript. The final, submitted version was approved by all authors.
Corresponding author
Ethics declarations
Conflict of interest
JP. Delord reports research funding from F. Hoffmann-La Roche, Novartis Pharmaceuticals Corporation, Genentech, Bristol-Myers Squibb, Debiopharm, and Merck Sharpe & Dohme; advisory board participation for Bristol-Myers Squibb, Genentech, Novartis Pharmaceuticals Corporation, Merck Sharpe & Dohme and Takeda; patent holding in the field of molecular signature of cancer drugs effects. G. Argilés reports research funding, travel grants and advisory board participation for F. Hoffmann-La Roche, Bristol-Myers Squibb, Bayer, Servier, Amgen, Merck Serono and Menarini; honoraria to his institution from Bayer, Servier, Novartis Pharmaceuticals Corporation, Boehringer Ingelheim, Boston Pharmaceuticals, F. Hoffmann-La Roche, and Genentech. J. Fayette reports honoraria for consultancy or advisory role from AstraZeneca, Bristol-Myers Squibb, Merck Sharpe & Dohme, Merck Serono, Innate Pharma, and Biogen; research funding from AstraZeneca and Bristol-Myers Squibb; travel, accommodation, or expenses from Bristol-Myers Squibb, AstraZeneca and Merck Sharpe & Dohme. L. Wirth reports acting in an advisory role for Eisai, Loxo Oncology, Merck, Ayala, Cue Biopharma and Genentech. S. Kasper reports personal fees, research grants, and advisory board membership from Roche, Merck Serono, Lilly, Amgen, Servier, Sanofi Aventis, Bristol-Myers Squibb, and Merck Sharpe & Dohme. S. Siena reports acting in an advisory role for Amgen, Bayer, Bristol-Myers Squibb, Roche, Merck, Merck Sharpe & Dohme, Novartis Pharmaceuticals Corporation, and Sanofi. R. Mesia reports an advisory role for Merck, Bristol-Myers Squibb, Merck Sharpe & Dohme, AstraZeneca, Roche, and Nanobiotix; speaker bureaus for Merck, Bristol-Myers Squibb, and Merck Sharpe & Dohme. A. Cervantes reports research grants to his institution form Novartis Pharmaceuticals Corporation to develop clinical trials on investigational compounds. J. Dekervel reports speaker fees, consulting fees or travel grants from Amgen, Bayer, Ipsen, Novartis Pharmaceuticals Corporation, Merck and Servier. L. Siu reports research funding for her institution from Novartis Pharmaceuticals Corporation for the conduct of this study. A. Myers, Y. Sun, H.-X. Hao, R. Tiedt, S. Vicente, and S. Zhao are all employed by Novartis Pharmaceuticals Corporation. R. Berardi declares that she has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Consent for publication
Not applicable as no individual person’s data are presented in this publication.
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 883 kb)
Rights and permissions
About this article
Cite this article
Delord, JP., Argilés, G., Fayette, J. et al. A phase 1b study of the MET inhibitor capmatinib combined with cetuximab in patients with MET-positive colorectal cancer who had progressed following anti-EGFR monoclonal antibody treatment. Invest New Drugs 38, 1774–1783 (2020). https://doi.org/10.1007/s10637-020-00928-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-020-00928-z