Abstract
Background
There are few reports of clinical outcomes or the natural history of definitive diverticular hemorrhage (DDH).
Aims
To describe 1-year clinical outcomes of patients with documented DDH treated with colonoscopic hemostasis, angioembolization, surgery, or medical treatment.
Methods
DDH was diagnosed when active bleeding or other stigmata of hemorrhage were found in a colonic diverticulum during urgent colonoscopy or extravasation on angiography or red blood cell (RBC) scanning. This was a retrospective analysis of prospectively collected data of DDH patients from two referral centers between 1993 and 2022. Outcomes were compared for the four treatment groups. The Kaplan–Meier analysis was for time-to-first diverticular rebleed.
Results
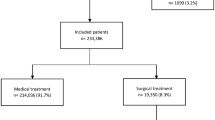
162 patients with DDH were stratified based on their final treatment before discharge—104 colonoscopic hemostasis, 24 medical treatment alone, 19 colon surgery, and 15 angioembolization. There were no differences in baseline characteristics, except for a higher Glasgow–Blatchford score in the angioembolization group vs. the colonoscopic group. Post-treatment, the colonoscopic hemostasis group had the lowest rate of RBC transfusions and fewer hospital and ICU days compared to surgical and embolization groups. The medical group had significantly higher rates of rebleeding and reintervention. The surgical group had the highest postoperative complications.
Conclusions
Medically treated DDH patients had significantly higher 1-year rebleed and reintervention rates than the three other treatments. Those with colonoscopic hemostasis had significantly better clinical outcomes during the index hospitalization. Surgery and embolization are recommended as salvage therapies in case of failure of colonoscopic and medical treatments.
Graphical Abstract
Colonoscopic hemostasis is recommended in patients with definitive diverticular hemorrhage for better clinical outcomes. Surgery and embolization are recommended as salvage therapies in case of failure of colonoscopic and medical treatments.




Similar content being viewed by others
Abbreviations
- ACCI:
-
Age-adjusted Charlson Comorbidity Index
- ASA:
-
American Society of Anesthesiologists (Prognostic score)
- BMI:
-
Body mass index
- CTA:
-
Computed tomography angiography
- CURE:
-
Center of Ulcer Research and Education
- DDH:
-
Definitive diverticular hemorrhage
- DEP:
-
Doppler endoscopic probe
- GI:
-
Gastrointestinal
- GBS:
-
Glasgow-Blatchford score
- gm/dl:
-
Grams per deciliter (for hemoglobin level)
- ICD:
-
International Classification of Diseases
- ICU:
-
Intensive care unit
- INR:
-
International normalized ratio
- IQR:
-
Interquartile range
- IRB:
-
Institutional Review Board
- MPEC:
-
Multipolar electrocoagulation
- NBVV:
-
Non-bleeding visible vessel
- NSAIDs:
-
Nonsteroidal anti-inflammatory drugs
- RBC:
-
Red blood cell (transfusion)
- SD:
-
Standard deviation
- SRH:
-
Stigmata of recent hemorrhage
References
Peery AF, Dellon ES, Lund J, Crockett SD et al. Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology. 2012;143:1179–1187.
Jensen DM, Machicado GA, Jutabha R, Kovacs TO. Urgent colonoscopy for the diagnosis and treatment of severe diverticular hemorrhage. N Engl J Med. 2000;342:78–82.
Jensen DM. Diagnosis and treatment of definitive diverticular hemorrhage (DDH). Am J Gastroenterol. 2018;113:1570–1573.
Jensen DM, Ohning GV, Kovacs TO, Jutabha R et al. Natural history of definitive diverticular hemorrhage based on stigmata of recent hemorrhage and colonoscopic Doppler blood flow monitoring for risk stratification and definitive hemostasis. Gastrointest Endosc. 2016;83:416–423.
Nagata N, Ishii N, Manabe N, Tomizawa K et al. Guidelines for Colonic Diverticular Bleeding and Colonic Diverticulitis: Japan Gastroenterological Association. Digestion. 2019;99(suppl 1):1–26.
Doi H, Sasajima K, Takahashi M, Sato T, Ootsu I, Chinzei R. Effectiveness of Conservative Treatment without Early Colonoscopy in Patients with Colonic Diverticular Hemorrhage. Can J Gastroenterol Hepatol. 2020;2020
Farrell JJ, Friedman LS. Gastrointestinal bleeding in the elderly. Gastroenterol Clin North Am. 2001;30:377–407.
Funaki B, Kostelic JK, Lorenz J, Ha TV et al. Superselective microcoil embolization of colonic hemorrhage. AJR Am J Roentgenol. 2001;177:829–836.
Hoedema RE, Luchtefeld MA. The management of lower gastrointestinal hemorrhage. Dis Colon Rectum. 2005;48:2010–2024.
