Abstract
Background
The complex mechanisms of colorectal cancer (CRC) pathogenesis and progression remain poorly understood. This study endeavors to unravel the role of UBXN11within the context of CRC.
Methods
UBXN11 expression level in CRC, stomach adenocarcinoma and esophageal carcinoma, and the overall survival in corresponding cancers were analyzed using UALCAN database. Human CRC cell lines and xenograft mouse model with UBXN11 overexpression were established to investigate the pathological role of UBXN11 in CRC progression. Luciferase assay, qPCR, and Western blot were performed to dissect the interaction between UBXN11 and NF-κB signaling.
Results
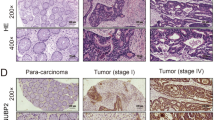
Heightened UBXN11 expression was observed in various digestive tract tumors, which was positively correlated with the reduced overall survival rates in CRC patients. Overexpression of UBXN11 significantly enhanced CRC cell proliferation in vitro and promoted tumor growth in vivo. Mechanistically, UBXN11 promoted CRC tumorigenesis through increasing the activation of NF-κB signaling pathway.
Conclusions
This study underscores the pivotal role of UBXN11 in CRC progression and paves the way for novel therapeutic strategies for CRC treatment.





Similar content being viewed by others
Data Availability
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
References
Assarzadegan N, Montgomery E. What is New in the 2019 World Health Organization (WHO) classification of tumors of the digestive system: review of selected updates on neuroendocrine neoplasms, appendiceal tumors, and molecular testing. Archives of Pathology and Laboratory Medicine. 2021;145:664–677.
Joensuu H, Hohenberger P, Corless CL. Gastrointestinal stromal tumour. Lancet. 2013;382:973–983.
Ahmed M. Colon cancer: a clinician’s perspective in 2019. Gastroenterology Res. 2020;13:1–10.
Benson AB, Venook AP, Al-Hawary MM, et al. Colon cancer, Version 2.2021, NCCN clinical practice guidelines in oncology. Journal of the National Comprehensive Cancer Network. 2021;19:329–359.
Biller LH, Schrag D. Diagnosis and treatment of metastatic colorectal cancer: a review. JAMA. 2021;325:669–685.
Kanth P, Inadomi JM. Screening and prevention of colorectal cancer. BMJ. 2021;374:n1855.
Cross AJ, Sinha R. Meat-related mutagens/carcinogens in the etiology of colorectal cancer. Environmental and Molecular Mutagenesis. 2004;44:44–55.
Rutter MD, Beintaris I, Valori R et al. World endoscopy organization consensus statements on post-colonoscopy and post-imaging colorectal cancer. Gastroenterology. 2018;155(909–925):e903.
Ben-Neriah Y. Karin M. Inflammation meets cancer, with NF-kappaB as the matchmaker Nature Immunology. 2011;12:715–723.
Perkins ND. The diverse and complex roles of NF-kappaB subunits in cancer Nature Reviews: Cancer. 2012;12:121–132.
Verzella D, Pescatore A, Capece D, et al. Life, death, and autophagy in cancer: NF-kappaB turns up everywhere Cell Death & Disease. 2020;11:210
Patel M, Horgan PG, McMillan DC, Edwards J. NF-kappaB pathways in the development and progression of colorectal cancer Translational Research. 2018;197:43–56.
Porta C, Ippolito A, Consonni FM, et al. Protumor steering of cancer inflammation by p50 NF-kappaB Enhances Colorectal Cancer Progression Cancer Immunol Res. 2018;6:578–593
Soleimani A, Rahmani F, Ferns GA, Ryzhikov M, Avan A, Hassanian SM. Role of the NF-kappaB signaling pathway in the pathogenesis of colorectal cancer Gene. 2020;726:144132.
Alexandru G, Graumann J, Smith GT, Kolawa NJ, Fang R, Deshaies RJ. UBXD7 binds multiple ubiquitin ligases and implicates p97 in HIF1alpha turnover Cell. 2008;134:804–816.
