Abstract
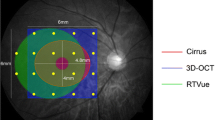
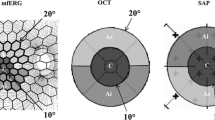
To compare the ability of the multifocal electroretinogram (mfERG) and frequency domain optical coherence tomography (fdOCT) to detect retinal abnormalities. A total of 198 eyes (100 patients) were referred by neuro-ophthalmologists to rule out a retinal etiology of visual impairment. All patients were evaluated with static automated perimetry (SAP) (Humphrey Visual Field Analyzer; Zeiss Meditec), mfERG (Veris, EDI) and fdOCT (3D-OCT 1000, Topcon). The mfERG was performed with 103 scaled hexagons and procedures conforming to ISCEV standards (Hood DC et al. (2008) Doc Ophthalmol 116(1):1–11). The fdOCT imaging included horizontal and vertical line scans through the fovea. Local mfERG and fdOCT abnormalities were compared to local regions of visual field sensitivity loss measured with SAP and categorized as normal/inconclusive or abnormal. 146 eyes were categorized as normal retina on both fdOCT and mfERG. The retina of 52 eyes (36 patients) was categorized as abnormal based upon mfERG and/or fdOCT. Of this group, 25 eyes (20 patients) were abnormal on both tests. However, 20 eyes (13 patients) were abnormal on mfERG, while the fdOCT was normal/inconclusive; and 7 eyes (7 patients) had normal or inconclusive mfERG, but abnormal fdOCT. Considerable disagreement exists between these two methods for detection of retinal abnormalities. The mfERG tends to miss small local abnormalities that are detectable on the fdOCT. On the other hand, the fdOCT can appear normal in the face of clearly abnormal mfERG and SAP results. While improved imaging and analysis may show fdOCT abnormalities in some cases, in others early damage may not appear on structural tests.








Similar content being viewed by others
References
Sutter EE, Tran D (1992) The full field topography of ERG components in man—I. The photopic luminance response. Vision Res 32(3):433–446
Hood DC (2000) Assessing retinal function with the multifocal technique. Prog Retin Eye Res 19(5):607–646
Hood DC, Bach M, Brigell M, Keating D, Kondo M, Lyons JS, Palmowski-Wolfe AM (2008) ISCEV guidelines for clinical multifocal electroretinography (2007 edition). Doc Ophthalmol 116(1):1–11
Hood DC, Frishman LJ, Saszik S, Viswanathan S (2002) Retinal origins of the primate multifocal ERG: implications for the human response. Invest Ophthalmol Vis Sci 43(5):1673–1685
Shimada Y, Horiguchi M (2003) Stray light-induced multifocal electroretinograms. Invest Ophthalmol Vis Sci 44(3):1245–1251
Wirth A, Zetterstrom B (1954) Effect of area and intensity on the size and shape of the electroretinogram; exclusion of stray light effects. Br J Ophthalmol 38(5):257–265
Boynton RM (1953) Stray light and the human electroretinogram. J Opt Soc Am 43(6):442–449
Bearse MA, Sutter EE (1996) Imaging localized retinal dysfunction with the multifocal electroretinogram. J Opt Soc Am A Opt Image Sci Vis 13(3):634–640
Sakata LM, Deleon-Ortega J, Sakata V, Girkin CA (2009) Optical coherence tomography of the retina and optic nerve–a review. Clin Experiment Ophthalmol 37(1):90–99
Lim JI, Tan O, Fawzi AA, Hopkins JJ, Gil-Flamer JH, Huang D (2008) A pilot study of Fourier-domain optical coherence tomography of retinal dystrophy patients. Am J Ophthalmol 146(3):417–426
Wirtitsch MG, Ergun E, Hermann B, Unterhuber A, Stur M, Scholda C, Sattmann H, Ko TH, Fujimoto JG, Drexler W (2005) Ultrahigh resolution optical coherence tomography in macular dystrophy. Am J Ophthalmol 140(6):976–983
Hughes EH, Siow YC, Hunyor AP (2009) Acute macular neuroretinopathy: anatomic localisation of the lesion with high-resolution OCT. Eye 23(11):2132–2134
Feigl B, Haas A (2000) Optical coherence tomography (OCT) in acute macular neuroretinopathy. Acta Ophthalmol Scand 78(6):714–716
Chan WM, Liu DT, Tong JP, Law RW, Lam DS (2005) Longitudinal findings of acute macular neuroretinopathy with multifocal electroretinogram and optical coherence tomography. Clin Experiment Ophthalmol 33(4):439–442
Turgot B, Turkcuoglu P, Serder Koca S, Aydemir O (2009) Detection of the regression on hydroxychloroquine retinopathy in optical coherence tomography. Clin Rheumatol 28(5):607–609
Rodriguez-Padilla JA, Hedges TR III, Monson B, Srinivansan V, Wojtkowski M, Reichel E, Duker JS, Schuman JS, Fujimoto JG (2007) High-speed ultra-high-resolution optical coherence tomography findings in hydroxychloroquine retinopathy. Arch Ophthalmol 125(6):775–780