Longstreth GF. Epidemiology and outcome of patients hospitalized with acute lower gastrointestinal hemorrhage: a population-based study. Am J Gastroenterol. 1997;92:419–424.
Vajravelu RK, Mamtani R, Scott FI, Waxman A, Lewis JD. Incidence, Risk Factors, and Clinical Effects of Recurrent Diverticular Hemorrhage: A Large Cohort Study. Gastroenterology. 2018;155:1416–1427.
Czymek R, Kempf A, Roblick UJ, Bader FG et al. Surgical Treatment Concepts for Acute Lower Gastrointestinal Bleeding. Journal of Gastrointest Surg. 2008;12:2212.
Bloomfeld RS, Rockey DC, Shetzline MA. Endoscopic therapy of acute diverticular hemorrhage. Am J Gastroenterol. 2001;96:2367–2372.
Hokama A, Uehara T, Nakayoshi T, Uezu Y et al. Utility of endoscopic hemoclipping for colonic diverticular bleeding. Am J Gastroenterol. 1997;92:543–546.
Ishii N, Hirata N, Omata F, Itoh T et al. Location in the ascending colon is a predictor of refractory colonic diverticular hemorrhage after endoscopic clipping. Gastrointest Endosc. 2012;76:1175–1181.
Kaltenbach T, Watson R, Shah J, Friedland S et al. Colonoscopy with clipping is useful in the diagnosis and treatment of diverticular bleeding. Clin Gastroenterol Hepatol. 2012;10:131–137.
Simpson PW, Nguyen MH, Lim JK, Soetikno RM. Use of endoclips in the treatment of massive colonic diverticular bleeding. Gastrointest Endosc. 2004;59:433–437.
Couto-Worner I, Gonzalez-Conde B, Estevez-Prieto E, Alonso-Aguirre P. Colonic diverticular bleeding: urgent colonoscopy without purging and endoscopic treatment with epinephrine and hemoclips. Rev Esp Enferm Dig. 2013;105:495–498.
Bender JS, Wiencek RG, Bouwman DL. Morbidity and mortality following total abdominal colectomy for massive lower gastrointestinal bleeding. Am Surg. 1991;57:536–540.
Chen CY, Wu CC, Jao SW, Pai L, Hsiao CW. Colonic diverticular bleeding with comorbid diseases may need elective colectomy. J Gastrointest Surg. 2009;13:516–520.
Renzulli P, Maurer CA, Netzer P, Dinkel H-P, Büchler MW. Subtotal colectomy with primary ileorectostomy is effective for unlocalized, diverticular hemorrhage. Langenbeck’s Arch Surg. 2002;387:67–71.
Heianna J, Miyauchi T, Yamano H, Yoshikawa K, Hashimoto M, Murayama S. Management of angiogram-negative acute colonic hemorrhage: safety and efficacy of colonoscopy-guided superselective embolization. Tech Coloproctol. 2014;18:647–652.
Teng HC, Liang HL, Lin YH, Huang JS et al. The efficacy and long-term outcome of microcoil embolotherapy for acute lower gastrointestinal bleeding. Korean J Radiol. 2013;14:259–268.
Rios A, Montoya MJ, Rodriguez JM, Serrano A et al. Severe acute lower gastrointestinal bleeding: risk factors for morbidity and mortality. Langenbecks Arch Surg. 2007;392:165–171.
Parkes BM, Obeid FN, Sorensen VJ, Horst HM, Fath JJ. The management of massive lower gastrointestinal bleeding. Am Surg. 1993;59:676–678.
Johnston JH, Jensen DM, Auth D. Experimental comparison of endoscopic yttrium-aluminum-garnet laser, electrosurgery, and heater probe for canine gut arterial coagulation. Importance of compression and avoidance of erosion. Gastroenterology. 1987;92:1101–8.
Charlson M, Szatrowski TP, Peterson J, Gold J. Validation of a combined comorbidity index. J Clin Epidemiol. 1994;47:1245–1251.
Blatchford O, Murray WR, Blatchford M. A risk score to predict need for treatment for upper gastrointestinal haemorrhage. Lancet. 2000;356:1318–1321.
Gralnek IM, Jensen DM, Gornbein J, Kovacs TO et al. Clinical and economic outcomes of individuals with severe peptic ulcer hemorrhage and nonbleeding visible vessel: an analysis of two prospective clinical trials. Am J Gastroenterol. 1998;93:2047–2056.
Dindo D, Demartines N, Clavien P-A. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–213.
Watanabe S, Sato A, Kobayashi K, Miyakawa A et al. Colonoscopic observation time as a predictor of stigmata of recent hemorrhage identification in colonic diverticular hemorrhage. Scand J Gastroenterol. 2023;58:304–309.