Liu W, Yu J, Wang YF, Shan QQ, Wang YX. Selection of suitable internal controls for gene expression normalization in rats with spinal cord injury Neural Regen Res. 2022;17:1387–1392.
Wang Y, Shan Q, Meng Y, Pan J, Yi S. Mrpl10 and Tbp are suitable reference genes for peripheral nerve crush injury. International Journal of Molecular Sciences. 2017;18:263.
Yadav K, Ali SA, Mohanty AK, Muthusamy E, Subaharan K, Kaul G. MSN, MWCNT and ZnO nanoparticle-induced CHO-K1 cell polarisation is linked to cytoskeleton ablation. J Nanobiotechnology. 2021;19:45.
Rezvani K. UBXD proteins: a family of proteins with diverse functions in cancer. International Journal of Molecular Sciences. 2016;17:1724.
Maccalli C, Li YF, El-Gamil M, Rosenberg SA, Robbins PF. Identification of a colorectal tumor-associated antigen (COA-1) recognized by CD4(+) T lymphocytes. Cancer Research. 2003;63:6735–6743.
Tekola-Ayele F, Zeng X, Ouidir M et al. DNA methylation loci in placenta associated with birthweight and expression of genes relevant for early development and adult diseases. Clinical Epigenetics. 2020;12:78.
Zhang J, Guo F, Zhou R et al. Proteomics and transcriptome reveal the key transcription factors mediating the protection of Panax notoginseng saponins (PNS) against cerebral ischemia/reperfusion injury. Phytomedicine. 2021;92:153613.
Ketkar H, Harrison AG, Graziano VR et al. UBX domain protein 6 positively regulates JAK-STAT1/2 signaling. Journal of Immunology. 2021;206:2682–2691.
Yue D, Xu S, Wang Q et al. Updated overall survival and exploratory analysis from randomized, phase II EVAN study of erlotinib versus vinorelbine plus cisplatin adjuvant therapy in stage IIIA epidermal growth factor receptor+ non-small-cell lung cancer. Journal of Clinical Oncology. 2022;40:3912–3917.
Ganly I, Makarov V, Deraje S et al. Integrated genomic analysis of hurthle cell cancer reveals oncogenic drivers, recurrent mitochondrial mutations, and unique chromosomal landscapes. Cancer Cell. 2018;34(256–270):e255.
Zhou X, Ke C, Lv Y et al. Asiaticoside suppresses cell proliferation by inhibiting the NF-kappaB signaling pathway in colorectal cancer. International Journal of Molecular Medicine. 2020;46:1525–1537.
Yu S, Zang W, Qiu Y, Liao L, Zheng X. Deubiquitinase OTUB2 exacerbates the progression of colorectal cancer by promoting PKM2 activity and glycolysis. Oncogene. 2022;41:46–56.
Baidoun F, Elshiwy K, Elkeraie Y et al. Colorectal cancer epidemiology: recent trends and impact on outcomes. Current Drug Targets. 2021;22:998–1009.
Dekker E, Tanis PJ, Vleugels JLA, Kasi PM, Wallace MB. Colorectal cancer. Lancet. 2019;394:1467–1480.
Funding
This research received no specific grant from any funding agency.
Author information
Authors and Affiliations
Contributions
Yubin Wang has given contributions to the conception of the design of the manuscript, analysis and interpretation of the data, and drafting the manuscript. Xiangbo Chen and Yubin Wang revised it critically. Xiangbo Chen, Changxin Chen, Rensong He, Yisen Huang, and Yubin Wang read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest, financial or otherwise, are declared by the authors.
Ethical approval
The study was approved by the Ethics Committee of Quanzhou First Hospital Affiliated to Fujian Medical University to ensure the adherence to ethical research standards. Written informed consent was also obtained from the participants.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, X., Chen, C., He, R. et al. UBXN11 Predicts as a Poor Index for Colorectal Cancer and Contributes to the Tumorigenesis by Activating NF-κB Signaling. Dig Dis Sci (2024). https://doi.org/10.1007/s10620-024-08414-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10620-024-08414-9