Kellner U, Kellner S, Weinitz S (2008) Chloroquine retinopathy: lipofuscin- and melanin-related fundus autofluorescence, optical coherence tomography and multifocal electroretinography. Doc Ophthalmol 116(2):119–123
Kellner S, Weinitz S, Kellner U (2009) Spectral domain optical coherence tomography detects early stages of chloroquine retinopathy similar to multifocal electroretinography, fundus autofluorescence and near-infrared autofluorescence. Br J Ophthalmol 93(11):1444–1447
Gerth C, Zawadzki RJ, Choi SS, Keltner JL, Park SS, Werner JS (2007) Visualization of lipofuscin accumulation in Stargardt macular dystrophy by high-resolution Fourier-domain optical coherence tomography. Arch Ophthalmol 125(4):575
Ergun E, Hermann B, Wirtitsch M, Unterhuber A, Ko TH, Sattmann H, Scholda C, Fujimoto JG, Stur M, Drexler W (2005) Assessment of central visual function in Stargardt’s disease/fundus flavimaculatus with ultrahigh-resolution optical coherence tomography. Invest Ophthalmol Vis Sci 46(1):310–316
Furino C, Boscia F, Cardascia N, Sborgia L, Sborgia C (2008) Fundus autofluorescence, optical coherence tomography and visual acuity in adult-onset foveomacular dystrophy. Ophthalmologica 222(4):240–244
Petropoulos IK, Desmangles PM, Matter MA (2008) Spectral optical coherence tomography findings in adult-onset foveomacular vitelliform dystrophy. Klin Monatsbl Augenheilkd 255(5):488–490
Saito W, Yamamoto S, Hayashi M, Ogata K (2003) Morphological and functional analyses of adult onset vitelliform macular dystrophy. Br J Ophthalmol 87(6):758–762
Benhamou N, Souied EH, Zolf R, Coscas F, Coscas G, Soubrane G (2003) Adult-onset foveomacular vitelliform dystrophy: a study by optical coherence tomography. Am J Ophthalmol 135(3):362–367
Pierro L, Tremolada G, Introini U, Calori G, Brancato R (2002) Optical coherence tomography findings in adult-onset foveomacular vitelliform dystrophy. Am J Ophthalmol 134(5):675–680
Hood DC, Wladis EJ, Shady S, Holopigian K, Li J, Seiple W (1998) Multifocal rod electroretinograms. Invest Ophthalmol Vis Sci 39(7):1152–1162
Mohamed Q, Harper CA (2007) Acute optical coherence tomographic findings in cancer-associated retinopathy. Arch Ophthalmol 125(8):1132–1133
Do P, Ferrucci S (2006) Adult-onset foveomacular vitelliform dystrophy. Optometry 77(4):156–166
Gass JDM (1974) A clinicopathologic study of a peculiar foveomacular dystrophy. Trans Am Ophthalmol Soc 72:139–156
Hood DC, Odel JG, Chen CS, Winn BJ (2003) The multifocal electroretinogram. J Neuroophthalmol 23(3):225–235
Gomes NL, Greenstein VC, Carlson JN, Tsang SH, Smith RT, Carr RE, Hood DC, Chang S (2009) A comparison of fundus autofluorescence and retinal structure in patients with Stargardt disease. Invest Ophthalmol Vis Sci 50(8):3953–3959
Greenstein VC, Carlson JN, Wang M, Tsang SH, Smith RT, Carr RE, Hood DC (2009) A comparison of retinal structure and visual function in foveal and preferred retinal location regions of patients with Stargardt disease. Poster presented at the annual meeting of the Association for research in vision and ophthalmology (ARVO), Fort Lauderdale, Florida, 3–7 May 2009
Rangaswamy NV, Hood DC, Birch DG, Locke KG (2009) A comparison of visual field sensitivity to photoreceptor thickness in retinitis pigmentosa (RP). Poster presented at the annual meeting of the Association for research in vision and ophthalmology (ARVO), Fort Lauderdale, Florida, 3–7 May 2009
Hood DC, Lin CE, Lazow MA, Locke KG, Zhang X, Birch DG (2009) Thickness of receptor and post-receptor retinal layers in patients with retinitis pigmentosa measured with frequency-domain optical coherence tomography. Invest Ophthalmol Vis Sci 50(5):2328–2336
Jacobson SG, Cideciyan AV, Aleman TS, Sumaroka A, Windsor EA, Schwartz SB, Heon E, Stone EM (2008) Photoreceptor layer topography in children with leber congenital amaurosis caused by RPE65 mutations. Invest Ophthalmol Vis Sci 49(10):4573–4577
Acknowledgments
We would like to thank Drs. Behrens, Bortz, Forman, Kostina-O’Neil, Lesser and Moazami for patient referrals. This study was supported by funds from EY09076 and 02115.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dale, E.A., Hood, D.C., Greenstein, V.C. et al. A comparison of multifocal ERG and frequency domain OCT changes in patients with abnormalities of the retina. Doc Ophthalmol 120, 175–186 (2010). https://doi.org/10.1007/s10633-009-9210-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10633-009-9210-9