Gobinet-Suguro M, Nagata N, Kobayashi K, Yamauchi A et al. Treatment strategies for reducing early and late recurrence of colonic diverticular bleeding based on stigmata of recent hemorrhage: a large multicenter study. Gastrointestinal Endoscopy. 2022;95:1210–1222.
Honda H, Ishii N, Takasu A, Shiratori Y, Omata F. Risk factors of early rebleeding in the endoscopic management of colonic diverticular bleeding. Journal of Gastroenterology and Hepatology. 2019;34:1784–1792.
Olafsson GD, Hreinsson JP, Björnsson ES. Incidence of diverticular bleeding: a population-based study. Scand J Gastroenterol. 2019;54:205–209.
Mizuki A, Tatemichi M, Nakazawa A, Tsukada N, Nagata H, Kanai T. Long-Term Clinical Course after Conservative and Endoscopic Treatment of Colonic Diverticular Bleeding. Digestion. 2016;94:186–191.
Niikura R, Nagata N, Aoki T, Shimbo T et al. Predictors for identification of stigmata of recent hemorrhage on colonic diverticula in lower gastrointestinal bleeding. J Clin Gastroenterol. 2015;49:e24-30.
Taki M, Oshima T, Tozawa K, Taniguchi Y et al. Analysis of risk factors for colonic diverticular bleeding and recurrence. Medicine (Baltimore). 2017;96:e8090.
Mohammed Ilyas MI, Szilagy EJ. Management of Diverticular Bleeding: Evaluation, Stabilization, Intervention, and Recurrence of Bleeding and Indications for Resection after Control of Bleeding. Clin Colon Rectal Surg. 2018;31:243–250.
Zuckerman DA, Bocchini TP, Birnbaum EH. Massive hemorrhage in the lower gastrointestinal tract in adults: diagnostic imaging and intervention. AJR Am J Roentgenol. 1993;161:703–711.
Khanna A, Ognibene SJ, Koniaris LG. Embolization as first-line therapy for diverticulosis-related massive lower gastrointestinal bleeding: evidence from a meta-analysis. J Gastrointest Surg. 2005;9:343–352.
Bierle DM, Raslau D, Regan DW, Sundsted KK, Mauck KF. Preoperative Evaluation Before Noncardiac Surgery. Mayo Clinic Proceedings. 2020;95:807–822.
Kaltenbach T, Asokkumar R, Kolb JM, Malvar C, Soetikno R. Use of the Endoscopic Clipping Over the Scope Technique to Treat Acute Severe Lower Gastrointestinal Bleeding in the Colon and Anal Transition Zone. Gastrointest Endosc Clin N Am. 2020;30:13–23.
Kobayashi K, Furumoto Y, Akutsu D, Matsuoka M et al. Endoscopic Detachable Snare Ligation Improves the Treatment for Colonic Diverticular Hemorrhage. Digestion. 2020;101:208–216.
Kobayashi K, Nagata N, Furumoto Y, Yamauchi A et al. Effectiveness and adverse events of endoscopic clipping versus band ligation for colonic diverticular hemorrhage: a large-scale multicenter cohort study. Endoscopy. 2022;54:735–744.
Nagata N, Ishii N, Kaise M, Shimbo T et al. Long-term recurrent bleeding risk after endoscopic therapy for definitive colonic diverticular bleeding: band ligation versus clipping. Gastrointest Endosc. 2018;88:841–53.e4.
Nagata N, Niikura R, Ishii N, Kaise M et al. Cumulative evidence for reducing recurrence of colonic diverticular bleeding using endoscopic clipping versus band ligation: Systematic review and meta-analysis. Journal of Gastroenterology and Hepatology. 2021;36:1738–1743.
Acknowledgments
This study was supported by a Veterans Administration Clinical Merit Review Research Grant [grant number 5I01CX001403] and the National Institutes of Health - National Institute of Diabetes and Digestive and Kidney (NIH - NIDDK) Center of Ulcer Research and Education Digestive Diseases Research Core Center (DDRCC) Human Studies Core [grant number P30DK41301].
Author information
Authors and Affiliations
Contributions
PW: Methodology; data curation; writing—original draft. UK: Data curation; formal analysis; writing—review and editing. DMJ: Conceptualization; supervision; funding acquisition; methodology; data curation; writing—review and editing. MEJ: Data curation; writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflicts of interest.
Ethical approval
All human studies have been approved by the appropriate ethics committee and have, therefore, been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All participants in the study gave their informed consent prior to their inclusion in the study. Details that might disclose the identity of the study participants were omitted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wangrattanapranee, P., Jensen, D.M., Khrucharoen, U. et al. Patient Outcomes of Definitive Diverticular Hemorrhage After Colonoscopic, Medical, Surgical, or Embolization Treatment. Dig Dis Sci 69, 538–551 (2024). https://doi.org/10.1007/s10620-023-08199-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-023-08199-3